Strain Among Caregivers of Older Adults Diagnosed With Breast Cancer
Objectives: To illustrate the predictors of strain among caregivers of older adults diagnosed with breast cancer.
Sample & Setting: This study involved 39 women diagnosed with breast cancer who were aged 69 years or older, receiving any type of treatment, and seeking an initial assessment in a geriatric oncology program at a large cancer center in the midwestern United States and their caregivers.
Methods & Variables: This cross-sectional study evaluated relationships among the variables of caregiver strain, age, employment status, patient characteristics, and patient scores on the comprehensive geriatric assessment. Bivariate statistics and logistic regression models were used.
Results: Increasing age of the caregiver was associated with less caregiver strain. Caregivers employed part-time experienced greater strain than those employed full-time.
Implications for Nursing: Nurses must assess for strain in caregivers of individuals diagnosed with cancer, particularly if they are younger and employed part-time. Caregivers of depressed patients should be assessed for strain and offered support.
Jump to a section
About 34 million Americans have provided unpaid caregiver support to an adult aged 50 years or older (National Alliance for Caregiving & AARP Public Policy Institute, 2015). Nearly 1 in 10 caregivers in the United States is aged 75 years or older; in addition, caregivers tend to be women and, on average, provide more than 34 hours of care per week for a length of 5.6 years (National Alliance for Caregiving & AARP Public Policy Institute, 2015). The average age of a caregiver in the United States is 49.2 years (National Alliance for Caregiving & AARP Public Policy Institute, 2015). Individuals aged from 45 to 64 years are most likely to be caregivers and commonly provide companionship, physical care, help with household repairs, and assistance with housework (Stepler, 2015). Caregivers of individuals with cancer are often unpaid and have wide-ranging roles, including the provision of emotional support and daily care, as well as the coordination of cancer care (American Cancer Society, 2016).
Caregivers often experience strain, which refers to the emotional and physical demands associated with providing care, particularly when the needs exceed the resources (Oncology Nursing Society, 2017). Burden is the perception of emotional, physical, social, and financial suffering because of the caregiver role (Zarit, Todd, & Zarit, 1986) and generally affects the mental health of the caregiver of an individual with cancer (Große, Treml, & Kersting, 2018). Strain and burden have similar effects on health, coping, well-being, sleep, social support, and other quality-of-life concerns that affect individuals with cancer and their caregivers (Berglund, Lytsy, & Westerling, 2015; Johansen, Cvancarova, & Ruland, 2018; Litzelman et al., 2015; Yang, Hao, George, & Wang, 2012). Strain can be a force that produces burden (Chen & Hu, 2002; Johansen et al., 2018; Thornton & Travis, 2003). Caregiver burden and strain are terms that describe many similar concepts and are often used together to describe the challenges of caregiving (Chen & Hu, 2002).
The caregiver is typically the invisible person in the patient–caregiver dyad, in that many of the caregiver’s concerns remain undetected and unaddressed (Adelman, Tmanova, Delgado, Dion, & Lachs, 2014). Caregivers of patients diagnosed with advanced cancer often fail to maintain self-care and report high levels of depression and anxiety (Dionne-Odom et al., 2017). Depending on the health of the patient, levels of caregiver strain can worsen and affect the caregiver’s quality of life, which can diminish over the course of an illness (Hsu et al., 2014; Stall et al., 2019). Caregiver strain and burden affect patient hospital readmissions (Bonin-Guillaume et al., 2015) and increase risk of caregiver morbidity and mortality (Aggarwal, Liao, Christian, & Mosca, 2009).
Theoretical frameworks or models exist that identify characteristics of the caregiver and the care recipient that predict caregiver strain (Northouse et al., 2013; Reblin, Small, Jim, Weimer, & Sherwood, 2018; Sherwood et al., 2004). Common care recipient characteristics used to describe caregiver strain include age (Goldzweig et al., 2019), type of illness (Schulz et al., 2008), functional status (Hsu et al., 2017; Russell et al., 2016), mood (Sacher, Meixensberger, & Krupp, 2018), fatigue (Poort et al., 2016), nutritional status (Tana et al., 2019), cognitive status (Rajasekaran et al., 2016), and pain (Porter et al., 2019). Using comprehensive geriatric assessment (CGA) to predict caregiver strain is supported in the literature (Rajasekaran et al., 2016). Common caregiver factors related to strain include employment status (Hsu et al., 2014), age (Ge & Mordiffi, 2017), and health (Kelley, Kent, Litzelman, Mollica, & Rowland, 2019). It is important for nurses to recognize risk factors associated with caregiver strain and burden to proactively provide support and access to necessary referrals (Adelman et al., 2014). However, caregiver strain and burden are often not part of the routine nursing assessment and can go undetected.
The purpose of this descriptive research is to determine the predictors of strain among caregivers of older adults diagnosed with breast cancer. The following aims were addressed:
• Describe the relationship among caregiver strain and the caregiver characteristics of age, employment status, caregiving recipient, perception of heath, and status of being the only caregiver to the individual who has been diagnosed with cancer.
• Describe the relationship among caregiver strain and patient stage of cancer, functional and cognitive status, depression, pain, fatigue, and nutritional status.
• Determine the predictors of caregiver strain among individuals who are diagnosed with cancer and caregiver characteristics.
There are two types of caregivers: formal and informal. Formal caregivers are paid care providers who work in the home or in an outside caregiving setting (e.g., long-term care facility, residential facility). In contrast, many caregivers are family members and are considered informal caregivers who are unpaid and have some personal connection to the person in need (American Cancer Society, 2016; Family Caregiver Alliance, 2016; Given, Sherwood, & Given, 2011). The U.S. Bureau of Labor Statistics defines informal caregivers as anyone aged 15 years or older providing unpaid care to any adult aged 65 years or older in the past three to four months because of an age-related condition (Stepler, 2015).
Informal caregivers are often untrained and unprepared to manage care of a person at home and frequently do not have the necessary resources to do so (Bove, Zakrisson, Midtgaard, Lomborg, & Overgaard, 2016). For caregivers of individuals with cancer, the range and intensity of disease- and treatment-associated symptoms and toxicities can be robust and require a great deal of attention, experience, and support, particularly with some targeted therapies (Kent et al., 2016). Informal caregiving can be associated with social isolation because of the high demands of the role and little or no respite (Kuluski et al., 2018); over time, this can affect the health and wellness of the patient–caregiver dyad (Given, Given, & Sherwood, 2012).
Lack of respite affects the mental and physical health of the informal caregiver by interfering with exercise, personal time, employment, social relationships, and a nutritious diet (Tatangelo, McCabe, Macleod, & You, 2018). Many informal caregivers make extended changes to employment, particularly if the person who is diagnosed with cancer is receiving chemotherapy or undergoing transplantation (de Moor et al., 2017); this can result in many financial concerns (Zafar et al., 2013).
Background
Caregiver Strain
Caregiving can yield strong relationships (Bangerter, Griffin, & Dunlay, 2019; Mosher, Bakas, & Champion, 2013); however, the role can consist of complex, inconvenient, and unpleasant tasks. Responsibilities of caregivers often include administering medication, facilitating tube feeding, monitoring symptoms, recognizing deterioration, and assessing for treatment-related effects (Ullgren, Tsitsi, Papastavrou, & Charalambous, 2018). Caregivers of individuals with cancer report difficulty anticipating the needs and expectations of the patient, which often change as a result of cancer treatment and progression. Financial concerns, age, gender, social isolation, and choice to be a caregiver are prime factors associated with strain (Adelman et al., 2014; Ferrell, Kravitz, Borneman, & Taratoot Friedmann, 2018). Providing support beyond one’s emotional and physical capacities often results in problems, such as depression in individuals diagnosed with cancer and their caregivers (Ferrell et al., 2018).
Caregivers often experience burden and strain at various points throughout the caregiving experience and lack support for their own physical and mental needs, which often go unnoticed and untreated (American Psychological Association, n.d.; Ferrell et al., 2018; Fujinami et al., 2015). Many caregivers of individuals with cancer report anxiety associated with medication management, financial concerns, and competing needs of other family members (Haun, Sklenarova, Brechtel, Herzog, & Hartmann, 2014). One year after a diagnosis of cancer, patients tend to report better physical health, as opposed to caregivers who report poorer health (Kim, Shaffer, Carver, & Cannady, 2016). Waiting for surgical procedures often results in elevation of strain and burden for the patient and the caregiver; however, after the procedure, individuals with cancer report a decrease in strain and burden, but caregiver levels of strain and burden remain the same (Kim, Shaffer, et al., 2016).
