Climate Change Should Be on Every Nursing Research Agenda
Human-caused climate change is a global emergency, and its harms are predicted to increase exponentially in the coming years, particularly if unsustainable practices continue unmitigated. Adverse effects of climate change on communities affected by or at risk for cancer, such as frail older adults, are already measurable and deadly. If nurse scientists continue to ignore these realities, more people are likely to suffer and die as a result. The purpose of this critical reflection is to discuss the vital necessity of including climate change in the research agenda of the Oncology Nursing Society and all nursing science. Using an approach grounded in critical theory and design justice, the authors provide specific suggestions for the incorporation of scientific considerations and nursing measures related to climate change into oncology nursing science.
Jump to a section
The urgency of the current global crisis that is human-caused climate change is undeniable. As of the submission of this manuscript on January 7, 2020, a quarter of the country of Australia is on fire, with more than 12.35 million acres already burned (McNamara, 2020). Experts have attributed these unprecedented wildfires to periods of drought, record-breaking heat, and strong winds—all phenomena associated with a changing climate (McNamara, 2020). Once considered impossible, research backing the association of specific disasters, such as the Australian wildfires, with the ongoing effects of human-caused climate change has grown exponentially in recent years (American Meteorological Society, 2020; Waldman, 2017). A 2019 special issue of the New England Journal of Medicine focused specifically on clinical guidance to manage increasingly evident health effects of a changing climate (Salas et al., 2019). The journal Science and numerous other scholarly institutions have declared climate change the greatest threat to humanity and global ecosystems (Hoegh-Guldberg et al., 2019). According to the World Health Organization (WHO) and other global health authorities, near-term health effects of climate change include direct effects from weather-related emergencies, such as periods of extreme heat and dramatic changes in rainfall patterns leading to wildfires, hurricanes, mudslides, and floods; indirect effects through increased incidence of disease, particularly vector-borne illnesses, increased allergens, and other environmental pollutants; mental health crises related to climate-related stress and displacement; and major disruptions to economies and built infrastructures, such as electrical grids, roads, and other supply routes (Intergovernmental Panel on Climate Change, 2018; WHO, 2018). The Fourth National Climate Assessment found that the health and well-being of all Americans is already affected by climate change and that these effects are expected to worsen (U.S. Global Change Research Program [USGCRP], 2018). The Intergovernmental Panel on Climate Change, in a 2018 executive report, states that higher temperatures lead to greater health risks and increased poverty, with significantly higher harm associated with warming of 2°C compared to warming of 1.5°C. Anthropogenic climate change has the potential to affect every living being on the planet, particularly individuals at risk for or living with a cancer diagnosis. Evidence indicates that, among those at risk, individuals and communities who have been socially, economically, and geographically marginalized have already experienced significant harms (Levy & Patz, 2015; Sorenson & Garcia-Trabanino, 2019; Veenema et al., 2019). These harms include displacement, economic losses, psychological morbidity, chronic illness burden, physical trauma, and death. Such harms are predicted to increase and expand as the effects of climate change accrue and become more apparent (USGCRP, 2018).
In 2019, the Oncology Nursing Society (ONS) released the results of an expert consensus study on contemporary oncology nursing research priorities (Von Ah et al., 2019). The top three priority areas for oncology nursing research identified were symptom science, particularly as it pertains to emergent cancer therapies such as immunotherapy, precision medicine, and the use of biosignatures; health disparities; and palliative and psychosocial care. Four “cross-cutting themes” designed to provide context and elaboration for each of these priorities were also named: aging, survivorship, healthcare delivery system implications, and the use of advanced research methods (Von Ah et al., 2019). Despite the direct and urgent threats posed by climate change to individuals with cancer and the delivery of high-quality oncology nursing care, climate change did not appear on ONS’s research agenda for 2019–2022. A search of the archives of ONS’s flagship journals, Oncology Nursing Forum and Clinical Journal of Oncology Nursing (CJON), revealed only two articles, both commentaries in CJON, that addressed this topic (Mayer & McCabe, 2013; Nix & Caldwell, 2018).
