Feelings of Disenfranchisement and Support Needs Among Patients With Thyroid Cancer
Purpose: To offer a better understanding of the experiences, preferences, and needs of patients with thyroid cancer.
Participants & Setting: 17 patients with thyroid cancer receiving treatment at a university-affiliated hospital in Montreal, Québec, Canada.
Methodologic Approach: Interviews were conducted with patients, and descriptive phenomenology was used to explore patients’ lived experience.
Findings: Coping with uncertainty was a major theme that emerged from interviews, with some of the main concerns being difficult treatment decisions, long surgery wait times, and fears about surgical complications, potential metastases, and death. Study participants reported that without a nurse and an interprofessional team, they would be lost in a system they believed minimized their illness and offered few resources to support them in a time of crisis.
Implications for Nursing: Nurses must understand how the needs of individuals with thyroid cancer are often overlooked because of the good prognosis associated with the disease and should work to meet these information and support needs.
Jump to a section
Thyroid cancer has been identified as the most rapidly growing form of cancer and is particularly prevalent in women aged 15–29 years (American Cancer Society, 2018; Canadian Cancer Society, 2012). Generally associated with a favorable prognosis, thyroid cancer usually involves medically focused treatment with hemithyroidectomy or total thyroidectomy, with or without adjuvant radioactive iodine treatments (nuclear medicine), and is followed by levothyroxine thyroid hormone replacement therapy and lifelong follow-up (Haugen et al., 2016).
A systematic review by Husson et al. (2011) reported conflicting results regarding quality-of-life impairments in the survivorship period; some studies reported persistent health problems and lower quality of life in thyroid cancer survivors compared to the general population, whereas others noted a tendency for quality of life to resume to baseline levels. In addition, a large study of 518 post-treatment individuals with thyroid cancer found that 65% continue to experience neurologic, musculoskeletal, and psychological symptoms, and 25% experience thyroid hormone imbalance (Schultz, Stava, & Vassilopoulou-Sellin, 2003). Other studies reveal the long-term impact of thyroid cancer on patients’ sense of vitality, mental health, and social functioning (Crevenna et al., 2003; Tan, Nan, Thumboo, Sundram, & Tan, 2007).
The only two qualitative studies on this topic conducted previous to the current study concern the experiences of people with thyroid cancer receiving radioactive iodine treatment (I-131) (Sawka et al., 2009; Stajduhar et al., 2000). These studies highlight certain features of the thyroid cancer experience as it relates to radioactive iodine treatment, including (a) the need for patients to be recognized as having a serious illness and to be normalized in their fears of cancer and of the unknown; (b) the social and physical isolation during radioactive iodine treatment and patients’ fear of radioactivity; (c) the need for patients to be better prepared and informed about pre- and post-treatment side effects, postradiation safety precautions, and dietary restrictions, all of which provide patients with heightened feelings of control and empowerment; and (d) the need to better understand treatment barriers, such as nursing workload and delays in treatment. Both studies include a comprehensive approach to understanding that addresses the physical and psychosocial needs of patients with cancer who are receiving treatment.
The current study is part of the implementation and evaluation of a supportive care program created by the current authors (Henry et al., 2018). The aim of this study is to better understand the experiences, preferences, and needs of people with thyroid cancer. The approach taken by this study is novel because it explores the experience of patients using a broader lens than had been employed in previous work. For example, the current study involves a larger, all-encompassing approach that stretches the length of the care continuum (including prediagnostic workup, diagnosis, waiting time for surgery, surgery and hospitalization, recovery from surgery, radioactive iodine treatment, scans, onset of levothyroxine thyroid hormone replacement therapy, transition to post-treatment follow-up, and survivorship) rather than a narrower, strictly treatment-based focus. In a sense, this study adopts an illness-focused conceptual framework (i.e., focus on the person behind the disease), rather than a disease-focused one (i.e., focus on the disease itself), that is akin to a more holistic approach to quality of life. This study also features a variety of thyroid cancer types, including presurgery patients with highly suspicious indeterminate thyroid biopsies, a common occurrence in thyroid cancer (Cooper et al., 2009). A wider perspective allows for a more comprehensive approach on which to optimize nursing and interprofessional care (Amir, Scully, & Borrill, 2004; Canadian Partnership Against Cancer, 2012; Oncology Nursing Society [ONS], 2017).
Methods
Sampling and Recruitment
Individual interviews were conducted with a purposive sample of patients with thyroid cancer from July 9 to August 11, 2015. Patients were selected to maximize variability on axes of gender, age, thyroid cancer type, staging (i.e., localized to the thyroid versus neck node involvement), initial level of distress, and planned treatment. Interviews were conducted until data reached saturation (i.e., no new themes emerged over three consecutive interviews) and was considered to be descriptively rich.
Participants were eligible if they met the following criteria:
• Had recently completed treatment for papillary, follicular, or medullar thyroid cancer
• Were aged 18 years or older
• Were capable of giving free and informed consent
• Were deemed to be physically well enough to participate in the interviews; this was based on self-perceived wellness and a Karnofsky Performance Status score of more than 60.
• Were able to communicate and be understood in English or French
• Were able and willing to communicate their thoughts in an interview context
There were no exclusion criteria. Participants were recruited at Jewish General Hospital in Montreal, Québec, Canada, an urban university-affiliated hospital. Ethics approval was obtained by the hospital’s research ethics committee, and all participants signed informed consent for the interviews.
Interview Context
The interviews were conducted by two of the authors (M.H. and Y.X.C.) in English or French, depending on patient preference, and they occurred either in person at the treating hospital or over the telephone. They were carried out using descriptive phenomenology (Giorgi, 2009) and respecting criteria for methodologic rigor (credibility, transferability, dependability, and confirmability) (Shenton, 2004). Descriptive phenomenology was deemed suitable for this study because it investigates lived experience and provides a rich description of facets of a given experience from the point of view of the investigated (Husserl, 1977, 1982; Shenton, 2004). Interviews were semistructured and strove to unearth rich, in-depth description through use of an interview canvas with questions originally based on a literature review (Husson et al., 2011) and a holistic quality-of-life construct (Calman, 1984). The interview canvas evolved throughout the interviews and included the following themes:
• The impact on the patient and his or her circle of family and friends of being diagnosed with thyroid cancer
• Experience with physical (e.g., fatigue, pain) and psychological (e.g., anxiety, depression, trauma, uncertainty, body image concerns) symptoms throughout the cancer trajectory
• Coping with cancer
• Thoughts about death and dying
• The decision-making process that surrounds treatments
• The balance between cancer and the patient’s family life, social life, work, and leisure activities
• The impact of cancer on various spheres (i.e., family life, social life, work, and leisure activities), including functionality
• Social support from the patient’s medical team, partner, family, and friends
• Communication around the illness
• Supportive care needs along the continuum of care
Probes were used to help patients further explain and clarify their stories. Interviews were audio recorded, transcribed verbatim in the interviewee’s language, and continually analyzed throughout the project using NVivo 10. One of the current authors (Y.X.C.) bracketed relevant interview excerpts (i.e., nodes) reflecting the experience of patients with thyroid cancer and combined these into overarching categories, which evolved as the analyses progressed. Another current author (M.H.), who is a more senior research team member, enriched the analysis after each interview through identification and discussion of further themes. Taken together, the themes that emerged from the interviews were intended to represent the essence of the thyroid cancer experience.