Caregivers with less experience in caring for a person with cancer report higher burden (Grover, Rina, Malhotra, & Khadwal, 2018), particularly while adapting to the caregiver role (Garlo, O’Leary, Van Ness, & Fried, 2010). Managing symptoms and illness associated with cancer treatment can be stressful for inexperienced caregivers. Caregivers of individuals diagnosed with lung cancer report that burden and anxiety are associated more with patient-reported quality of life than stage of cancer (Borges et al., 2017). For some caregivers, financial concerns and schedule conflicts are a primary source of burden (Hartnett, Thom, & Kline, 2016). In the last year of life of individuals with ovarian cancer, distress and unmet needs increase in caregivers (Butow et al., 2014).
Patient Characteristics Influencing Caregiver Strain and Burden
Among individuals diagnosed with aggressive cancers who screen positive for depression, 73% of these patient–caregiver dyads report severe emotional strain and require psychological support (Sacher et al., 2018). Caregivers of individuals with cancer who require many hours of support for a long duration often report poor mental health (Kent & Dionne-Odom, 2019). In people with cancer who are bedridden, predictors of strain and burden are associated with functional ability, caregiver employment concerns, caregiver health problems, and the ability of the caregiver to maintain health (Bekdemir & Ilhan, 2018). Caregivers of patients with impaired cognitive function tend to report greater burden (Juntunen et al., 2018), and as the patient’s cognitive limitations progress, distress increases (Stall et al., 2019). Poor sleep, reduced physical activity, impairment in immune function, and financial concerns are issues encountered by caregivers of individuals with cancer (Northouse, Williams, Given, & McCorkle, 2012).
Caregivers of individuals with functional impairment, as detected by the Timed Up and Go Test, report greater caregiver burden (Bień-Barkowska, Doroszkiewicz, & Bień, 2017). Severity of cognitive limitations (Black et al., 2018) and extent of comorbidities (Dauphinot et al., 2016) can affect caregiver distress. Poor sleep in patient–caregiver dyads is often experienced midway through chemotherapy treatment (Kotronoulas, Wengström, & Kearney, 2016), and can affect strain and burden. Nutrition and hydration are primary concerns in caregivers of patients at the end of life; this tends to be a source of strain and burden (Baillie et al., 2018). Individuals diagnosed with cancer and caregivers often disagree on the patient extent of functional limitation, with the caregivers reporting higher burden (Hsu et al., 2017).
Supporting the Caregiver
When patient–caregiver dyads are addressed as a unit of care and receive adequate support to cope with and manage the disease, quality of life and self-efficacy can improve (Northouse et al., 2013). Family caregivers and individuals diagnosed with advanced lung cancer tend to benefit from regular contact with professionals offering education and psychosocial support (Badr, Smith, Goldstein, Gomez, & Redd, 2015). Isolation, reduced personal interactions, and little respite can be exhausting to the individual with cancer and to caregivers, which may affect care and relationships and reduce health-related quality of life (Segrin, Badger, & Sikorskii, 2019). Caregivers who experience positive personal interactions and engage socially report less depression (Sibalija, Savundranayagam, Orange, & Kloseck, 2018). Respite services can be helpful in supporting the quality of life of a caregiver (Riekkola, Rutberg, Lilja, & Isaksson, 2018). Nurses and the healthcare team must understand the respite services available in the community and promote their use.
Caregivers often realize the importance of self-care, but it does present a challenge with competing responsibilities (Marcotte, Tremblay, Turcotte, & Michaud, 2019) and reduced personal time (Gomes et al., 2019). Changes in levels of support affect the physical activity of caregivers (Stacey, James, Chapman, & Lubans, 2016). Financially strained caregivers have fewer resources for self-care (Ferrell et al., 2018). Exercise is one important aspect of self-care that may not incur a great deal of cost. Caregiver exercise helps improve health and well-being (Cuthbert et al., 2018). Caregivers who are able to exercise three or more times per week report better physical well-being versus those with fewer than three days of exercise, who report more depression and anxiety (Paek et al., 2018). A pedometer can improve caregiver physical activity and enhance general health and physical functioning (Frensham, Parfitt, & Dollman, 2018). There are many free exercise programs online that can help caregivers participate in exercise without leaving home. Some such resources include the following:
• AARP (www.aarp.org/caregiving/life-balance/info-2017/find-time-for-exercise.html)
• Family Caregiver Alliance (www.caregiver.org/exercise-caregiver-health-and-well-being)
• Go4Life, from the National Institute on Aging at the National Institutes of Health (https://go4life.nia.nih.gov/caregivers-and-exercise-take-time-for-yourself)
Telehealth delivery of wellness or other classes can help support the person with cancer and the caregiver (Karlsen, Moe, Haraldstad, & Thygesen, 2018). Wellness education delivered via telehealth fosters learning, establishes relationships, and is perceived as beneficial by caregivers (Serwe, Hersch, & Pancheri, 2017; Serwe, Hersch, Pickens, & Pancheri, 2017). Telehealth education options can reduce caregiver anxiety and burden (Zheng, Head, & Schapmire, 2016). In many cases, the only technology necessary is a computer with Internet capability.
Many literature reviews of family caregiving among people with cancer have been conducted to better understand how to support family caregivers (Ferrell & Wittenberg, 2017; Frambes, Given, Lehto, Sikorskii, & Wyatt, 2018; Northouse, Katapodi, Song, Zhang, & Mood, 2010). Northouse et al. (2010) reviewed 29 randomized clinical trials involving interventions including psychosocial counseling, education, and skills training, resulting in a small to moderate reduction in caregiver burden. Ferrell and Wittenberg (2017) reviewed 50 caregiver intervention studies; interventions included psychotherapeutic counseling that ranged from one session to multiple sessions during a two-year period, exercise programs, educational programs, ongoing support, and skills training.
Supporting older caregivers compared to younger caregivers may require different interventions. Older caregivers report different barriers to receiving help and support as compared to younger caregivers, in that they may have limited exposure to people who can provide support (LaValley & Gage-Bouchard, 2018). Caregivers of older cancer survivors report higher levels of distress and lower quality of life (Jansen et al., 2018) and express increased burden in caring for patients with cognitive limitations (Besser & Galvin, 2019) as compared to the general population. Younger caregivers may have more resources because they are employed, but they often have less time because of employment. Older caregivers often report no time for physical activity and many other aspects of self-care (Queen, Butner, Berg, & Smith, 2017).
Caregivers of individuals who are diagnosed with cancer fill many roles that can be stressful, causing strain and distress. People diagnosed with severe disease require more intense caregiving, and patients with depression tend to cause strain and burden in caregivers. Financial concerns, employment, and lack of self-care are concerns expressed among caregivers of patients with cancer in the oncology literature, which is similar to issues experienced by caregivers of individuals diagnosed with dementia, stroke, and other serious illnesses.
Methods
This study employed a prospective, descriptive, cross-sectional design and was approved by the Ohio State University Institutional Review Board. Women aged 69 years or older who had been diagnosed with any stage of breast cancer and were receiving any type of treatment (surgery, endocrine therapy, chemotherapy, radiation therapy) and their caregivers who presented to the Senior Adult Oncology Program (SAOP) of the Stefanie Spielman Comprehensive Breast Center at the Ohio State University in Columbus from 2013 through 2018 were invited to participate. All study participants had to be able to read and understand the consent form.
The geriatric nurse practitioner (GNP) obtained written consent from each individual with cancer and her designated caregiver. Cancer diagnosis, staging, and treatment information were obtained from the electronic health record. The GNP administered all eight of the CGA instruments with each participating patient while in the examination room; this required about 20 minutes. CGA instruments consisted of the following:
• Brief Fatigue Inventory (BFI)
• Geriatric Depression Scale (GDS)
• Fall assessment
• Timed Up and Go Test
• Mini-Cog
• Grip strength
• Numeric pain rating scale
• Mini Nutritional Assessment
At the same time, caregivers completed one caregiver instrument, the Modified Caregiver Strain Index (MCSI), which required about five minutes, and answered questions related to age, perceptions of self-health, and employment status. The sample size for this study was dependent on the number of patient–caregiver dyads that completed all the instruments. Thirty-nine dyads, each made up of a patient with cancer and her caregiver, participated in the study. The data collected for this study are part of ongoing CGA data collection and used in clinical research projects and for clinical care and decision making.
