Complementary Medicine and the Role of Oncology Nurses in an Acute Care Hospital: The Gap Between Attitudes and Practice
Purpose/Objectives: To describe hospital nurses’ knowledge, attitudes, and practices regarding complementary medicine (CM); to compare the knowledge and attitudes of nurse managers to staff nurses with diverse oncology experience; and to assess attitudes toward integrating CM into the role of the hospital oncology nurse.
Design: Descriptive, cross-sectional study.
Setting: Rambam Health Care Campus in northern Israel.
Sample: A convenience sample of 434 hospital nurses with varied oncology experience.
Methods: Nurses completed a knowledge and attitude questionnaire developed for the current study. Data were analyzed using parametric and nonparametric statistical tests.
Main Research Variables: Hospital nurses’ knowledge of and attitudes toward CM, and attitudes toward integrating CM into the role of the hospital oncology nurse.
Findings: Nurses lack knowledge and are unaware of the risks associated with CM. However, they believe this approach can improve the quality of life of patients with cancer; 51% expressed an interest in receiving training. Oncology nurses were ambivalent about the feasibility of applying an integrative approach, whereas nurse managers expressed significantly more positive attitudes toward integrating CM within the scope of nursing practices.
Conclusions: A large discrepancy remains between nurses’ strong interest in CM and awareness of associated benefits, and their ambivalence toward its integration in their nursing practice.
Implications for Nursing: Although improving nurses’ knowledge should be mandatory, it remains insufficient; a shift in the approach to integrating CM into conventional health care is needed, from practitioners’ responsibility to healthcare policymakers’ responsibility. Legislations and policies are necessary, along with providing respectable infrastructures.
Jump to a section
Awareness and implementation of complementary therapies (CT), alternative medicine, and integrative health care is growing among patients, healthcare professionals, therapists, and researchers worldwide. However, confusion exists regarding terms and definitions, and different terms often are used interchangeably. The term complementary and alternative medicine (CAM) refers to healthcare approaches outside of mainstream Western conventional medicine (National Center for Complementary and Integrative Health [NCCIH, 2016]); the terms complementary medicine (CM) and complementary therapy refer to adjunct therapies that are practiced in conjunction with conventional medicine. As opposed to the nonmainstream approaches (CAM), the integrative health approaches (CM and CT) refer to incorporating complementary approaches into conventional health care in a coordinated manner (Lindquist, Snyder, & Tracy, 2014; NCCIH, 2016).
The theory of integral nursing (Dossey, 2008) provides a conceptual framework for integrating complementary therapies into the nursing care of patients with cancer. The philosophical assumptions of the theory are open, dynamic, and developmental. The theory relates to the four meta paradigms of nursing theory: person, health, environment, and nurse. According to Dossey’s (2008) theory, the person is viewed as a whole physical, mental, emotional, social, and spiritual human being. Other concepts in the theory are healing, patterns of knowing, and transdisciplinary dialogues. The worldviews of CM and nursing are compatible and applicable to nursing practice, education, and research in the field of oncology care.
According to the NCCIH (2016), more than 30% of adults and about 12% of children in the United States use healthcare approaches outside of mainstream conventional medicine. Studies on the use of CAM among patients with cancer reveal a large variability in prevalence. A survey of 956 patients with cancer in 14 European countries revealed that 36% (range = 15%–73%) used some form of CAM (Molassiotis et al., 2005). A literature review (1975–2002) on the use of CAM for breast cancer reported a range of 48%–70% in U.S. patients (Nahleh & Tabbara, 2003). Yates et al. (2005) reported that 91% of newly diagnosed patients with cancer, recruited by 17 community clinical oncology program affiliates throughout the United States (N = 752), used at least one form of CAM. It appears that patients with cancer tend to use CAM more frequently than other populations, particularly to cope with their symptoms and the side effects of conventional treatments.
