Effects of Making Art and Listening to Music on Symptoms Related to Blood and Marrow Transplantation
Purpose/Objectives: To understand the benefits of making art and listening to music and whether those activities may be beneficial for reducing symptoms associated with blood and marrow transplantation.
Design: A randomized, three-group, pre-/post-pilot design.
Setting: Outpatient Blood and Marrow Transplant Clinic at the University of Kansas Cancer Center in Kansas City.
Sample: 39 adults aged from 22–74 years receiving blood and marrow transplantations.
Methods: Participants were randomly assigned to one of three groups: (a) art making, (b) diversional music (comparison), or (c) control (usual treatment). The Therapy-Related Symptoms Checklist was used to assess the patients’ self-reported symptoms related to treatment. The Spielberger State-Trait Anxiety Index was used to measure self-reported anxiety symptoms. Vital signs were obtained pre- and postintervention to measure physiologic stress.
Main Research Variables: Therapy-related symptoms, state anxiety, and physiologic distress.
Findings: Of the 39 participants, 14 were randomized to the control group, 14 to the art group, and 11 to the diversional music group. No significant differences in age, gender, ethnicity, or diagnosis existed between groups. No statistical differences were found between groups on all measures following the intervention.
Conclusions: Although the results of the current study did not indicate significant differences, healthcare professionals may still consider creative therapies as a viable option for patients within hospital or outpatient clinics because they do not require specialty training or costly resources, and they may be an enjoyable activity to occupy time for patients and caregivers.
Implications for Nursing: Art making and music listening are safe and desirable for patients undergoing blood and marrow transplantation in an outpatient clinic. Nurses might consider partnering with therapists to offer these creative therapies as diversion during treatment.
Jump to a section
Blood and marrow transplantation (BMT) can have positive effects on blood and marrow cancers, but it often results in adverse side effects, creating the need for alternative therapies (Carlson & Bultz, 2008; Gabriel et al., 2001; Nainis et al., 2006). The basis of BMT involves transplanting stem cells, which are intended to replace and destroy diseased cells to produce healthy blood-producing cells (Leukemia and Lymphoma Society, 2013). After transplantation, blood and platelet infusions are needed while the immune system and bone marrow return to normal functioning. During treatment, patients are required to adhere to strict infection precautions because of weakened immune systems (Mosher, Redd, Rini, Burkhalter, & DuHamel, 2009; University of Kansas Hospital Cancer Center, 2008). Once blood counts have returned to a normal level, the patient is discharged home with visits to an outpatient clinic two to three times per week for evaluation.
Infection prevention is an important consideration of everyday life for patients undergoing BMT. According to the Leukemia and Lymphoma Society (2013), to decrease the risk of infection, precautions are taken, including patient isolation, limited contact with children, certain dietary precautions, hand hygiene, and personal protective equipment. Required precautions to prevent infections may create feelings of isolation because of physical and social barriers (Gabriel et al., 2001; Mosher et al., 2009).
In addition to feelings of isolation during BMT, other health-related side effects can occur and affect quality of life, which increases the need for interventions to address physical and psychosocial demands (Frodin, Borjeson, Lyth, & Lofti, 2011). Side effects for patients undergoing BMT vary by individual characteristics, treatment stage, and treatment plan. Physical side effects that may have implications for participation in daily activities include musculoskeletal stiffness, cramps, weakness, joint swelling, fatigue, diarrhea, hair loss, mucositis, nausea, vomiting, pneumonia, and premature menopause (Mosher et al., 2009). Emotional and psychological side effects that survivors may face are intrusive recollections of treatment, distressing cognitive side effects, fear of relapse and death, difficulty resuming former roles, sense of isolation, decrease in sexual interest, financial insecurity, anxiety, and depression (Mosher et al., 2009).