Instruments
The nine-item BFI (Mendoza et al., 1999) is an acceptable subjective tool in the measurement of fatigue in individuals with cancer. Each item is rated from 0 (no fatigue) to 10 (extreme fatigue). The BFI is scored as a continuous variable in that the higher the score, the more fatigue. For this study, a cutoff point of mild fatigue can be considered with a total score of 1–3 (Chang et al., 2007; Mendoza et al., 1999). Construct validity was determined using factor analysis for the nine items ranging from 0.81 (usual fatigue) to 0.92 (activity). Cronbach coefficient alphas showed high reliability (greater than 0.95). Concurrent validity was evaluated with the Functional Assessment of Cancer Therapy–Fatigue scale (Cella et al., 1993).
The GDS is a 15-item tool intended to help clinicians screen for depression (Yesavage et al., 1982). Individuals select “yes” or “no” responses for each item, and having five or more items indicating depression is considered to be a positive screen for depression. Validation was shown by comparison to two well-known measures of depression: the Zung Self-Rating Scale for Depression (Cronbach alpha of 0.87) (Zung, Richards, & Short, 1965) and the Hamilton Rating Scale for Depression (Cronbach alpha of 0.9) (Hamilton, 1960).
The gold standard for fall screening is the simple question of whether a fall has occurred in the past six months (American Geriatrics Society, British Geriatrics Society, & American Academy of Orthopaedic Surgeons Panel on Falls Prevention, 2001).
The Timed Up and Go Test (Podsiadlo & Richardson, 1991) considers gait and balance in the ability to rise from a sitting position, ambulate 10 feet, and return to a sitting position. The Timed Up and Go Test has been found to be correlated with falls (Shumway-Cook, Brauer, & Woollacott, 2000). Scores are in seconds; greater length of time required to complete the Timed Up and Go Test indicates greater functional impairment, with 12 or more seconds indicating risk of falling. Test-retest reliability ranges from 0.89 to 0.99. It is highly correlated with other standard measures of performance, such as the Berg Balance Scale (Cronbach alpha of 0.72) (Berg, Wood-Dauphinee, Williams, & Maki, 1992) and the Barthel Index (Cronbach alpha of 0.55) (Collin, Wade, Davies, & Horne, 1988).
The Mini-Cog (Borson, Scanlan, Brush, Vitaliano, & Dokmak, 2000) is a valid and reliable assessment of cognitive limitations that combines the clock-drawing test with a three-item recall. The three-item recall is an assessment of short-term memory and is used as part of the Mini-Mental State Examination (Folstein, Folstein, & McHugh, 1975). The Mini-Cog is recommended by the Hartford Geriatric Nursing Institute and the National Comprehensive Cancer Network (2019) for clinical assessment and patient care. Scoring is calculated for two sections: clock-drawing is scored from 0 (inability to draw the clock) to 2 (ability to draw the clock), and recall is scored from 0 (no recall) to 3 (full recall). A total score of 3 or less (sometimes 2 or less is used as a cutoff point) was used for this study to indicate cognitive impairment. Sensitivity for the Mini-Cog is 0.99 and 0.96 in diagnostic value (Borson et al., 2000). Inter-rater scoring on the clock-drawing portion of the Mini-Cog is 0.97 (Borson et al., 2000).
Grip strength was measured in the right hand using the Jamar® Hydraulic Hand Dynamometer (Patterson Medical, n.d.). Grip strength measurements predict limitations in mobility for patients with breast cancer (Massy-Westropp, Gill, Taylor, Bohannon, & Hill, 2011). Means of scores of three successive trials for the right hand were recorded. Grip strength of 37 kg or less indicates risk of mobility limitation.
A numeric pain rating scale was used to measure pain (McCaffery & Beebe, 1989). Patients were asked to describe their current pain on a scale from 0 (no pain) to 10 (extreme pain). Mild pain was considered to be rated 1–3, 4–6 was considered moderate pain, and 7–10 was considered severe pain. A cutoff point of 3 or greater was used to represent a rating of mild to moderate pain.
The six-item Mini Nutritional Assessment (MNA) is commonly used to assess for malnutrition (Kaiser et al., 2009) and is validated in geriatric patients (—X age of 82 years). Possible scores range from 0 to 14, with normal nutritional status indicated with 12–14 points, risk of malnutrition with 8–11 points, and malnourishment with 0–7 points. The score of 11 had a sensitivity of 90% and a specificity of 76%, with an area under the curve of 95% (Kaiser et al., 2009).
The MCSI (Robinson, 1983; Thornton & Travis, 2003) is a 13-item tool that measures the financial, psychological, personal, physical, and social domains of caregiving. Each item is scored as 0 (never), 1 (sometimes), or 2 (yes). Possible total scores range from 0 to 26, with higher scores indicating greater caregiver strain. Internal reliability via Cronbach alpha is 0.9 (Thornton & Travis, 2003).
Analysis
Descriptive statistics were used to summarize characteristics of the patient with cancer, characteristics of the caregiver, and scores on the assessment instruments. Bivariate tests were used to determine the bivariate relationships of characteristics of the patient with cancer and of the caregiver with caregiver strain using correlation statistics for continuous variables (e.g., patient GDS score, caregiver age) and analysis of variance for categorical variables (e.g., patient cancer stage, caregiver employment status). Three variables (caregiver age, caregiver employment status, and GDS scores of the patient with cancer) significantly associated with caregiver strain in the bivariate tests were sequentially added to a series of linear regression models to examine their effects on caregiver strain, after adjusting for other factors in the model. A model with a single independent variable of caregiver age (model 1) was used initially, then caregiver employment status (model 2) and GDS scores of the patients with cancer (model 3) were added as independent variables to predict the dependent variable of caregiver strain. All statistical tests were two-sided, with a significance level of 0.05. 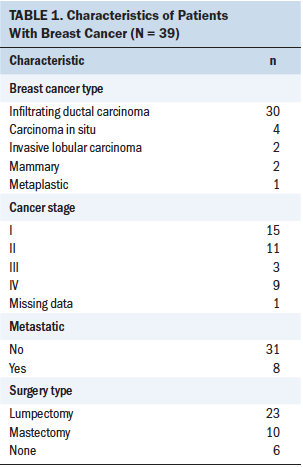
Results
The mean age of the patients with cancer was 77.9 years (SD = 5.9) (see Table 1), and the mean age of the caregivers was 64 years (SD = 15) (see Table 2). Most (n = 30) patients had been diagnosed with infiltrating ductal carcinoma and had early-stage disease (n = 26 for stage I or II disease); a majority of patients had nonmetastatic disease (n = 31) and had undergone lumpectomy (n = 23). Of the caregivers, 22 were the solo caregiver to the patient. Twelve caregivers reported being employed full-time, and 27 rated their health as excellent or very good. 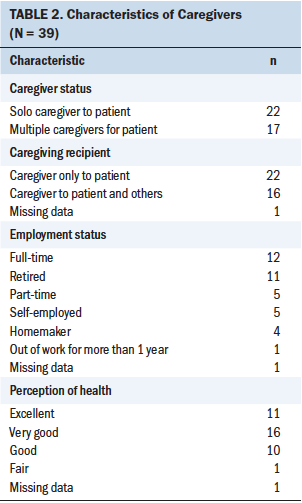
Mean scores for each instrument of the CGA and for the MSCI are reported in Table 3. Average caregiver strain, as evaluated with the MSCI, was 4.1, reflecting a moderate level of strain in the sample. 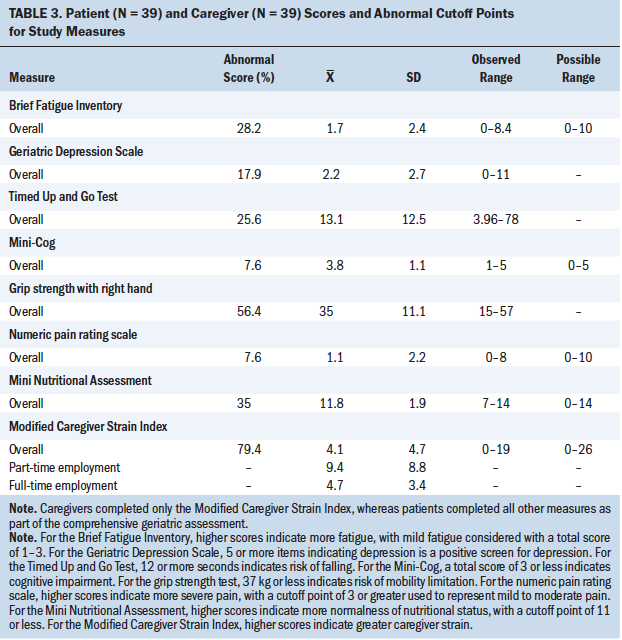
Increasing age of the caregiver was associated with less caregiver strain (r = –0.45, p = 0.02). Employment status of the caregiver was significantly related to caregiver strain (p = 0.03) (see Table 4). Caregivers who were employed part-time experienced greater strain (mean = 9.4, SD = 8.8) than those who were employed full-time (mean = 4.7, SD = 3.4) and those who reported being a homemaker, self-employed, retired, or out of work for more than one year (mean = 2.7, SD = 3.4). The only characteristic of patients with cancer that significantly contributed to caregiver strain was depression, as measured by the GDS (r = 0.32, p = 0.05). 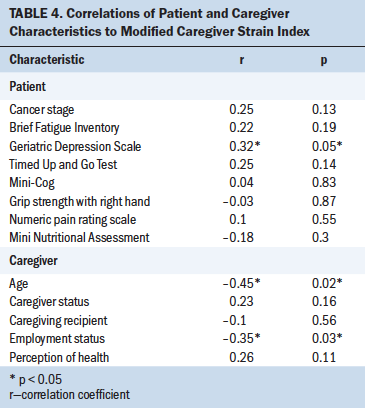