Nurses’ knowledge and attitudes toward CAM and implementing CAM therapies have been studied in a variety of clinical practices in Western and Eastern countries, such as nurse midwives in the United States and Israel (Hastings-Tolsma & Terada, 2009; Samuels et al., 2010), critical care nurses in Australia and the United States (Cooke, Mitchell, Tiralongo, & Murfield, 2012; Tracy & Lindquist, 2003), surgical nurses in Sweden (Bjerså, Stener Victorin, & Fagevik Olsén, 2012), oncology nurses in Germany, Norway, and the United States (Conrad et al., 2014; Risberg et al., 2004; Roja-Cooley & Grant, 2009), Iranian hospital nurses (Balouchi, Rahnama, Hastings-Tolsma, Shoja, & Bolaydehyi, 2016), and nursing students in Turkey (Topuz, Uysal, & Yilmaz, 2015). Chang and Chang (2015) summarized the main results in a literature review of 15 studies. The majority of nurses (66%) held positive attitudes toward CAM; however, 47%–68% lacked the necessary knowledge to provide CAM or communicate its benefits and risks to patients. Interestingly, studies conducted in Eastern countries, such as China, Japan, Korea, and Taiwan, reported similar results compared to Western countries. One explanation might be attributed to the Western professional education in developed Asian countries (Chu & Wallis, 2007; Holroyd, Zhang, Suen, & Xue, 2008; Osaka et al., 2009; Yom & Lee, 2008).
Literature findings reveal widespread use of CAM among patients, particularly patients with cancer. However, regardless of nurses’ positive attitudes toward CAM, they generally use CT and CM inadequately in practice. To better understand this discrepancy, the current study aims to learn about hospital nurses’ CM knowledge and attitudes as well as their attitude toward integrating CM in the role of the oncology nurse at a large tertiary hospital in Israel.
The objectives of this study were (a) to describe hospital nurses’ CM knowledge, attitudes, and practice; (b) to compare CM knowledge and attitudes between nurse managers and staff nurses with varied daily oncology experience; and (c) to explore hospital nurses’ attitudes toward integrating CM in the role of the oncology nurse in an acute care hospital setting.
Methods
Sample and Setting
The current study is part of a larger research study conducted in 12 medical centers throughout northern, central, and southern Israel, with a sample of 973 nurses. The larger sample was recruited from a variety of settings in nine hospitals (with and without oncology units) and ambulatory medical centers within the community (home-hospice care services and primary care clinics) (Ben-Arye et al., 2017). Participation was offered to a convenience sample of all nurses working at a 1,000-bed tertiary academic hospital, Rambam Health Care Campus, in northern Israel during the first quarter of 2015. The hospital is a referral center for 12 district hospitals, providing more than 2 million residents with comprehensive services in all medical specialties, including a regional oncology center and a CM unit. A response rate of 60% was achieved (434 of 721 questionnaires distributed). Most respondents were from medical–surgical or oncology units, 23% of respondents held managerial positions (i.e., nurse supervisors, unit managers, and charge nurses), and 77% were direct patient-care staff nurses (see Table 1).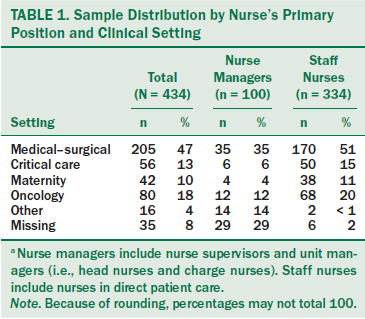
Instrument
A preliminary version of the questionnaire was developed based on an extensive literature review, covering issues such as health professionals’ attitudes toward incorporating CM in the care of patients with cancer; CM training programs for health professionals; and effectiveness and safety of CM in oncology care. Revision of this preliminary questionnaire was conducted in two phases. In the first phase, the clarity of questions and their intent were addressed via a focus group of 11 nurses without formal CM training, and with varied personal and professional backgrounds. In the second phase, the questionnaire was reviewed for content validity by five certified CM nurse practitioners who had graduated from integrative oncology programs.
For the purpose of this study, and to avoid confusion of terms, the authors use the following clarification of CM in the questionnaire: CM relates to CT, traditional, and natural or folk medicine. In addition, a list of CTs commonly used by Israeli patients with cancer is provided (i.e., nutrition, dietary supplements, Chinese medicine/acupuncture, manual/movement interventions, mind-body-spirit therapies, and anthroposophic medicine).
The final survey instrument was comprised of 26 questions and divided into two sections: part 1, demographic and professional characteristics (13 questions); and part 2, CM knowledge, attitudes, and practices (9 questions) and CM training attitudes (4 questions). In part 1, examples of demographic characteristics were age, gender, family status, religion and religiosity, country of origin, and year of immigration. Professional characteristics referred to seniority, hospital department, professional education, postgraduate oncology training, frequency of caring for patients with cancer, and spiritual quest. In part 2, questions were in the form of multiple items assessing the same concept.