Climate change has serious implications for the practice of oncology nursing and for the communities that oncology nurses serve (Mayer & McCabe, 2013). For example, climate change–associated events, including increased “natural” disasters (e.g., wildfires, hurricanes), can damage critical infrastructure for delivering cancer care, such as hospitals and clinics, and may cut off access to vital resources, such as electricity, food, and clean water (Nix & Caldwell, 2018). Figure 1 describes how this occurred on the island of Puerto Rico following 2017’s Hurricane Maria, as told from the perspective of an oncology nurse living and working in San Juan (S.P.-M.). These emergencies disrupt care and supply chains for vital medications, such as chemotherapy, and other pharmacotherapies necessary for supportive care and symptom management (USGCRP, 2018). 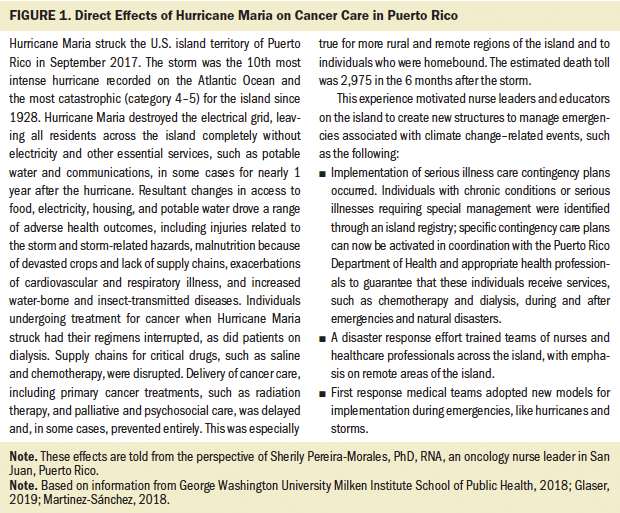
Climate change–related disasters, such as the recent wildfires in northern California and Australia, also adversely affect air quality and other aspects of the natural and built environment that may increase risks for developing or exacerbating certain cancers and other chronic conditions, such as asthma and obstructive lung disease (Schweitzer et al., 2018). Various practices related to cancer care including drug manufacturing processes, disposal of cancer drugs, hospital-driven pollution, and carbon costs of cancer-related technologies (e.g., increased use of artificial intelligence for research involving big data and clinical decision support) have direct environmental effects that may also exacerbate some aspects of climate change (Glaser, 2019; McCarthy & Bernstein, 2019).
Critical Theory Perspectives on Climate Change and Oncology Nursing Science
Oncology nursing science is founded on a plurality of philosophical and theoretical traditions that are constantly evolving and that are derived from nursing, other scientific disciplines, and the humanities. These range from positivistic, biomedical models of health (e.g., those used to generate and test hypotheses in some genetics and precision health research) (Zhu et al., 2019), to descriptive, phenomenologic inquiries (Lundquist et al., 2019), to emancipatory, constructivist epistemologies (Driscoll & Goodman, 2019; Gifford et al., 2019). Critical theory represents a large and diverse body of philosophy and scholarship with origins in Germany’s Frankfurt School of philosophers and social theorists (Mosqueda-Díaz et al., 2014). These scholars of the 1920s and 1930s distinguished critical theory from traditional theory by its goals: to critically assess and critique power dynamics and other social forces that shape culture and health in such a way as to move society closer toward collective liberation from all forms of structural oppression and inequity (Bohman, 2005). Since that time, critical theory has evolved to encompass numerous scholarly traditions with their own diverse canons of foundational literature, including, but not limited to, various feminisms, critical race theory, queer theory, postcolonial criticism, and the emergent fields of critical digital studies and design justice (Argüello, 2016; Benjamin, 2019; Bohman, 2005; Broussard, 2019; Costanza-Chock, 2018; Noble, 2018).
Critical theorists position individuals and communities as the experts of their own situated realities, as opposed to passive objects to be studied. In addition, critical theorists seek to engage and center the perspectives and leadership of the individuals who experience forms of injustice, such as climate- and cancer-related health inequities. Critical theorists remain particularly attuned to individuals whose identities and voices are typically marginalized or silenced by structures of oppression in society, such as neighborhood segregation by class, economic status, gender essentialism, or institutionalized racism. Nurses maintain close proximity to and collaboration with the individuals and communities they serve, so it is not surprising that examples of critical theory in nursing scholarship abound, including applications to philosophical and political discourses in nursing (Aranda, 2019), nursing education (Georges, 2005), and oncology nursing practice (Ramvi & Ueland, 2019). Kagan et al.’s (2014) landmark anthology, Philosophies and Practices of Emancipatory Nursing: Social Justice as Praxis, is required reading in many U.S.-based nursing education programs.
