Improving Self-Efficacy and Self-Care in Adult Patients With a Urinary Diversion: A Pilot Study
Purpose/Objectives: To evaluate the feasibility and acceptability of a multimodality educational intervention for improving self-efficacy (SE) and self-care in patients with a new urinary diversion (UD).
Design: Two-arm randomized, controlled trial.
Setting: Academic medical center in New York.
Sample: 8 adults diagnosed with bladder cancer requiring UD.
Methods: A multimodality educational intervention consisting of video, Microsoft PowerPoint® slides, and medical illustrations was developed. SE was assessed pre- and postintervention related to care of the UD. Education scale scores provided evidence for intervention acceptability and assessment of UD self-care skills.
Main Research Variables: Feasibility, acceptability, results of SE, and self-care scales.
Findings: Enrollment and retention was 100%. All participants took part in every aspect of the study. No issues were apparent with administration of the study; however, a lack of self-care independence was noted between the study arms. The control group was younger in age than the intervention group.
Conclusions: A supplemental multimethod educational intervention is acceptable in this population and feasible to integrate into hospital care or into an appropriately powered study.
Implications for Nursing: A need exists for ongoing postdischarge support and education in this population. Additional studies are needed to determine the best approach for this.
Jump to a section
Bladder cancer continues to be a significant health problem, with an estimated 79,030 Americans being diagnosed in 2017 (Siegel, Miller, & Jemal, 2017). A majority of bladder cancer originates in the transitional cell epithelium lining the bladder wall; 30% of these cases are estimated to invade the muscle wall of the bladder (Chou et al., 2016; National Cancer Institute, 2017). The gold standard for treatment of muscle invasive bladder cancer consists of radical cystectomy with a urinary diversion (UD), constructed with segments of small and large intestines (Mohamed et al., 2012). Three types of UDs are used: incontinent conduit (IC), continent cutaneous diversion (CCD), and orthotopic neobladder (ONB) (Lee et al., 2014). The IC is an incontinent diversion that empties urine through a stoma on the abdominal wall into an ostomy bag; the most common type is referred to as an ileal conduit. The CCD is a UD that requires intermittent catheterization of a stoma located on the abdominal wall when healed. The ONB is a form of continent UD that is anastomosed to the native urethra and allows normal micturition when healed (Lee et al., 2014) (see Figures 1–3).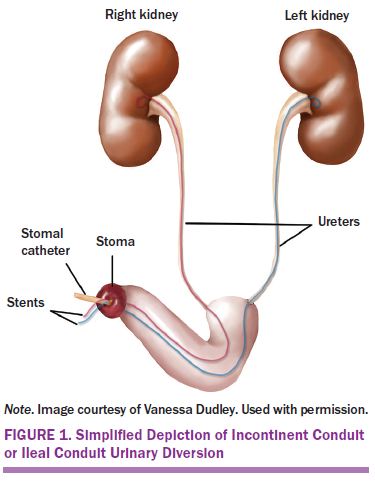
New self-care skills are required to manage a UD after surgery; the patient and his or her family will ultimately be responsible for care of the UD once discharged home from the hospital (Mohamed et al., 2014). Shorter lengths of hospital stay imply patients and families have less time to absorb all of the information presented to them, leading to challenges in adequately preparing them for adaptation after surgery (Aghazadeh et al., 2011; Mohamed et al., 2014). Self-care skills specific to RC differ postoperatively depending on the type of UD used. Continent UD requires irrigation through drainage catheters until the UD is completely healed and drainage tubes are removed, whereas IC UD requires managing and changing urostomy appliance and bag. In addition, both forms of UD require the connecting and emptying of urinary drainage bags.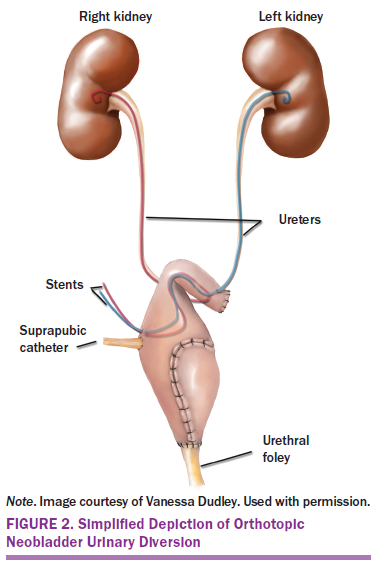
Self-efficacy (SE) represents “beliefs in one’s capabilities to organize and execute the course of action required to produce given attainments” (Bandura, 1997, p. 3). Improved SE can lead to successful adaptation of new behaviors, such as self-care skills (Bandura, 1977). Interventions targeting SE specific to this population represent a possible area of focus in overcoming the challenges related to adaptation after surgery, particularly self-care needs.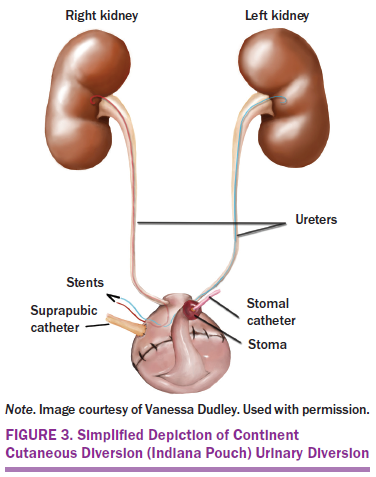
The aim of this pilot study was to explore the feasibility and acceptability of a hospital-based, supplemental, multimethod education intervention aimed at improving SE and self-care in patients with bladder cancer status post-RC with a UD. Variables of interest related to feasibility and acceptability that were evaluated include recruitment, enrollment, retention, and accessibility.