Creative Therapies
Creative interventions can be used to address the side effects of the disease process. Creative therapies are an opportunity for personalized expression of the cancer experience with physical, emotional, and spiritual activities (Carlson & Bultz, 2008). Participation in creative interventions has shown improvements in physiologic health, anxiety, and stress for patients with cancer and other chronic illnesses (Sandmire, Gorham, Rankin, & Grimm, 2012; Stuckey & Nobel, 2010). Music and art interventions have been used for pain reduction, diversion from unpleasant treatment, coping, and making sense of illness for people with a variety of conditions (Cassileth, Vickers, & Magill, 2003; Collie, Bottorff, & Long, 2006; Mische Lawson, Glennon, et al., 2012; Mische Lawson, Williams, et al., 2012).
Engaging in art making has shown particular benefit for patients with cancer to manage side effects associated with treatment (Archer, Buxton, & Sheffield, 2015; Mische Lawson, Williams, et al., 2012; Nainis et al., 2006). Past research has looked at the effects of art therapy and art making as two forms of visual artistic expression that may provide psychosocial support for individuals with cancer (Collie et al., 2006). Other studies have examined the effectiveness of art making as an approach that is practical, cost efficient, and does not require a trained art therapist (Collie et al., 2006; Mische Lawson, Glennon, et al., 2012; Mische Lawson, Williams, et al., 2012). When patients engage in art therapy or art making, they may be able to more clearly understand what they are experiencing, reduce emotional pain, and have an opportunity to revitalize themselves and be proud of what they have created (Collie et al., 2006). In addition, art making is a way for patients to occupy their time during treatment and has been found to have an effect on patients’ energy level, concentration, and psychological stress (Mische Lawson, Williams, et al., 2012).
Similar to art, music has shown a positive impact on individuals with cancer. Literature suggests that music therapy may reduce mood disturbances, such as anxiety and depression, in this population (Carlson & Bultz, 2008). Benefits of music therapy include immediate and long-term effects (Cassileth et al., 2003). Creative therapies, such as art and music therapy, have been linked to improved psychological symptoms in patients with cancer (Puetz, Morley, & Herring, 2013). Art and music therapies require specially trained professionals to lead the interventions and, therefore, can be costly and time consuming (Mische Lawson, Williams, et al., 2012). Providing low-cost interventions is increasingly important to maximize resources for patient-centered care.
The purpose of the current study is to understand the benefits of making art and listening to music and whether they are beneficial for reducing symptoms associated with BMT. The authors hypothesized that one hour of making art or listening to music would reduce therapy-related symptoms (e.g., fatigue, nausea), anxiety, and physiologic stress. The three specific aims were (a) to determine the advantage of a one-hour session of making art compared to usual care and diversional music on patients’ global cancer-related symptoms as measured by the Therapy-Related Symptoms Checklist (TRSC), (b) to determine the effect of the intervention modalities on patients’ anxiety with the Spielberger State-Trait Anxiety Index (STAI), and (c) to determine the feasibility of vital signs (e.g., blood pressure, pulse, temperature, respiration) as a measure of physiologic stress for future research with patients undergoing BMT.
Methods
Researchers recruited 39 patients receiving treatment in the University of Kansas Hospital’s outpatient BMT clinic to participate in the study. Participants were offered a $25 gift card incentive to participate in the study. Patients were included in the study if they were (a) receiving treatments at the hospital’s BMT clinic, (b) aged 18 years or older, (c) cognitively intact, (d) able to provide informed consent, and (e) capable of participating in the intervention for 60 minutes. Nurses on staff identified patients that were excluded from recruitment because of health reasons or immunosuppression precautions, and all others were invited to participate.
The study used a randomized, three-group, pre-/post-pilot design to measure how art making and diversional music influenced therapy-related side effects of patients with cancer. Participants were randomly assigned to one of three groups: (a) art making, (b) diversional music (comparison), or (c) control (usual treatment).
Intervention
The Tiles of Hope (TOH) program (i.e., the art-making intervention) started in 2009 as a way for patients undergoing BMT to reflect on the cancer experience using art. Patients were able to paint as many times as they desired during treatment at the BMT clinic. For the current study, patients were provided with all the necessary supplies (e.g., paintbrushes, paint, pencils) to paint a blank 4-inch by 4-inch ceramic tile in their treatment room. Volunteers provided a brief description of the TOH program, and participants painted freely for 60 minutes. Once tiles were finished, they were taken to a local ceramic studio to be glazed and fired. The tiles were then displayed anonymously in the hallway of the cancer center.
