Effects of Educational Interventions in Facilitating Mammography Screening Among Asian American Women: A Meta-Analysis
Problem Identification: This meta-analysis evaluated the effects of various types of educational interventions on increasing breast cancer screening uptake among Asian American women.
Literature Search: Web of Science, MEDLINE®, PubMed®, and Cochrane Library were searched for randomized controlled trials published from 2010 to 2020 of interventions developed to promote mammography uptake among Asian American women.
Data Evaluation: A random-effects model was used to estimate pooled effect sizes using relative risk measures. A funnel plot was used to assess publication bias.
Synthesis: Seven studies were included in this review. Educational interventions identified were primarily culturally sensitive approaches combined with access-enhancing, individually tailored, or group-based approaches. The interventions were effective at increasing the receipt of mammography.
Implications for Nursing: This review provides insight into the importance of combining other approaches with educational interventions to increase their effectiveness for Asian American women. Future interventions can incorporate various approaches to enhance the ability of Asian American women to overcome barriers to breast cancer screening.
Jump to a section
Breast cancer is the most frequently diagnosed cancer, accounting for an estimated 31% of new cancer cases and 15% of cancer deaths among U.S. women every year (Siegel et al., 2023). To lower the risk of dying from breast cancer, the American Cancer Society (ACS, 2021) and other leading health organizations suggest that women with an average risk of breast cancer have a mammogram at age 45 years or as early as age 40 years (Society of Breast Imaging, 2022). Increased awareness and participation in mammography screening can help women to identify breast cancer at an early stage, which, in turn, can improve survival through the availability of more treatment options at the time of diagnosis (ACS, 2021). However, despite the known benefits of early mammography screening, the potential for improved mortality and survival rates has not manifested in populations of Asian American women.
Asian American women have the lowest rate of mammography use across all U.S. racial and ethnic groups because of various barriers (ACS, 2019, 2022). The following types of barriers specific to mammography screening in Asian women have been identified: (a) economic (e.g., lower socioeconomic status, lack of insurance); (b) social (e.g., lack of recommendation and support for screening from physicians, family, and friends); (c) knowledge (e.g., misconceptions about cancer, lack of knowledge about breast cancer and the importance of screening); (d) logistical (e.g., lower English proficiency, extended wait times during mammography visits); and (e) emotional (e.g., fears, feelings of embarrassment) (Lu et al., 2012). Although these barriers are experienced similarly among multiple underserved groups in the United States, the strong cultural views held by Asian American women, including fatalism and modesty, may exacerbate other barriers to breast cancer screening behaviors, particularly among older Asian American women (Jang et al., 2021; Liang et al., 2009). According to Liang et al. (2004), a sense of fatalism about health may lead Chinese immigrants to believe that their life expectancy is predetermined. To offset the possibility of having a life-threatening disease such as cancer, Asian women may believe that practicing healthy habits, including a healthy diet and physical activity, can replace screening to prevent cancer (Heiniger et al., 2015; Liang et al., 2009; Zhang et al., 2020). In addition, modesty in Asian women is rooted in their perspectives about Western medicine. They may prefer Eastern medicine because of fear of the adverse effects of Western medicine or radiation from mammography x-rays (Liang et al., 2004). Traditional views of modesty can also affect choosing only female health professionals to perform mammography screening (Andrews, 2006).
Researchers have addressed Asian American women’s disproportionately lower breast cancer screening rates by developing various types of interventions. To understand the effectiveness of the interventions, two meta-analyses (Han et al., 2009; Legler et al., 2002) examined interventions developed between 1984 and 2008 for women from U.S. ethnic minority groups and revealed that access-enhancing interventions yielded the greatest effect sizes on adherence rates. Individual-directed interventions in healthcare settings (e.g., one-on-one counseling) had the next highest effect size (Han et al., 2009; Legler et al., 2002). When both strategies were used, the intervention effects increased 1.5 times (Legler et al., 2002). From 2000 to date, interventions developed to promote cancer screening have continued to evolve and use diverse strategies to provide tailored programs and/or theory-based and culturally relevant materials in community settings. A conceptual model that was developed based on interventions published between 1999 and 2017 suggested that mammography screening interventions should address individual factors, including Asian American women’s sociodemographic characteristics, cultural views, knowledge and attitude about mammography, and health history because each is related to intervention effectiveness (Jang et al., 2021). Chan and So (2015) indicated that about 80% of breast and cervical cancer screening interventions developed between 2002 and 2014 used more than one intervention strategy to address the various barriers of ethnic minority women. However, despite the evolution of using diverse interventions to facilitate mammography screening for Asian American women during the past decade, meta-analyses identifying whether these newly developed mammography screening interventions resulted in better effects are lacking. Therefore, the purpose of this study was to identify randomized controlled trials published from 2010 to 2020 of educational interventions for Asian American women aimed at increasing breast cancer screening and to estimate the effects of the interventions.
