Optimism, Symptom Distress, Illness Appraisal, and Coping in Patients With Advanced-Stage Cancer Diagnoses Undergoing Chemotherapy Treatment
Purpose/Objectives: To explore the relationships between optimism, self-efficacy, symptom distress, treatment complexity, illness appraisal, coping, and mood disturbance in patients with advanced-stage cancer.
Design: Cross-sectional study.
Setting: Smilow Cancer Hospital at Yale New Haven in Connecticut, an outpatient comprehensive cancer center.
Sample: A convenience sample of 121 adult patients with stages III–IV cancer undergoing active chemotherapy.
Methods: Participants completed common self-report questionnaires to measure variables. Treatment hours and visits were calculated from data retrieved from medical record review. Mediation and path analysis were conducted to identify direct and indirect pathways from the significant antecedent variables to mood disturbance.
Main Research Variables: Dispositional optimism, self-efficacy, social support, treatment complexity, symptom distress, illness appraisal, coping, and mood disturbance.
Findings: Greater optimism and self-efficacy were associated with less negative illness appraisal, less avoidant coping, and decreased mood disturbance. Conversely, greater symptom distress was associated with greater negative illness appraisal, greater avoidant coping, and greater mood disturbance. In the final model, optimism and symptom distress had direct and indirect effects on mood disturbance. Indirect effects were partially mediated by illness appraisal.
Conclusions: Mood disturbance resulted from an interaction of disease stressors, personal resources, and cognitive appraisal of illness. Avoidant coping was associated with greater disturbed mood, but neither avoidant nor active coping had a significant effect on mood in the multivariate model.
Implications for Nursing: Illness appraisal, coping style, and symptom distress are important targets for intervention. Optimism is a beneficial trait and should be included, along with coping style, in comprehensive nursing assessments of patients with cancer.
Jump to a section
Major advances in the science of cancer treatment during the past two decades have changed the trajectory of disease and improved survival for patients diagnosed with advanced-stage cancer (Haylock, 2010; Institute of Medicine, 2006). However, compared to individuals with early-stage cancer who experience treatment-free survival, life with stage III or IV cancer is often one of interminable treatment. In addition, cancer treatment regimens are of varying complexity, which may involve lengthy infusions and frequent outpatient visits for chemotherapy treatment and supportive care (Cusack, Jones-Wells, & Chisholm, 2004; Sumpio, Knobf, & Jeon, 2016). The prolonged treatment trajectory can be viewed as a significant stressor, which may influence a person’s coping ability. Personal characteristics, such as optimism and self-efficacy, have been shown to predict positive psychological and physical outcomes (Aspinwall & MacNamara, 2005; Carver et al., 2005; Collie et al., 2005; Von Ah & Kang, 2007). Those with an optimistic disposition are also more likely to use adaptive coping strategies (Schou, Ekeberg, & Ruland, 2005). Although substantial research on stress and coping in women with breast cancer exists, less research has focused on patients with non-breast and advanced-stage cancers. The purpose of this study was to explore personal characteristics, illness stressors, and coping strategies in individuals with advanced cancer to identify how they cope in the current era of complex cancer treatment.
Stress-Coping Model and Cancer
The diagnosis of advanced stage cancer is a life-threatening condition and, combined with treatment, poses obvious significant stress. Lazarus and Folkman’s (1984) transactional model of stress and coping provides a framework for understanding how individuals with advanced cancer cope with adversity (Lazarus, 1990). Stress is conceptualized as a relationship between a person and the environment, which is appraised as taxing personal resources and threatening one’s well-being. The theory posits that one’s life goals, experiences, confidences, and personality dispositions are key antecedent variables that influence stress appraisal. Cognitive appraisal is based on a person’s evaluation of what is at stake, taking into consideration their personality characteristics, social support, and coping resources to determine how best to manage the stressor. Cognitive appraisal and coping are identified as critical mediators of the stressful person–environment transaction.
Two personal characteristics identified as positive resources in stressful situations are dispositional optimism and self-efficacy. Dispositional optimism is a stable personality trait, typified by an overall life orientation that outcomes in one’s future will be generally positive (Scheier & Carver, 1985). This belief keeps optimists engaged in activities in ways that seek to overcome obstacles and attain life goals. The theory posits that differences between optimists and pessimists may account for differences in coping style as well. Even with cancer, an optimistic disposition engenders adaptive coping behaviors, which yields a more positive mood (Carver et al., 1993). Self-efficacy is another important personal characteristic theorized to mitigate stress. According to social cognitive theory, self-efficacy is the “belief in one’s capabilities to organize and execute the courses of action required to produce given attainments” (Bandura, 1997, p. 3). Self-efficacy is influenced by one’s accomplishments and vicarious experiences and is considered a situational belief (van der Bijl & Shortbridge-Baggett, 2001).