The participants assigned to the music group followed the same protocol as the TOH art group but were given a sterilized Apple iPad mini with the Spotify® music mobile application. For additional protection, each device was placed in a disposable, waterproof sleeve, and disposable headphones were supplied to each participant. Researchers instructed participants to listen to a preexisting radio playlist, create their own playlist, or listen to individual songs for 60 minutes. Preexisting playlists included a variety of music genres from a variety of eras. Participants unfamiliar with the tablet computer were provided instructions on how to use it, but minimal interaction occurred between the participants and researchers throughout the 60 minutes. The tablet computers were protected with a passcode to prevent access to other applications or features to minimize co-intervention biases.
The control group participated in typical activities during BMT, such as watching television, talking with a caregiver, and using a computer. Control group participants were asked to not engage in art making or music listening for the 60-minute study period but were offered the opportunity to do those activities after the research period concluded. Although participants were welcome to engage in TOH or music listening as many times as they wished throughout treatment, they participated only once in either art making, music listening, or the control condition for this study.
Instruments
The TRSC is a self-report checklist of 25 symptoms related to treatment. Participants score items, such as nausea, fever, hair loss, jaw pain, and depression, on a Likert-type scale, with higher scores indicating greater severity of symptoms. Each item is scored on a five-point scale from 0 (none) to 4 (very). The TRSC instructs participants to identify and rate their symptoms that occurred since the last cancer treatment session. For this study, participants rated their symptoms at that time. Previous studies show that the TRSC is a valuable survey with the oncology population in reporting symptoms that might otherwise go unreported to medical staff (Mische Lawson, Williams, et al., 2012; Williams et al., 2013). Literature supports reliability and validity of the TRSC for use with the oncology population (Williams et al., 1997). Cronbach alphas of the total scale and the four-item subscales were all greater than 0.7.
The STAI measures self-reported anxiety symptoms at that moment in time, using statements such as “I feel calm” or “I feel nervous,” with higher scores indicating greater anxiety. Scores ranged from 1 (not at all) to 4 (very much so). The STAI has been applied and demonstrated effectiveness in previous creative arts and oncology studies (Nainis et al., 2006; Sandmire et al., 2012). The literature also supports reliability and validity (Cronbach alpha = 0.85–0.95 for all items) of the STAI for use with the oncology population (Spielberger & Vagg, 1984; Spielberger, Gorusch, & Lushene, 1969).
Vital signs, including heart rate, blood pressure, respirations, and temperature, were taken pre- and postintervention. Although use of vital signs as a measure of physiologic stress is an emerging practice, previous research has shown that vital sign measurements can effectively assess physiologic changes after music interventions (Akombo, 2006; Bradt, Dileo, Grocke, & Magill, 2011; Chafin, Roy, Gerin, & Christenfeld, 2004; Ferrer, 2007). Participants also completed a demographic form, outlining highest level of education, marital status, cancer type, treatment stage, and other health-related issues.
Procedures
Researchers obtained approval prior to conducting research from the cancer center protocol review and the university institutional review board at the University of Kansas Medical Center and the University of Kansas Cancer Center, both in Kansas City. Researchers provided written and oral information about the research study and obtained informed written consent before beginning data collection. The TOH program volunteers introduced the free tile-painting program to clinic patients. Those who expressed interest in painting were asked if they would like to participate in the research study through convenience sampling. The recruited participants were then randomly assigned to one of the three groups using a computer-generated randomization table. Participants then completed the demographic form, the STAI, and the TRSC, and a nurse acting as the research assistant gathered the vital sign data. The participants then began the intervention and completed each outcome measure again after 60 minutes of participation in the assigned intervention. Only patients participated in this study; however, caregivers were often present and occasionally participated in their own tile painting. Patients were invited to participate in the study throughout the BMT process, including pretreatment, during the transplantation, and post-treatment. Because patients were isolated to individual treatment rooms and entered the facility through a limited access entry, contamination across groups was avoided.