Methodologic Rigor
Credibility was ensured through peer debriefing (review of progressive and final data analysis by M.H. and Y.X.C.), prolonged engagement (principal investigator M.H. is an experienced psychologist who works clinically with individuals with thyroid cancer), charted observations and notes, and audit trails. Transferability was ensured by having a varied sample of participants with sociodemographic characteristics comparable to the overall population of individuals with thyroid cancer. Dependability was ensured through auditing and clear documentation of the research process, as well as reflexivity (investigators M.H. and Y.X.C. kept written accounts of internal and external dialogue throughout the research process). Confirmability was ensured through audits and triangulation; the data collection and analysis processes were constantly reviewed by two of the current authors (M.H. and Y.X.C.), and the data were fed back to participants in subsequent interviews for their input (Shenton, 2004). Although one of the current authors (M.H.) is a psychologist on the unit, she had not met the patients participating in this study prior to their interviews.
Results
Sample
Of the 27 patients contacted for interviews, 17 agreed to participate in the study. The mean age of participants was 45.2 years (SD = 16.5). Sociodemographic and medical characteristics of the study sample are presented in Table 1. Sixteen interviews were conducted face-to-face at the hospital, and one was conducted via telephone; the interviews had a median duration of 53 minutes (range = 38–69 minutes). 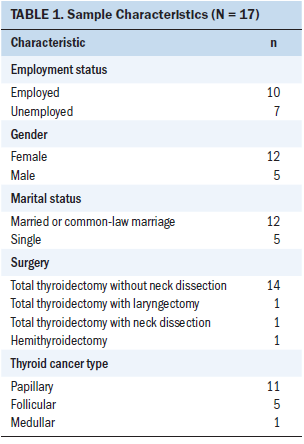
Patient Experience
Coping with uncertainty was a major theme that emerged from patient interviews. For example, patients felt that the intensity of their fears was not fully acknowledged by surgeons and endocrinologists, and they struggled with the challenges associated with what they perceived as complex treatment decision making. Patients feared cancer progression, surgical complications, and having their “throat slit,” reflecting the sensitive area in which surgery was to be performed. The younger parents interviewed often expressed concern about the welfare of their children when they were undergoing treatment. Patients also expressed distress associated with excruciatingly long waiting periods for cancer surgery. In addition, patients reported feeling socially awkward because of the visibility of their postoperative surgical scars. Some patients feared dependency on (and, in some cases, withdrawal from) levothyroxine thyroid hormone replacement therapy, did not understand the dietary restrictions imposed by radioactive iodine treatments, and feared social reintegration because they had been exposed to radiation. Patients noted their appreciation for nurses and members of the interprofessional team who helped them to address these issues.
A need to be taken seriously: Patients who had undergone biopsy were aware, prior to their diagnosis, that cancer could be the outcome. However, most patients nonetheless felt the full emotional blow of being told that their biopsy revealed or was suspicious for cancer. They still experienced the bad news with shock and devastation, and they either stopped listening or became silent when they heard the word “cancer” in an attempt to maintain their composure.
Hearing you have cancer, the doctor will answer whatever they can, but in that moment, you are struck with that news. You can’t think of all the questions you have had. You forget everything within two seconds of hearing that “C-word.” I even had written [questions] down because I knew I was going to hear that C-word, but I had forgot to even take my phone out. No matter how mentally prepared you are, you can never, ever, in my opinion, be ready to hear that news. It is going to affect you emotionally. My husband, I mean, the whole family, was in shock. (Participant 1)
Although information about the slow-growing nature of thyroid cancer and its good prognosis reassured patients, the word “cancer” was typically emotionally laden and was still associated with a shortened life. Some patients experienced confusion and ambiguity when optimistic prognoses contradicted their original, relatively uninformed notion that “all cancers kill.” This led some patients to doubt the curative nature of the proposed surgery to the point of mistrusting their doctor and perceiving him or her to be deceitful (e.g., the doctor was pretending that the patient’s tumor was benign to reassure him or her). Patients’ fears were reinforced if they knew of people who had died of cancer, particularly thyroid or head and neck cancer, or if they believed that “doctors don’t always tell you the whole picture.” Patients felt the need for reassurance from their nurse.
I have a history of cancer in my family. My mom died at a very young age of 49. She had a mastectomy, then it spread to her back and spine. I was there to change the dressings with my father. I’m well aware of cancer and what it can do and how it can affect the family. (Participant 5)
Several patients mentioned feeling frustrated because they believed their concerns were minimized by physicians, particularly when healthcare providers reassured them that thyroid cancer was “nothing to be worried about” and was “the best cancer” to have. This was also the message patients felt they received from thyroid cancer survivors, whom they described as having forgotten the harrowing nature of their experience. Some patients worried whether their feelings were normal and whether they were even permitted to experience psychological turmoil in light of the medical team’s reassurance. Being presented with the facts of thyroid cancer and its associated good prognosis was as important to many patients as others recognizing and legitimating their experience of being diagnosed with and treated for cancer or suspected cancer. They reported their nurse being more attuned to their experience of cancer, as well as acknowledging their feelings and providing a space to express and process them.
It’s bad to say . . . and it’s really annoying when people go like, “Oh, yeah, thyroid cancer is the best cancer to have!” Because lots of doctors told me a lot of times, and it’s true, but, like, still, it’s still cancer! . . . They would repeat it a lot, every doctor I went to. Maybe it’s a form of reassurance, but it wasn’t. (Participant 7)
Patients reported similar concerns in relationships with their peers. For example, they felt that their peers occasionally minimized patients’ concerns but at other times exaggerated the dangers. Patients said they needed others to understand and legitimize their emotional reactions; however, when peers’ responses were exaggerated, they exacerbated patients’ fears and concerns. Above all, patients wanted to keep things normal during the months that they waited for surgery. Although the diagnosis of a suspected or confirmed thyroid cancer was felt to be traumatizing, the context surrounding the illness (e.g., other stressful life events, others’ reactions) also contributed to feelings of vulnerability.