Bandura’s theory of self-efficacy guided this study (Bandura, 1977). Bandura (1977) identified four major categories of influence on SE that were targeted by the interventions in this study: performance accomplishment, vicarious experience, verbal persuasion, and emotional arousal. Performance accomplishment occurs when a task is mastered or accomplished successfully. Vicarious experiences result through observation of others completing a task or behavior successfully. Verbal persuasion takes place through verbal explanations or encouragement. Emotional cues or physiologic cues are the body’s physiologic response to anticipated behavior. Interventions focused on these four categories have the potential desired outcome of improved SE, leading to potential behaviors of adequate self-care. Interventions for this study have been imbedded into a model with Bandura’s corresponding source of SE (see Figure 4).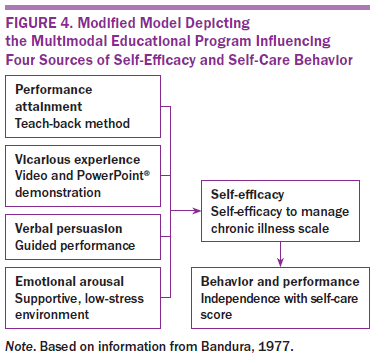
Review of the Literature
In alignment with Bandura’s (1977) theory, educational programs represent interventions that have the potential to improve SE and self-care behavioral outcomes. A review of the literature found a dearth of studies on educational interventions regarding patients with UD, and none that have evaluated or measured SE in patients with a UD. An educational study that includes a measure of SE and self-care on a similar population was then highlighted as a need to help demonstrate the potential benefits of such interventions.
Educational Interventions for Patients With a Urinary Diversion
Three studies were identified that examined educational interventions in patients with a UD (Ali & Khalil, 1989; Mohamed & Mohamed, 2014; Watson, 1983). Unfortunately, none evaluated or targeted SE.
A randomized, controlled trial (RCT) by Watson (1983) explored the effects of postoperative counseling sessions on self-esteem and self-concept in fecal ostomy and patients with IC. Those in the intervention group received three to four postoperative counseling sessions that covered topics such as cancer, ostomy experience, and self-esteem. Self-concept and self-esteem scores were significantly improved in the intervention group (p ≤ 0.01). In addition, the study found that those in the intervention group reported a greater level of ostomy self-care then the control group (p < 0.05).
Mohamed and Mohamed (2014) studied the impact of educational sessions on patients with IC in Egypt. The interventions in the RCT were five two-hour educational sessions that covered self-care, demonstration and return demonstration, and handouts. Urostomy self-care was found to be significantly superior in the intervention group immediately following the intervention (p < 0.001) and at six months (p < 0.001).
An RCT by Ali and Khalil (1989) examined the effects of a preoperative psycho-educational training program on postoperative anxiety levels of Egyptian patients with UD. The intervention group received a 30–60 minute educational intervention one to two days preoperatively. The intervention included a visit from a peer with an ostomy, ostomy education, and time to express concerns and anxiety regarding the surgery. The intervention group’s anxiety decreased postoperatively on day 3 (p < 0.05) and at the time of discharge (p < 0.05).
These studies possess several limitations. Mohamed and Mohamed (2014) was published by a university hospital journal in Egypt, and the findings may not be generalizable. Findings from Ali and Khalil (1989) were also specific to Egyptian patients and may not be generalizable. The studies by Watson (1983) and Ali and Khalil (1989) were very small and about 30 years old. The three studies were limited in that they only included IC or did not specify the type of UD the participants had in the study. Although these studies discussed important information related to the current study, such as self-care and patient education, SE was not evaluated or discussed, which is an important focus.