Data Analysis
Researchers used descriptive statistics to analyze demographic data and analysis of covariance (ANCOVA) to analyze differences between groups on all outcomes. Although participants were randomly assigned to one of three groups to control for group differences, differences existed between groups on some pretest scores (i.e., STAI, TRSC, blood pressure, and respiration). Researchers used pretest measures of each outcome variable as the covariate to control for differences between groups at pretesting (Portney & Watkins, 2009; Vickers, 2001). To conduct ANCOVA, researchers computed change scores (difference from pre- to postintervention) for each measure. Missing data were excluded from analysis, which prevented calculation of subscale and total scores for some participants.
Results
Participants were aged from 22–74 years (mean = 49.54, SD = 14.42) and were mostly Caucasian, with the majority diagnosed with acute myelogenous leukemia (see Table 1).
[[{"type":"media","view_mode":"media_original","fid":"21881","attributes":{"alt":"","class":"media-image","height":"1062","typeof":"foaf:Image","width":"367"}}]]
Nineteen men and 20 women participated in the study. Thirty-seven patients had received or were scheduled to receive a transplantation, with most transplantations being allogeneic. Two participants were receiving their second transplantation because the first transplantation was unsuccessful. No significant differences in age, gender, ethnicity, or diagnosis existed between the three groups. Pretest reports of therapy-related symptoms for all participants showed that patients indicated at least mild severity for 13 of 25 symptoms and were most bothered by feeling sluggish, pain, and loss of appetite (see Table 2). 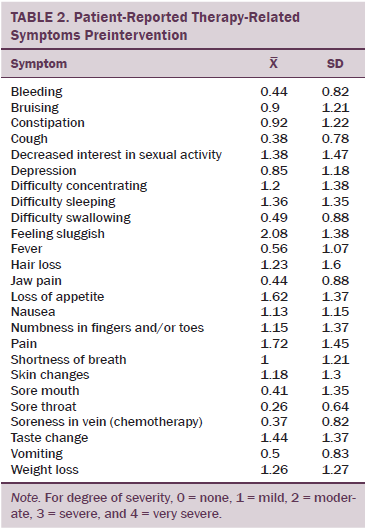
The authors hypothesized that engaging in art or music would reduce state anxiety and therapy-related symptoms as measured by the STAI and TRSC. Results did not support the hypothesis because ANCOVA showed no significant differences from pre- to post-test on summary scores of both measures. The authors also hypothesized that engaging in art or music would reduce physiologic stress as measured by participants’ vital signs (blood pressure, pulse, temperature, and respiration). Again, results did not support the hypothesis because ANCOVA showed no significant differences from pre- to post-test on any vital sign measures (see Table 3). To provide detail of changes across groups, the authors performed pre- and post-test means and standard deviations of the 13 symptoms for which patients indicated at least mild severity at pretest. Although differences were not significant, the music group showed the most improvement in the three symptoms patients found most bothersome at pretest (feeling sluggish, pain, and loss of appetite). 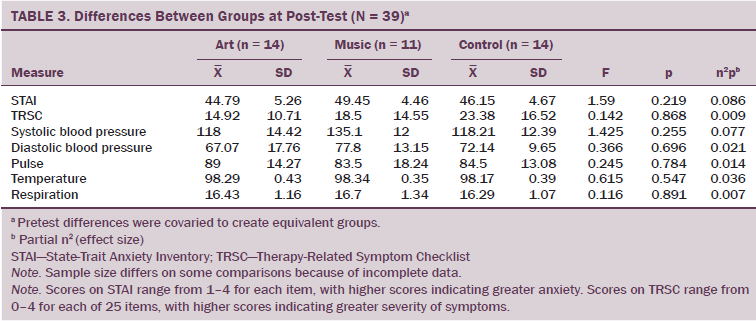
The authors aimed to determine the feasibility of vital signs as a measure of physiologic stress with patients undergoing BMT. Collecting vital signs immediately before and after the intervention or control period proved to be problematic because of nursing staff availability and demands of the individual’s treatment process. Very little variation existed across all three groups in respiration and pulse pre- and postintervention. Because individuals with extremely compromised immune systems were excluded from the study, all temperatures were within normal limits. Variations in blood pressure were found, but several patients were receiving BMT treatment and/or maintenance medications that could affect blood pressure, making this an unusable measure.