I act like it’s no big deal, so I think people are confused. You tell them you have cancer, and their immediate reaction is, “Oh, my God! Ahhh!” and then I’m like, “It’s no big deal.” I don’t want to deal with that reaction; it makes me rehash those emotions. I don’t want to go there. I just went there, and it’s not fun. I don’t want to go back there. I don’t talk about it like it’s “ahhh.” I don’t want to think about it. (Participant 6)
It was very minimized: “Yes, but you don’t have chemo, you’re not losing your hair, you’re not losing a breast.” . . . “No, I lost my thyroid gland, I got operated [on] twice, my company revenues declined, and I have a son who is now depressed. It’s very trivial!” (Participant 11)
Some patients experienced grief, including feeling disillusioned about their previous conception of themselves as healthy and fearing they would lose a valued part of their body, forever altering the essence of who they were.
Whenever you are going to lose a piece of your body, there is some mourning. I think my self-concept was that I was a very healthy person. . . . You feel somehow not intact. So, probably that’s a part of it and just, you know, a reminder of your vulnerability. I had always had the self-belief that I was very strong and . . . it reminds you that you’re vulnerable, that anybody is vulnerable. (Participant 15)
Other patients simply refused to talk about their cancer, feeling that they could not rely on anyone for support, were ashamed, feared being a burden, or wanted to be stoic. The diagnosis was still always in the back of their minds; they struggled in silence as they repeated their mantra: that everything was going to be OK. They wanted to believe this.
It’s weird because on an intellectual level, I’m not worried, you know? It’s like this sort of disconnect between what my mind said, and, obviously, my emotions are somewhere else. And you also, you want to project this calm, that there’s no problem. I can say that I don’t put this in front of anybody, except maybe my husband. I tended to be very stoic. (Participant 16)
Complex treatment decision-making process: Patients experienced oscillation between their former nihilistic beliefs and their newly formed optimistic perspectives on thyroid cancer and its associated treatments; this dichotomy intensified during the long waiting period for surgery and sometimes led to confusion about what treatment decisions to make. Alignment with their surgeons’ and endocrinologists’ optimistic views regarding prognosis led patients to choose a more conservative approach to treatment. When aligned with their fears, however, patients opted for a more extensive approach. Patients experienced having a life-threatening illness and tried to rationalize this fear by reminding themselves that it was an easily treatable condition with few risks of complications. The fear inevitably came back at various points during the long waiting period for surgery. Patients reported turning to their nurse for emotional and decision-making support at that time.
In cases of unambiguous thyroid cancer, treatment options were discussed in a relatively straightforward manner, as Participant 12 reported: “It all kind of happened in Dr. B.’s office just like that. . . . He said, ‘You know, level five—we just automatically remove it,’ and so there wasn’t much thinking process. It was just like, ‘OK, let’s go!’” In contrast, patients’ thyroid biopsy results were often inconclusive, leading to confusion regarding what treatment option to pursue when two equivalent options were presented (e.g., wait and see with repeated thyroid ultrasounds versus surgery, total thyroidectomy versus hemithyroidectomy) and a need for additional decision-making support. Unless complete clarity existed in the diagnosis and treatment plan, patients generally reported being reluctant to undergo surgery. They tried to remain optimistic regardless of the likelihood of a cancer diagnosis, still believing that their final pathology report postsurgery could reveal a benign tumor. Some patients based their treatment decision on this hope and pushed for a more conservative approach (e.g., wanting a hemithyroidectomy rather than the recommended total thyroidectomy), only to be shocked and experience decisional regret when ultimately told they needed a second surgery.
I didn’t expect it to be cancer. Cancer was a shock to me. . . . . After the first surgery, I thought it was over. [The news about needing a second operation] was very difficult to manage emotionally. I didn’t feel like it. I knew this could happen, but I guess in my mind it wouldn’t. Still, I can’t believe it. People told me, “You have a cancer,” and I say, “No, I don’t have a cancer. I have a 21% hope.” (Participant 2)
Some family members opposed the recommendations of the medical team, encouraging the use of more natural methods, such as homeopathy and health behavior changes like diet and exercise, instead of surgery. One patient reported feeling pressured by the surgeon to make a quick medical decision during the sole appointment prior to surgery instead of being encouraged to think through—and be helped through—the ambiguity. Participant 10 said, “I don’t know if it’s just me, but I felt all the surgeons that I’ve met really wanted to operate [on] me.”
In addition, some patients felt confused when disagreements arose among their endocrinologist, surgeon, or other physicians regarding the best treatment course. They feared angering one physician by taking advice from another, feeling as though they needed their nurse to serve as a mediator and facilitate communication. Participant 17 said, “There was some tension between my endocrinologist and my surgeon’s team about what calcium I should be taking and the number I should be taking and all that. . . . It’s sort of the feeling of the child of divorced parents.”
Patients felt pressured to coordinate their own care and follow-up visits, particularly when being seen by different departments with no oversight. This was problematic not only in the instance of differing medical opinions, but also during the transition to endocrinology, when some patients felt abandoned with no guidance and had the responsibility of making their own appointments with their endocrinologist.
I didn’t know what would happen after the surgery. I felt a little bit alone and lost. OK, now I no longer have a thyroid—what’s going to happen? Who will give me my [levothyroxine] Synthroid® prescriptions? I don’t know how it works. It’s very frustrating! (Participant 15)
I remember hearing [this] from one of the doctors early on: “You are my patient. I understand you are pregnant and you are having a baby, but you are my priority.” The person used the word “terminate,” as in terminate the pregnancy. When you are 28 weeks pregnant and you have gone that far and the baby is healthy, using that word was not cool. It sent me out of [there] thinking, “Oh, my God. I’m going to have to abort this baby and then deliver it!” . . . I don’t want you to sugarcoat anything, but you know. [To] this day, hearing that, it’s hard. . . . At the time, I didn’t have a nurse or anybody I could talk to, so [I had] to digest and process this information by myself and [come] to a proper conclusion as to what I’m going to do. (Participant 17)
Most patients noted that they were reluctant to seek clarification from the surgeon after the initial consultation, fearing that this would be perceived as them challenging the surgeon’s recommendations and could sabotage their surgery (e.g., increased waiting times, heightened risk for complications) or that the surgeon simply would not have the time to address their questions. Patients generally felt that their nurse was more accessible and less intimidating. They could count on their nurse to answer questions and support them in their experience and decision making; their nurse also had access to their surgeon, if needed.