Knowledge and attitude assessment involved a set of general knowledge questions; a question with five items assessed knowledge of evidenced-based complementary clinical findings (e.g., alleviation of nausea following acupressure, alleviation of hot flushes in patients with breast cancer by means of hypnosis, improvement in the quality of life (QOL) of patients with non-small cell lung cancer treated with the herb Astragalus); and a question on the effectiveness of CM modalities on QOL for patients with cancer specified six different modalities (i.e., nutrition, dietary supplements, Chinese medicine/acupuncture, manual/movement interventions, mind-body-spirit therapies, and anthroposophic medicine). Two general Likert-type questions, ranging from 1 (very low/negligibly) to 7 (very high/considerably), were asked.
• To what extent can CM improve the QOL of patients with cancer?
• To what extent can CM harm patients with cancer?
A set of questions were asked about respondents’ attitudes toward CM training, including interest in CM training, fields of interest, topics of greatest importance, and where training should occur. In addition, the questionnaire included an integrative care scenario in which CM is combined with conventional care and made available on the unit (present or future) for supportive cancer care. Nurses were asked to describe their attitudes toward the role of the oncology nurse in this scenario. Four choices were provided: (a) refer patients to integrative care based on clinical indications, (b) take an active role in developing an integrative care plan, (c) provide integrative care on the basis of appropriate training, or (d) no need for nurses to be involved in integrative care.
Procedures
The study was reviewed and approved by the hospital’s institutional human research ethics committee (Helsinki Committee). Participation was voluntary, and consent was implied by completing the questionnaire. Questionnaires were first disseminated during a meeting of managerial nurses. Subsequently, head nurses of units were held responsible to distribute the questionnaires to their staff. To ensure anonymity, completed and unidentified questionnaires were returned via a sealed envelope to the statistics department for analysis.
Data Analysis
Data were analyzed using SPSS®, version 21, and a Microsoft® Excel spreadsheet. Demographic and professional characteristics were analyzed using descriptive statistics (mean, SD, frequencies, and percentages). Pearson’s chi-square test and Fisher’s exact test were used to compare prevalence of categorical variables and demographic data between the participants in various groups, as appropriate. A one-way analysis of variance tested for differences among groups for two continuous variables, age and nursing experience, assuming a normal distribution. In cases of non-normal distribution, the authors used the Kruskal Wallis Test, where p values less than 0.05 were considered significant.
Results
Demographic and Professional Characteristics