The stress-coping model has been widely tested in patients with breast and prostate cancers (Kershaw et al., 2008; Northouse et al., 1999, 2002; Northouse, Kershaw, Mood, & Schafenacker, 2005). In women with breast cancer, significant relationships were found among optimism, family support, appraisal, and quality of life (QOL), and illness appraisal partially mediated the effects of symptom distress and family support on mood (Northouse et al., 1999). In women with recurrent breast cancer (Northouse et al., 2002), those with higher self-efficacy reported less hopelessness, less negative illness appraisal, and higher QOL. Self-efficacy had a direct effect on mental QOL and a mediated effect on QOL through illness appraisal. Patients with prostate cancer who were less efficacious, were younger, had more symptoms, had more advanced disease, and had more current concerns had more negative illness appraisal (Kershaw et al., 2008). Self-efficacy had an indirect effect on mental QOL that was mediated by illness appraisal (Kershaw et al., 2008).
Friedman et al. (2006) also found that optimistic women with breast cancer reported better overall QOL, less cancer-specific distress, and less mood disturbance than pessimistic women. Von Ah and Kang (2007) explored the effects of optimism, illness appraisal, and mood disturbance on women undergoing adjuvant chemotherapy for breast cancer. Optimism was directly related to mood disturbance after adjuvant therapy, but illness appraisal did not mediate the relationship between optimism and mood disturbance. In individuals with colon cancer, optimism, cancer threat appraisal, and social support were significantly associated with psychological distress and predicted distress at 12 months (Lynch, Steginga, Hawkes, Pakenham, & Dunn, 2008).
The results of coping studies have been mixed. A study by Carver et al. (1993) found that optimism was positively correlated with active coping style and planning style preoperatively, and negatively correlated to avoidant coping, denial, and behavioral disengagement styles. The coping styles of acceptance and denial mediated the effect of optimism on mood distress pre- and postoperatively. However, active coping style was not associated with lower levels of distress. Schou et al. (2005) reported that women with breast cancer who were optimists responded with a fighting spirit coping style, which was associated with better global QOL and functioning, whereas pessimists responded with helpless/hopeless coping and experienced worse global QOL. In the aforementioned study, patients with prostate cancer who had more negative illness appraisal used more active coping at four months and more avoidant coping at eight months (Kershaw et al., 2008). Active and avoidant coping had a significant direct effect on QOL.
The varied findings in these studies warrant rethinking the model and its variables, particularly in the face of changing survival and treatment paradigms in advanced-stage disease. A trend toward increasing complexity has implications for the stressed patient’s experience. Sumpio et al. (2016) described varying complexity in the hours spent in treatment and the type of visits participants encountered. Individuals who were younger, female, and with colon and esophageal diagnoses had significantly longer chemotherapy treatment visits. Participants with lung cancer and women spent more hours in visits for supportive care. From the patient’s viewpoint, treatment complexity represents the physical effort required to undergo treatment and may be a potential stressor in advanced-stage disease. Illness appraisal, in addition to confidence about managing treatment, may be influenced by the particular regimen’s complexity relative to its benefit.
In summary, review of stress-coping studies in patients with cancer reveals that not all models included the same personal resource variables or illness appraisal, in addition to coping, as mediators. Inconsistent findings and gaps still exist in the understanding of theorized relationships. Although increasing attention has been paid to cancer diagnoses other than breast cancer, fewer studies have included patients with pancreatic and lung cancers. The influence of modern treatment complexity has not been studied. For patients with advanced-stage cancer, exploring the relationship of optimism, self-efficacy, symptom distress, and treatment complexity with illness appraisal, coping, and mood disturbance will contribute to the understanding of the experience of this paradigm shift in the trajectory of advanced cancer.
Methods
A descriptive cross-sectional design was used. Participants were recruited from the outpatient treatment center of Smilow Cancer Hospital at Yale New Haven in Connecticut, a National Cancer Institute–designated comprehensive cancer center. Potential participants were first identified by the oncologist and asked if they were willing to speak to the nurse researcher. If the patient agreed, the nurse researcher explained the study and obtained informed consent for those willing to participate. The institution’s human subjects committee approved the study. Of 137 potential participants, 121 consented to participate (enrollment rate of 88%). All participants met the following inclusion criteria: aged 21 years or older, had stage III or IV cancer, were currently receiving chemotherapy and had continually received chemotherapy for three months prior to study enrollment, could speak and read English, and did not have any condition that precluded cognitive understanding of the study’s questionnaires.
Instruments
Optimism: The 10-item Life Orientation Test–Revised (LOT-R) (Scheier, Carver, & Bridges, 1994) was used to measure dispositional optimism. Of the 10 items, 3 measure optimism, 3 measure pessimism, and 4 serve as fillers. Items are scored on a five-point scale from 1 (strongly disagree) to 5 (strongly agree). Possible range of scores is 6–30. LOT-R is a well-validated tool with established population-based norms (Glasemer et al., 2012). The LOT-R has internal consistency of alpha ranging from 0.74–0.78 (Scheier et al., 1994; Schou et al., 2005). In this study, reliability coefficient was 0.77.