Methods
Study Selection
PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines were followed to perform this meta-analysis. To estimate the effects of existing interventions on Asian American women, a systematic search was conducted in Web of Science, MEDLINE®, PubMed®, and Cochrane Library to identify intervention studies that reported changes in mammography uptake at postintervention. Hand searches from the reference lists of the retrieved studies were also conducted to avoid the possibility of missing eligible studies that were not included in the databases. The study inclusion criteria were as follows: (a) randomized controlled trials, (b) publication from January 2010 through December 2020, (c) interventions specifically developed for Asian American women in the United States, and (d) written in English. Studies were excluded from analysis if they employed a quasi-experimental design, failed to report data concerning differences in mammography uptake at postintervention, or included minority groups other than Asian American women.
When searching MEDLINE and Cochrane Library, specified selection criteria and MeSH (Medical Subject Headings) were used to retrieve the initial pool of potentially eligible studies, including the following combinations: early detection of cancer, Asian Americans, breast neoplasms, mammography, and mammogram. Search terms used for Web of Science included breast cancer (or breast neoplasm) AND Asian American (or Asian American women) AND mammography (or early detection of cancer). The first search was conducted in March 2020 and was updated in June 2021 to identify studies that had been published since that time.
With the assistance of a research librarian who guided the search strategy, two reviewers (L.-T.H.L. and C.-Y.T.) independently extracted potentially relevant studies by screening for titles and abstracts based on the predetermined selection criteria. If a study’s fulfillment of the inclusion criteria could not be determined by the title or abstract, the reviewers further examined the study by reading the full text. However, if the full text did not provide sufficient information, that study was excluded.
During the evaluation of each study, the reviewers used 13 items from the Joanna Briggs Institute’s (2017) critical appraisal tools to help evaluate methodologic qualities, including true randomization used for assignment of participants; allocation concealment (i.e., procedures used to prevent research personnel from knowing which treatment or control group is next in the allocation process); group comparability; blinding procedures for participants, intervention personnel, and outcome assessors; intention-to-treat analyses; outcome measurements; and any deviations from the planned study design. Once all potentially eligible studies were evaluated, each reviewer provided an overall appraisal about whether to include the study in the final analysis. If there was a discrepancy in the perception of eligibility of any study, a consensus meeting was held to further determine that study’s quality and resolve the disagreement.
Selection of Articles
Figure 1 presents the data collection and study selection process, including reasons for exclusion. Initially, 173 potentially eligible studies were identified. Of those, 35 were duplicates. Of the 138 remaining studies, 123 were removed for lack of relevance to the topic of interest, whether for examining different types of cancer and populations or using other types of study designs, such as reviews or cross-sectional designs. The remaining 15 studies were selected for full-text review, and only 7 met the inclusion criteria to be included in the meta-analysis. The other eight articles were excluded for the following reasons: used community-based interventions without randomization (n = 2), did not measure mammography screening (n = 2), were quasi-experimental studies (n = 2), included Pacific Islander participants (n = 1), and reported on a secondary data analysis (n = 1).

The two reviewers’ (L.-T.H.L. and C.-Y.T.) appraisal of the methodologic quality of the studies was consistent regarding the inclusion of the studies in the analysis. All studies presented elements essential to understanding the overall intervention procedures and outcomes using appropriate study design and analysis. The answers to certain items in the Joanna Briggs Institute’s (2017) critical appraisal tools could not be ascertained based on the available information in the studies, which was either lacking or unclear. When reporting procedures of randomization and allocation concealment, only two studies specifically indicated that they used a randomization list or sequentially numbered, opaque, sealed envelopes to implement the participant allocation procedures (Lee, Ghebre, et al., 2017; Lee-Lin et al., 2015). Three of the quality appraisal items were related to blinding procedures for treatment assignment to reduce potential for bias; however, the nature of the interventions seemed not to allow participants or intervention deliverers to be prevented from awareness of treatment assignment. Although this type of limitation could be compensated for by concealing group assignment from the outcome assessors, only one study reported this to be the case (Lee et al., 2014). Two studies provided descriptions of reasons for loss to follow-up but did not explain in detail how incomplete follow-up data were analyzed (Lee et al., 2014; Lee, Ghebre, et al., 2017).