Educational Interventions for Self-Efficacy and Self-Care in Other Populations
Studies of other populations targeting or evaluating SE exist, however, and have demonstrated improved SE or that SE has had a positive impact on the patient’s health status, including self-care and self-management (Chen, Sheu, Chang, Wang, & Huang, 2010; Dowse, Barford, & Browne, 2014).
Patients with fecal ostomies are very similar to those with incontinent UD in that they have had a major life-altering surgery on their intestines, with the need of an ostomy appliance. An educational intervention targeting Chinese patients with fecal ostomies, administered by expertly trained patients, significantly improved stoma-related knowledge total score (p = 0.00), stoma care SE total score (p = 0.00), stoma self-management total score (p = 0.003), and psychosocial adjustment total scores (p = 0.00) (Cheng, Xu, Dai, & Yang 2012).
Despite extensive review of the literature, only three studies were identified that evaluated interventions on patients after radical cystectomy with a UD, and none of them evaluated SE. No studies included participants with a continent UD. This review of literature highlights a major knowledge gap related to patients with UD with respect to adaptation to life after surgery. Studies of other populations have demonstrated that educational interventions can have positive effects on SE and self-care without harm. Benefits of such programs should be further explored in patients with a UD.
Methods
A two-arm RCT was designed to assess the feasibility of a hospital-based, supplemental, multimethod educational intervention aimed at improving SE and self-care in patients with radical cystectomy with a UD. Institutional review board approval was obtained from Weill Cornell Medical College and Stony Brook University prior to the start of the study, and written informed consent was obtained from all participants.
A convenience sample, consisting of individuals diagnosed with bladder cancer scheduled for a radical cystectomy with a UD, were recruited through New York Presbyterian Hospital/Weill Cornell Medical College in New York. Inclusion criteria were being aged 50 years or older, speak English, and have a histologically proven diagnosis of bladder cancer. Those with conditions preventing self-care, including severe cognitive impairment, were not eligible for participation in the study. All participants were screened for severe cognitive impairment using the six-item cognitive impairment test from Brooke and Bullock (1999). The tool has a sensitivity of 92.1% and a specificity of 95.6% for detecting dementia (Long, Shapiro, & Leung, 2012). Scores greater than 8 may be suggestive of dementia.
Investigators identified and offered eligible individuals participation in the study during preadmission testing or in the preoperative holding area.
Intervention
A multimethod educational intervention was developed for each of the three different UDs and included (a) a simplified medical illustration of participant-specific UD, (b) a step-by-step UD self-care instructional video, and (c) a pictorial Microsoft PowerPoint®. The content was driven by Bandura’s (1977) four sources of SE and were based on first-hand observed difficulties experienced by patients with a UD. The main focus of the educational intervention was management of the UD-specific tubes for continent UD and urostomy appliance management for incontinent UD. The National Action Plan to Improve Health Literacy (U.S. Department of Health and Human Services, 2010) recommends simplified illustrations, pictorial guides, and videos as methods of delivering health information to patients; these recommendations guided the development of the multimethod educational program. The video, PowerPoint, illustrations, and surveys were administered at the bedside by one of the investigators using a tablet computer. The intervention was enhanced by professional demonstration, followed by a chance for return demonstration. The intervention was designed as one hour in duration, with an optional 30 minutes for participant questions, and was delivered on postoperative day 4, 5, or 6.
Measures
Patient demographic data were captured electronically and included age, gender, bladder cancer diagnosis, highest year of education, and type of UD.
SE was measured using the six-item Self-Efficacy to Manage Chronic Disease (SES6G) scale (Stanford Patient Education Research Center, n.d.). High internal consistency was demonstrated by Cronbach alphas ranging from 0.8–0.95 (Ritter & Lorig, 2014). The scale consists of six questions regarding SE. Answers range from 1 (not at all confident in performing behavior) to 10 (totally confident) on a Likert-type scale. The mean of the six answers is the SE score; the higher the score, the better the SE. The SES6G was used because it provided a general assessment of SE and no validated SE scale exists for patients with a UD. The SES6G can be found at http://patienteducation.stanford.edu/research/secd6.html. An exploratory question regarding UD SE was created and labeled exploratory SE (ESE) in an effort to gain important insight regarding SE in the context of UD self-care that was not covered by the SES6G or any other currently available SE scales. One of two possible questions were asked depending on whether the participant had a continent or incontinent UD. The questions were specific to SE related to self-care skills commonly performed by the participants.
• Continent UD: (ONB or CCD) How confident are you that you will be able to irrigate/flush your UD and manage your tubes?