You can have a meeting with your doctor every few months, but that lasts 5 minutes, 10 minutes maximum. You leave there, and you have all these things going through your head. Doctors are going to take the time to answer your questions for the most part, but when you leave, you still have questions that come up an hour later when you are driving home or waiting for the bus. You can’t just call and speak to your doctor. You have to make another appointment, which is three months later. . . . The doctor said that I could contact him if I had questions about the surgery, but the secretary didn’t want to let me talk to him. (Participant 13)
Fear and anxiety about having the cancer spread, experiencing surgical complications, and having their “throat slit”: Patients feared the possibility of surgical complications (particularly voice loss or impairment and calcium deficiency), early menopause or depression postsurgery, dying (either on the operating table or from the cancer), and their cancer metastasizing to other organs while waiting for, or as a consequence of, the surgery. Patients described themselves as information seeking and viewed their nurse as a reliable source of information to turn to when questions inevitably arose. Some patients were fearful of a resident performing the surgery because they believed this would increase their risk of complications. Although patients voiced this concern, they were still willing to accept the risk because of their diagnosis of cancer.
My scan results have been received, but I don’t know if it has spread. Do I still have cancer? I don’t know, and I’m only meeting Dr. K. in September, so until then, I’m waiting to hear. . . . I’m not saying I am emotionally anxious, but it would be nice to know so I can enjoy my summer. (Participant 11)
The location of the cancer caused additional anxiety for patients because of the delicate nature of the neck area. Some patients mentioned their fear of having their “throat slit,” a term that evoked frightening visual images of a serial killer and a guillotine. As Participant 1 said, “You get your throat slit—now tell me how you are going to feel about it!”
Patients’ hospitalization postsurgery was generally described as uneventful, except for some abrupt interactions with unit staff who were perceived as uncaring (e.g., nurses on night shifts) and uninformed regarding patients’ need for pain control. When complications occurred postsurgery (e.g., calcium deficiency, loss of voice), they perpetuated the ambiguity and anxiety that patients had hoped would abate. Some felt as though their capacity to cope had been eroded; they had expended all their resources while waiting for surgery and no longer felt capable of coping with another challenge. Patients tended to conflate normal postsurgical symptoms with cancer. For example, they did not know if their fatigue was a normal postsurgical symptom or a cancer-related symptom. Some realized how dependent they were on their voice and how “handicapped” they felt without it. They worried they would never recover vocal cord function and had trouble navigating the hospital system to address their concerns. Patients said their nurse was resourceful and offered them needed guidance and support.
I thought [the voice loss experienced over two months] could be permanent, and I got very concerned at the end, but it just came back, just like that, within, like, one or two days. I felt a pain, a sharp pain in my neck, and I thought, “What the heck? What’s going on now?” and then two days later, my voice came. The pain I felt I think was my nerves coming back. Within four or five days, I was able to talk—not powerfully but I had speech. Back to normal, I was relieved. . . . I don’t know how much longer I could have gone on without a complete meltdown. (Participant 14)
Wanting to protect their children: Most patients were young women dealing with multiple roles and leading full, active lives that included work. Some patients had children to care for, whereas others were caregivers for parents or other relatives. Younger patients were preoccupied with how their children would react to the cancer and to different types of separation (e.g., hospitalization, isolation precautions associated with radioactive iodine treatments). Parents reported needing guidance from their nurse to know how to communicate with their children about their cancer and treatments in an age-appropriate way. They imagined that they could die and leave their children motherless or fatherless, and some, consequently, prepared their wills. Patients reported either not talking to their children at all for fear of traumatizing them when they were already in a fragile state or, on the opposite end of the spectrum, preparing their children for the eventuality of their death. Many children were described by patients as preoccupied, anxious, and even depressed, particularly those who were younger or who had preexisting difficulties. They feared their parent dying and worried about the parent’s health and well-being.
I was living alone with my son. The day before my first operation, he was so frightened. He broke down. I had put together a nice album. I wanted to leave him nice things in case something happened. . . . I made my . . . [will]. I did so many things because I was told . . . [death] was possible . . . and I saw people die of this. I told my son and said. “It’s OK. You can cry. You will be grieving but no more than one year. After that, you live your life—you’re happy now! (Participant 9)
The word “cancer” is very scary, especially for an 8-year-old and [when the cancer is] associated with your mother. . . . She voiced that fear [of losing me] all the time. Every time we would go out the door, [she would say,] “Mommy, be careful!” (Participant 8)
Some patients were forced to postpone their plans to have children because of their radioactive iodine treatments. Others feared long-term infertility, and those who had children were concerned they would harm their children with radiation. Some pregnant patients feared transmitting the cancer to their unborn child.
I’m not allowed to get pregnant for another 6–12 months. I have a newborn, but my plan was to have two babies back to back, so now I have to wait. (Participant 17)
Long wait time for cancer surgery: Patients reported needing to wait several months for their thyroid cancer surgery. Considering the level of fear and anxiety patients reported experiencing when diagnosed with cancer, this significant wait only added to their psychological stress. The wait also increased the likelihood that patients would experience other major life events (e.g., change in health of a family member, change in living condition), compounding their vulnerability. One patient described this wait as “psychological warfare.”
For me, the hardest part in all of this is the waiting. . . . It makes me angry. . . . It makes me kind of aggressive inside. . . . I try constantly to keep calm, you know, stay chill, keep the anxiety down and the nerves down. . . . The longer it takes to wait for this surgery—that, on a daily basis, weighs on me. So, as the date approaches, it gets harder and harder and harder. . . . Waiting is just killing me! Waiting is killing me! (Participant 7)
Patients had trouble managing their emotions and keeping their fears and uncertainties at bay during this long wait. They tried their best to “keep it all together” and devoted an incredible amount of energy to this aim. They were worried because they had to wait months to find out their surgery date. Some patients tried to bargain with the medical team to find out their date, others called the hospital secretaries every day, and a few threatened to change hospitals or commit suicide if their surgery date was not immediately made known to them. Once a surgery date was set and confirmed, patients felt an immediate sense of relief and comfort, but then they got increasingly anxious as this date approached. They feared the surgery itself, as well as the possibility of their surgery being canceled at the last minute. When their surgery date was changed or when they were told that the surgery date had been only tentatively made, patients felt desperate, increasingly angry, and insulted, and some even thought that the healthcare system “didn’t really care” if they had cancer or about what would happen to them. Participant 2 said, “All along, in my head, I was sure they would cancel my surgery date because my cancer wasn’t a priority.” Patients were appreciative of being able to turn to their nurse for support and reassurance during the waiting period for surgery.