Data Analyses
The primary outcome of interest was the receipt of mammography postintervention. Using relative risk (RR), a preferable measure when an outcome of interest is greater than 10% (Zhang & Yu, 1998), an effect size was calculated for each study. Given the possible sources of heterogeneity arising from Asian American women’s different countries of origin, a random-effects model was used to estimate a single pooled effect size across studies. The goal was to adjust for two possible sources of sampling errors, derived from the sample size within studies and the total number of studies included. This assumption related to heterogeneity was verified by calculating Cochran’s Q statistic, which follows the chi-square distribution with k–1 degrees of freedom. However, given the limited number of studies included in the analysis and to address a limitation inherent in Cochran’s Q statistic, the I2 statistic was calculated. A criterion of 50% was set as a threshold to examine the presence of substantial heterogeneity and the percentage of the variability in effect estimates that resulted from heterogeneity (Higgins et al., 2021).
To visualize the estimated effects, a forest plot was created to provide effect sizes and 95% confidence intervals (CIs) across studies and an overall estimated log RR. Publication bias was also examined by generating a funnel plot with the log of the RR on the horizontal axis and precision (1/standard error) on the vertical axis because the selected studies were all published and identified in the databases. If a noticeably asymmetrical funnel plot was observed, a trim-and-fill method was performed to adjust for potential publication bias because of the lack of feasibility of unpublished results. All analyses were performed using SAS, version 9.4. To provide better visualization, the Meta and Metafor package R was used to create the forest plot and funnel plot.
Results
Study Characteristics
Seven randomized controlled trials published from 2012 to 2017 were included in this meta-analysis. The randomized controlled trials examined three interventions for Chinese American women and four for Korean American women. In total, the studies included 1,157 Chinese American women and 1,129 Korean American women. Sample sizes varied across studies, ranging from 120 to 664 participants per study. All interventions were implemented in community settings. With one exception that compared two experimental groups and one control group (Wang et al., 2012), all studies evaluated the efficacy of an intervention by comparing an experimental group with a control group that received a printed brochure or standard educational information (see Table 1).