Self-efficacy: The Cancer Behavior Inventory–Brief Form (CBI-B) (Merluzzi, Nairn, & Martinez-Sanchez, 1999) measures self-efficacy for coping with cancer. The original tool has 14 items, measuring seven key coping domains (2 items each): maintaining activity and independence, coping with treatment-related side effects, accepting cancer, seeking and understanding medical information, affective regulation, seeking support, and stress management for medical appointments. Item responses range from 1 (not at all confident) to 9 (totally confident). In this study, a total score for self-efficacy was used, calculated as the sum of all 14 items (range = 14–126). The tool has established internal consistency reliability (alpha = 0.85) (Merluzzi et al., 1999). Alpha reliability coefficient in this study was 0.81.
Social support: The Social Support Questionnaire (SSQ) (Sarason, Levine, Basham, & Sarason, 1983) is a 12-item measure that assesses two dimensions of support: number of people available for provision of support and satisfaction with available support. Responses range from 1 (very dissatisfied) to 6 (very satisfied). The internal consistency of the tool has been reported as an alpha of 0.96 (Friedman et al., 2006). In this study, alpha reliability coefficient was 0.94.
Symptom distress: M.D. Anderson Symptom Inventory (MDASI) (Cleeland et al., 2000) is a widely used tool that assesses symptom severity and symptom interference with daily life. In this study, only the symptom severity scale was used. The symptom severity scale is comprised of 13 core symptoms: pain, fatigue, nausea, sleep disturbance, distress (being upset), shortness of breath, remembering things, lack of appetite, dry mouth, feeling drowsy, feeling sad, vomiting, and numbness or tingling. Participants rate their symptoms on a scale from 0–10, with higher scores indicating worse symptom distress. Internal consistency reliability for the scale is high (alpha = 0.87–0.89) (Cleeland et al., 2000; Hsu & Tu, 2014). In this study, alpha reliability coefficient was 0.87.
Treatment complexity: The number of treatment visits and total visit hours were calculated for each participant for a standardized period of three months just prior to and including the date of study consent. The time frame was selected so that participants experienced the treatment to reflect attitudes and beliefs about the treatment experience. Time required for each treatment-related visit was calculated and summed to obtain a continuous score for total hours. The total number of visits made for treatment was counted (Sumpio et al., 2016).
Illness appraisal: Appraisal was measured using the Appraisal of Illness Scale (Munkres, Oberst, & Hughes, 1992). The 27-item scale focuses on evaluation of resources, appraisal of loss, financial strain, and threat of illness. Higher scores indicate a more negative view of the illness. The tool has reported reliability as high as an alpha of 0.95 (Kershaw et al., 2008); in this study, alpha reliability coefficient was 0.89.
Coping: Coping was measured by the Brief COPE scale (Carver, 1997). As originally designed, the 28-item tool measures 14 coping strategies (i.e., self-distraction, active coping, denial, self-blame, seeking emotional support, seeking instrumental support, behavioral disengagement, venting, positive reframing, planning, use of humor, alcohol/drug use, acceptance, and religion). There is support for using a two-factor structure of active coping and avoidant coping (Carver, n.d.; Kershaw et al., 2008; Kershaw, Northouse, Kritpracha, Schaefenacker, & Mood, 2004). Alpha reliability coefficient was 0.85 for the active coping scale and 0.63 for the avoidant scale. The reliability of the avoidant scale was lower than the active scale in prior studies with patients with cancer (0.63–0.64) (Kershaw et al., 2004, 2008).
Mood disturbance: The Profile of Mood States–Short Form (POMS-SF) (Curran, Andrykowski, & Studts, 1995) was used to measure mood disturbance. The POMS-SF consists of a list of 37 adjectives rated on a five-point scale from 1 (not at all) to 5 (a lot), with an overall score calculated for total mood disturbance. The six affective dimensions measured are tension-anxiety, depression-dejection, anger-hostility, vigor-activity, fatigue-inertia, and concentration-confusion. Internal consistency estimates of the POMS scale range from alpha of 0.8–0.91. In this study, alpha reliability coefficient was 0.88.
Statistical Analysis
Descriptive analyses were conducted for demographic variables to determine the sample characteristics. All statistical analyses were performed using SAS®, version 9.3. All variables were standardized for a zero mean and a one standard deviation for mediation analysis. Bivariate analysis using Pearson correlation was conducted to determine required relationships between variables. First, candidate mediators were selected based on significant Pearson correlations of each potential mediator (i.e., illness appraisal, active coping, and avoidant coping) with the outcome variable (i.e., mood disturbance). Then, each antecedent variable was examined to determine significant correlations with candidate mediators and mood disturbance. General linear models (GLMs) were performed to check for multicollinearity among antecedent variables. Variance inflation factor (VIF) and tolerance of each antecedent variable were checked, and any highly influencing variable was removed to keep VIFs acceptable for the remaining variables. Path-analysis was conducted using PROC CALIS with LINEQS in SAS. The model included all possible direct and indirect pathways from the antecedent variable to mood disturbance through the mediators and the correlation between the mediators. Model fit was examined using goodness of fit index, Bentler comparative fit index (CFI), and standardized root mean square (SRMR). Insignificant coefficients were removed to improve model fit (Hooper, Coughlin, & Mullen, 2008; Iacobucci, 2010). Point estimates and standard error of mediation effects were obtained from the final path-model.