Given the myriad ways in which planetary health intersects with and amplifies other structural and social determinants of health (Watts et al., 2018), a critical theory–informed approach that centers the individuals and communities at greatest risk for harm is essential for the generation of oncology nursing research priorities and strategies to address the global climate emergency. Epidemiologic studies indicate that the worst effects of climate change, so far, have largely been felt by communities pushed to the margins by what scholars of Black feminism such as Patricia Hill Collins have named the “matrix of domination” (Anderson et al., 2019; Collins, 1990; Shultz et al., 2019). This matrix includes structures of power and oppression that shape society, such as modern economic imperialism and settler colonialism (Barker, 2009), neoliberalism (Shrubsole, 2015), centered whiteness and white supremacy (Bailey et al., 2017; Berry & Gross, 2020; Crenshaw, 1991; Kendi, 2019), ableism (Barbarin, 2019), and heteropatriarchy (Collins, 1990; Costanza-Chock, 2018). Stated more specifically, critical theory indicates that some of the individuals at greater risk of harm from the effects of anthropogenic climate change and its intersections with other sociopolitical and economic structures of oppression include the following:
• Older adults, particularly those who are geographically or socially isolated (McDermott-Levy et al., 2019)
• Individuals not fluent in the dominant language of a region or country
• Migrants and climate refugees displaced from their homes by heat waves, floods, wildfires, or other natural disasters and their resulting economic or political consequences (Benevolenza & DeRigne, 2019; Nix & Caldwell, 2018)
• Individuals who are unhoused or who do not have access to stable housing and, therefore, may be ineligible for financial support from disaster funds in the event of a catastrophic event (Gibson, 2019)
• Black communities, Indigenous communities, and other communities of color adversely affected by overexposure to ongoing and historical harms caused by White domination, imperialism, and settler colonialism (Berry & Gross, 2020; Kendi, 2019; Kim, 2018)
• Individuals who are lesbian, gay, bisexual, transgender, queer, intersex, or asexual, who may be made to feel unwelcome and unsafe in climate shelters and care centers (Goodwin, 2019)
• Disabled or neurodiverse individuals (Barbarin, 2019)
• Individuals who are frail, immunosuppressed, or have multiple chronic conditions (Salas et al., 2019)
• Those with reduced agency for autonomous decision making, such as individuals in institutional settings, individuals involved with carceral systems, and the very young (Mrkusic & Gross, 2018)
• Resource-starved communities in poor and economically or politically unstable regions (Sorenson & Garcia-Trabanino, 2019; USGCRP, 2018; Veenema et al., 2019)