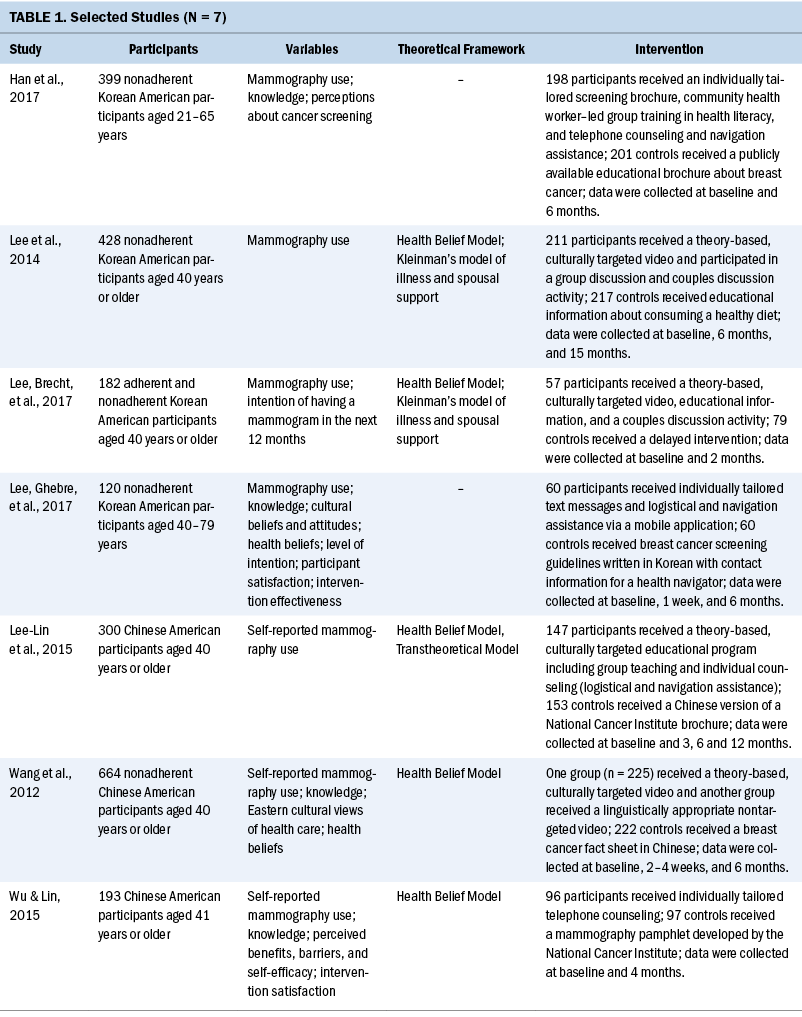
All the interventions were developed primarily to improve participants’ knowledge about breast cancer and address barriers to screening. The studies used different educational methods combined with additional intervention strategies, such as enhancing access to breast cancer screening, providing logistical assistance (Lee-Lin et al., 2015), involving spousal support (Lee, Brecht, et al., 2017; Lee et al., 2014), and/or providing individually tailored counseling sessions, messages, or brochures (Han et al., 2017; Lee, Ghebre, et al., 2017; Lee-Lin et al., 2015; Wu & Lin, 2015). Four interventions that used theory-based tailored approaches were guided by the Health Belief Model (Lee, Brecht, et al., 2017; Lee et al., 2014; Wang et al., 2012; Wu & Lin, 2015). One intervention integrated the Health Belief Model and the Transtheoretical Model to assess Chinese American women’s stages of change toward adopting mammography into breast cancer screening behavior (Lee-Lin et al., 2015).
Regarding the primary outcome of interest, significant increases in the receipt of mammography at follow-up were observed mainly in the interventions that included more than one intervention strategy. However, one study involving only one specific type of educational material delivered via a culturally targeted video was particularly effective among Chinese American women, with low levels of Western acculturation (Wang et al., 2012).
Pooled Results
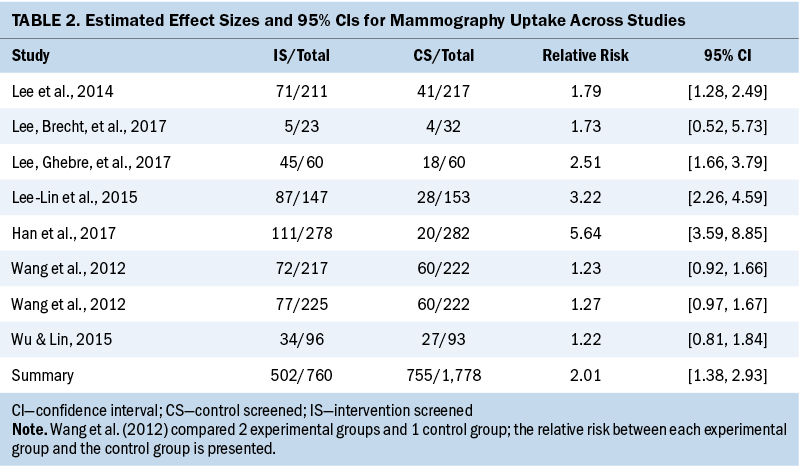
The estimated pooled educational intervention effect and 95% CI, as well as the effect size, were calculated for each study using a random-effects model. The RR of the pooled estimate was 2.01 (95% CI [1.38, 2.93]), indicating that, in general, the educational interventions were effective at increasing mammography receipt among Asian American women (see Table 2). A significant Cochran’s Q statistic of 53.75 (degrees of freedom = 7, p < 0.05), as well as 87% of the total variability in effect sizes measured by I2, showed consistent results regarding the heterogeneity across studies.
Publication Bias
All the included studies were identified through the prespecified databases. To detect publication bias, a funnel plot was assessed for symmetry or asymmetry. The appearance of the funnel plot was symmetrical, suggesting that no publication bias was present.