Discussion
Although the current study did not find any significant changes in therapy-related symptoms and state anxiety from one hour of art making or diversional music, previous literature has demonstrated the potential benefits of music or art interventions for patients receiving cancer treatment (Mische Lawson, Gannon, et al., 2012; Mische Lawson, Williams, et al., 2012). Previous quantitative studies have demonstrated that one hour of art making while receiving cancer treatment resulted in significantly less therapy-related symptoms, state anxiety, stress, pain, tiredness, depression, drowsiness, and breathlessness, as well as significantly higher well-being and appetite as self-reported using the STAI, the TRSC, or the Edmonton Symptom Assessment Scale (Mische Lawson, Glennon, et al., 2012; Nianis et al., 2006). Although the current authors used similar measures (STAI and TRSC) to measure anxiety- and therapy-related symptoms in this study, differences were not detected in the intervention group, which may be because of the addition of an active comparison group and small sample size. Forty-five participants were needed (15 per group) to adequately power the study, but the authors were unable to recruit the full sample because of construction on the BMT unit at the time of the study, resulting in reduced patient numbers. Although results did not indicate benefit from participation in making art or listening to music, no adverse events were found, indicating that the interventions were harmless. This is consistent with previous literature that indicates art and music interventions do not cause harm, are noninvasive, and can be inexpensive (Cassileth et al., 2003; Wood, Molassiotis, & Payne, 2011).
Previous research on music interventions indicated mixed results, particularly in the reduction of pain and fatigue (Bradt et al., 2011). In addition, when listening to music, patients with cancer reported reduction of anxiety on the STAI and improvements on overall mood and physiologic symptoms (Bradt et al., 2011). The music intervention in the current study did not reduce anxiety as measured by the STAI. The music interventions in previous studies included music preselected by therapists and/or researchers to produce a desired effect (e.g., relaxation, pain reduction) (Nilsson, 2008). The current study used the Spotify mobile application, allowing access to a wide range of music the participants could choose. Participants possibly chose music that was more invigorating than calming, influencing self-reported anxiety (Nilsson, 2008). Spiritual or gospel music was also frequently chosen, which may have fostered reflection of the cancer experience during the intervention. Reflecting on one’s cancer experience may have temporarily increased self-reported anxiety, particularly compared to the control group engaging in typical activities used for distraction (Mische Lawson, Williams, et al., 2012). Because the music intervention was offered through a tablet computer, anxiety related to the use of technology may have influenced results, particularly for individuals who do not routinely use technology (Czaja et al., 2006; Volkom, 2014).
The interventions may have benefited patients, but the authors may not have detected benefits because of measuring outcomes immediately after participation in a short experience. Evidence suggests length and frequency of art or music therapy may influence overall benefits. Although some studies have demonstrated that patients reported statistically significant reductions in symptoms of pain, tiredness, depression, anxiety, drowsiness, appetite, well-being, and breathlessness immediately after one hour of art therapy (Mische Lawson, Glennon, et al., 2012; Nianis et al., 2006), others have shown longer intervention periods of eight weeks or more to be beneficial in reducing cancer-related distress (Garland, Tamagawa, Todd, Speca, & Carlson, 2013). In addition, a systematic review of randomized, controlled trials of creative art therapies on psychological symptoms of patients with cancer found that creative art therapies demonstrated significant effects on reducing anxiety, depression, and pain, as well as increasing quality of life, after but not during the intervention (Puetz et al., 2013). This suggests that effects may not be realized until later; therefore, measuring outcomes immediately after intervention may not detect improvements. Future research is needed to better understand the best time to assess overall benefits of interventions and frequency and duration of interventions that are the most beneficial.