The sample size of 121 was enough to detect a medium effect size (bivariate correlation of 0.3), with 92% power at a 5% significance level. Therefore, candidate antecedent variables having a medium correlation with mediators and mood disturbance would have enough chance to be selected for the final mediation model. For path analysis, a minimum sample size of 10 participants is recommended for every parameter estimated (Streiner, 2005). Because the final mediation model includes only five of nine variables explored, the sample size of 121 was acceptable for the path analysis.
Results
The study sample consisted of 121 adult participants, with nearly equal number of women and men (see Table 1). Age ranged from 31–85 years. The majority of participants were White, married, and diagnosed with colon, esophageal, lung, or pancreatobiliary cancer. Time since diagnosis was an average of 2.5 years (SD = 2.3 years), but that varied across diagnosis groups (1.2–5 years). 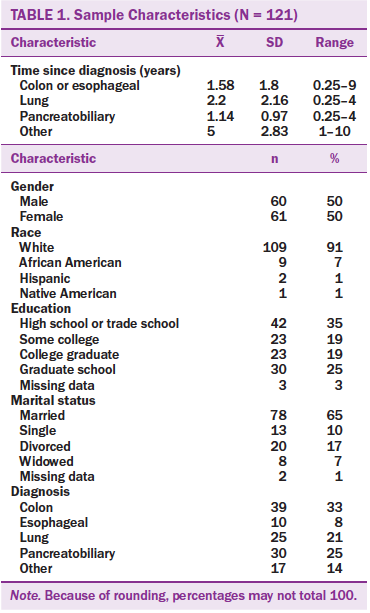
Relationships Among Variables
Pearson correlations between potential mediators and mood disturbance are shown in Table 2. Avoidant coping was positively associated with illness appraisal (r = 0.46) and active coping (r = 0.3). Mood disturbance had strong significant associations with illness appraisal (r = 0.56) and avoidant coping (r = 0.47), but not active coping. Based on the correlations, illness appraisal and avoidant coping were selected as candidate mediators. Because of the lack of association with mood disturbance, active coping did not meet the criteria for a mediator. 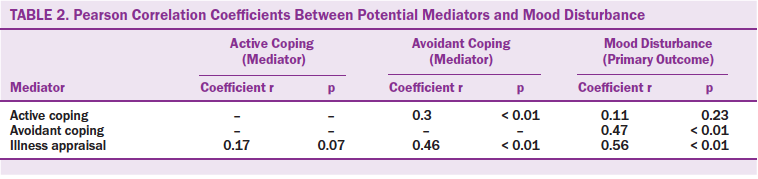
Table 3 shows correlations of all antecedent variables with the mediators and mood disturbance. For completeness of description, associations between antecedents and active coping are presented. Greater optimism and self-efficacy was associated with less negative appraisal of illness severity, less avoidant coping, and decreased mood disturbance. Conversely, greater symptom distress was associated with a greater negative appraisal of illness, greater avoidant coping, and greater mood disturbance. Optimism, self-efficacy, and symptom distress were not associated with active coping style. Older age was significantly associated with less avoidant coping (r = –0.27) and less mood disturbance (r = –0.22), but not with illness appraisal. Despite the significant associations of social support with illness appraisal and provider support with mood disturbance, these two variables were eliminated from the mediation analysis because of lack of correlations with mediators and mood disturbance. Total hours and visits were not significant correlates of any coping style or mood disturbance and, therefore, were also excluded from further analysis.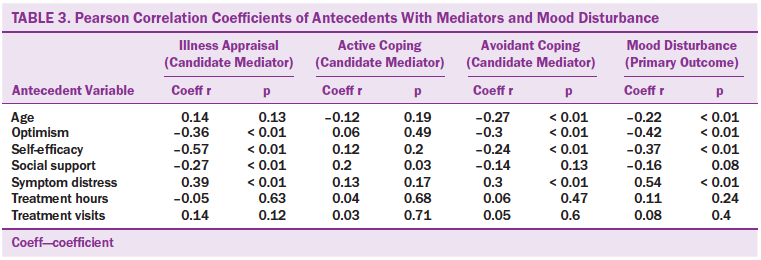
Three multivariate analyses (GLMs) predicting appraisal of illness, avoidant coping, and mood disturbance were conducted with optimism, self-efficacy, symptom distress, and age (see Table 4). Self-efficacy had highest VIF of 1.5 in all three models because of a high correlation with optimism (r = 0.51) and was not significantly associated with mood disturbance (p = 0.47) after controlling for the other antecedent variables. Therefore, self-efficacy was removed from the models to reduce multicollinearity and all other covariates had acceptable VIF around 1. In the GLMs with optimism, symptom distress, and age, all three had significant effects on illness appraisal and avoidant coping. However, age was not significantly associated with mood disturbance (p = 0.22) after controlling for optimism and symptom distress, which kept the significant associations. 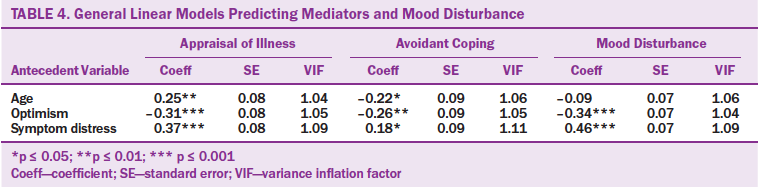
Path Analysis