Discussion
This meta-analysis responded to efforts for reducing health disparities in the United States. Given the changes of using diverse interventions to help improve mammography screening uptake, this study aimed to review randomized controlled trials developed between 2010 and 2020 to understand the effects of educational interventions on mammography uptake among Asian American women. The analysis revealed that educational interventions statistically resulted in about a twofold increase in the likelihood of Chinese and Korean American women receiving a mammogram. Most of the interventions in this review used more than one strategy, and they were primarily culturally targeted combined with access-enhancing, individually tailored, or group-based approaches. In addition, five interventions employed the Health Belief Model, which is tailored to an individual’s knowledge, attitude, and perceptions about mammography. One study combined the Health Belief Model with the Transtheoretical Model to further understand women’s readiness to engage in mammography screening (Lee-Lin et al., 2015). To increase Asian American women’s engagement in mammography screening, interventions can be strengthened by targeting them to individuals’ beliefs and addressing multifaceted barriers to improve effectiveness.
This finding regarding the positive effects of using various intervention strategies is consistent with a previous review that cancer screening interventions developed from 2010 to 2020 incorporated multiple intervention strategies (Chan & So, 2015). In the studies reviewed, culturally targeted interventions were educational interventions that had been used primarily to promote mammography screening for Asian American women. They addressed the common cultural characteristics and barriers Asian American women encounter by providing linguistically and culturally appropriate audiovisual and written information. A systematic review by Zhang et al. (2020) summarized that the culturally targeted interventions are particularly effective for Chinese American women with low acculturation. Another study evaluated a culturally targeted intervention using a video (versus a fact sheet) on how to overcome barriers related to breast cancer screening, in which postintervention mammography receipt was higher among Chinese American women with lower Western acculturation (Wang et al., 2012). Among Chinese American women with higher Western acculturation, the culturally targeted video, a generic video, and the fact sheet all had similar effects (Wang et al., 2012). However, Zhang et al. (2020) indicated that culturally targeted interventions that involved cultural adaptation in language only and cancer-related knowledge may be insufficient to help Chinese American women overcome barriers related to cultural views. Because of the limited studies included in this review, the differences in the strength of educational interventions among Chinese and Korean American women could not be further examined. However, the findings align with previous studies based on the greater effects of educational interventions observed in Korean American women. As shown by the estimated pooled educational effect for each study, the effects of educational interventions developed for Korean American women are relatively higher than the effects of interventions developed for Chinese American women. Only one intervention that resulted in a greater effect in Chinese American women combined a culturally targeted educational intervention with interactive group discussions to address cultural barriers for mammography screening (Lee-Lin et al., 2015).
Growing evidence suggests that intervention effects can be bolstered by using multiple intervention strategies because they can address barriers across the full spectrum of healthcare access, knowledge, social support, and cultural health beliefs (Legler et al., 2002; Masi et al., 2007; Schueler et al., 2008). The Centers for Disease Control and Prevention (2021) recommend combining different strategies to maximize effects of improving access to breast and cervical cancer screening for underserved women. The findings of this review support the incorporation of multiple intervention strategies to address various barriers, which may result in a better effect on mammography screening uptake. Lee-Lin et al.’s (2015) intervention used the following three strategies: (a) interactive group discussions using materials based on the Transtheoretical Model to improve knowledge and address cultural barriers, (b) telephone counseling, and (c) logistical assistance to navigate the healthcare system. This intervention led to a relatively stronger effect on mammography uptake than the other interventions in the included studies. A positive effect, although relatively smaller, was observed in the study’s control group, which received a printed Chinese version of a brochure developed by the National Cancer Institute, which provided information about what a mammogram is, who needs to get a mammogram, how a mammogram works, and where to go to receive a mammogram (Lee-Lin et al., 2015). Greater effects were also observed in an intervention that provided screening brochures, group training, and navigation assistance to Korean American women to increase mammography uptake (Han et al., 2017). A conceptual framework developed by Jang et al. (2021) suggested that healthcare accessibility and availability are important factors in the success of a mammography screening intervention for Asian American women. These results exemplify the necessity of providing Asian American women with educational interventions that use multiple strategies to incorporate navigation assistance and culturally sensitive information so that Asian American women receive support that addresses multilevel barriers.