Climate Change as a Cross-Cutting Oncology Nursing Research Theme
This critical perspective explores opportunities for oncology nurses and nurse scientists to immediately incorporate climate change into their research and strategic priorities. A critical theory–informed nursing response to climate change requires design justice: centering the leadership and priorities of individuals and communities who have been pushed to the margins in decision-making processes related to research priorities, resource allocation, and other responses to anthropogenic climate change. Design justice requires intentional reflection on who is involved in the design of systems and nursing responses to cancer and climate change, who is benefiting from those systems, and who is most likely being harmed. In addition,
design justice focuses on the ways that design reproduces, is reproduced by, and/or challenges the matrix of domination . . . to ensure a more equitable distribution of design’s benefits and burdens; fair and meaningful participation in design decisions; and recognition of community based design traditions, knowledge, and practices. (Costanza-Chock, 2018, pp. 1, 5)
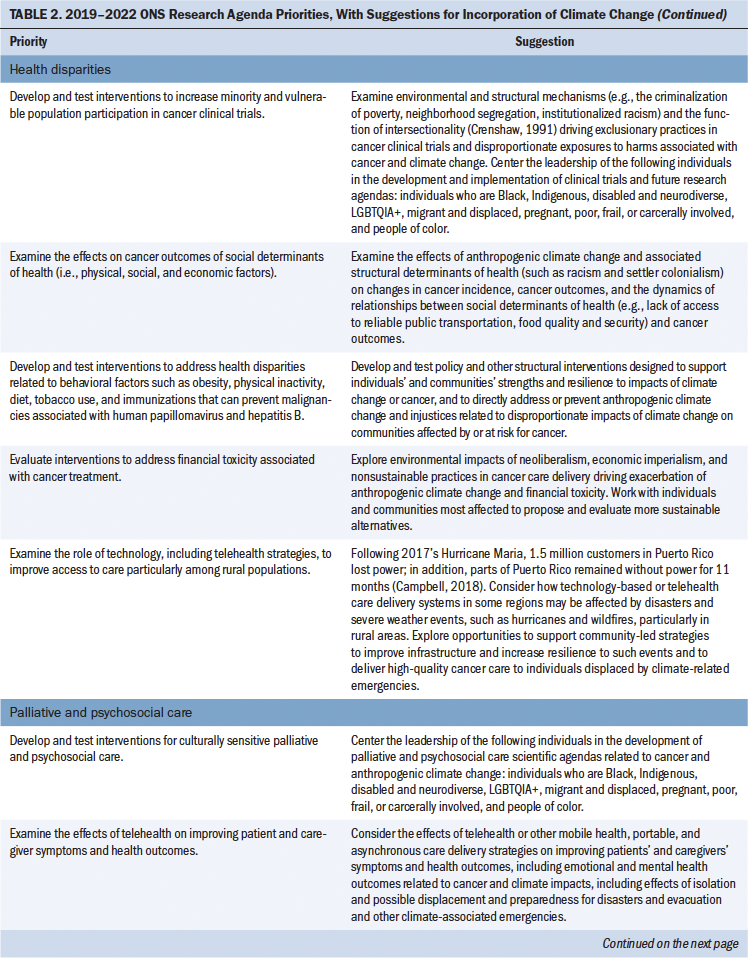
Table 1 describes each of the 10 guiding principles of design justice and their implications for oncology nursing research priority-setting. Using the lens of critical theory, including the 10 principles of design justice, the current authors reviewed the 2019–2022 ONS Research Agenda (Von Ah et al., 2019). The first column of Table 2 displays the research priorities outlined in the original agenda, whereas the second column provides descriptions of the current authors’ corresponding suggestions for immediate incorporation of climate change as a cross-cutting oncology nursing research theme. 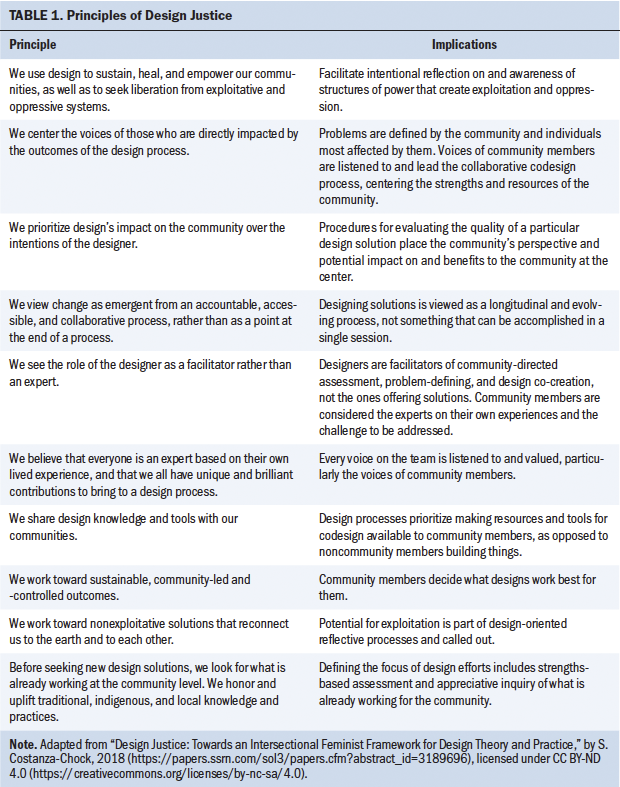
State of the Nursing Science on Climate Change
Nursing science and leadership to address the global climate emergency is rapidly emerging but not fast enough. A 2019 edition of the journal Creative Nursing was dedicated to addressing effects of climate change on health and nursing practice (Huffling, 2019; Kerr et al., 2019; Morgan, 2019; Potter, 2019). Nurse-led organizations, including the Alliance of Nurses for Healthy Environments, the Emergency Nurses Association, and the Public Health Nursing section of the American Public Health Association, have already publicly committed to supporting research, practice, and policy designed to address climate change and climate justice. Related resources created include the WHAM (Work–Home–Adaptation–Mitigation) Grid, which describes actions nurses can take at work and home to address climate change (https://bit.ly/38t7CCI); the Nurses Climate Challenge, which is a campaign to educate health professionals on the effects of climate change on human health (https://nursesclimatechallenge.org) (Demorest et al., 2019); and Climate