The average age of the participants was 41.1 years (SD = 9.5). Nurses were predominantly female, married, Israeli born, Jewish, and secular, and expressed a moderate interest in spiritual quests. Most respondents held bachelor’s or master’s degrees; 29% had oncology postgraduate training and a mean of 16.1 years of work experience. Thirty-five percent of the respondents practiced CM for personal use, 9% had trained in the use of CM, and 9% were experienced CM caregivers. Nurse managers were significantly more likely to be older, female, married, Jewish, experienced in nursing, hold a master’s degree, have a higher prevalence of CM training, and be experienced CM caregivers (see Table 2).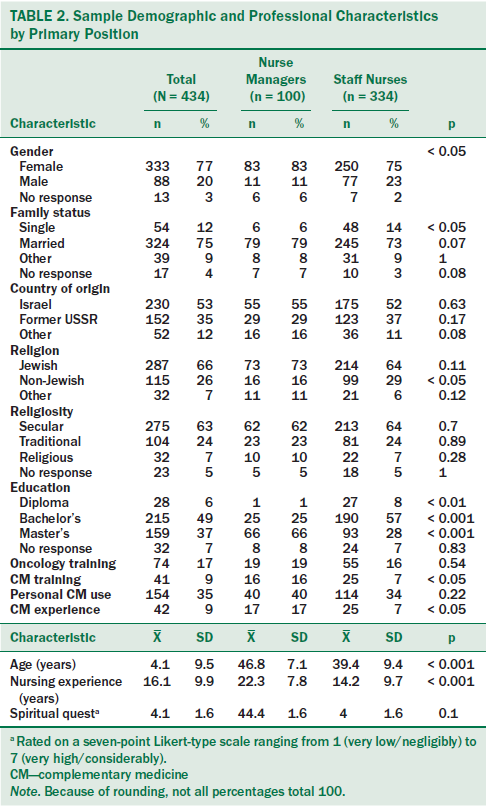
Based on a self-reported question of how frequently nurses take care of patients with cancer on their unit, 42% answered “on a routine everyday basis,” 47% said “occasionally,” and 11% reported “never.” Oncology nurses working on a routine basis with patients with cancer had more postgraduate oncology training than nurses providing care occasionally or never. Nurses in the “occasionally” group had more years of nursing experience; nurses on units with no patients with cancer were more likely to be female, Jewish, and secular; with less personal experience using CM compared to nurses in the other two groups (see Table 3).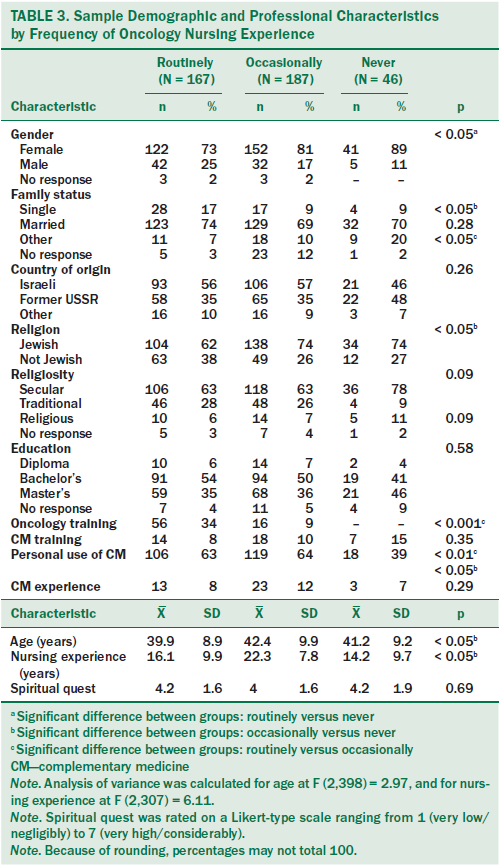
Knowledge and Attitudes
About 25% of participants reported having general CM knowledge and even fewer had knowledge of research findings on specific CM effects. The CM modality perceived by a majority of the nurses to be most beneficial in improving QOL for patients with cancer was mind-body-spirit therapies (e.g., meditation, hypnotherapy, spiritual guidance). This was followed by manual/movement interventions (e.g., reflexology, yoga, Tai Chi), traditional Chinese Medicine/acupuncture, and nutrition. Herbs/dietary supplements (including homeopathy) and anthroposophic medicine (e.g., iscador injections, art and music therapies) were perceived as least beneficial.
Nurses’ attitudes regarding the potential of CM to improve QOL in patients with cancer were relatively positive (4.9 on a 7-point scale), while the perceived risk of CM was very low (1.7 on a 7-point scale) (see Table 4).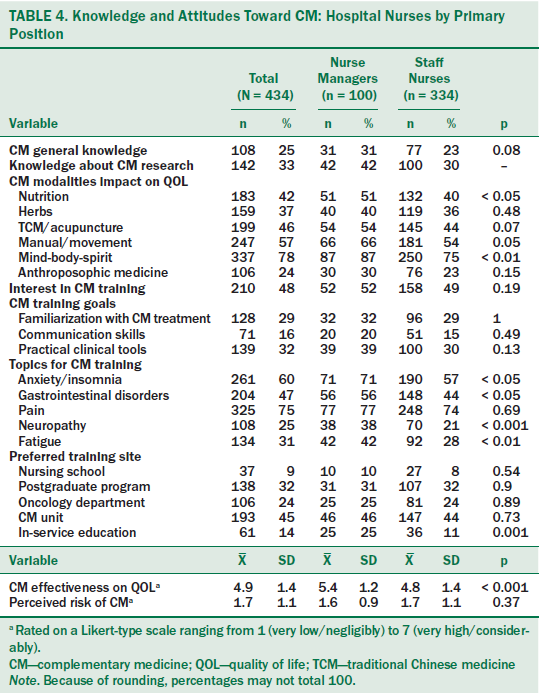
About half of the respondents expressed interest in CM training. Respondents were most interested in learning clinical practice tools and gaining familiarization with CM modalities. The topics of greatest importance were pain relief, followed by alleviation of anxiety/insomnia and gastrointestinal disorders. The topics perceived as least important were fatigue and neuropathy. The preferred training sites were CM units, followed by postgraduate programs.
Nurses in managerial positions held a significantly stronger belief, compared to staff nurses, that CM can improve the QOL of patients with cancer, and, in particular, that nutrition, manual and movement, and mind-body-spirit therapies are most beneficial. In addition, nurse managers listed significantly more important CM topics to focus on. Pain relief was the only topic that both groups of nurses viewed as the most important topic in the training program, with no significant difference between the groups.