The findings of this review are contrary to those of a previous meta-analysis, which suggested that mammography uptake among Asian and Pacific Islander Americans could not be improved through educational interventions (Han et al., 2009). These inconsistent results could be because of advances in the technology used for educational interventions. When compared to educational interventions developed prior to 2010, which primarily used classroom instruction to teach a group of participants, interventions developed after 2010 had options for delivery via different platforms, including mobile applications, websites, and classroom instruction, to meet individuals’ needs. Of note, the earlier meta-analysis identified only five interventions for Asian American women, including Vietnamese, Korean, Filipino, and Samoan American women. The interventions in the current review were entirely developed for Korean or Chinese American women. The heterogeneity among Asian American cultures and experiences, as well as the different inclusion criteria used for each meta-analysis, may not allow a direct comparison of the estimated effect sizes. Despite their inconsistencies, the current study and the meta-analysis by Han et al. (2009) both found that culturally sensitive interventions showed a positive effect in underserved populations.
Limitations
This review included only seven randomized controlled trials. Because of the exclusive study samples examined and the restrictions used in the search, the findings derived from this meta-analysis may not generalize to other groups of Asian American women. In addition, subgroup analyses could not be performed with substantial credibility because of the small number of studies. However, the number and types of interventions developed for Asian American women have been insufficient to address the heterogeneity within this population. In fact, during the past 36 years, two meta-analyses (Han et al., 2009; Legler et al., 2002) and the current study have consistently identified only a very small number of interventions (three, five, and seven, respectively) aimed at addressing breast cancer disparities affecting Asian American women. The paucity of the evidence not only signifies that attention to these disparities has been overdue and overlooked, but also suggests the importance of disaggregating data to show which Asian American populations have the greatest need for increased screening. Without addressing the diversity of this population and the specific barriers experienced by each subgroup, the disparities in health burden from cancer may persist or even increase. A final limitation of this analysis is that most studies relied on participant responses as the primary method to confirm receipt of mammography.
Implications for Nursing
Nurses are at the forefront of health promotion to address the importance of cancer screening. Oncology nurses can use multiple educational intervention strategies to address multilevel barriers for Chinese and Korean American women. However, because there are more than 20 cultures encompassed by those who identify as Asian American (Abrams, 2019), nurses and other healthcare professionals should recognize the uniqueness and heterogeneity of Asian Americans. For example, overall breast cancer mortality trends for Asian American women gradually decreased from 2003 to 2011; however, Filipino American women had an increase during the same period (Thompson et al., 2016). Oncology nurses and nurse scientists should be aware of the differences among various ethnic groups. When developing educational interventions or cancer awareness campaigns to promote breast cancer screening, nurses can target distinct barriers for each subgroup in the United States. When possible, nurses can collaborate with public health professionals and community members who are familiar with Eastern culture to reveal which strategies should be incorporated in the campaigns to reach more Asian American women. Because the ultimate goal is to help Asian American women increase their cancer screening uptake, nurses who serve as health navigators can be incorporated in the outreach programs to boost cancer screening, particularly for hard-to-reach populations, to provide culturally sensitive services.

Conclusion
The findings of this meta-analysis provide essential directions for developing educational interventions to increase mammography uptake among Asian American women. Future research that considers the feasibility of an intervention and the resources needed to reach out to a greater number of Asian American women eligible for cancer screening can increase success by embracing multiple innovative intervention strategies, including culturally and linguistically targeted teaching materials, as well as logistical assistance. Lastly, the limited number of interventions for Asian American women identified in this review suggests that oncology nurses, public health practitioners, and nursing scientists must continuously work to address cancer disparities affecting Asian American individuals and ultimately provide effective and sustainable interventions to achieve better health outcomes in the United States.
About the Authors
Li-Ting Huang Longcoy, PhD, DrPH, RN, is a postdoctoral fellow in the College of Nursing at the University of Illinois, Chicago; Chun-Yi Tai, PhD, RN, is an associate professor in the School of Nursing at the National Taipei University of Nursing and Health Sciences in Taipei City, Taiwan; Joshua Longcoy, MPH, is a statistician in the Center for Community Health Equity at Rush University Medical Center in Chicago, IL; Judy Huei-yu Wang, PhD, is an associate professor in the Lombardi Comprehensive Cancer Center at Georgetown University Medical Center in Washington, DC; and Jingjing Yin, PhD, is an associate professor of biostatistics, Logan Cowan, PhD, MPH, is an associate professor, and Kelly L. Sullivan, PhD, FACE, FRSPH, is an associate professor, all in the Jiann-Ping Hsu College of Public Health at Georgia Southern University in Statesboro. This research was supported, in part, by National Cancer Institute training grants from the Cancer Education and Career Development Program (T32CA057699). L.-T.H. Longcoy, Tai, Wang, Cowan, and Sullivan contributed to the conceptualization and design. L.-T.H. Longcoy and Tai completed the data collection. J. Longcoy, and Yin provided statistical support. J. Longcoy, Yin, and Cowan provided the analysis. All authors contributed to the manuscript preparation. Tai can be reached at yii@ntunhs.edu.tw, with copy to ONFEditor@ons.org. (Submitted February 2022. Accepted September 23, 2022.)