Change and Health: An Interprofessional Response, a free, open-source health curriculum on climate change (https://globalhealthcenter.umn.edu/education/climatehealth). Measurement science on climate nursing is also evolving. The Climate, Health, and Nursing Tool (CHANT) is a psychometrically validated online survey to measure nurses’ awareness of and engagement with issues pertaining to climate change (https://envirn.org/nurses-climate-survey) (Schenk et al., 2020). 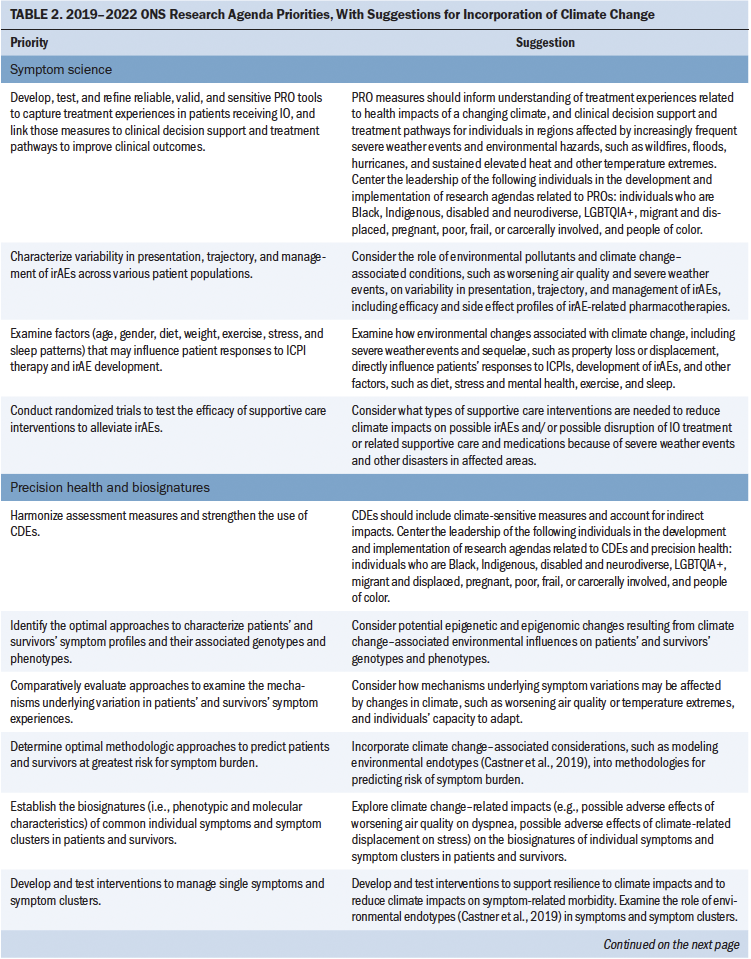

The time is now for climate change to become a cross-cutting theme in every nursing research agenda. Indeed, oncology nurses can and must support science, practice, and policy that contributes to mitigation of climate change and increased resilience to related effects, improving the care and quality of life for individuals with cancer and other vulnerable groups across the globe. The reality of climate change necessitates the creation of a new vision for oncology nursing research, one that (a) begins by acknowledging societal structures of power and oppression that render privilege and relative protection to some while placing others directly in harm’s way, (b) centers the voices and leadership of individuals and communities at greatest risk for harm, and (c) promotes resilience and human health by nursing the health of the climate that supports it.
The authors gratefully acknowledge Raeann Leblanc, PhD, DNP, AGPCNP-BC, CHPN, in the College of Nursing at the University of Massachusetts Amherst for their consultation on this article.
About the Author(s)
Rachel K. Walker, PhD, RN, is an associate professor in the College of Nursing at the University of Massachusetts Amherst; Sherily Pereira-Morales, PhD, RNA, is an associate professor in the School of Nursing at the Medical Sciences Campus of the University of Puerto Rico in San Juan; Rachel Kerr, DNP, RN, is the Environmental Health Nurse Fellowship program coordinator for the Alliance of Nurses for Healthy Environments in the School of Nursing at the University of Minnesota in St. Paul; and Elizabeth Schenk, PhD, MHI, RN-BC, FAAN, is a nurse scientist and sustainability coordinator at Providence St. Patrick Hospital in Missoula, MT, and an assistant research professor in the College of Nursing at Washington State University in Spokane, WA. Walker’s work on this article was sponsored, in part, by a Career Catalyst Research Award from Susan G. Komen (CCR16376422) and the UManage Center for Building the Science of Symptom Self-Management (P20NR016599). The opinions presented here are solely those of the authors and do not necessarily represent those of the National Institutes of Health or the Susan G. Komen Foundation. Walker and Schenk contributed to the conceptualization and design. All authors contributed to the manuscript preparation. Walker can be reached at r.walker@umass.edu, with copy to ONFEditor@ons.org.