• Incontinent UD: (IC) How confident are you that you will be able to change your ostomy bag and wafer?
The self-care skills of participants with a CCD and ONB are similar; therefore, they received the same ESE question for simplicity.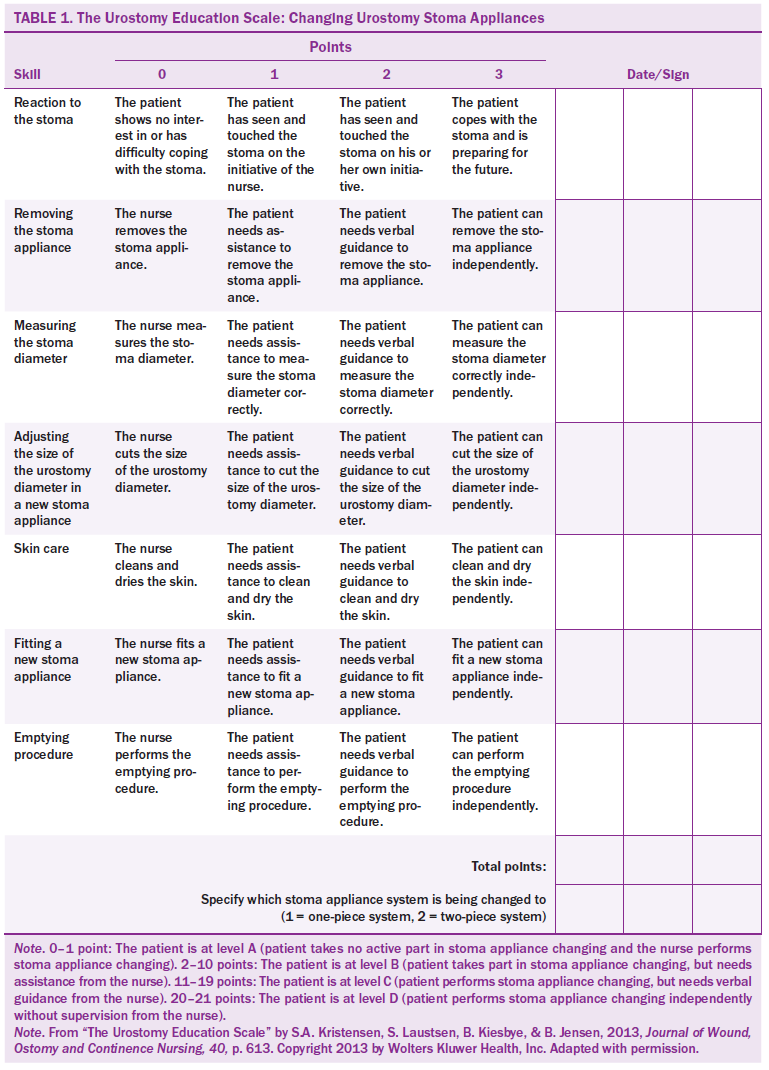
The Urostomy Education Scale (UES) was used to evaluate feasibility and self-care skills of study participants with an IC UD (Jensen, de Blok, Kiesbye, & Kristensen, 2013; Kristensen, Laustsen, Kiesbye, & Jensen, 2013). The UES evaluates seven different skills; the answers range from 0–3 points. The cumulative score ranges from 0–21; the higher the points, the more skilled and independent the participant is at self-care. The tool was tested and validated by Kristensen et al. (2013). Content validity through the modified Delphi technique found the scale to be exhaustive and exclusive (Kristensen et al., 2013). Written permission was obtained to use this tool. No tool exists for evaluating self-care skills of patients with a continent UD in the postoperative period. Therefore, an exploratory continent UD scale (ECUDS) was developed in an effort to gain additional important insight into self-care skills in the context of a continent UD. The ECUDS included similar grading system and was modeled after the UES to maintain homogeneity of the grades among the three UD groups. The UES is demonstrated in Table 1 and the ECUDS in Figure 5.
Procedures
Each participant’s demographic information was recorded preoperatively. Participants were randomized to the control group or the intervention group; subsequent participants received alternating assignments to the study arms using a running list of the consecutive dates/times of the office appointments. The SES6G scale and the ESE question were administered to all participants.
Standard-of-care UD instructions occurred on or around postoperative day 3 or 4. Standard of care for self-care instruction was clinician demonstration followed by patient return demonstration. In addition, the wound ostomy and continence nurse (WOCN) visited all patients with incontinent UDs. After the standard-of-care educational session, outcomes were measured for the control group with the SES6G scale and the ESE question. The UES or ECUDS scores were then recorded, which provided evidence of self-care independence, as well as intervention feasibility.