References
Abrams, Z. (2019, December 1). Countering stereotypes about Asian Americans. American Psychological Association. https://www.apa.org/monitor/2019/12/countering-stereotypes
American Cancer Society. (2019). Breast cancer facts and figures, 2019–2020. https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and…
American Cancer Society. (2021). Cancer facts and figures, 2021. https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and…
American Cancer Society. (2022). Breast cancer facts and figures, 2022–2024. https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and…
Andrews, C.S. (2006). Modesty and healthcare for women: Understanding cultural sensitivities. Community Oncology, 3(7), 443–446. http://doi.org/10.1016/S1548-5315(11)70732-X
Centers for Disease Control and Prevention. (2021). Resources to share. U.S. Department of Health and Human Services. https://www.cdc.gov/cancer/nbccedp/resources/index.htm
Chan, D.N.S., & So, W.K.W. (2015). A systematic review of randomised controlled trials examining the effectiveness of breast and cervical cancer screening interventions for ethnic minority women. European Journal of Oncology Nursing, 19(5), 536–553. https://doi.org/10.1016/j.ejon.2015.02.015
Han, H.-R., Lee, J.-E., Kim, J., Hedlin, H.K., Song, H., & Kim, M.T. (2009). A meta-analysis of interventions to promote mammography among ethnic minority women. Nursing Research, 58(4), 246–254. https://doi.org/10.1097/nnr.0b013e3181ac0f7f
Han, H.-R., Song, Y., Kim, M., Hedlin, H.K., Kim, K., Lee, H.B., & Roter, D. (2017). Breast and cervical cancer screening literacy among Korean American women: A community health worker–led intervention. American Journal of Public Health, 107(1), 159–165. https://doi.org/10.2105/ajph.2016.303522
Heiniger, L.E., Sherman, K.A., Shaw, L.-K.E., & Costa, D. (2015). Fatalism and health promoting behaviors in Chinese and Korean immigrants and Caucasians. Journal of Immigrant and Minority Health, 17(1), 165–171. https://doi.org/10.1007/s10903-013-9922-5
Higgins, J.P.T., Thomas, J., Chandler, J., Cumpston, M., Li, T., Page, M.J., & Welch, V.A. (Eds.). (2021). Cochrane Handbook for Systematic Reviews of Interventions version 6.2. Cochrane. https://training.cochrane.org/handbook/archive/v6.2
Jang, M.K., Chung, D.W., Hamlish, T., Rhee, E., Mathew, A., Li, H., & Doorenbos, A.Z. (2021). Factors influencing mammography uptake following a screening intervention among Asian American women: A systematic review. Journal of Immigrant and Minority Health, 23(6), 1293–1304. https://doi.org/10.1007/s10903-021-01172-0
Joanna Briggs Institute. (2017). The Joanna Briggs Institute critical appraisal tools for use in JBI systematic reviews: Checklist for randomized controlled trials. https://jbi.global/sites/default/files/2019-05/JBI_RCTs_Appraisal_tool2…
Lee, E.E., Brecht, M.-L., Park, H., Lee, J., & Oh, K.M. (2017). Web-based study for improving mammography among Korean American women. Journal of Cancer Education, 32(2), 257–263. https://doi.org/10.1007/s13187-015-0920-2
Lee, E., Menon, U., Nandy, K., Szalacha, L., Kviz, F., Cho, Y., . . . Park, H. (2014). The effect of a couples intervention to increase breast cancer screening among Korean Americans. Oncology Nursing Forum, 41(3), E185–E193. https://doi.org/10.1188/14.ONF.e185-e193
Lee, H., Ghebre, R., Le, C., Jang, Y.J., Sharratt, M., & Yee, D. (2017). Mobile phone multilevel and multimedia messaging intervention for breast cancer screening: Pilot randomized controlled trial. JMIR MHealth UHealth, 5(11), e154. https://doi.org/10.2196/mhealth.7091
Lee-Lin, F., Nguyen, T., Pedhiwala, N., Dieckmann, N., & Menon, U. (2015). A breast health educational program for Chinese-American women: 3-to 12-month postintervention effect. American Journal of Health Promotion, 29(3), 173–181. https://doi.org/10.4278/ajhp.130228-quan-91
Legler, J., Meissner, H.I., Coyne, C., Breen, N., Chollette, V., & Rimer, B.K. (2002). The effectiveness of interventions to promote mammography among women with historically lower rates of screening. Cancer Epidemiology, Biomarkers and Prevention, 11(1), 59–71.