Table 5 summarizes the results from the sequential linear regression models. Model 1 suggests that a one-year increase in caregiver age was associated with a 0.13-point (standard error [SE] = 0.05) decrease in caregiver MCSI score (p = 0.02). R2 was 0.204 for model 1, indicating that caregiver age as a single independent variable explained 20.4% of the variance of caregiver strain. The effect of caregiver age on caregiver strain was much smaller (b = –0.06, SE = 0.06, p = 0.36) after adding caregiver employment status to the model (model 2). The coefficient (b) estimates of model 2 suggest that part-time employment was associated with 5.95 higher MCSI scores (SE = 2.6, p = 0.03) and full-time employment was associated with 3.45 higher MCSI scores (SE = 1.86, p = 0.08) when compared to other employment statuses (not full-time or part-time employment). R2 was 0.375 for model 2, indicating that adding employment status to the model explained an additional 17.1% of the variance of caregiver strain compared to model 1. The effects of caregiver employment status continued after further adding patient GDS scores to the model (model 3). Results of model 3 suggest that a 1-point increase in patient GDS scores was associated with a 0.55-point (SE = 0.27) increase in caregiver strain (p = 0.05) and that GDS scores of the patient with cancer explained an additional 10% variance after caregiver age and employment status were already considered (R2 = 0.475 versus 0.375 for model 3 versus model 2, respectively). 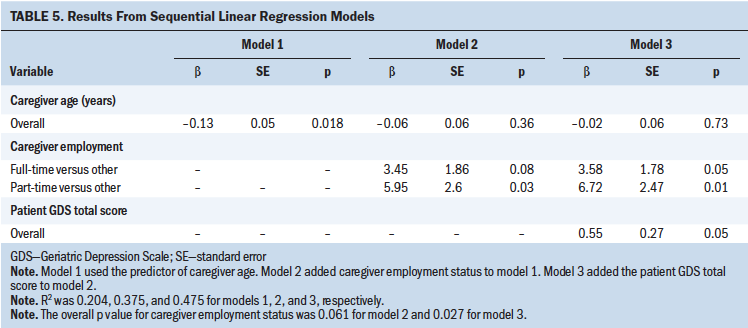
Discussion
Most patients in this study screened negative for cognition impairment, depression, and fatigue, but many had difficulty with gait on the Timed Up and Go Test, experienced poor upper extremity strength, and screened positive for nutritional impairment. Caregiver age and scores on the MCSI were negatively correlated, indicating that the younger the caregiver, the more the perceived strain, which is supported in the literature (Ge & Mordiffi, 2017). Younger caregivers are more likely to be employed, be caring for children, have a family, and have multiple responsibilities (de Moor et al., 2017; Haun et al., 2014) and schedule conflicts (Hartnett et al., 2016), all of which contribute to strain. Of note, older age of the individual with cancer is correlated with less impact of caregiver strain (Goldzweig et al., 2019).
Employed caregivers of individuals with cancer experience many conflicts that can affect work performance, which can cause financial strain (Adelman et al., 2014), particularly when caring for a person diagnosed with advanced cancer (de Moor et al., 2017). Work impairment (inability to perform role because of caregiver responsibility) among caregivers of individuals with cancer is about 25% (Wood, Taylor-Stokes, & Lees, 2019), and the threat of losing a job and the resulting financial hardship is of prime concern (Hussain, Wark, & Ryan, 2018). Employment reduces the caregiver’s ability to attend clinic visits and help with activities throughout the day, and may contribute to notions of guilt (Haun et al., 2014). Retired caregivers may have more time for providing companionship and assisting with daily needs (Adelman et al., 2014). Part-time employment was related to greater caregiver strain, which may be attributable to financial concerns and the inability to work full-time. Part-time workers may also have many competing responsibilities in addition to caregiving, which may increase strain.
More than half (n = 27) of the caregivers in the current study perceived their health to be excellent or very good; however, 11 reported their health to be good or fair. Many caregivers struggle to exercise and perform self-care activities, particularly when patients are functionally dependent (American Psychological Association, n.d.). The mean Timed Up and Go Test score of 13 seconds (cutoff point of 12 or more seconds) and the mean grip strength of 35 kg (cutoff point of 37 kg or less) suggested some functional impairment of patients in the sample. Functional status was not predictive of caregiver strain, which may be because the mean Timed Up and Go Test score and grip strength were not far below the normal cutoff points for impairment. Caregivers tend to report high burden when caring for individuals with cancer who experience impaired functional status (Hsu et al., 2014).
Depression was found to be the only patient characteristic significantly associated with caregiver strain. Depression experienced by the person with cancer can be a formidable contributor to caregiver strain and is common (42%) among caregivers of individuals with cancer (Geng et al., 2018). Although the mean score on the GDS was 2.2, which is not above the cutoff point that indicates a positive screen, 17% of patients did screen positive for depression. Depression is commonly reported by people who are diagnosed with breast cancer, particularly when there are limited social interactions (Sibalija et al., 2018). Caregivers should have the ability to recognize depression and assist the patient in receiving treatment (Ferrell et al., 2018). Nurses must be aware that caregiver depression can be more acute during cancer treatment but does decrease over time (Lee et al., 2017).
Limitations
The current authors were not able to draw causal inference because of the cross-sectional nature of the study. Perhaps several data points over a yearlong period would have shown times when strain was increased for caregivers of individuals receiving treatment for aggressive tumors. In addition, the small sample size (N = 39 patient–caregiver dyads) only had sufficient power to detect medium or larger effect sizes (e.g., r ≥ 0.3, R2 ≥ 0.09). Larger sample sizes are needed to further examine characteristics that yielded small-to-medium associations with caregiver strain but failed to reach statistical significance (e.g., r = 0.25 and r = 0.26 for the associations of patient Timed Up and Go Test scores and caregiver health with caregiver strain, respectively). Findings were interpreted based on effect sizes, clinical significance, and statistical significance. For example, GDS scores of patients with cancer had borderline statistical significance (p = 0.053) and explained an additional 10% of the variance after adjusting for caregiver age and employment status, which is of medium effect size. Also, the magnitude of effect is of clinical significance, with a 1-point increase in GDS scores being associated with a 0.55-point increase in caregiver strain. Compared to caregiver age and employment status, patient GDS scores have greater clinical implications because of their modifiable nature through better symptom management. Finally, the data were from a convenience sample in one clinic. Findings may not be generalizable to patients and their caregivers in other regions. Nevertheless, the study findings provide valuable preliminary data for future large-scale studies. Data concerning caregiver relationship to the individual with cancer, driving distance to the cancer center, race, and income were not collected and will be added to future research designs.