In addition to standard of care, trained nurse practitioners administered the multimethod educational intervention to the intervention group on postoperative day 4, 5, or 6 on the inpatient hospital unit. Outcomes were measured for all participants using the SES6G scale and the ESE question related to UD. The UES scores or the ECUDS scores provided evidence intervention feasibility and explored self-care independence.
Data Analysis
All data and surveys were collected and managed using Research Electronic Data Capture (REDCap) electronic data capture tools hosted at Weil Cornell Medical Center (Harris et al., 2009). REDCap is a secure, web-based application designed to support data capture for research studies.
Although pilot studies are not specifically designed for hypothesis testing, statistical analyses were performed using SPSS®, version 22.0. Descriptive statistics were used to analyze the demographic data. The Wilcoxon rank sum test was used to assess to differences in SE between intervention and the control groups. All p values were two-tailed, using an alpha level of 0.05. As a secondary endpoint, the results of the UES or ECUDS scores were analyzed. Fisher’s exact test was used to explore the relationship between the intervention and the outcome of self-care independence.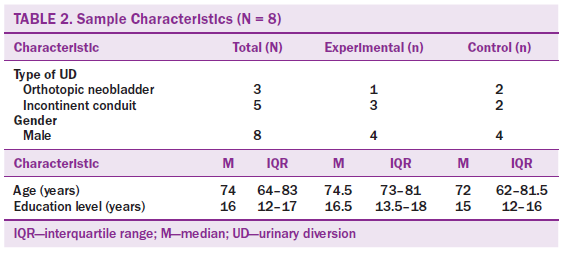
Results
A total of 10 participants with a reported diagnosis of bladder cancer met inclusion criteria; two did not meet inclusion criteria and were excluded because they did not speak English (see Table 2). The median score for the six-item cognitive impairment test was 4 (interquartile range = 0–5), suggesting the participants did not have severe cognitive impairment. Data were analyzed for between-group comparisons related to SE and self-care outcomes and are displayed in Table 3. The intervention arm was not found to be associated with self-care independence (p = 0.4286). In the entire sample, only two of the participants from the control group were independent with self-care skills. There was no evidence of a change in pre- versus post-SES6G score in the intervention group (p = 0.125). Because of sample size limitations, a paired test on the participants with continent UD in the intervention group was not possible. No evidence of a change was noted in the ESE question scores in the continent UD control group or the incontinent UD intervention group (p = 0.5 for both associations). No evidence of change was noted in the ESE question among the participants with incontinent patients in the control group (p = 0.5).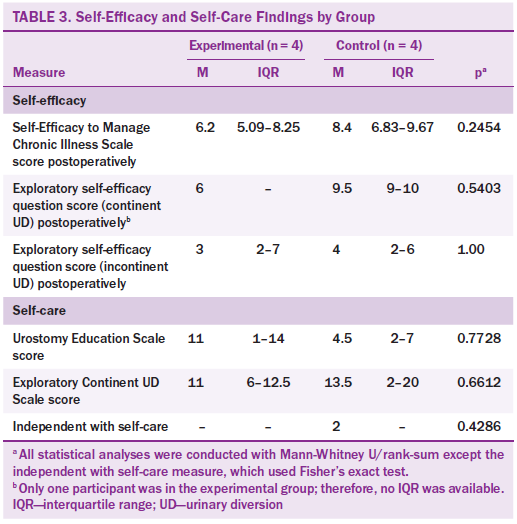
Discussion
The sample size for this pilot study is far too small to draw any statistics-based conclusions or inferences. The sample consisted mainly of well-educated, older adult men, and lacked a substantial number of patients in the CCD category. No association was found between intervention and control groups or within the intervention groups with respect to SE or self-care; in other words, the intervention did not have a significant effect on SE or self-care of this very small sample. No statistically significant associations were noted between the intervention and independence with self-care skills. There was a distinct lack of self-care independence, with only two participants in the entire sample independent with self-care skills. Those who were independent with self-care skills were found in the control group and represented the youngest participants in the group (younger than age 65 years). Although the current sample size is small and not powered for hypothesis testing, a strong data analysis plan exists.