Figure 1 shows estimated coefficients and standard errors of pathways from optimism and symptom distress to mood disturbance through illness appraisal and avoidant coping in the path-model. Although age was not tested for mediation effect, age was included in the path-model for a covariance; therefore, all estimated coefficients were adjusted for age. To increase the goodness of fit, the authors removed the insignificant correlation from avoidant coping to mood disturbance (coefficient = 0.12 [0.08], p = 0.13), resulting in acceptable model fit index scores, including goodness of fit of 0.99 (greater than 0.95 indicates good fit), SRMR of 0.02 (less than 0.05 indicates good fit), and CFI of 0.99 (greater than 0.95 indicates good fit) (Hooper et al., 2008). Significant indirect effects from optimism (–0.12 [0.04], p < 0.01) and symptom distress (0.15 [0.04]), p < 0.01) on mood disturbance by mediating illness appraisal were estimated from the model, whereas these two antecedent variables still had substantive direct effects on mood disturbance. 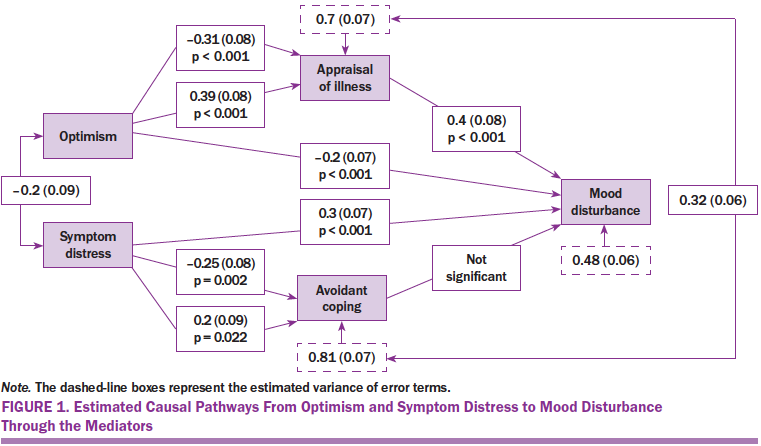
The results of the mediation and multivariate analysis were used to construct a final model. Optimism retained its significance in the path analysis and countered the negative effects of symptom distress and negative illness appraisal on mood. Optimism and symptom distress had direct and indirect effects on mood disturbance. Illness appraisal partially mediated the effects of optimism and symptom distress on mood. The expected theoretical association of optimism and active coping style was not found, and avoidant coping did not predict mood disturbance despite associations with optimism and symptom distress.
Discussion
In patients with advanced-stage cancer, optimism, symptom distress, and appraisal of illness severity play key roles in the transaction between stress and mood. As previously shown in patients with breast cancer (Carver et al., 1994; Friedman et al., 1996; Von Ah & Kang, 2007), the authors of the current study found that optimism awards benefit in terms of maintaining a more positive mood. The finding is particularly confirmatory in a sample inclusive of those with pancreatic and lung cancers. Even in the face of a life-threatening diagnosis, those with a more optimistic disposition have a generalized expectancy that they will continue to attain their life’s goals, and this belief drives behaviors and cognitions that help mitigate the stress of cancer (Rasmussen, Wrosch, Scheier, & Carver, 2006)
The study also confirms appraisal of illness’s role as a partial mediator of symptom distress and optimism on mood, comparable to the longitudinal study by Kershaw et al. (2008). Illness appraisal is particularly salient to those with advanced disease who face protracted treatment and uncertain survival. Given that advanced cancer is an ever-changing clinical scenario, cross-sectional evaluation of appraisal may be methodologically appropriate. Specifically, the effects found for illness appraisal can be thought of as reflecting the patient’s concurrent cognitive assessment of illness severity and whether they have the personal resources and capacity to cope.
The current study shows that, in advanced-stage disease, the stress-coping model is more parsimonious than expected. Social support was not found to provide the same benefit to the current sample as in previous studies (Hochhausen et al., 2007; Von Ah & Kang, 2007). That result may reflect the impact of symptom distress, which may be a tipping point upon which other beneficial resources, such as social support, become less effective in maintaining positive mood. Surprisingly, neither number of visits nor hours spent in treatment emerged as significant stressors. This indicates that the physical stresses of treatment may be less consequential to the individual compared with other illness factors, such as symptom distress. Alternatively, it may also mean that a person experiences less stress being under the watchful eyes of their treatment team, and, in advanced-stage disease, this surveillance is welcome.