[The secretary] told me that the waiting time [for the surgery] had increased quite a bit. . . . After having argued with her multiple times, I finally obtained a date and wanted it confirmed because the date had already changed many times. She refused and said the date could even change on the day of the surgery. That was very, very stressful. (Participant 15)
Scar as a visible sign of thyroid cancer: Prior to surgery, patients expressed apprehension over the appearance of their scar, and several patients were concerned that their scar would be visible to others. It helped when the scars were hidden in a neck crease, allowing them to go unnoticed.
I’m very fortunate that I have these lines in my neck naturally that I’ve always thought, “Oh, they’re so ugly!” But now that I have this scar hidden in one of those lines, I’m thinking these lines are great—no one is ever going to know. . . . [The surgeon] did it right on the line. (Participant 4)
It took patients time to adjust to the scar; they felt self-conscious, attempted to camouflage the scar by covering or shifting attention away from it, and even considered plastic surgery or alternative surgeries in another country (e.g., robotic surgery with an incision in the axilla area).
I was wearing scarves a lot because it was the fall. Nobody had to know—I would put a scarf on, but now I feel more comfortable wearing a necklace. Usually, I wear my hair down. I didn’t tie my hair up for a long time. (Participant 10)
Patients indicated that, when in public, they would be approached by other thyroid surgery survivors, who, on viewing the scar, would engage them in a dialogue about their experience. This was alternatively viewed as supportive, intrusive, and reminiscent of the trauma of disease and treatment. For some, the scar was a sign of weakness to cover up, a mark of stigma and shame. Sometimes the scar rehashed self-esteem issues or past traumatic events involving shame. The concerns seemed to be related to the developmental stage of the individual. For example, younger patients, who were at a stage of their lives when they would expect to be healthy, found dealing with disease to be mystifying, which was a view shared with their peers; this prompted feelings in the patient that the cancer was strange and mysterious. Sometimes, onlookers would be naïve, inexperienced, and tactless, making insensitive observations to patients about their appearance or experience. This was particularly true in the case of hyperplastic healing (keloid) in young adults. Responding to others’ probes and questions required that patients feel confident and socially comfortable.
Fearing dependence on levothyroxine thyroid hormone replacement therapy: Most patients had never previously taken medication; it was a major adjustment for them to consider taking levothyroxine, given as thyroid hormone replacement therapy, daily for life. Patients found having to remember to take the medication every day stressful and experienced considerable fear of withdrawal symptoms on days they forgot. Some were concerned about becoming ill or even dying if a dose was missed.
I wanted to keep half of my thyroid and wanted to avoid taking the pill forever. That was a major concern for me, and I’m still having trouble adjusting to the fact that I have to take something every day. (Participant 2)
When patients had trouble adjusting to the medication and experienced chronic fatigue, they felt slowed down compared to their peers and as though they were unable to carry on all aspects of their previously active lives. For some, the medication represented an attack on their freedom, spontaneity, and independence, as well as a loss of self-sufficiency. Being dependent on medication evoked long-standing issues around autonomy and invited rebellion, with some patients systematically forgetting to take the medication. Others felt insecure because they could no longer rely solely on themselves for their needs. For example, one patient feared being unable to refill the medication in the case of an emergency or if access to a pharmacy was restricted (e.g., in times of war, if pharmacies ran out, if stranded in the wilderness).
My next step is to learn how to make it or substitute it myself if I couldn’t take it. Being able to stockpile at least two years’ supply, you know, just that would help. . . . Every day, I try to better my life by eliminating the dependency or bad habit or something, and now this one—it’s just there. I can’t do anything about it. (Participant 14)
Withdrawal from levothyroxine thyroid hormone replacement therapy, implementation of low-iodine diet, feelings of physical isolation, and fear of exposing others to radiation: Patients had multiple concerns related to radioactive iodine treatment, including withdrawal from levothyroxine thyroid hormone replacement therapy, implementation of a low-iodine diet, and feelings of physical isolation. Although most patients in the current study received an injection of recombinant human thyroid–stimulating hormone to prevent a hypothyroid state or a scan prior to radioactive iodine treatments, some patients elected to withdraw their levothyroxine because they could not afford to pay or did not want another medical intervention. Patients then experienced intense fatigue and were lethargic, which, on rare occasions, was felt by patients and family members as tragic because this state was equated with illness progression and the end of life. Patients said they felt restricted by the low-iodine diet and expressed frustration and helplessness over finding food that met the requirements (such as avoiding ionized salt, dairy products, and egg yolk and whole eggs) but was tasteless. They felt constrained, forced, and punished.
The hardest part about the whole process is the [low-iodine] diet. The diet was horrible. It was really hard to find something to eat. . . . I was living off of fruits and vegetables, and I was very nauseated. The food was tasteless—it was horrible. I was always hungry, but food would make me nauseated. (Participant 13)
When physically isolated from others because of the radiation, some patients were able to reflect, for the first time, on their illness and treatment experience during the preceding several months and were only then able to come out of “survival mode.” This was a very emotional time for some patients and was particularly challenging because of the absence of their supportive circle of family and friends. Some patients felt profoundly disconnected from others and even abandoned.
Being in isolation for those . . . three days without seeing anyone is when it all hit me. I sat there and I thought, “What the hell happened in the past year?” I went into survival mode when I found out. . . . Then, all of a sudden, I had all this time to myself because I was radioactive, and all these emotions came rushing in, and that was when it was overwhelming. (Participant 8)
Young mothers had to separate from their children, some for the very first time. They saw their children’s reaction to the separation and were distressed, fearing long-term impact on their children’s psychological well-being. Patients also felt anxious about the safety precautions because radioactivity cannot be seen and was viewed by patients as being abstract and intangible. Some feared that they would remain radioactive after the required isolation period and became anxious when around others for fear of hurting them, particularly their children.
Positive impact: Once treatments were completed, patients (provided they did not experience complications) generally reframed their experiences and spoke of how the physical component was “much easier than expected.” The diagnosis of thyroid cancer was reported in certain instances to have had a positive impact on patients in hindsight, influencing them to quit smoking, increasingly appreciate life and live in the moment, and show more empathy, care, and concern toward people around them.