Feasibility and Acceptability
One of the main purposes for a pilot study is to assess the feasibility of a larger study and acceptability of the study by the participants. No direct measure of feasibility was employed; however, enrollment and retention represents one alternate way of measuring feasibility. During the study period, eight patients met inclusion criteria. Two participants were not included because they did not speak English. Of the eight remaining patients, all were enrolled and completed the study. The study and interventions were highly accessible by participants because they were in the hospital and additional appointments or travel arrangements were not required. All participants completed all of the instruments, further demonstrating feasibility and acceptability. No problems were noted with the intervention implementation. All interventions were delivered on time except for one, which was delivered on postoperative day 10 instead of day 4, 5, or 6 at the request of the participant. The intervention could easily be integrated into standard of care at minimal cost as a CD-ROM or web-based program available at any time for patient use. No problems were noted with administration of the intervention and data collection with a tablet computer using REDCap and over a secured network. High enrollment, retention, and completion of all study interventions by participants demonstrates that a larger intervention of this type is acceptable and feasible (see Table 4).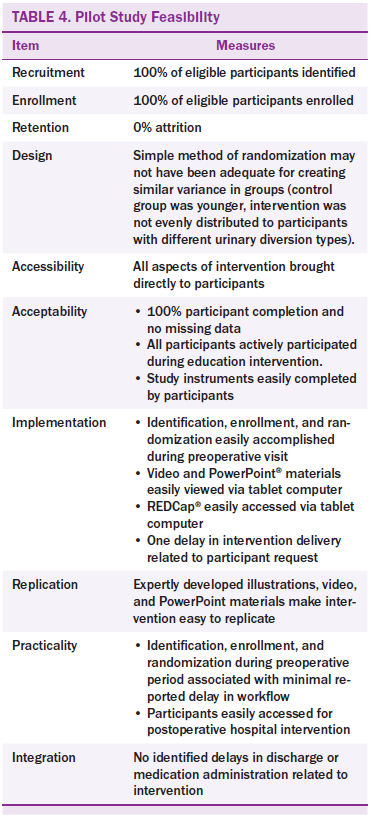
Limitations
There were multiple limitations to this study. The small sample size is the most obvious limitation; however, pilot studies are generally not intended for hypothesis testing (Leon, Davis, & Kraemer, 2011). The study duration was relatively short at four months. The study was investigator-administered, and interventions were not blinded. The self-report nature of the SE scales is a limitation. Race was not recorded, further limiting generalizability. No women were enrolled in the study, which could be explained by the relatively short duration of the study and the higher rates of bladder cancer among men (American Cancer Society, 2014). Lack of a program evaluation tool and participant input on intervention development may have limited the efficacy of the intervention. Lack of a validated continent UD self-care skills evaluation tool and validated SE scale for patients with UD were further limitations; however, one of the functions of a pilot study is refinement of study tools (Leon et al., 2011). Despite the limitations, the primary goal of feasibility was demonstrated with eight participants in a four-month period. All of the participants completed the study, and the tools captured all the information that was needed. Development and validation of new tools that measure SE and self-care skills will strengthen future studies.
Implications for Nursing Practice
Studies are lacking on interventions aimed at improving adaptation to life after radical cystectomy with a UD. Interventions that aim to improve SE may lead to improved self-care. If individuals feel that they can complete the necessary skills required for self-care and are able to successfully perform those skills, there will be improved adaptation to life after radical cystectomy with a UD. This pilot study demonstrates that a larger study is feasible and acceptable.
Although the study was not powered for hypothesis testing, a finding that would benefit from further study was that, even with an intense multimethod educational intervention, a lack of self-care independence was noted by the time of discharge. The only two participants independent with self-care were the youngest participants in the study; this would also be of interest for further research.
Future studies may benefit from including the preoperative period and the early discharge period at the patient’s home as an additional focus of interventions and support. Delayed intervention to one of the participants highlights that, even at postoperative day 4, some patients are not ready for education. Researchers could also assess the participants’ dexterity and ability to perform UD-related skills on a mannequin in the preoperative period.