References
American Meteorological Society. (2020). Explaining extreme events in 2018 from a climate perspective. https://www.ametsoc.org/ams/index.cfm/publications/bulletin-of-the-amer…
Anderson, G.B., Barnes, E.A., Bell, M.L., & Dominici, F. (2019). The future of climate epidemiology: Opportunities for advancing health research in the context of climate change. American Journal of Epidemiology, 188(5), 866–872. https://doi.org/10.1093/aje/kwz034
Aranda, K. (2019). The political matters: Exploring material feminist theories for understanding the political in health, inequalities and nursing. Nursing Philosophy, 20(4), e12278. https://doi.org/10.1111/nup.12278
Argüello, T.M. (2016). Fetishizing the health sciences: Queer theory as an intervention. Journal of Gay and Lesbian Social Services, 28(3), 231–244. https://doi.org/10.1080/10538720.2016.1191407
Bailey, Z.D., Krieger, N., Agénor, M., Graves, J., Linos, N., & Bassett, M.T. (2017). Structural racism and health inequities in the USA: Evidence and interventions. Lancet, 389(10077), 1453–1463. https://doi.org/10.1016/S0140-6736(17)30569-X
Barbarin, I. (2019, November 2). Climate Darwinism makes disabled people expendable. Forbes. https://www.forbes.com/sites/imanibarbarin/2019/11/02/climate-darwinism…
Barker, A.J. (2009). The contemporary reality of Canadian imperialism: Settler colonialism and the hybrid colonial state. American Indian Quarterly, 33(3), 325–351. https://doi.org/10.1353/aiq.0.0054
Benevolenza, M.A., & DeRigne, L. (2019). The impact of climate change and natural disasters on vulnerable populations: A systematic review of literature. Journal of Human Behavior in the Social Environment, 29(2), 266–281. https://doi.org/10.1080/10911359.2018.1527739
Benjamin, R. (2019). Race after technology: Abolitionist tools for the New Jim Code. Polity. https://politybooks.com/bookdetail/?isbn=9781509526390
Berry, D.R., & Gross, K.N. (2020). A Black women’s history of the United States. Beacon Press. http://www.beacon.org/A-Black-Womens-History-of-the-United-States-P1524…
Bohman, J. (2005). Critical theory. Stanford Encyclopedia of Philosophy. https://plato.stanford.edu/entries/critical-theory
Broussard, M. (2019). Artificial unintelligence: How computers misunderstand the world. MIT Press. https://mitpress.mit.edu/books/artificial-unintelligence
Campbell, A.F. (2018, August 15). It took 11 months to restore power to Puerto Rico after Hurricane Maria. A similar crisis could happen again. Vox. https://www.vox.com/identities/2018/8/15/17692414/puerto-rico-power-ele…
Castner, J., Amiri, A., Rodriguez, J., Huntington-Moskos, L., Thompson, L.M., Zhao, S., & Polivka, B. (2019). Advancing the symptom science model with environmental health. Public Health Nursing, 36(5), 716–725. https://doi.org/10.1111/phn.12641
Collins, P.H. (1990). Black feminist thought: Knowledge, consciousness, and the politics of empowerment (1st ed.). Routledge.
Costanza-Chock, S. (2018, June 3). Design justice: Towards an intersectional feminist framework for design theory and practice. Proceedings of the Design Research Society 2018. https://ssrn.com/abstract=3189696
Crenshaw, K. (1991). Mapping the margins: Intersectionality, identity politics, and violence against women of color. Stanford Law Review, 43(6), 1241–1299. https://doi.org/10.2307/1229039
Demorest, S., Spengeman, S., Schenk, E., Cook, C., & Weston, H.L. (2019). The Nurses Climate Challenge: A national campaign to engage 5,000 health professionals around climate change. Creative Nursing, 25(3), 208–215. https://doi.org/10.1891/1078-4535.25.3.208
Driscoll, S.D., & Goodman, R. (2019). Emancipatory praxis for cervical cancer health equity in Guatemala. International Journal for Human Caring, 23(1), 71–79. https://doi.org/10.20467/1091-5710.23.1.71
Georges, J.M. (2005). Linking nursing theory and practice: A critical-feminist approach. Advances in Nursing Science, 28(1), 50–57. https://doi.org/10.1097/00012272-200501000-00006
George Washington University Milken Institute School of Public Health. (2018). Project report: Ascertainment of the estimated excess mortality from Hurricane Maria in Puerto Rico. https://publichealth.gwu.edu/sites/default/files/downloads/projects/PRs…
Gibson, A. (2019). Climate change for individuals experiencing homelessness: Recommendations for improving policy, research, and services. Environmental Justice, 12(4), 159–163. https://doi.org/10.1089/env.2018.0032