No significant differences were determined for any set of CM knowledge and attitudes questions among nurses with different oncology experience (i.e., routinely, occasionally, or never). The only significant difference was found regarding interest in CM training. Nurses who provide oncology care on a routine basis expressed significantly greater interest in CM training compared to nurses who provide oncology care occasionally or never (61% versus 47% and 32%, respectively; p < 0.01).
Oncology Nurse’s Role
In the integrative care scenario (CM is available on the unit for use with conventional care), about 66% of nurses surveyed agreed that the scope of oncology nursing practice should include patient referral to CM, active participation in preparing a care plan, and providing CM (65%, 66%, and 59%, respectively). Only 4% stated that CM should not be part of a nurse’s role. Nurse managers, in particular, scored significantly higher than staff nurses in their beliefs that oncology nurses should be active in developing integrative care plans (79% versus 61%) and providing integrated care (70% versus 55%). No difference between the two groups was found regarding patient referral to integrative care (see Table 5).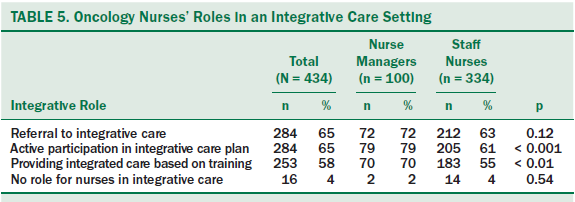
Compared with oncology nurses, nurse managers supported more incorporation of integrated care into the role of the oncology nurse in a hospital setting (see Table 6).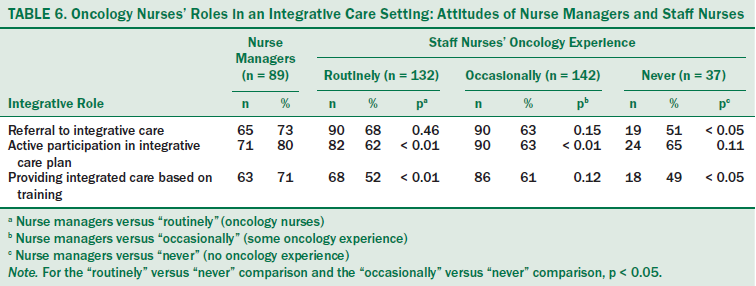
Discussion
Knowledge and Attitudes
The current study demonstrates that hospital nurses, in general, lack knowledge about CM, are unfamiliar with evidence-based research, and are unaware of the risks of CM. Nurses expressed more favorable attitudes toward treatments they were more acquainted with, such as mind-body-spirit therapies, therapeutic touch, and movement therapies, compared to dietary supplements and anthroposophic medicine. However, they believe that CM can improve QOL for patients with cancer. Somewhat surprising was the finding that nurses in oncology units were not more knowledgeable and did not hold more positive attitudes toward CM compared to their colleagues in non-oncology units.
Lack of evidence-based knowledge about CM in professional nurses may hinder nurse–patient communication and the ability to assess needs and to discuss safe treatment options. Nurses must have the knowledge to assist patients in choosing CMs and CTs in conjunction with conventional care and in accordance with the patient’s personal preferences. The discrepancy between nurses’ positive attitudes toward CM and their lack of knowledge is consistent with other research findings, and leads to the conclusion that undergraduate and graduate CM educational programs should be mandatory (Ben-Arye et al., 2017; Geller, Studee, & Chandra, 2005; Lindquist et al., 2014; Muecke et al., 2016; Rojas-Cooley & Grant 2009).
In addition to the positive attitudes toward CM, about 50% of the nurses surveyed expressed interest in CM training, whereas oncology nurses reported even greater interest compared to their colleagues in other units. All respondents expected to acquire more knowledge about CMs and clinical practice tools, and preferred to study within hospital settings such as CM units and oncology departments.
Only 10% of the nurses in the current study reported formal CM training. Nurses are interested in expanding their CM formal education to improve QOL for patients with cancer, in particular for symptoms where conventional medicine does not always offer adequate solutions. A study among 187 RNs in Hong Kong reported that the most common sources for CM information were newspapers, magazines, friends, and books (Holryd et al., 2008).
The lack of formal CM education and lack of awareness of the potential risks of CM when combined with Western medicine should be of concern to policymakers, healthcare professionals, and patients. For nurses to be a reliable source of CM for patients, their education must be based on scientific evidence-based knowledge and expertise in the field of integrative health care. To date, there still is no mandatory CM educational policy in most countries, including the United States and Israel; therefore, nurses rely on varied resources that might be of questionable scientific basis.