Implications for Nursing
Nursing support and adequate communication for caregivers should be an essential part of the cancer management plan (Marcotte et al., 2019) and should begin during the initial visit to the cancer center. Patients with cancer and caregivers perceive the oncology healthcare team to be a primary source of support throughout the cancer diagnosis and treatment process (Law, Levesque, Lambert, & Girgis, 2018), and communication is a central aspect of this. Assessing how caregivers are managing at home at each patient encounter and providing some coping mechanisms (e.g., support groups, community services, education) is important (Mahendran et al., 2017). Caregiver strain and burden assessment findings should be included in the medical record following each visit.
Despite many educational and psychotherapeutic interventions to support caregivers that have been studied, it is important to understand the effectiveness of strategies to support caregivers and not overestimate the ability of providers to address important concerns (Irwin, Dudley, Northouse, Berry, & Mallory, 2018). Being aware of the interventions that are available within the cancer center and assessing the effectiveness of these interventions during visits are important. Caregiver strain can be accentuated when the role of the caregiver requires skills such as medication administration, management of toxicities, and other tasks that can be overwhelming (Ullgren et al., 2018). In situations where the caregiver is managing toxicities and treatment, nurses and social workers should be conducting ongoing assessments to guide the survivorship care plan.
Nurses must assess if there are multiple caregivers to provide support or only one. Caregivers who share responsibilities report lower burden (Shiba, Kondo, & Kondo, 2016). A planning tool for survivorship care in people who are diagnosed with cancer and their caregivers is helpful to nurses managing needs of the dyad (Sterba et al., 2019). Many caregivers most likely have other responsibilities, such as maintaining employment and caring for a family.
Caregivers may feel relief when assured that their role can be demanding (Northouse et al., 2013; Rutkowski et al., 2018). Training programs are available to help nurses better communicate with individuals diagnosed with cancer and families of patients with cancer (Wittenberg, Goldsmith, Williams, & Lee, 2018). Websites and other electronic resources are also available to help caregivers (Wittenberg, Xu, Goldsmith, & Mendoza, 2019):
• AgingCare (www.agingcare.com/topics/29/caregiving) offers caregiver information on community support services, a reading list of caregiver material, and answers to common questions.
• The Family Caregiver Alliance (www.caregiver.org) provides online support groups and caregiver education materials.
• The U.S. Department of Veterans Affairs (www.caregiver.va.gov) has a website designed to help caregivers throughout diagnosis, treatment, and care.
• The Patient and Caregiver Support Program at Memorial Sloan Kettering Cancer Center is specific to cancer (www.mskcc.org/experience/patient-support/counseling/support-groups-programs/patient-patient-support).
Access to these and other resources can be initiated by nurses or social workers. Generally, in academic medical centers and large private practices, social workers are available to help patients navigate community resources. In smaller community clinics, nurses are often the point of access for caregivers and community resources. Nurses should be aware of caregiver support resources and work with social workers to offer any support options available.
Although the current study revealed that younger caregivers perceived more strain, older caregivers report burden and strain as well (Jeong et al., 2016) and may have limited support—their families may not live close to them; some may have survived their family and friends; and some may experience isolation because of their own functional limitations. Caregivers who receive social support tend to report less burden (Naganuma, Kihara, Fujita, Yamaoka, & Takahashi, 2018). Aging caregivers may experience comorbidities, resulting in limited ability to assist the patient in activities of daily living. Including the caregiver in the nursing assessment can identify some of the challenges faced by the caregiver. Nurses should understand the social support options available through local area agencies on aging and community centers. In some states, homecare options may be available to help provide caregivers with assistance. Support services may also be available from the cancer center, such as support groups, caregiver educational sessions, and exercise programs.
Caregivers who are employed may require more support and encouragement from the nursing team. The Working Caregiver (www.workingcaregiver.com) is a resource for common issues in caregiving and can be a first step in pursuing necessary information. Nurses must be sensitive to the employment and financial concerns of individuals with cancer and their caregivers. Deductibles and co-payments for patients can be expensive and a major concern for many families. For those who are employed part-time, assessing financial concerns can possibly be addressed by social workers.
The need for disease and healthcare information is a prime concern for caregivers (Marcotte et al., 2019). Providing education about symptom management may also help to reduce strain, particularly in new caregivers (Ferrell & Wittenberg, 2017; Garlo et al., 2010), and potentially establish confidence in providing care, especially when a skill is required (Havyer van Ryn, Wilson, & Griffin, 2017). Cancer care is complex and involves scientific terminology that can be stressful to patients and caregivers. Patient–caregiver breast cancer education on nutrition, rest, activity, and side effect management reduces caregiver strain (Kochaki Nejad, Mohajjel Agndam, Hassankhani, & Sanaat, 2016). Educational interventions influencing competence reduce depression and anxiety in patients and caregivers (Chan, Glass, Chua, Ali, & Lim, 2018). Older adults diagnosed with cancer and their caregivers are less likely to receive adequate disease information and participate in treatment decisions, and more likely to receive less attention from the healthcare team (Shin et al., 2019). Recognizing that older caregivers and individuals with cancer are in need of cancer education, symptom management information, and support from the oncology nursing team should be enhanced.
Future research specific to caregivers of older women diagnosed with breast cancer should develop a model specific to using CGA in recognizing risk for caregiver strain and burden before the patient–caregiver relationship is compromised. This study explained only 37.5% of the variance among the variables; therefore, future research should include other individual and caregiver variables not included in this study, such as distress, financial concerns, distance to cancer center, illness severity, end of life, and relationship to the individual with cancer. 
Conclusion
Depression in older adults with cancer, employment status, and age of the caregiver are related to caregiver strain. Caregiver part-time employment status, younger caregiver age, and depression of the individual with cancer are predictive of strain among caregivers of older women diagnosed with breast cancer. Assessment is important to recognizing issues such as depression, cognitive impairments, risk of falls, and pain in the patient, as well as strain and issues with coping in the caregiver.
About the Author(s)
Janine Overcash, PhD, CNP-APRN, FAANP, FAAN, is a professor in the College of Nursing, Susan Fugett, MSW, LISW-S, OSW-C, CSW-G, is a clinical social worker in the Stefanie Spielman Comprehensive Breast Center, Alai Tan, PhD, is a research associate professor in the College of Nursing, Jane Ginther, BSN, RN-BC, is a staff nurse in the Ohio State University Wexner Medical Center, and Nicole Williams, MD, is an assistant professor in the Stefanie Spielman Comprehensive Breast Center, all at the Ohio State University in Columbus. No financial relationships to disclose. Overcash and Fugett contributed to the conceptualization and design and completed the data collection. Tan provided statistical support and analysis. All authors contributed to the manuscript preparation. Overcash can be reached at overcash.1@osu.edu, with copy to ONFEditor@ons.org. (Submitted March 2019. Accepted May 24, 2019.)