Gifford, W., Thomas, R., Barton, G., & Graham, I.D. (2019). Providing culturally safe cancer survivorship care with Indigenous communities: Study protocol for an integrated knowledge translation study. Pilot and Feasibility Studies, 26(5), 33. https://doi.org/10.1186/s40814-019-0422-9
Glaser, A. (2019, September 20). Artificial intelligence can’t think without polluting. Slate. https://slate.com/technology/2019/09/artificial-intelligence-climate-ch…
Goodwin, N. (2019, March 15). There is no Planet B: Why climate change is an LGBTQ issue. GLAAD. https://www.glaad.org/amp/no-planet-b-why-climate-change-is-an-lgbtq-is…
Hoegh-Guldberg, O., Jacob, D., Taylor, M., Guillén Bolaños, T., Bindi, M., Brown, S., . . . Zhou, G. (2019). The human imperative of stabilizing global climate change at 1.5°C. Science, 365(6459), eaaw6974. https://doi.org/10.1126/science.aaw6974
Huffling, K. (2019). Building a global movement for health: Nurse leadership on climate change. Creative Nursing, 25(3), 191–194. https://doi.org/10.1891/1078-4535.25.3.191
Intergovernmental Panel on Climate Change. (2018). Global warming of 1.5°C: An IPCC special report on the impacts of global warming of 1.5°C above pre-industrial levels and related global greenhouse gas emission pathways, in the context of strengthening the global response to the threat of climate change, sustainable development, and efforts to eradicate poverty: Summary for policymakers. http://report.ipcc.ch/sr15/pdf/sr15_spm_final.pdf
Kagan, P.N., Smith, M.C., & Chinn, P.L. (Eds.). (2014). Philosophies and practices of emancipatory nursing: Social justice as praxis. Routledge.
Kendi, I.X. (2019). How to be an anti-racist. One World.
Kerr, R., Nerbonne, J.F., & Potter, T. (2019). Sparking a movement for a healthy climate through leadership development. Creative Nursing, 25(3), 216–221. https://doi.org/10.1891/1078-4535.25.3.216
Kim, J. (2018). Settler modernity, debt imperialism, and the necropolitics of the promise. Social Text, 36(2), 41–61. https://doi.org/10.1215/01642472-4362349
Levy, B.S., & Patz, J.A. (2015). Climate change, human rights, and social justice. Annals of Global Health, 81(3), 310–322. https://doi.org/10.1016/j.aogh.2015.08.008
Lundquist, D.M., Berry, D.L., Boltz, M., DeSanto-Madeya, S.A., & Grace, P.J. (2019). Wearing the mask of wellness: The experience of young women living with advanced breast cancer. Oncology Nursing Forum, 46(3), 329–337. https://doi.org/10.1188/19.ONF.329-337
Martinez-Sánchez, O. (2018). Impacts from hurricanes Irma and María in the Caribbean [Sidebar 7.1]. Bulletin of the American Meteorological Society, 99(8, Suppl.), S202–S203. https://doi.org/10.1175/2018BAMSStateoftheClimate.1
Mayer, D.K., & McCabe, M. (2013). Climate change and cancer care. Clinical Journal of Oncology Nursing, 17(3), 231–232. https://doi.org/10.1188/13.CJON.231-232
McCarthy, G., & Bernstein, A. (2019). Combating EPA rollbacks—Health care’s response to a retreat on climate. New England Journal of Medicine, 381(8), 696–698. https://doi.org/10.1056/NEJMp1909643
McDermott-Levy, R., Kolanowski, A.M., Fick, D.M., & Mann, M.E. (2019). Addressing the health risks of climate change in older adults. Journal of Gerontological Nursing, 45(11), 21–29. https://doi.org/10.3928/00989134-20191011-04
McNamara, A. (2020, January 2). Australia fires: 5 questions answered. CBS News. https://www.cbsnews.com/news/australia-fires-fire-map-5-questions-answe…
Morgan, R.E. (2019). Determined action to tackle health determinants: A collaborative response to the challenge of climate change mitigation in practice settings. Creative Nursing, 25(3), 195–200. https://doi.org/10.1891/1078-4535.25.3.195
Mosqueda-Díaz, A., Vílchez-Barboza, V., Valenzuela-Suazo, S., & Sanhueza-Alvarado, O. (2014). Critical theory and its contribution to the nursing discipline. Investigación y Educación en Enfermería, 32(2), 356–363. https://doi.org/10.17533/udea.iee.v32n2a18
Mrkusic, M., & Gross, D.A. (2018, December 5). Incarcerated people remain vulnerable to the worst ravages of a warming world. NOVA Next. https://www.pbs.org/wgbh/nova/article/climate-change-mass-incarceration…
Noble, S.U. (2018). Algorithms of oppression: How search engines reinforce racism. NYU Press.