Liang, W., Wang, J., Chen, M.-Y., Feng, S., Yi, B., & Mandelblatt, J.S. (2009). Cultural views, language ability, and mammography use in Chinese American women. Health Education and Behavior, 36(6), 1012–1025. https://doi.org/10.1177/1090198109331669
Liang, W., Yuan, E., Mandelblatt, J.S., & Pasick, R.J. (2004). How do older Chinese women view health and cancer screening? Results from focus groups and implications for interventions. Ethnicity and Health, 9(3), 283–304. https://doi.org/10.1080/1355785042000250111
Lu, M., Moritz, S., Lorenzetti, D., Sykes, L., Straus, S., & Quan, H. (2012). A systematic review of interventions to increase breast and cervical cancer screening uptake among Asian women. BMC Public Health, 12, 413. https://doi.org/10.1186/1471-2458-12-413
Masi, C.M., Blackman, D.J., & Peek, M.E. (2007). Interventions to enhance breast cancer screening, diagnosis, and treatment among racial and ethnic minority women. Medical Care Research and Review, 64(5, Suppl.), 195S–242S. https://doi.org/10.1177/1077558707305410
Schueler, K.M., Chu, P.W., & Smith-Bindman, R. (2008). Factors associated with mammography utilization: A systematic quantitative review of the literature. Journal of Women’s Health, 17(9), 1477–1498. https://doi.org/10.1089/jwh.2007.0603
Siegel, R.L., Miller, K.D., Wagle, N.S., & Jemal, A. (2023). Cancer statistics, 2023. CA: A Cancer Journal for Clinicians, 73(1), 17–48. https://doi.org/10.3322/caac.21763
Society of Breast Imaging. (2022). Things to know about breast imaging. https://www.sbi-online.org/end-the-confusion/things-to-know-about-breas…
Thompson, C.A., Gomez, S.L., Hastings, K.G., Kapphahn, K., Yu, P., Shariff-Marco, S., . . . Palaniappan, L.P. (2016). The burden of cancer in Asian Americans: A report of national mortality trends by Asian ethnicity. Cancer Epidemiology, Biomarkers and Prevention, 25(10), 1371–1382. https://doi.org/10.1158/1055-9965.EPI-16-0167
Wang, J.H.-Y., Schwartz, M.D., Brown, R.L., Maxwell, A.E., Lee, M.M., Adams, I.F., & Mandelblatt, J.S. (2012). Results of a randomized controlled trial testing the efficacy of a culturally targeted and a generic video on mammography screening among Chinese-American immigrants. Cancer Epidemiology, Biomarkers and Prevention, 21(11), 1923–1932. https://doi.org/10.1158/1055-9965.epi-12-0821
Wu, T.-Y., & Lin, C. (2015). Developing and evaluating an individually-tailored intervention to increase mammography adherence among Chinese American women. Cancer Nursing, 38(1), 40–49. https://doi.org/10.1097/ncc.0000000000000126
Zhang, J., & Yu, K.F. (1998). What’s the relative risk? A method of correcting the odds ratio in cohort studies of common outcomes. JAMA, 280(19), 1690–1691. https://doi.org/10.1001/jama.280.19.1690
Zhang, X., Li, P., Guo, P., Wang, J., Liu, N., Yang, S., . . . Zhang, W. (2020). Culturally tailored intervention to promote mammography screening practice among Chinese American Women: A systematic review. Journal of Cancer Education, 35(6), 1052–1060. https://doi.org/10.1007/s13187-020-01730-4