References
Adelman, R.D., Tmanova, L.L., Delgado, D., Dion, S., & Lachs, M.S. (2014). Caregiver burden: A clinical review. JAMA, 311, 1052–1060. https://doi.org/10.1001/jama.2014.304
Aggarwal, B., Liao, M., Christian, A., & Mosca, L. (2009). Influence of caregiving on lifestyle and psychosocial risk factors among family members of patients hospitalized with cardiovascular disease. Journal of General Internal Medicine, 24, 93–98. https://doi.org/10.1007/s11606-008-0852-1
American Cancer Society. (2016). What is a cancer caregiver? Retrieved from https://www.cancer.org/treatment/caregivers/what-a-caregiver-does/who-a…
American Geriatrics Society, British Geriatrics Society, & American Academy of Orthopaedic Surgeons Panel on Falls Prevention. (2001). Guideline for the prevention of falls in older persons. Journal of the American Geriatrics Society, 49, 664–672. https://doi.org/10.1046/j.1532-5415.2001.49115.x
American Psychological Association. (n.d.). Family caregivers’ needs are often invisible. Retrieved from https://www.apa.org/pi/about/publications/caregivers/faq/invisible-need…
Badr, H., Smith, C.B., Goldstein, N.E., Gomez, J.E., & Redd, W.H. (2015). Dyadic psychosocial intervention for advanced lung cancer patients and their family caregivers: Results of a randomized pilot trial. Cancer, 121, 150–158. https://doi.org/10.1002/cncr.29009
Baillie, J., Anagnostou, D., Sivell, S., Van Godwin, J., Byrne, A., & Nelson, A. (2018). Symptom management, nutrition and hydration at end-of-life: A qualitative exploration of patients’, carers’ and health professionals’ experiences and further research questions. BMC Palliative Care, 17, 60. https://doi.org/10.1186/s12904-018-0314-4
Bangerter, L.R., Griffin, J.M., & Dunlay, S.M. (2019). Positive experiences and self-gain among family caregivers of persons with heart failure. Gerontologist, 59, e433–e440. https://doi.org/10.1093/geront/gny162
Bekdemir, A., & Ilhan, N. (2018). Predictors of caregiver burden in caregivers of bedridden patients. Journal of Nursing Research, 27, e24. https://doi.org/10.1097/jnr.0000000000000297
Berg, K.O., Wood-Dauphinee, S.L., Williams, J.I., & Maki, B. (1992). Measuring balance in the elderly: Validation of an instrument. Canadian Journal of Public Health, 83(Suppl. 2), S7–S11.
Berglund, E., Lytsy, P., & Westerling, R. (2015). Health and wellbeing in informal caregivers and non-caregivers: A comparative cross-sectional study of the Swedish general population. Health and Quality of Life Outcomes, 13, 109. https://doi.org/10.1186/s12955-015-0309-2
Besser, L.M., & Galvin, J.E. (2019). Perceived burden among caregivers of patients with frontotemporal degeneration in the United States. International Psychogeriatrics, 31, 1191–1201. https://doi.org/10.1017/s104161021800159x
Bień-Barkowska, K., Doroszkiewicz, H., & Bień, B. (2017). Silent strain of caregiving: Exploring the best predictors of distress in family carers of geriatric patients. Clinical Interventions in Aging, 2017, 263–274. https://doi.org/10.2147/cia.s125664
Black, C.M., Ritchie, C.W., Khandker, R.K., Wood, R., Jones, E., Hu, X., & Ambegaonkar, B.M. (2018). Non-professional caregiver burden is associated with the severity of patients’ cognitive impairment. PLOS ONE, 13, e0204110. https://doi.org/10.1371/journal.pone.0204110
Bonin-Guillaume, S., Durand, A.-C., Yahi, F., Curiel-Berruyer, M., Lacroix, O., Cretel, E., . . . Gentile, S. (2015). Predictive factors for early unplanned rehospitalization of older adults after an ED visit: Role of the caregiver burden. Aging Clinical and Experimental Research, 27, 883–891. https://doi.org/10.1007/s40520-015-0347-y
Borges, E.L., Franceschini, J., Costa, L.H.D., Fernandes, A.L.G., Jamnik, S., & Santoro, I.L. (2017). Family caregiver burden: The burden of caring for lung cancer patients according to the cancer stage and patient quality of life. Journal Brasileiro de Pneumologia, 43, 18–23. https://doi.org/10.1590/s1806-37562016000000177
Borson, S., Scanlan, J., Brush, M., Vitaliano, P., & Dokmak, A. (2000). The Mini-Cog: A cognitive ‘vital signs’ measure for dementia screening in multi-lingual elderly. International Journal of Geriatric Psychiatry, 15, 1021–1027. https://doi.org/10.1002/1099-1166(200011)15:11<1021::AID-GPS234>3.0.CO;…
Bove, D.G., Zakrisson, A.-B., Midtgaard, J., Lomborg, K., & Overgaard, D. (2016). Undefined and unpredictable responsibility: A focus group study of the experiences of informal caregiver spouses of patients with severe COPD. Journal of Clinical Nursing, 25, 483–493. https://doi.org/10.1111/jocn.13076
Butow, P.N., Price, M.A., Bell, M.L., Webb, P.M., deFazio, A., & Friedlander, M. (2014). Caring for women with ovarian cancer in the last year of life: A longitudinal study of caregiver quality of life, distress and unmet needs. Gynecological Oncology, 132, 690–697. https://doi.org/10.1016/j.ygyno.2014.01.002
Cella, D.F., Tulsky, D.S., Gray, G., Sarafian, B., Linn, E., Bonomi, A., . . . Brannon, J. (1993). The Functional Assessment of Cancer Therapy scale: Development and validation of the general measure. Journal of Clinical Oncology, 11, 570–579. https://doi.org/10.1200/JCO.1993.11.3.570
Chan, E.-Y., Glass, G., Chua, K.-C., Ali, N., & Lim, W.-S. (2018). Relationship between mastery and caregiving competence in protecting against burden, anxiety and depression among caregivers of frail older adults. Journal of Nutrition, Health and Aging, 22, 1238–1245. https://doi.org/10.1007/s12603-018-1098-1
Chang, Y.J., Lee, J.S., Lee, C.G., Lee, W.S., Lee, K.S., Bang, S.-M.,. . . Yun, Y.H. (2007). Assessment of clinical relevant fatigue level in cancer. Supportive Care in Cancer, 15, 891–896. https://doi.org/10.1007/s00520-007-0219-x
Chen, M.L., & Hu, L.C. (2002). The generalizability of Caregiver Strain Index in family caregivers of cancer patients. International Journal of Nursing Studies, 39, 823–829.
Collin, C., Wade, D.T., Davies, S., & Horne, V. (1988). The Barthel ADL Index: A reliability study. International Disability Studies, 10, 61–63.
Cuthbert, C.A., King-Shier, K.M., Ruether, J.D., Tapp, D.M., Wytsma-Fisher, K., Fung, T.S., & Culos-Reed, S.N. (2018). The effects of exercise on physical and psychological outcomes in cancer caregivers: Results From the RECHARGE randomized controlled trial. Annals of Behavioral Medicine, 52, 645–661. https://doi.org/10.1093/abm/kax040
Dauphinot, V., Ravier, A., Novais, T., Delphin-Combe, F., Moutet, C., Xie, J., . . . Krolak-Salmon, P. (2016). Relationship between comorbidities in patients with cognitive complaint and caregiver burden: A cross-sectional study. Journal of Post-Acute and Long-Term Care Medicine, 17, 232–237. https://doi.org/10.1016/j.jamda.2015.10.011
de Moor, J.S., Dowling, E.C., Ekwueme, D.U., Guy, G.P., Jr., Rodriguez, J., Virgo, K.S., . . . Yabroff, K.R. (2017). Employment implications of informal cancer caregiving. Journal of Cancer Survivorship, 11, 48–57. https://doi.org/10.1007/s11764-016-0560-5
Dionne-Odom, J.N., Demark-Wahnefried, W., Taylor, R.A., Rocque, G.B., Azuero, A., Acemgil, A., . . . Bakitas, M.A. (2017). The self-care practices of family caregivers of persons with poor prognosis cancer: Differences by varying levels of caregiver well-being and preparedness. Supportive Care in Cancer, 25, 2437–2444. https://doi.org/10.1007/s00520-017-3650-7
Family Caregiver Alliance. (2016). Caregiver statistics: Demographics. Retrieved from https://www.caregiver.org/caregiver-statistics-demographics
Ferrell, B., & Wittenberg, E. (2017). A review of family caregiving intervention trials in oncology. CA: A Cancer Journal for Clinicians, 67, 318–325. https://doi.org/10.3322/caac.21396
Ferrell, B.R., Kravitz, K., Borneman, T., & Taratoot Friedmann, E. (2018). Family caregivers: A qualitative study to better understand the quality-of-life concerns and needs of this population. Clinical Journal of Oncology Nursing, 22, 286–294. https://doi.org/10.1188/18.CJON.286-294
Folstein, M.F., Folstein, S.E., & McHugh, P.R. (1975). “Mini-mental state”. A practical method for grading the cognitive state of patients for the clinician. Journal of Psychiatric Research, 12, 189–198.