Nurse managers demonstrated significantly more positive attitudes than staff nurses regarding their belief in the contribution of CM to patients’ QOL. This finding may be attributed to higher rate of CM training in this group as well as the nurse managers’ professional characteristics, as they are more experienced and formally educated in nursing and in the field of CM. The fact that nurse managers expressed positive CM attitudes could lead to organizational policy and cultural change.
Oncology Nursing Role
Sixty-five percent of nurses surveyed wanted to include referral of patients to integrative care into oncology nursing practice. The referral component of the role requires assessment of patients’ needs and preferences, a knowledge base of CTs, and up-to-date information regarding availability of expert practitioners and resources. This finding emphasizes the large gap between nurses’ positive attitudes toward referral of patients to CM and the lack of clear CM policies, clinical standards of care, and appropriate training. Nurses in managerial positions are significantly more supportive of oncology nurses taking an active part in planning and providing integrated care, in addition to referral, than staff nurses. These findings may be attributed to their professional vision of expanding the role of the oncology nurse in supportive care. Of special interest is the finding that the group of oncology nurses was significantly more ambivalent about integrating CM in their everyday nursing role compared to nurse managers. This finding is particularly interesting since CM is already offered to some extent as part of the palliative care activity in the hospital’s oncology units.
A study by Shorofi and Arbon (2017) attempted to understand the current trend of CAM among hospital-based nurses in Australia. The study included a sample of 322 surgical nurses from five metropolitan hospitals. Although 96% of the nurses indicated that they personally used CAM, most of the nurses reported rarely or never taking history of CAM use. CAM referrals were found to be positively related to nurses attitudes and knowledge about CAM. Even nurses with positive attitudes and knowledge about CAM find it difficult to use CAM in hospital settings. A focus group analysis with 10 hospital nurses who completed CAM education, such as Reiki, aromatherapy, and guided imagery, identified obstacles to CAM use (Kryak, 2014). Main barriers were time, environment (e.g., noise, interruptions by other staff members), and resources. Factors that were recognized to promote the use of CAM were education, nurse-driven consultations, healing space (i.e., quiet, private CAM treatment room), and standard of care. Additional research is needed to better understand the discrepancy between oncology nurses’ positive attitudes toward integrating CM in supportive oncology care and their ambivalence about actual implementation of CM within the scope of their nursing practice.
Limitations
The current study has several limitations. The survey was conducted in a single setting but was part of a larger study representative of nurses in Israel; however, the generalizability of the findings may not be fully representative of nurses cross-culturally. The reliance on respondents’ self-reports may lead to social desirability responses. Using a convenience sample may have caused sampling bias (i.e., nurses who returned the survey may have more or less favorable views of CM). Although the authors used a content validity nursing-specific instrument, it lacks other psychometric testing. Strengths were the high response rate (60%) and the large sample size.
Implications for Nursing
The study findings have implications for nursing policy, practice, education, and research. A void exists in legislation and formal policy position statements about CM and nursing in general, and, in particular, regarding oncology nursing in Israel. Even in countries where such policies exist, nurses are uninformed and unaware of them (Rojas-Cooley & Grant, 2009). A clear international and national perspective is necessary through position statements and state regulations. A need exists to envision models of integrative oncology nursing care in different settings; develop national guidelines and evidenced-based standards of care; define nurses’ role descriptions, including authorities and responsibilities; allocate resources (e.g., applicable patient–nurse load, time, and therapeutic physical environment); and create respectable infrastructure for oncology nursing practice.
CM education should become mandatory and integrated into formal undergraduate and graduate programs to ensure the quality and safety of nursing care. The objective of providing a CM knowledge base for nurses is to enable them to communicate with patients about CM preferences, risks, and therapy options, and to provide referrals. Education also is required for nurses to practice CM therapies formally recognized to be safe and an integral part of nurses’ role. Incorporating CM into the nursing clinical ladder model is recommended. According to this ladder, all novice nurses will be required to gain basic knowledge that will enable them to understand the benefits and risks of CM to patients. The expert integrative nurse practitioner will advance the field by setting standards of care and providing consultation, exemplary practice, education, and research.