During the week, I was in the hospital with no voice, stuck to an IV bag. To pass the time . . . [I was] helping people as much as I could in the hospital, giving directions, any way I could. . . . Some guy in my room that was having another procedure, I went to the restaurant and got him food because he couldn’t get food. . . . The experience was powerful. I’m definitely not the same person . . . maybe nicer, more thoughtful . . . more emotional. (Participant 14)
Patients realized that life is fragile and were committed to valuing and emphasizing family and friends. They also realized the significance of their own accomplishments and decided to take a more proactive approach to life and living. For some patients, the experience of thyroid cancer served as a reminder of a larger sense of perspective, rendering daily stressors less important in comparison. As Participant 12 said, “I have grandkids. I’d like to see them when they grow up and everything. . . . I said to myself, ‘This is it—I have to enjoy myself.’”
Some patients still feared a cancer recurrence post-treatment, particularly when undergoing scans and before coming to the hospital for follow-up visits. They were hypervigilant about physical symptoms. However, patients reflected positively on their cancer diagnosis (as compared to other cancers) and favorable thyroid surgery outcomes.
Discussion
The breadth and depth of concerns expressed by participants in the current study highlight the complexity of thyroid cancer when viewed through a biopsychosocial lens. The distress experienced by individuals with thyroid cancer is understandable when also considering their accumulation of known risk factors for distress, including the following (Holland et al., 2015):
• Younger age
• Female sex
• Dependents living at home
• Trajectory of care comprising a single medical visit presurgery
• Illness minimization
• Context of uncertainty and ambiguous decision making
• Long waiting period for treatment
• Visible scar
This list does not include patients’ personal characteristics, which also shape their degree of resilience and vulnerability in response to the disease and include the following (Agaibi & Wilson, 2005):
• Flexibility
• Coping style
• Emotional regulation
• Self-esteem
• Secure attachment
• Health literacy
• Social supports
• Concomitant life stressors
• Psychiatric history
This complexity of the thyroid cancer experience contrasts with individuals’ reports of feeling minimized in their experience of thyroid cancer because of a good medical prognosis; such minimization is akin to disenfranchised grief, in which a loss is not openly acknowledged or socially supported (Selby et al., 2007). Disenfranchised grief has been associated with deterioration in patients’ physical and mental health and has been found to be a significant predictor of depression (Selby et al., 2007). Recognizing the emotional turmoil people with thyroid cancer experience, even in the face of an excellent prognosis, can allow patients to effectively process their emotions, rather than simply avoid them. This promotes habituation (i.e., decreased response to a stimulus following repeated exposure) and does not reinforce vigilance and avoidance pathways that maintain trauma (Blair & Blair, 2013) and compromise function (Chawla & Ostafin, 2007).
This study not only emphasized the iatrogenic effects of being diagnosed with and treated for thyroid cancer, but also identified certain systemic issues of concern that exacerbate patients’ uncertainty and stress response. In Canada, patients with thyroid cancer must contend with significantly longer than usual surgical wait times (more than six months from the time of an identified thyroid abnormality) in the face of a life-threatening condition (Brake et al., 2013). As corroborated by interview data from the current study, other studies have shown that patients experiencing delays in treatment voice concerns about lack of communication and support from their medical providers, experience increased anxiety, and exhibit an overall poorer prognosis (Tran et al., 2015). The current study illustrates how wait times in thyroid cancer care can complicate patients’ decision-making process and psychological response by increasing the period of uncertainty to the point of becoming unbearable and even psychologically traumatic, with stress becoming chronic. Patients felt that these long wait times eroded their capacity to cope with challenges arising postsurgery (e.g., voice loss, the need for a second surgery, radioactive iodine treatments and associated diet restrictions and safety precautions). Psychological stress associated with long-term perseverative cognition (worry, rumination, and anticipatory stress) has been shown to negatively affect the cardiovascular, immune, endocrine, and neurovisceral systems (Brosschot, Gerin, & Thayer, 2006).
The decision-making process in thyroid cancer is thought to be straightforward, with treatment presented as a step-by-step approach. However, the current study suggests that decision making is complex; it cannot be assumed that individuals with thyroid cancer will simply choose the option that prolongs life the longest. Many other factors influence decision making, such as treatment effectiveness, the benefit–harm balance (i.e., weighing the benefits of treatment against its potential harm), and the long-term consequences of treatment on functionality (i.e., effects on physical and emotional function) (Reyna, Nelson, Han, & Pignone, 2015). When a medical situation is uncertain or ambiguous, patients tend to choose the safest option—one that minimizes risks—even if the outcome is therapeutically suboptimal. The more aggressive treatment is then likely considered to be the riskiest option (Reyna et al., 2015). In the context of thyroid cancer, patients fear the consequences of surgery and anesthesia (e.g., the possibility of dying on the surgical table) and the functional impact of a full thyroidectomy on their voice, levels of fatigue, and mental health. Patients interviewed for the current study noted their desire to keep half of their thyroid because of inconclusive biopsy results and the potential long-term effects of depending on levothyroxine thyroid hormone replacement therapy. Decision making was described by patients as being influenced by individual beliefs and values; making a decision went beyond the rational weighing of pros and cons and was not always in accordance with the best available treatment (Reyna et al., 2015).
Decision aids that help to sort out patients’ ambiguity and integrate their treatment preferences could be developed and used as an antidote to distress in cancer centers treating patients with thyroid cancer. Decision aids are widely used for a variety of medical conditions requiring patient decision making and have been found to be effective in increasing knowledge, compared to usual care alone, particularly when the decision aid comprised detailed information about the various treatment options (Stacey et al., 2014). In addition, decision aids result in more accurate perceptions of risk, final decisions being more congruent with patient values, and lower decisional conflict from lack of information or unclear values around the decision to be made.
Findings from the current study suggest the need to adopt an illness-focused, rather than a strictly disease-focused, perspective in medically caring for patients with thyroid cancer, broadening the disease-centered approach proposed in the American Thyroid Association’s guidelines on the management of thyroid cancer in adult patients (Haugen et al., 2016). The healthcare system needs to more clearly distinguish between (a) a manageable medical disease with a likelihood of survival and recovery and (b) the experience of the illness, or the disease’s effects on the body and mind. While treating the disease, it is important to acknowledge and empathize with the patient regarding its impact, recognizing that a good cancer prognosis does not preclude a patient from experiencing distress.