The expected theoretical effects of coping style were only somewhat supported. The authors found that greater avoidant coping was associated with diminished optimism and self-efficacy and greater mood disturbance, but was not predictive of mood disturbance. In this respect, avoidant coping reflects a tactic used by a stressed patient overwhelmed by diagnosis and treatment, but it is not possible to conclude a causal relationship with mood. The current authors also found no positive impact of active coping, which theoretically is the mechanism by which optimistic patients experience improved outcomes. Although other studies have shown that patients with advanced cancer use active and avoidant coping styles, only avoidant coping predicted greater negative QOL or mood disturbance (Costanzo, Lutgendorf, Rothrock, & Anderson, 2006; Kershaw et al., 2004, 2008). With advanced-stage cancer, other coping styles, such as adjusting values and goals, positive reframing, and spiritual support, may more effectively balance mood (Thomsen, Rydahl-Hansen, & Wagner, 2010).
Limitations
Results from this convenience sample from one cancer center may not be generalizable to other samples. The study relied exclusively on self-report survey instruments. Although the instruments have established reliability and validity in cancer research, concerns exist about the mono-methodology of self-report (Donaldson & Grant-Vallone, 2002). In addition, the lower reliability of the avoidant coping scale is a limitation that needs further examination in future studies. The multicollinearity between optimism and self-efficacy created a statistical barrier to multivariate analysis, and the true effect of self-efficacy could not be evaluated as planned. Finally, the cross-sectional design may limit directional interpretation of the relationships.
Implications for Nursing
Findings of this study provide important implications for nursing research and practice. With improved screening and diagnostics, an initial diagnosis of stage III or IV cancer more likely represents pathological status, as opposed to widespread disease with dwindling function that characterized advanced, end-stage cancer in the past. Likewise, the standards for treating advanced-stage cancer have evolved. The course of treatment for many patients is one of aggressive first-line therapy, which, if it fails, is often followed by second-, third-, and fourth-line courses of chemotherapy (Sumpio et al., 2016). This study helps to clarify the understanding of factors relevant to coping with the reality of modern treatment.
Nurses in practice should be mindful of the impact of dispositional optimism and symptom distress on mood disturbance experienced during treatment. Although nurses are diligent in assessing pain and symptom distress, assessment of optimism is not standardized or common. The LOT-R is valuable for individual diagnosis (Glaesmer et al., 2012). For example, knowing that a person has a more pessimistic disposition provides insight to a trait that might place them at a greater risk of distress in the face of high symptom severity. Patients with less optimism may benefit from other supportive resources (e.g., counseling) to help them manage the stress of illness. Likewise, by assessing coping strategies, a nurse can tailor interventions to help those who rely on less effective avoidant coping strategies to identify more effective ways to cope with their illness. Tools assessing optimism and coping style should be included in the comprehensive assessment of all patients undergoing cancer treatment. As research has shown (Northouse et al., 2005, 2013), illness appraisal also remains an important target for intervention. In the fast-paced environment of treatment clinics, nurses may overlook evaluating a patient’s cognitions and fears. Asking patients what they think is going on with their treatment and providing clarifying information about symptoms can help patients differentiate disease progression from treatment side effects. For patients diagnosed with advanced-stage cancer, it may be difficult to achieve cure, but one can be taught to manage stressors more effectively.
Conclusion
This study explored stress and coping in patients with advanced-stage cancer undergoing active chemotherapy treatment. Mood resulted from a complex interaction of disease stressors, personal resources, and cognitive appraisal of illness. Patients who resort to avoidant coping when dealing with the realities of advanced-stage disease may be at greater risk for mood disturbance, but more research on coping style is needed. Such studies will enhance our knowledge of changes in appraisal and coping as survival trajectories lengthen.
About the Author(s)
Sumpio is an educator and quality coordinator at Smilow Cancer Hospital at Yale New Haven in Connecticut; Jeon is a research scientist in the School of Nursing at Yale University in West Haven, CT; Northouse is a professor emerita in the School of Nursing at the University of Michigan in Ann Arbor; and Knobf is a professor in the School of Nursing at Yale University. This research was funded by a Clinical and Translational Science Award grant (No. TL1 TR000141) from the National Center for Advancing Translation Science, a component of the National Institutes of Health. Sumpio, Northouse, and Knobf contributed to the conceptualization and design. Sumpio completed the data collection. Jeon provided statistical support. All of the authors provided the analysis and contributed to the manuscript preparation. Sumpio can be reached at catherine.sumpio@ynhh.org, with copy to editor at ONFEditor@ons.org. Submitted June 2016. Accepted for publication September 10, 2016.
References
Aspinwall, L.G., & MacNamara, A. (2005). Taking positive changes seriously. Cancer, 104, 2549–2556. doi:10.1002/cncr.21244
Bandura, A. (1997). Self-efficacy: The exercise of control. New York, NY: Freeman.