Families and support networks should be identified and offered UD care instructions and information following radical cystectomy with UD (see Table 5). They should be offered an opportunity to participate in a larger study and give feedback. A larger study during a longer period of time would allow for recruitment of all three types of patients with UD, and allow for a more diverse sample.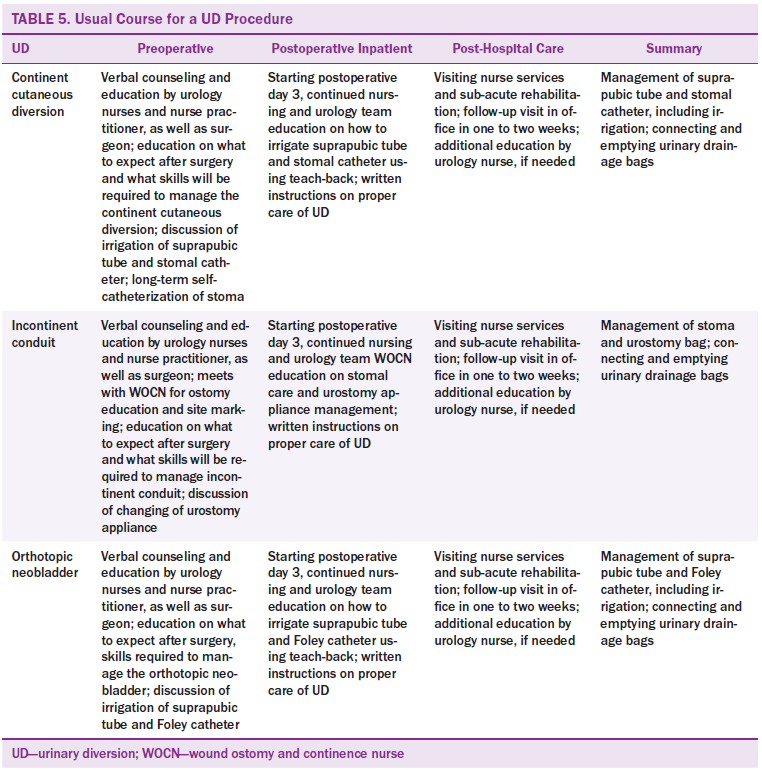
An SE scale should be developed and validated for patients with a UD. Development of a validated tool for evaluating continent UD irrigation skills in the postoperative period is also needed.
The groundwork for a larger, multi-institutional study has been laid. The authors have demonstrated that a larger study is feasible and necessary. Limitations of the study have been clearly delineated. Areas of the study that should be expanded on have been identified, such as a postoperative outpatient education component, where trained experts visit the participant’s home to reinforce self-care education. SE and self-care scales for patients with a UD have been created and will provide the groundwork for future development of validated scales. Variables, such as age, have been identified as areas that need more attention in a larger study. This is the first study of its kind that attempted to capture all three types of UDs to allow a more streamlined approach to patient education and maximizing the resources available to them.
Conclusion
Patients with a UD are an understudied, predominantly older adult population of cancer survivors that have tremendous needs following surgery. A hospital-based, supplemental, multimethod education intervention aimed at improving SE and self-care represents a possible method to educate patients and families. Its use in larger studies is warranted. A need exists for ongoing postdischarge support and education in this population.
The authors gratefully acknowledge Annie Rohan, PhD, RN, NNP-BC, CPNP-PC, FAANP, for her support and mentorship and Vanessa Dudley for her illustrations.
About the Author(s)
Merandy was, at the time of this writing, a DNP student and Jonas Nurse Scholar at Stony Brook University in New York; and Morgan is a nurse practitioner, Lee is an assistant professor, and Scherr is a professor and the clinical director of urologic oncology, all in the Department of Urology at New York Presbyterian Hospital/Weill Cornell Medical College in New York, NY. This research was supported, in part, by a grant (UL1 TR000457-06) from the Weill Cornell Medical College Clinical and Translational Science Center. Merandy, Morgan, and Lee completed the data collection. Merandy and Lee provided statistical support and the analysis. All of the authors contributed to the conceptualization and design and the manuscript preparation. Merandy can be reached at kym9003@nyp.org, with copy to editor at ONFEditor@ons.org. Submitted July 2016. Accepted for publication September 20, 2016.
References
Aghazadeh, M.A., Barocas, D.A., Salem, S., Clark, P.E., Cookson, M.S., Davis, R., . . . Chang, S.S. (2011). Determining factors for hospital discharge status after radical cystectomy in a large contemporary cohort. Journal of Urology, 185, 85–89. doi:10.1016/j.juro.2010.08.016
Ali, N.S., & Khalil, H.Z. (1989). Effect of psychoeducational intervention on anxiety among Egyptian bladder cancer patients. Cancer Nursing, 12, 236–242.
American Cancer Society. (2014). Cancer treatment and survivorship facts and figures, 2014–2015. Retrieved from http://www.cancer.org/acs/groups/content/@research/documents/document/a…
Bandura, A. (1977). Self-efficacy: Toward a unifying theory of behavioral change. Psychological Review, 84, 191–215.
Bandura, A. (1997). Self-efficacy: The exercise of control. New York, NY: Freeman.
Brooke, P., & Bullock, R. (1999). Validation of a 6 item cognitive impairment test with a view to primary care usage. International Journal of Geriatric Psychiatry, 14, 936–940.