Limitations and Strengths
The study had a relatively small sample size. The authors aimed to recruit 45 participants (15 per group), but researchers were unable to recruit the full sample because of scheduling conflicts, competing workload of clinical researchers, and renovations in the BMT clinic. Incomplete questionnaires further reduced the sample for analyses. The sample also may have been healthier than the general population of patients undergoing BMT because participants were excluded by nursing staff because of health reasons or immunosuppression precautions.
The physical environment may have caused a disruption because construction work took place on the BMT unit for several months during the study. Construction decreased the number of patients available to participate in the study because of the amount of treatment rooms on the unit and changed the work demands of nurse researchers involved in data collection. Because medical treatment at the BMT clinic was a priority over participation in research, patients were occasionally interrupted by the nursing staff or physicians attending to their individual treatments. These interruptions may have disrupted the experience of flow, as described by Nakamura and Csikszentmihalyi (2002), influencing the postintervention survey results.
Some technical problems also occurred. The authors used a paid Spotify subscription on tablet computers to offer the music intervention. The paid subscription eliminated popup advertisements to maximize the music listening experience. However, the Spotify account could not be used by more than one participant at the same time. When multiple participants were using Spotify at the same time, the song changed on all devices when one person changed the song. The random assignment rarely required more than one music participant simultaneously, but this may have created a negative experience for the first few music group participants before the authors learned of this issue. In addition, not all the participants were familiar with using Spotify or a tablet computer. Although the research protocol included instructing the participants to use the technology, some learned more easily than others, which may have influenced their experience.
Vital signs have been used as a measure of physiologic stress in previous studies (Nilsson, 2008); however, they may not have detected meaningful results with this population. A systematic review of music interventions showed vital signs and salivary cortisol as the most commonly used outcome measures for physiologic stress (Nilsson, 2008; Smith, Birmingham, & Uchino, 2012). Research demonstrated mixed results using vitals as an outcome measure for art and music interventions (Mische Lawson, Williams, et al., 2012; Nilsson, 2008; Wood et al., 2011). For the current study, several of the medications associated with BMT caused changes in blood pressure, which may have influenced the results more than participation in the intervention. Future research is needed to determine a meaningful outcome measure for physiologic stress within this population.
Although a number of limitations existed, several strengths were also found in this study. The study sample was representative of the population of patients receiving treatment at the BMT clinic in terms of age, gender, and ethnicity. Participants were willing to be randomized into each of the three groups. Allowing participants to engage in the intervention of their choice after the data collection period appeared to increase agreement to randomization and decrease drop out. The technology for offering the music intervention was easily usable and well liked by study participants.
Conclusion
The study provides a good basis for further research. Future research may consider using a randomized, controlled trial design with a larger sample size. Using measures of physiologic stress other than vital signs may be beneficial because more research is needed for outcomes measuring physiologic stress within this population. Although the results of the present study did not indicate significant differences, healthcare professionals may still consider creative therapies as a diversion for patients within the hospital or outpatient clinics because they do not require specialty training or costly resources, and they may be an enjoyable activity to occupy time for patients and caregivers. Previous qualitative studies of creative therapies have revealed positive effects for individuals with cancer (Mische Lawson, Glennon, et al., 2012). Creative therapies also cause no physical harm when the correct precautions are followed.
The authors gratefully acknowledge Jill Hardy, RN, BSN, and Gladys Shaw, RN, for their contributions to recruitment and data collection, as well as the patients who participated in this study.