Nix, M., & Caldwell, D. (2018). Natural disasters: A Louisiana gulf perspective of maintaining patient care. Clinical Journal of Oncology Nursing, 22(4), 460–463. https://doi.org/10.1188/18.CJON.460-463
Potter, T. (2019). Planetary health: The next frontier in nursing education. Creative Nursing, 25(3), 201–207. https://doi.org/10.1891/1078-4535.25.3.201
Ramvi, E., & Ueland, V.I. (2019). Between the patient and the next of kin in end-of-life care: A critical study based on feminist theory. Nursing Ethics, 26(1), 201–211. https://doi.org/10.1177/0969733016688939
Salas, R.N., Malina, D., & Solomon, C.G. (2019). Prioritizing health in a changing climate. New England Journal of Medicine, 381(8), 773–774. https://doi.org/10.1056/NEJMe1909957
Schenk, E.C., Cook, C., Demorest, S., & Burduli, E. (2020). CHANT: Climate, Health, and Nursing Tool: Item development and exploratory factor analysis. In E.C. Schenk (Ed.), Annual review of nursing research: Vol. 38. Nursing perpectives on environmental health (pp. 97–111). Springer Publishing Company.
Schweitzer, M.D., Calzadilla, A.S., Salamo, O., Sharifi, A., Kumar, N., Holt, G., . . . Mirsaeidi, M. (2018). Lung health in era of climate change and dust storms. Environmental Research, 163, 36–42. https://doi.org/10.1016/j.envres.2018.02.001
Shrubsole, G. (2015). All that is solid melts into air: Climate change and neoliberalism. Soundings, 59, 115–128. https://doi.org/10.3898/136266215814890486
Shultz, J.M., Kossin, J.P., Shepherd, J.M., Ransdell, J.M., Walshe, R., Kelman, I., & Galea, S. (2019). Risks, health consequences, and response challenges for small-island-based populations: Observations from the 2017 Atlantic hurricane season. Disaster Medicine and Public Health Preparedness, 13(1), 5–17. https://doi.org/10.1017/dmp.2018.28
Sorenson, C., & Garcia-Trabanino, R. (2019). A new era of climate medicine—Addressing heat-triggered renal disease. New England Journal of Medicine, 381(8), 693–696. https://doi.org/10.1056/NEJMp1907859
U.S. Global Change Research Program. (2018). Fourth national climate assessment: Vol. II. Impacts, risks, and adaptation in the United States. https://nca2018.globalchange.gov
Veenema, T.G., Rush, Z., DePriest, K., & McCauley, L. (2019). Climate change-related hurricane impact on Puerto Rico and the U.S. Virgin Islands, environment risk reduction, and the social determinants of health. Nursing Economic$, 37(1), 13–22.
Von Ah, D., Brown, C.G., Brown, S.J., Leak Bryant, A., Davies, M., Dodd, M., . . . Cooley, M.E. (2019). Research agenda of the Oncology Nursing Society: 2019–2022. Oncology Nursing Forum, 46(6), 654–669. https://doi.org/10.1188/19.ONF.654-669
Waldman, S. (2017, December 14). Global warming tied to Hurricane Harvey. Scientific American. https://www.scientificamerican.com/article/global-warming-tied-to-hurri…
Watts, N., Amann, M., Ayeb-Karlsson, S., Belesova, K., Bouley, T., Boykoff, M., . . . Costello, A. (2018). The Lancet Countdown on health and climate change: From 25 years of inaction to a global transformation for public health. Lancet, 391(10120), 581–630. https://doi.org/10.1016/S0140-6736(17)32464-9
World Health Organization. (2018). Climate change and health. https://www.who.int/news-room/fact-sheets/detail/climate-change-and-hea…
Zhu, Y., Koleck, T.A., Bender, C.M., & Conley, Y.P. (2019). Genetic underpinnings of musculoskeletal pain during treatment with aromatase inhibitors for breast cancer: A biological pathway analysis. Biological Research for Nursing. Advance online publication. https://doi.org/10.1177/1099800419895114