Carver, C.S. (1997). You want to measure coping but your protocol’s too long: Consider the Brief COPE. International Journal of Behavioral Medicine, 4, 92–100. doi:10.1207/s15327558ijbm0401_6
Carver, C.S. (n.d.). COPE (complete version). Retrieved from http://www.psy.miami.edu/faculty/ccarver/sclCOPEF.html
Carver, C.S., Pozo, C., Harris, S.D., Noriega, V., Scheier, M.F., Robinson, D.S., . . . Clark, K.C. (1993). How coping mediates the effect of optimism on distress: A study of women with early stage breast cancer. Journal of Personality and Social Psychology, 65, 375–390.
Carver, C.S., Pozo-Kaderman, C., Harris, S.D., Noriega, V., Scheier, M.F., Robinson, D.S., . . . Clark, K.C. (1994). Optimism versus pessimism predicts the quality of women’s adjustment to early stage breast cancer. Cancer, 73, 1213–1220.
Carver, C.S., Smith, R.G., Antoni, M.H., Petronis, V.M., Weiss, S., & Derhagopian, R.P. (2005). Optimistic personality and psychosocial well-being during treatment predict psychosocial well-being among long-term survivors of breast cancer. Health Psychology, 24, 508–516. doi:10.1037/0278-6133.24.5.508
Cleeland, C.S., Mendoza, T.R., Wang, X.S., Chou, C., Harle, M.T., Morrissey, M., & Engstrom, M.C. (2000). Assessing symptom distress in cancer: The M.D. Anderson Symptom Inventory. Cancer, 89, 1634–1646.
Collie, K., Wong, P., Tilston, J., Butler, L.D., Turner-Cobb, J., Kreshka, M.A., . . . Koopman, C. (2005). Self-efficacy, coping, and difficulties interacting with health care professionals among women living with breast cancer in rural communities. Psycho-Oncology, 14, 901–912. doi:10.1002/pon.944
Costanzo, E.S., Lutgendorf, S.K., Rothrock, N.E., & Anderson, B. (2006). Coping and quality of life among women extensively treated for gynecologic cancer. Psycho-Oncology, 15, 132–142. doi:10.1002/pon.930
Curran, S.L., Andrykowski, M.A., & Studts, J.L. (1995). Short Form of the Profile of Mood States (POMS-SF): Psychometric information. Psychological Assessment, 7, 80–83. doi:10.1037/1040-3590.7.1.80
Cusack, G., Jones-Wells, A., & Chisholm, L. (2004). Patient intensity in an ambulatory oncology research center: A step forward in the field of ambulatory cancer. Nursing Economics, 22, 58–63.
Donaldson, S.I., & Grant-Vallone, E.J. (2002). Understanding self-report bias in organizational behavior research. Journal of Business and Psychology, 17, 245–260. doi:10.1023/A:1019637632584
Friedman, L.C., Kalidas, M., Elledge, R., Chang, J., Romero, C., Husain, I., . . . Liscum, K.R. (2006). Optimism, social support and psychosocial functioning among women with breast cancer. Psycho-Oncology, 15, 595–603. doi:10.1002/pon.992
Glaesmer, H., Rief, W., Martin, A., Mewes, R., Brähler, E., Zenger, M., & Hinz, A. (2012). Psychometric properties and population-based norms of the Life Orientation Test-Revised (LOT-R). British Journal of Health Psychology, 17, 432–445. doi:10.1111/j.2044-8287.2011.02046.x
Haylock, P.J. (2010). Advanced cancer: Emergence of a new survivor population. Seminars in Oncology Nursing, 26, 144–150. doi:10.1016/j.soncn.2010.05.008
Hochhausen, N., Altmaier, E.M., McQuellon, R., Davies, S.M., Papadopolous, E., Carter, S., & Hensiee-Downey, J. (2007). Social support, optimism, and self-efficacy predict physical and emotional well-being after bone marrow transplantation. Journal of Psychosocial Oncology, 25, 87–101. doi:10.1300/J077v25n01_05
Hooper, D., Coughlin, J., & Mullen, M. (2008). Structural equation modeling: Guidelines for determining model fit. Electronic Journal for Business Research Methods, 6, 53–60.
Hsu, M.C., & Tu, C.H. (2014). Improving quality-of-life outcomes for patients with cancer through mediating effects of depressive symptoms and functional status: A three-path mediation model. Journal of Clinical Nursing, 23, 2461–2472. doi:10.1111/jocn.12399
Iacobucci, D. (2010). Structural equations modeling: Fit indices, sample size, and advanced topics. Journal of Consumer Psychology, 2, 90–98. doi:10.1016/j.jcps.2009.09.003
Institute of Medicine. (2006). From cancer patient to cancer survivor: Lost in transition. Washington, DC: National Academies Press.