References
Akombo, D.O. (2006). Effects of listening to music as an intervention for pain and anxiety in bone marrow transplant patients (Unpublished doctoral dissertation). University of Florida, Gainesville. Retrieved from http://etd.fcla.edu/UF/UFE0015752/akombo_d.pdf
Archer, S., Buxton, S., & Sheffield, D. (2015). The effect of creative psychological interventions on psychological outcomes for adult cancer patients: A systematic review of randomised controlled trials. Psycho-Oncology, 24, 1–10. doi:10.1002/pon.3607
Bradt, J., Dileo, C., Grocke, D., & Magill, L. (2011). Music interventions for improving psychological and physical outcomes in cancer patients. Cochrane Database of Systematic Reviews, 8, CD006911. doi:10.1002/14651858.CD006911.pub2
Carlson, L.E., & Bultz, B.D. (2008). Mind-body interventions in oncology. Current Treatment Options in Oncology, 9, 127–134. doi:10.1007/s11864-008-0064-2
Cassileth, B.R., Vickers, A.J., & Magill, L.A. (2003). Music therapy for mood disturbance during hospitalization for autologous stem cell transplantation. Cancer, 98, 2723–2729. doi:10.1002/cncr.11842
Chafin, S., Roy, M., Gerin, W., & Christenfeld, N. (2004). Music can facilitate blood pressure recovery from stress. British Journal of Health Psychology, 9, 393–403. doi:10.1348/1359107041557020
Collie, K., Bottorff, J.L., & Long, B.C. (2006). A narrative view of art therapy and art making by women with breast cancer. Journal of Health Psychology, 11, 761–775. doi:10.1177/1359105306066632
Czaja, S.J., Charness, N., Fisk, A.D., Hertzog, C., Nair, S.N., Rogers, W.A., & Sharit, J. (2006). Factors predicting the use of technology: Findings from the Center for Research and Education on Aging and Technology Enhancement (CREATE). Psychology and Aging, 21, 333–352. doi:10.1037/0882-7974.21.2.333
Ferrer, A.J. (2007). The effect of live music on decreasing anxiety in patients undergoing chemotherapy treatment. Journal of Music Therapy, 44, 242–255. doi:10.1093/jmt/44.3.242
Frodin, U., Borjeson, S., Lyth, J., & Lotfi, K. (2011). A prospective evaluation of patients’ health-related quality of life during auto-SCT: A 3-year follow-up. Bone Marrow Transplantation, 46, 1345–1352. doi:10.1038/bmt.2010.304
Gabriel, B., Bromberg, E., Vandenbovenkamp, J., Walka, P., Kornblith, A.B., & Luzzatto, P. (2001). Art therapy with adult bone marrow transplant patients in isolation: A pilot study. Psycho-Oncology, 10, 114–123. doi:10.1002/pon.498
Garland, S.N., Tamagawa, R., Todd, S.C., Speca, M., & Carlson, L.E. (2013). Increased mindfulness is related to improved stress and mood following participation in a mindfulness-based stress reduction program in individuals with cancer. Integrative Cancer Therapies, 12, 31–40. doi:10.1177/1534735412442370
Leukemia and Lymphoma Society. (2013). Blood and marrow stem cell transplantation. Retrieved from https://www.lls.org/content/nationalcontent/resourcecenter/freeeducatio…
Mische Lawson, L., Glennon, C., Amos, M., Newberry, T., Pearce, J., Salzman, S., & Young, J. (2012). Patient perceptions of an art-making experience in an outpatient blood and marrow transplant clinic. European Journal of Cancer Care, 21, 403–411. doi:10.1111/j.1365-2354.2011.01316.x
Mische Lawson, L., Williams, P., Glennon, C., Carithers, K., Schnabel, E., Andrejack, A., & Wright, N. (2012). Effect of art making on cancer-related symptoms of blood and marrow transplantation recipients [Online exclusive]. Oncology Nursing Forum, 39, E353–E360. doi:10.1188/12.ONF.E353-E360
Mosher, C.E., Redd, W.H., Rini, C.M., Burkhalter, J.E., & DuHamel, K.N. (2009). Physical, psychological, and social sequelae following hematopoietic stem cell transplantation: A review of the literature. Psycho-Oncology, 18, 113–127. doi:10.1002/pon.1399
Nainis, N., Paice, J.A., Ratner, J., Wirth, J.H., Lai, J., & Shott, S. (2006). Relieving symptoms in cancer: Innovative use of art therapy. Journal of Pain and Symptom Management, 31, 162–169. doi:10.1016/j.jpainsymman.2005.07.006
Nakamura, J., & Csikszentmihalyi, M. (2002). The concept of flow. In C.R. Snyder & S.J. Lopez (Eds.), Handbook of positive psychology (pp. 89–105). New York, NY: Oxford University Press.