Frambes, D., Given, B., Lehto, R., Sikorskii, A., & Wyatt, G. (2018). Informal caregivers of cancer patients: Review of interventions, care activities, and outcomes. Western Journal of Nursing Research, 40, 1069–1097. https://doi.org/10.1177/0193945917699364
Frensham, L.J., Parfitt, G., & Dollman, J. (2018). Effect of a 12-week online walking intervention on health and quality of life in cancer survivors: A quasi-randomized controlled trial. International Journal of Environmental Research and Public Health, 15, 2081. https://doi.org/10.3390/ijerph15102081
Fujinami, R., Sun, V., Zachariah, F., Uman, G., Grant, M., & Ferrell, B. (2015). Family caregivers’ distress levels related to quality of life, burden, and preparedness. Psycho-Oncology, 24, 54–62. https://doi.org/10.1002/pon.3562
Garlo, K., O’Leary, J.R., Van Ness, P.H., & Fried, T.R. (2010). Burden in caregivers of older adults with advanced illness. Journal of the American Geriatrics Society, 58, 2315–2322. https://doi.org/10.1111/j.1532-5415.2010.03177.x
Ge, L., & Mordiffi, S.Z. (2017). Factors associated with higher caregiver burden among family caregivers of elderly cancer patients: A systematic review. Cancer Nursing, 40, 471–478. https://doi.org/10.1097/ncc.0000000000000445
Geng, H.-M., Chuang, D.-M., Yang, F., Yang, Y., Liu, W.-M., Liu, L.-H., & Tian, H.-M. (2018). Prevalence and determinants of depression in caregivers of cancer patients: A systematic review and meta-analysis. Medicine, 97, e11863. https://doi.org/10.1097/md.0000000000011863
Given, B.A., Given, C.W., & Sherwood, P.R. (2012). Family and caregiver needs over the course of the cancer trajectory. Journal of Supportive Oncology, 10, 57–64.
Given, B.A., Sherwood, P., & Given, C.W. (2011). Support for caregivers of cancer patients: Transition after active treatment. Cancer Epidemiology, Biomarkers and Prevention, 20, 2015–2021. https://doi.org/10.1158/1055-9965.epi-11-0611
Goldzweig, G., Schapira, L., Baider, L., Jacobs, J.M., Andritsch, E., & Rottenberg, Y. (2019). Who will care for the caregiver? Distress and depression among spousal caregivers of older patients undergoing treatment for cancer. Supportive Care in Cancer. Advance online publication. https://doi.org/10.1007/s00520-019-04711-6
Gomes, G.A.O., Luchesi, B.M., Gratão, A.C.M., Orlandi, F.S., Say, K.G., Inouye, K., . . . Pavarini, S.C.I. (2019). Prevalence of physical inactivity and associated factors among older caregivers of older adults. Journal of Aging and Health, 31, 793–813. https://doi.org/10.1177/0898264318756422
Große, J., Treml, J., & Kersting, A. (2018). Impact of caregiver burden on mental health in bereaved caregivers of cancer patients: A systematic review. Psycho-Oncology, 27, 757–767. https://doi.org/10.1002/pon.4529
Grover, S., Rina, K., Malhotra, P., & Khadwal, A. (2018). Correlates of positive aspects of caregiving among family caregivers of patients with acute myeloblastic leukaemia. Indian Journal of Hematology and Blood Transfusion, 34, 612–617. https://doi.org/10.1007/s12288-018-0957-6
Hamilton, M. (1960). A rating scale for depression. Journal of Neurology, Neurosurgery, and Psychiatry, 23, 56–62. https://doi.org/10.1136/jnnp.23.1.56
Hartnett, J., Thom, B., & Kline, N. (2016). Caregiver burden in end-stage ovarian cancer. Clinical Journal of Oncology Nursing, 20, 169–173. https://doi.org/10.1188/16.CJON.169-173
Haun, M.W., Sklenarova, H., Brechtel, A., Herzog, W., & Hartmann, M. (2014). Distress in cancer patients and their caregivers and association with the caregivers’ perception of dyadic communication. Oncology Research and Treatment, 37, 384–388. https://doi.org/10.1159/000364885
Havyer, R.D., van Ryn, M., Wilson, P.M., & Griffin, J.M. (2017). The effect of routine training on the self-efficacy of informal caregivers of colorectal cancer patients. Supportive Care in Cancer, 25, 1071–1077. https://doi.org/10.1007/s00520-016-3494-6
Hsu, T., Loscalzo, M., Ramani, R., Forman, S., Popplewell, L., Clark, K., . . . Hurria, A. (2014). Factors associated with high burden in caregivers of older adults with cancer. Cancer, 120, 2927–2935. https://doi.org/10.1002/cncr.28765
Hsu, T., Loscalzo, M., Ramani, R., Forman, S., Popplewell, L., Clark, K., . . . Hurria, A. (2017). Are disagreements in caregiver and patient assessment of patient health associated with increased caregiver burden in caregivers of older adults with cancer? Oncologist, 22, 1383–1391. https://doi.org/10.1634/theoncologist.2017-0085
Hussain, R., Wark, S., & Ryan, P. (2018). Caregiving, employment and social isolation: Challenges for rural carers in Australia. International Journal of Environmental Research and Public Health, 15, E2267. https://doi.org/10.3390/ijerph15102267
Irwin, M.M., Dudley, W., Northouse, L., Berry, D.L., & Mallory, G.A. (2018). Oncology nurses’ knowledge, confidence, and practice in addressing caregiver strain and burden. Oncology Nursing Forum, 45, 187–196. https://doi.org/10.1188/18.ONF.187-196
Jansen, L., Dauphin, S., van den Akker, M., De Burghgraeve, T., Schoenmakers, B., & Buntinx, F. (2018). Prevalence and predictors of psychosocial problems in informal caregivers of older cancer survivors—A systematic review: Still major gaps in current research. European Journal of Cancer Care, 27, e12899. https://doi.org/10.1111/ecc.12899
Jeong, A., Shin, D.W., Kim, S.Y., Yang, H.K., Shin, J.Y., Park, K., . . . Park, J.-H. (2016). The effects on caregivers of cancer patients’ needs and family hardiness. Psycho-Oncology, 25, 84–90. https://doi.org/10.1002/pon.3878
Johansen, S., Cvancarova, M., & Ruland, C. (2018). The effect of cancer patients’ and their family caregivers’ physical and emotional symptoms on caregiver burden. Cancer Nursing, 41, 91–99. https://doi.org/10.1097/ncc.0000000000000493
Juntunen, K., Salminen, A.-L., Törmäkangas, T., Tillman, P., Leinonen, K., & Nikander, R. (2018). Perceived burden among spouse, adult child, and parent caregivers. Journal of Advanced Nursing, 74, 2340–2350. https://doi.org/10.1111/jan.13733
Kaiser, M.J., Bauer, J.M., Ramsch, C., Uter, W., Guigoz, Y., Cederholm, T., . . . Sieber, C.C. (2009). Validation of the Mini Nutritional Assessment short-form (MNA-SF): A practical tool for identification of nutritional status. Journal of Nutrition, Health and Aging, 13, 782–788.