Kershaw, T., Northouse, L., Kritpracha, C., Schaefenacker, A., & Mood, D. (2004). Coping strategies and quality of life in women with advanced breast cancer and their caregivers. Psychology and Health, 19, 139–155.
Kershaw, T.S., Mood, D.W., Newth, G., Ronis, D.L., Sanda, M.G., Vaishampayan, U., & Northouse, L.L. (2008). Longitudinal analysis of a model to predict quality of life in prostate cancer patients and their spouses. Annals of Behavioral Medicine, 36, 117–128. doi:10.1007/s12160-008-9058-3
Lazarus, R.S., & Folkman, S. (1984). Stress, appraisal, and coping. New York, NY: Springer.
Lazarus, R.S. (1990). Theory-based stress measurement. Psychological Inquiry, 1, 3–13.
Lynch, B.M., Steginga, S.K., Hawkes, A.L., Pakenham, K.L., & Dunn, J. (2008). Describing and predicting psychological distress after colon cancer. Cancer, 112, 1363–1370. doi:10.1002/cncr.23300
Merluzzi, T.V., Nairn, R.C., & Martinez-Sanchez, M.A. (1999). A manual for the Cancer Behavior Inventory: A measure of self-efficacy for coping with cancer. Retrieved from http://psychology.nd.edu/faculty/thomas-v-merluzzi
Munkres, A., Oberst, M.T., & Hughes, S.H. (1992). Appraisal of illness, symptom distress, self-care burden, and mood states in patients receiving chemotherapy for initial and recurrent cancer. Oncology Nursing Forum, 19, 1201–1209.
Northouse, L., Kershaw, T., Mood, D., & Schafenacker, A. (2005). Effects of a family intervention on the quality of life of women with recurrent breast cancer and their family caregivers. Psycho-Oncology, 14, 478–491. doi:10.1002/pon.871
Northouse, L.L., Caffey, M., Deichelbohrer, L., Schmidt, L., Guziatek-Trojniak, L., West, S., . . . Mood, D. (1999). The quality of life of African American women with breast cancer. Research in Nursing and Health, 22, 449–460.
Northouse, L.L., Mood, D., Kershaw, T., Schaefenacker, A., Mellon, S., Walker, J., . . . Decker, V. (2002). Quality of life of women with recurrent breast cancer and their families. Journal of Clinical Oncology, 20, 4050–4064. doi:10.1200/JCO.2002.02.054
Northouse, L.L., Mood, D.W., Schafenacker, A., Kalemkenan, G., Zalupski, M., LoRusso, P., . . . Kershaw, T. (2013). Randomized clinical trial of a brief and extensive dyadic intervention for advanced cancer patients and their family caregivers. Psycho-Oncology, 22, 555–563. doi:10.1002/pon.3036
Rasmussen, H.N., Wrosch, C., Scheier, M.F., & Carver, C.S. (2006). Self-regulation processes and health: The importance of optimism and goal adjustment. Journal of Personality, 74, 1722–1747. doi:10.1111/j.1467-6494.2006.00426.x
Sarason, I.G., Levine, H.M., Basham, R.B., & Sarason, B.R. (1983). Assessing social support: The Social Support Questionnaire. Journal of Personality and Social Psychology, 44, 127–139.
Scheier, M.F., & Carver, C.S. (1985). Optimism, coping, and health: Assessment and implications of generalized outcome expectations. Health Psychology, 4, 219–247.
Scheier, M.F., Carver, C.S., & Bridges, M.W. (1994). Distinguishing optimism from neuroticism (and trait anxiety, self-mastery, and self-esteem): A reevaluation of the Life Orientation Test. Journal of Personality and Social Psychology, 67, 1063–1078.
Schou, I., Ekeberg, Ø., & Ruland, C.M. (2005). The mediating role of appraisal and coping in the relationship between optimism-pessimism and quality of life. Psycho-Oncology, 14, 718–727. doi:10.1002/pon.896
Streiner, D.L. (2005). Finding our way: An introduction to path analysis. Canadian Journal of Psychiatry, 50, 115–122. doi:10.1177/070674370505000207
Sumpio, C., Knobf, M.T., & Jeon, S. (2016). Treatment complexity: A description of chemotherapy and supportive care treatment visits in patients with advanced-stage cancer diagnosis. Supportive Care in Cancer, 24, 298–293. doi:10.1007/s00520-015-2775-9
Thomsen, T.G., Rydahl-Hansen, S., & Wagner, L. (2010). A review of potential factors relevant to coping in patients with advanced cancer. Journal of Clinical Nursing, 19, 3410–3426. doi:10.1111/j.1365-2702.2009.03154.x
van der Bijl, J.J., & Shortbridge-Baggett, L.M. (2001). The theory and measurement of the self-efficacy construct. Scholarly Inquiry for Nursing Practice, 15, 189–207.
Von Ah, D., & Kang, D.H. (2007). Correlates of mood disturbance in women with breast cancer: Patterns over time. Journal of Advanced Nursing, 61, 676–689. doi:10.1111/j.1365-2648.2007.04563.x