Implications for Nursing
This study supports the routine provision of a nurse who screens for common symptoms of concern using clinical practice guidelines (Canadian Partnership Against Cancer, 2012; Howell et al., 2010; National Comprehensive Cancer Network, 2017) and patient-reported outcomes (Ader, 2007), as well as engages a needs-based interprofessional team that includes allied professionals, such as psychologists, social workers, dietitians, and speech therapists, for patients with thyroid cancer. The nurse can be present in the consultation room when the physician informs patients of biopsy results that indicate a suspected or confirmed thyroid cancer. This nurse can then follow patients throughout their trajectory of care and provide needed information, additional communication, comfort, reassurance, and continuity of care. A psychologist could be introduced to patients needing help with managing anxiety and body image issues, as well as with readjusting to functional impairments, including fatigue and loss of voice. A social worker could assist families, increasing age-appropriate communication with children and promoting compatible coping styles in the couple and family. Dietitians could provide guidance on the low-iodine diet in preparation for radioactive iodine treatments. Speech therapists could work with patients on managing voice impairments. This care would be in line with what is offered to patients with early-stage breast cancer as part of the National Accreditation Programs for Breast Centers (ONS, 2017); a navigation process is required for accreditation as a Certified Quality Breast Center of Excellence. The current study shows that access to a nurse and other allied healthcare professionals should not be solely based on medical prognosis, but rather on reported unmet needs.
Limitations
This study took place at a university-affiliated hospital in a Canadian city and may not reflect the care provided in other institutions or cities. Patients’ experiences may differ according to the healthcare systems in place in a given country, particularly the waiting periods for thyroid cancer surgery; this is a topic meriting further inquiry. A similar medical setting where patients do not have access to a nurse and interprofessional care could have rendered very different results. This study strove for variability in thyroid cancer type and included medullary thyroid cancer; patients with undifferentiated thyroid cancer may have a different experience because of their more extensive treatment and uncertain prognosis. The current study also did not include patients with anaplastic thyroid cancer, which is known to have a much poorer prognosis; accordingly, patients with this type of thyroid cancer may not feel as disenfranchised as the patients interviewed for this study because these patients are more readily provided with support. This study also focused on the early phases of diagnosis; additional research is needed to investigate longer-term adjustment issues. 
Conclusion
This study emphasizes how the needs of individuals with thyroid cancer have been overlooked because of a good medical prognosis. Findings from this study highlight the need for healthcare providers to more specifically address the psychosocial complexities and the healthcare system challenges of this group of patients. In addition to treating the disease, systematic access to a nurse championing an interprofessional team offers comprehensive support at a time of potential crisis.
About the Author(s)
Melissa Henry, PhD, UQAM, MPs, BSc, is an assistant professor and Yu Xin Chang, McG., is a medical student, both in the Gerald Bronfman Department of Oncology, and Saul Frenkiel, BSc, MD, CM(McG.), FRCSC, is a professor in the Department of Otolaryngology–Head and Neck Surgery, all at McGill University; Gabrielle Chartier, RN, BScN, MScN, CON, is a nurse pivot at Jewish General Hospital; Richard Payne, MD, CM(McG.), MSc, FRCSC, is an associate professor in the Department of Otolaryngology–Head and Neck Surgery at McGill University; Christina MacDonald, RN, BScN, MScN, CON, is an oncology clinical nurse specialist at Jewish General Hospital; Carmen Loiselle, BScN, MSc, PhD, is a professor in the Ingram School of Nursing, and Martin J. Black, MD, CM(McG.), FRCSC, is an associate professor, and Alex M. Mlynarek, MSc, MD, CM(McG.), FRCSC, is an assistant professor, both in the Department of Otolaryngology–Head and Neck Surgery, all at McGill University; Antoinette Ehrler, RN, BScN, is the codirector of the Segal Cancer Centre, Zeev Rosberger, PhD, MA, is a senior investigator at the Lady Davis Institute for Medical Research, Michael Tamilia, MD, is an endocrinologist in the Division of Endocrinology, all at Jewish General Hospital; and Michael P. Hier, MD, is chief of the Department of Otolaryngology–Head and Neck Surgery at Jewish General Hospital and an associate professor in the Department of Otolaryngology–Head and Neck Surgery at McGill University, all in Montreal, Québec, Canada. This research is part of the implementation and evaluation of a supportive care program developed by the authors and funded by Genzyme. Henry was supported by a Clinician-Scientist Salary Award from the Fonds de Recherche du Québec—Santé. Chang was supported by a Canadian Institutes of Health Research Health Professional Student Research Award, as well as a McGill University Faculty of Medicine 2015 Fall Bursary Program Student Research Award. Mention of specific products and opinions related to those products do not indicate or imply endorsement by the Oncology Nursing Society. Henry, Chang, Frenkiel, Payne, Loiselle, Black, Mlynarek, Ehrler, Rosberger, Tamilia, and Hier contributed to the conceptualization and design. Henry, Chang, Frenkiel, Chartier, Payne, Black, Ehrler, Tamilia, and Hier completed the data collection. Henry and Chartier provided statistical support. Henry, Chang, Frenkiel, Payne, Black, Ehrler, Rosberger, Tamilia, and Hier provided the analysis. Henry, Chang, Frenkiel, Payne, MacDonald, Loiselle, Black, Mlynarek, Ehrler, Rosberger, Tamilia, and Hier contributed to the manuscript preparation. Henry can be reached at melissa.henry@mcgill.ca, with copy to ONFEditor@ons.org. (Submitted January 2018. Accepted March 27, 2018.)
References
Ader, D.N. (2007). Developing the Patient-Reported Outcomes Measurement Information System (PROMIS). Medical Care, 45, S1–S2. https://doi.org/10.1097/01.mlr.0000260537.45076.74
Agaibi, C.E., & Wilson, J.P. (2005). Trauma, PTSD, and resilience: A review of the literature. Trauma, Violence, and Abuse, 6, 195–216. https://doi.org/10.1177/1524838005277438
American Cancer Society. (2018). Key statistics for thyroid cancer. Retrieved from https://www.cancer.org/cancer/thyroid-cancer/about/key-statistics.html
Amir, Z., Scully, J., & Borrill, C. (2004). The professional role of breast cancer nurses in multi-disciplinary breast cancer care teams. European Journal of Oncology Nursing, 8, 306–314. https://doi.org/10.1016/j.ejon.2003.12.011
Blair, K.S., & Blair, R.J.R. (2013). Generalized anxiety disorder and social phobia considered from a cognitive neuroscience perspective. In K.N. Ochsner & S.M. Kosslyn (Eds.), The Oxford handbook of cognitive neuroscience: Volume 2: The cutting edges (pp. 450–462). New York, NY: Oxford University Press.
Brake, M., Moore, P., Taylor, S.M., Trites, J., Murray, S., & Hart, R. (2013). Expectantly waiting: A survey of thyroid surgery wait times among Canadian otolaryngologists. Journal of Otolaryngology–Head and Neck Surgery, 42, 47.