Qualitative and quantitative research with healthcare policymakers, nurse managers, educators, and staff nurses in different settings are needed to better understand barriers to the realization of the integrative approach and challenges for the role of the oncology nurse. There is a lack of cross-cultural research in the field with standardized tools and explicit definitions of concepts. Interventional evidence-based studies are needed to measure the effectiveness of CM education and implementation programs. Research is needed to evaluate how nurses can incorporate CM into practice.
Conclusion
The holistic worldview of the discipline of nursing is compatible with the integrative healthcare worldview (Dossey, 2008): they both view the person as an integrative whole, comprising body, mind, and spirit; and they both are patient-centered and combine evidence-based medicine with a caring individualized approach. Oncology nursing is one of the most appropriate nursing fields to face the challenge of integrating authorized and safe CM therapies into the conventional medicine and nursing practices.
However, findings of research studies, including the current study, repeatedly reveal a large discrepancy among nurses’ strong interest in CM, their awareness of its contribution to patients’ QOL, and its poor realization in nursing practice. Researchers tend to attribute this reality to the lack of nurses’ CM knowledge, a main barrier impeding application. Accordingly, the inevitable conclusion is the need to improve nurses’ knowledge by training and educational programs.
It is timely and crucial to make a shift in the approach that nurses are not responsible for practicing CM in oncology care. The authors offer an approach that promotes policymakers’ responsibility to advance integration of CM within the care of patients with cancer. Changes may occur once health policymakers recognize that considerable regulatory work is needed in the field of CM. However, informed decisions regarding (a) safe and evidenced-based therapies and (b) who should practice what forms of CM (physicians, nurses, CM specialists, or interprofessional-certified teams) need to be made prior. There currently is a void in regulations, policies, and standards for education and practices within and outside of the nursing profession.
The authors gratefully acknowledge Ronit Leibe, MS, for her statistical assistance.
About the Author(s)
Admi is an interdisciplinary research coordinator and Eilon-Moshe is an internal auditor, both at the Rambam Health Care Campus; and Ben-Arye is the director of the Integrative Oncology Program at Clalit Health Services, all in Haifa, Israel. No financial relationships to disclose. All authors contributed to the conceptualization and design, data collection, statistical support, analysis, and manuscript preparation. Admi can be reached at h_admi@rambam.health.gov.il, with copy to editor at ONFEditor@ons.org. Submitted July 2016. Accepted for publication November 10, 2016.
References
Balouchi, A., Rahnama, M., Hastings-Tolsma, M., Shoja, M.M., & Bolaydehyi, E. (2016). Knowledge, attitude and use of complementary and integrative health strategies: A preliminary survey of Iranian nurses. Journal of Integrative Medicine, 14, 121–127.
Ben-Arye, E., Shulman, B., Eilon, Y., Woitiz, R., Cherniak, V., Sharabi, I., . . . Admi, H. (2017). Attitudes among nurses toward the integration of complementary medicine into supportive cancer care. Oncology Nursing Forum, 44, 428–434. doi:10.1188/ONF.17.428-434
Bjerså, K., Stener Victorin, E., & Fagevik Olsén, M. (2012). Knowledge about complementary, alternative and integrative medicine (CAM) among registered health care providers in Swedish surgical care: A national survey among university hospitals. BMC Complementary and Alternative Medicine, 12, 42.
Chang, H.Y., & Chang, H.L. (2015). A review of nurses’ knowledge, attitudes, and ability to communicate the risks and benefits of complementary and alternative medicine. Journal of Clinical Nursing, 24, 1466–1478. doi:10.1111/jocn.12790
Chu, F.Y., & Wallis, M. (2007). Taiwanese nurses’ attitudes towards and use of complementary and alternative medicine in nursing practice: A cross-sectional survey. International Journal of Nursing Studies, 44, 1371–1378. doi:10.1016/j.ijnurstu.2006.07.001
Conrad, A.C., Muenstedt, K., Micke, O., Prott, F.J., Muecke, R., & Huebner, J. (2014). Attitudes of members of the German Society for Palliative Medicine toward complementary and alternative medicine for cancer patients. Journal of Cancer Research and Clinical Oncology, 140, 1229–1234. doi:10.1007/s00432-014-1656-9
Cooke, M., Mitchell, M., Tiralongo, E., & Murfield, J. (2012). Complementary and alternative medicine and critical care nurses. Australian Critical Care, 25, 213–223. doi:10.1016/j.aucc.2011.12.055
Dossey, B.M. (2008). Theory of integral nursing. Advances in Nursing Science, 31, E52–E73. doi:10.1097/01.ANS.0000311536.11683.0a
Geller, S.E., Studee, L., & Chandra, G. (2005). Knowledge, attitudes, and behaviors of healthcare providers for botanical and dietary supplement use for postmenopausal health. Menopause, 12, 49–55.