Chen, S.Y., Sheu, S., Chang, C.S., Wang, T.H., & Huang, M.S. (2010). The effects of the self-efficacy method on adult asthmatic patient self-care behavior. Journal of Nursing Research, 18, 266–274. doi:10.1097/NRJ.0b013e3181fbe33f
Cheng, F., Xu, Q., Dai, X.D., & Yang, L.L. (2012). Evaluation of the expert patient program in a Chinese population with permanent colostomy. Cancer Nursing, 35, E27–E33. doi:10.1097/NCC.0b013e318217cbe9
Chou, R., Selph, S.S., Buckley, D.I., Gustafson, K.S., Griffin, J.C., Grusing, S.E., & Gore, J.L. (2016). Treatment of muscle-invasive bladder cancer: A systematic review. Cancer, 122, 842–851. doi:10.1002/cncr.29843
Dowse, R., Barford, K., & Browne, S.H. (2014). Simple, illustrated medicines information improves ARV knowledge and patient self-efficacy in limited literacy South African HIV patients. AIDS Care, 26, 1400–1406. doi:10.1080/09540121.2014.931559
Harris, P.A., Taylor, R., Thielke, R., Payne, J., Gonzalez, N., & Conde, J.G. (2009). Research electronic data capture (REDCap)—A metadata-driven methodology and workflow process for providing translational research informatics support. Journal of Biomedical Informatics, 42, 377–381. doi:10.1016/j.jbi.2008.08.010
Jensen, B.T., de Blok, W., Kiesbye, B., & Kristensen, S.A. (2013). Validation of the urostomy education scale: The European experience. Urologic Nursing, 33, 219–229.
Kristensen, S. A., Laustsen, S., Kiesbye, B., & Jensen, B.T. (2013). The Urostomy Education Scale: A reliable and valid tool to evaluate urostomy self-care skills among cystectomy patients. Journal of Wound, Ostomy, and Continence Nursing, 40, 611–617. doi:10.1097/01.WON.0000436778.39349.12
Lee, R.K., Abol-Enein, H., Artibani, W., Bochner, B., Dalbagni, G., Daneshmand, S., . . . Shariat, S.F. (2014). Urinary diversion after radical cystectomy for bladder cancer: Options, patient selection, and outcomes. BJU International, 113, 11–23. doi:10.1111/bju.12121
Leon, A.C., Davis, L.L., & Kraemer, H.C. (2011). The role and interpretation of pilot studies in clinical research. Journal of Psychiatric Research, 45, 626–629. doi:10.1016/j.jpsychires.2010.10.008
Long, L.S., Shapiro, W.A., & Leung, J.M. (2012). A brief review of practical preoperative cognitive screening tools. Canadian Journal of Anaesthesia, 59, 798–804. doi:10.1007/s12630-012-9737-1
Mohamed, N.E., Chaoprang Herrera, P., Hudson, S., Revenson, T.A., Lee, C.T., Quale, D.Z., . . . Diefenbach, M.A. (2014). Muscle invasive bladder cancer: Examining survivor burden and unmet needs. Journal of Urology, 191, 48–53. doi:10.1016/j.juro.2013.07.062
Mohamed, N.E., Diefenbach, M.A., Goltz, H.H., Lee, C.T., Latini, D., Kowalkowski, M., . . . Hall, S.J. (2012). Muscle invasive bladder cancer: From diagnosis to survivorship. Advances in Urology, 2012, 142135. doi:10.1155/2012/142135
Mohamed, N.M., & Mohamed, Z.A. (2014). Impact of self-care instructional program on urostomy patients’ outcome. Medical Journal of Cairo. Retrieved from http://medicaljournalofcairouniversity.net/home2/images/pdf/2014/Decemb…
National Cancer Institute. (2017). Bladder cancer treatment (PDQ®)—Health professional version. Retrieved from https://www.cancer.gov/types/bladder/hp/bladder-treatment-pdq
Ritter, P.L., & Lorig, K. (2014). The English and Spanish Self-Efficacy to Manage Chronic Disease scale measures were validated using multiple studies. Journal of Clinical Epidemiology, 67, 1265–1273. doi:10.1016/j.jclinepi.2014.06.009
Siegel, R.L., Miller, K.D., & Jemal, A. (2017). Cancer statistics, 2017. CA: A Cancer Journal for Clinicians, 67, 7–30. doi:10.3322/caac.21387
Stanford Patient Education Research Center. (n.d.). Self-efficacy for managing chronic disease 6-item scale. Retrieved from http://patienteducation.stanford.edu/research/secd6.pdf
U.S. Department of Health and Human Services. (2010). National action plan to improve health literacy. Retrieved from https://health.gov/communication/initiatives/health-literacy-action-pla…
Watson, P.G. (1983). The effects of short-term postoperative counseling on cancer/ostomy patients. Cancer Nursing, 6, 21–26.