Brosschot, J.F., Gerin, W., & Thayer, J.F. (2006). The perseverative cognition hypothesis: A review of worry, prolonged stress-related physiological activation, and health. Journal of Psychosomatic Research, 60, 113–124. https://doi.org/10.1016/j.jpsychores.2005.06.074
Calman, K.C. (1984). Quality of life in cancer patients—An hypothesis. Journal of Medical Ethics, 10, 124–127.
Canadian Cancer Society. (2012). Canadian cancer statistics 2012. Toronto, ON: Canadian Cancer Society, Public Health Agency of Canada, & Statistics Canada.
Canadian Partnership Against Cancer. (2012). Navigation: A guide to implementing best practices in person-centred care. Toronto, ON: Canadian Partnership Against Cancer.
Chawla, N., & Ostafin, B. (2007). Experiential avoidance as a functional dimensional approach to psychopathology: An empirical review. Journal of Clinical Psychology, 63, 871–890. https://doi.org/10.1002/jclp.20400
Crevenna, R., Zettinig, G., Keilani, M., Posch, M., Schmidinger, M., Pirich, C., . . . Dudczak, R. (2003). Quality of life in patients with non-metastatic differentiated thyroid cancer under thyroxine supplementation therapy. Supportive Care in Cancer, 11, 597–603. https://doi.org/10.1007/s00520-003-0474-4
Cooper, D.S., Doherty, G.M., Haugen, B.R., Kloos, R.T., Lee, S.L., Mandel, S.J., . . . Tuttle, R.M. (2009). Revised American Thyroid Association management guidelines for patients with thyroid nodules and differentiated thyroid cancer. Thyroid, 19, 1167–1214. https://doi.org/10.1089/thy.2009.0110
Giorgi, A. (2009). The descriptive phenomenological method in psychology: A modified Husserlian approach. Pittsburgh, PA: Duquesne University Press.
Haugen, B.R., Alexander, E.K., Bible, K.C., Doherty, G.M., Mandel, S.J., Nikiforov, Y.E., . . . Wartofsky, L. (2016). 2015 American Thyroid Association management guidelines for adult patients with thyroid nodules and differentiated thyroid cancer: The American Thyroid Association guidelines task force on thyroid nodules and differentiated thyroid cancer. Thyroid, 26, 1–133. https://doi.org/10.1089/thy.2015.0020
Henry, M., Frenkiel, S., Chartier, G., MacDonald, C., Payne, R.J., . . . Hier, M.P. (2018). Thyroid cancer patients receiving an interdisciplinary team-based care approach (ITCA-ThyCa) appear to display better outcomes: Program evaluation results indicating a need for further integrated care and support. Psycho-Oncology, 27, 937–945. https://doi.org/10.1002/pon.4590
Holland, J.C., Breitbart, W.S., Jacobsen, P.B., Loscalzo, M.J., McCorkle, R., & Butow, P.N. (Eds.). (2015). Psycho-oncology (3rd ed.). New York, NY: Oxford University Press.
Howell, D., Keller-Olaman, S., Oliver, T., Hack, T., Broadfield, L., Biggs, K., . . . Syme, A.A. (2010). A Pan-Canadian practice guideline: Screening, assessment and care of psychosocial distress (depression, anxiety) in adults with cancer. Retrieved from https://www.capo.ca/pdf/ENGLISH_Depression_Anxiety_Guidelines_for_Posti…
Husserl, E. (1977). Phenomenological psychology: Lectures, summer semester, 1925 (J. Scanlon, Trans.). The Hague, Netherlands: Martinus Nijhoff.
Husserl, E. (1982). Ideas pertaining to a pure phenomenology and to a phenomenological philosophy: First book: General introduction to a pure phenomenology (K. Kersten, Trans.). New York, NY: Springer.
Husson, O., Haak, H.R., Oranje, W.A., Mols, F., Reemst, P.H., & van de Poll-Franse, L.V. (2011). Health-related quality of life among thyroid cancer survivors: A systematic review. Clinical Endocrinology, 75, 544–554. https://doi.org/10.1111/j.1365-2265.2011.04114.x
National Comprehensive Cancer Network. (2017). NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines®): Thyroid carcinoma [v.2.2017]. Retrieved from https://www.nccn.org/professionals/physician_gls/pdf/thyroid.pdf
Oncology Nursing Society. (2017). 2017 oncology nurse navigator core competencies. Retrieved from https://bit.ly/2v2HmOn
Reyna, V.F., Nelson, W.L., Han, P.K., & Pignone, M.P. (2015). Decision making and cancer. American Psychologist, 700, 105–118. https://doi.org/10.1037/a0036834
Sawka, A.M., Goldstein, D.P., Brierley, J.D., Tsang, R.W., Rotstein, L., Ezzat, S., . . . Magalhaes, L. (2009). The impact of thyroid cancer and post-surgical radioactive iodine treatment on the lives of thyroid cancer survivors: A qualitative study. PLOS ONE, 4, e4191. https://doi.org/10.1371/journal.pone.0004191
Schultz, P.N., Stava, C., & Vassilopoulou-Sellin, R. (2003). Health profiles and quality of life of 518 survivors of thyroid cancer. Head and Neck, 25, 349–356. https://doi.org/10.1002/hed.10217
Selby, S., Jones, A., Burgess, T., Clark, S., Moulding, N., & Beilby, J. (2007). Disenfranchised grievers—The GP’s role in management. Australian Family Physician, 36, 768–770.
Shenton, A.K. (2004). Strategies for ensuring trustworthiness in qualitative research projects. Education for Information, 22, 63–75.
Stacey, D., Légaré, F., Col, N.F., Bennett, C.L., Barry, M.J., Eden, K.B., & Wu, J.H. (2014). Decision aids for people facing health treatment or screening decisions. Cochrane Database of Systematic Reviews, 2014, CD001431. https://doi.org/10.1002/14651858.CD001431.pub4
Stajduhar, K.I., Neithercut, J., Chu, E., Pham, P., Rohde, J., Sicotte, A., & Young, K. (2000). Thyroid cancer: Patients’ experiences of receiving iodine-131 therapy. Oncology Nursing Forum, 27, 1213–1218.
Tan, L.G., Nan, L., Thumboo, J., Sundram, F., & Tan, L.K. (2007). Health-related quality of life in thyroid cancer survivors. Laryngoscope, 117, 507–510. https://doi.org/10.1097/MLG.0b013e31802e3739
Tran, K., Sandoval, C., Rahal, R., Porter, G., Siemens, R., Hernandez, J., . . . Bryant, H. (2015). Wait times for prostate cancer treatment and patient perceptions of care in Canada: A mixed-methods report. Current Oncology, 22, 361–364. https://doi.org/10.3747/co.22.2795