Hastings-Tolsma, M., & Terada, M. (2009). Complementary medicine use by nurse midwives in the U.S. Complementary Therapies in Clinical Practice, 15, 212–219. doi:10.1016/j.ctcp.2009.06.016
Holroyd, E., Zhang, A.L., Suen, L.K., & Xue, C.C. (2008). Beliefs and attitudes towards complementary medicine among registered nurses in Hong Kong. International Journal of Nursing Studies, 45, 1660–1666.
Kryak, E.D. (2014). Impact of intrinsic and extrinsic factors on nurses’ use of hospital-endorsed complementary and alternative medicine treatments [Thesis]. Drexel University.
Lindquist, R., Snyder, M., & Tracy, M.F. (2014). Complementary and alternative therapies in nursing (7th ed.). New York, NY: Springer.
Molassiotis, A., Fernadez-Ortega, P., Pud, D., Ozden, G., Scott, J.A., Panteli, V., . . . Patiraki, E. (2005). Use of complementary and alternative medicine in cancer patients: A European survey. Annals of Oncology, 16, 655–663. doi:10.1093/annonc/mdi110
Muecke, R., Paul, M., Conrad, C., Stoll, C., Muenstedt, K., Micke, O., . . . Huebner, J. (2016). Complementary and alternative medicine in palliative care: A comparison of data from surveys among patients and professionals. Integrative Cancer Therapies, 15, 10–16.
Nahleh, Z., & Tabbara, I.A. (2003). Complementary and alternative medicine in breast cancer patients. Palliative and Supportive Care, 1, 267–273.
National Center for Complementary and Integrative Health. (2016). Complementary, alternative, or integrative health: What’s in a name? Retrieved from https://nccih.nih.gov/health/integrative-health
Osaka, I., Kurihara, Y., Tanaka, K., Nishizaki, H., Aoki, S., & Adachi, I. (2009). Attitudes toward and current practice of complementary and alternative medicine in Japanese palliative care units. Journal of Palliative Medicine, 12, 239–244. doi:10.1089/jpm.2008.0215
Risberg, T., Kolstad, A., Bremnes, Y., Holte, H., Wist, E.A., Mella, O., . . . Cassileth, B.R. (2004). Knowledge of and attitudes toward complementary and alternative therapies; a national multicentre study of oncology professionals in Norway. European Journal of Cancer, 40, 529–535. doi:10.1016/j.ejca.2003.11.011
Rojas-Cooley, M.T., & Grant, M. (2009). Complementary and alternative medicine: Oncology nurses’ knowledge and attitudes. Oncology Nursing Forum, 36, 217–224. doi:10.1188/09.ONF.217-224
Samuels, N., Zisk-Rony, R.Y., Singer, S.R., Dulitzky, M., Mankuta, D., Shuval, J.T., & Oberbaum, M. (2010). Use of and attitudes toward complementary and alternative medicine among nurse-midwives in Israel. American Journal of Obstetrics and Gynecology, 203, 341.
Shorofi, S.A., & Arbon, P. (2017). Complementary and alternative medicine (CAM) among Australian hospital-based nurses: Knowledge, attitude, personal and professional use, reasons for use, CAM referrals, and socio-demographic predictors of CAM users. Complementary Therapies in Clinical Practice, 27, 37–45.
Topuz, S., Uysal, G., & Yilmaz, A.A. (2015). Knowledge and opinions of nursing students regarding complementary and alternative medicine for cancer patients. International Journal of Caring Sciences, 8, 656–664.
Tracy, M.F., & Lindquist, R. (2003). Nursing’s role in complementary and alternative therapy use in critical care. Critical Care Nursing Clinics of North America, 15, 289–294.
Yates, J.S., Mustian, K.M., Morrow, G.R., Gillies, L.J., Padmanaban, D., Atkins, J.N., . . . Colman, L.K. (2005). Prevalence of complementary and alternative medicine use in cancer patients during treatment. Supportive Care in Cancer, 13, 806–811.
Yom, Y.H., & Lee, K.E. (2008). A comparison of the knowledge of, experience with and attitudes towards complementary and alternative medicine between nurses and patients in Korea. Journal of Clinical Nursing, 17, 2565–2572.