Nilsson, U. (2008). The anxiety-and pain-reducing effects of music interventions: A systematic review. AORN Journal, 87, 780–807. doi:10.1016/j.aorn.2007.09.013
Portney, L.G., & Watkins, M.P. (2009). Foundations of clinical research: Applications to practice (3rd ed.). Upper Saddle River, NJ: Pearson and Prentice Hall.
Puetz, T.W., Morley, C.A., & Herring, M.P. (2013). Effects of creative arts therapies on psychological symptoms and quality of life in patients with cancer. JAMA Internal Medicine, 173, 960–969. doi:10.1001/jamainternmed.2013.836
Sandmire, D.A., Gorham, S.R., Rankin, N.E., & Grimm, D.R. (2012). The influence of art making on anxiety: A pilot study. Journal of the American Art Therapy Association, 29, 68–73. doi:10.1080/07421656.2012.683748
Smith, T.W., Birmingham, W., & Uchino, B.N. (2012). Evaluative threat and ambulatory blood pressure: Cardiovascular effects of social stress in daily experience. Health Psychology, 31, 763–766. doi:10.1037/a0026947
Spielberger, C., Gorusch, R., & Lushene, R. (1969). The State-Trait Anxiety Inventory manual. Palo Alto, CA: Consulting Psychologist Press.
Spielberger, C., & Vagg, P. (1984). Psychometric properties of the STAI: A reply to Ramanaiah, Franzen, and Schill. Journal of Personal Assessment, 48, 95–97.
Stuckey, H.L., & Nobel, J. (2010). The connection between art, healing, and public health: A review of current literature. American Journal of Public Health, 100, 254–263. doi:10.2105/ajph.2008.156497
University of Kansas Hospital Cancer Center. (2008). The University of Kansas Hospital blood and marrow transplant program education manual. Kansas City, KS: University of Kansas Hospital.
Vickers, A.J. (2001). The use of percentage change from baseline as an outcome in a controlled trial is statistically inefficient: A simulation study. BMC Medical Research Methodology, 1, 6. doi:10.1186/1471-2288-1-6
Volkom, M.V. (2014). Revisiting the digital divide: Generational differences in technology use in everyday life. North American Journal of Psychology, 16, 557–574.
Williams, P.D., Ducey, K., Williams, A., Sears, A., Tobin-Rummelhart, S., & Bunde, P. (1997). A Therapy-Related Symptom Checklist (TRSC) for oncology patients: A self-report instrument. Oncology Nursing Forum, 24, 301.
Williams, P.D., Graham, K.M., Storlie, D., Pedance, T.M., Haeflinger, K.V., Williams, D.D., . . . Williams, A.R. (2013). Therapy-Related Symptom Checklist (TRSC) use during treatments at a Cancer Center. Cancer Nursing, 36, 245–254. doi:10.1097/NCC.0b013e3182595406
Wood, M.M., Molassiotis, A., & Payne, S. (2011). What research evidence is there for the use of art therapy in the management of symptoms in adults with cancer? A systematic review. Psycho-Oncology, 20, 135–145. doi:10.1002/pon.1722
About the Author(s)
Mische Lawson is an associate professor in the Department of Occupational Therapy Education at the University of Kansas Medical Center in Kansas City; Glennon is the director of Cancer Services at the University of Kansas Cancer Center in Kansas City; Fiscus is an occupational therapist at Edgemere Senior Living in Dallas, TX; Harrell, Krause, and Moore are all research assistants in the Department of Occupational Therapy at the University of Kansas Medical Center in Kansas City; and Smith is an occupational therapist at Rehab Alliance in Laguna Hills, CA. This study was supported, in part, by funding from the University of Kansas Medical Center Interprofessional Clinical Research Grant. Mische Lawson and Glennon contributed to the conceptualization and design. Mische Lawson provided the statistical support. All authors contributed to the data collection. Mische Lawson, Fiscus, Harrell, Krause, Moore, and Smith contributed to the analysis and manuscript preparation. Mische Lawson can be reached at lmische-lawson@kumc.edu, with copy to editor at ONFEditor@ons.org. Submitted May 2015. Accepted for publication July 24, 2015.