Karlsen, C., Moe, C.E., Haraldstad, K., & Thygesen, E. (2019). Caring by telecare? A hermeneutic study of experiences among older adults and their family caregivers. Journal of Clinical Nursing, 28, 1300–1313. https://doi.org/10.1111/jocn.14744
Kelley, D.E., Kent, E.E., Litzelman, K., Mollica, M.A., & Rowland, J.H. (2019). Dyadic associations between perceived social support and cancer patient and caregiver health: An actor-partner interdependence modeling approach. Psycho-Oncology, 28, 1453–1460. https://doi.org/10.1002/pon.5096
Kent, E.E., & Dionne-Odom, J.N. (2019). Population-based profile of mental health and support service need among family caregivers of adults with cancer. Journal of Oncology Practice, 15, e122–e131. https://doi.org/10.1200/jop.18.00522
Kent, E.E., Rowland, J.H., Northouse, L., Litzelman, K., Chou, W.-Y., Shelburne, N., . . . Huss, K. (2016). Caring for caregivers and patients: Research and clinical priorities for informal cancer caregiving. Cancer, 122, 1987–1995. https://doi.org/10.1002/cncr.29939
Kim, Y., Shaffer, K.M., Carver, C.S., & Cannady, R.S. (2016). Quality of life of family caregivers 8 years after a relative’s cancer diagnosis: Follow-up of the National Quality of Life Survey for Caregivers. Psycho-Oncology, 25, 266–274. https://doi.org/10.1002/pon.3843
Kochaki Nejad, Z., Mohajjel Aghdam, A., Hassankhani, H., & Sanaat, Z. (2016). The effects of a patient-caregiver education and follow-up program on the breast cancer caregiver strain index. Iran Red Crescent Medical Journal, 18, e21627. https://doi.org/10.5812/ircmj.21627
Kotronoulas, G., Wengström, Y., & Kearney, N. (2016). Alterations and interdependence in self-reported sleep-wake parameters of patient–caregiver dyads during adjuvant chemotherapy for breast cancer. Oncology Nursing Forum, 43, 288–301. https://doi.org/10.1188/16.ONF.288-301
Kuluski, K., Peckham, A., Gill, A., Arneja, J., Morton-Chang, F., Parsons, J., . . . Sheridan, N. (2018). “You’ve got to look after yourself, to be able to look after them” a qualitative study of the unmet needs of caregivers of community based primary health care patients. BMC Geriatrics, 18, 275. https://doi.org/10.1186/s12877-018-0962-5
LaValley, S.A., & Gage-Bouchard, E.A. (2018). Life course stage and social support mobilization for end-of-life caregivers. Journal of Applied Gerontology. Advance online publication. https://doi.org/10.1177/0733464818766666
Law, E., Levesque, J.V., Lambert, S., & Girgis, A. (2018). The “sphere of care”: A qualitative study of colorectal cancer patient and caregiver experiences of support within the cancer treatment setting. PLOS ONE, 13, e0209436. https://doi.org/10.1371/journal.pone.0209436
Lee, C.-Y., Lee, Y., Wang, L.-J., Chien, C.-Y., Fang, F.-M., & Lin, P.-Y. (2017). Depression, anxiety, quality of life, and predictors of depressive disorders in caregivers of patients with head and neck cancer: A six-month follow-up study. Journal of Psychosomatic Research, 100, 29–34. https://doi.org/10.1016/j.jpsychores.2017.07.002
Litzelman, K., Skinner, H.G., Gangnon, R.E., Nieto, F.J., Malecki, K., & Witt, W.P. (2015). The relationship among caregiving characteristics, caregiver strain, and health-related quality of life: Evidence from the Survey of the Health of Wisconsin. Quality of Life Research, 24, 1397–1406. https://doi.org/10.1007/s11136-014-0874-6
Mahendran, R., Lim, H.A., Tan, J.Y.S., Ng, H.Y., Chua, J., Lim, S.E., . . . Griva, K. (2017). Evaluation of a brief pilot psychoeducational support group intervention for family caregivers of cancer patients: A quasi-experimental mixed-methods study. Health and Quality of Life Outcomes, 15, 17. https://doi.org/10.1186/s12955-017-0595-y
Marcotte, J., Tremblay, D., Turcotte, A., & Michaud, C. (2019). Needs-focused interventions for family caregivers of older adults with cancer: A descriptive interpretive study. Supportive Care in Cancer, 27, 2771–2781. https://doi.org/10.1007/s00520-018-4573-7
Massy-Westropp, N.M., Gill, T.K., Taylor, A.W., Bohannon, R.W., & Hill, C.L. (2011). Hand grip strength: Age and gender stratified normative data in a population-based study. BMC Research Notes, 4, 127. https://doi.org/10.1186/1756-0500-4-127
McCaffery, M., & Beebe, A. (1989). Pain: Clinical manual for nursing practice. St. Louis, MO: Mosby.
Mendoza, T.R., Wang, X.S., Cleeland, C.S., Morrissey, M., Johnson, B.A., Wendt, J.K., & Huber, S.L. (1999). The rapid assessment of fatigue severity in cancer patients: Use of the Brief Fatigue Inventory. Cancer, 85, 1186–1196. https://doi.org/10.1002/(sici)1097-0142(19990301)85:5<1186::aid-cncr24>…
Mosher, C.E., Bakas, T., & Champion, V.L. (2013). Physical health, mental health, and life changes among family caregivers of patients with lung cancer. Oncology Nursing Forum, 40, 53–61. https://doi.org/10.1188/13.ONF.53-61
Naganuma, Y., Kihara, S., Fujita, Y., Yamaoka, K., & Takahashi, K. (2018). The relation between social cohesion and the care burden of family healthcare providers. Bioscience Trends, 12, 520–522. https://doi.org/10.5582/bst.2018.01175
National Alliance for Caregiving & AARP Public Policy Institute. (2015). Caregiving in the U.S. Retrieved from https://www.aarp.org/content/dam/aarp/ppi/2015/caregiving-in-the-united…
National Comprehensive Cancer Network. (2019). NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines®): Older adult oncology [v.1.2019]. Retrieved from https://www.nccn.org/professionals/physician_gls/pdf/senior.pdf
Northouse, L., Williams, A.-L., Given, B., & McCorkle, R. (2012). Psychosocial care for family caregivers of patients with cancer. Journal of Clinical Oncology, 30, 1227–1234. https://doi.org/10.1200/jco.2011.39.5798
Northouse, L.L., Katapodi, M.C., Song, L., Zhang, L., & Mood, D.W. (2010). Interventions with family caregivers of cancer patients: Meta-analysis of randomized trials. CA: A Cancer Journal for Clinicians, 60, 317–339. https://doi.org/10.3322/caac.20081
Northouse, L.L., Mood, D.W., Schafenacker, A., Kalemkerian, G., Zalupski, M., LoRusso, P., . . . Kershaw, T. (2013). Randomized clinical trial of a brief and extensive dyadic intervention for advanced cancer patients and their family caregivers. Psycho-Oncology, 22, 555–563. https://doi.org/10.1002/pon.3036
Oncology Nursing Society. (2017). Caregiver strain and burden. Retrieved from https://www.ons.org/pep/caregiver-strain-and-burden
Paek, M.-S., Nightingale, C.L., Tooze, J.A., Milliron, B.-J., Weaver, K.E., & Sterba, K.R. (2018). Contextual and stress process factors associated with head and neck cancer caregivers’ physical and psychological well-being. European Journal of Cancer Care, 27, e12833. https://doi.org/10.1111/ecc.12833
Patterson Medical. (n.d.). Jamar® hydraulic hand dynamometer owner’s manual. Retrieved from https://www.performancehealth.com/amfile/file/download/file_id/6971/pro…
Podsiadlo, D., & Richardson, S. (1991). The timed “Up & Go”: A test of basic functional mobility for frail elderly persons. Journal of the American Geriatrics Society, 39, 142–148.
Poort, H., Peters, M.E.W.J., Gielissen, M.F.M., Verhagen, C.A.H.H.V.M., Bleijenberg, G., van der Graaf, W.T.A., . . . Knoop, H. (2016). Fatigue in advanced cancer patients: Congruence between patients and their informal caregivers about patients’ fatigue severity during cancer treatment with palliative intent and predictors of agreement. Journal of Pain and Symptom Management, 52, 336–344. https://doi.org/10.1016/j.jpainsymman.2016.02.017
Porter, L.S., Samsa, G., Steel, J.L., Hanson, L.C., LeBlanc, T.W., Bull, J., . . . Keefe, F.J. (2019). Caregiver-guided pain coping skills training for patients with advanced cancer: Background, design, and challenges for the CaringPals study. Clinical Trials, 16, 263–272. https://doi.org/10.1177/1740774519829695
Queen, T.L., Butner, J., Berg, C.A., & Smith, J. (2017). Activity engagement among older adult spousal caregivers. Journals of Gerontology, Series B, 74, 1278–1282. https://doi.org/10.1093/geronb/gbx106
Rajasekaran, T., Tan, T., Ong, W.S., Koo, K.N., Chan, L., Poon, D.,. . . Kanesvaran, R. (2016). Comprehensive Geriatric Assessment (CGA) based risk factors for increased caregiver burden among elderly Asian patients with cancer. Journal of Geriatric Oncology, 7, 211–218. https://doi.org/10.1016/j.jgo.2016.03.003
Reblin, M., Small, B., Jim, H., Weimer, J., & Sherwood, P. (2018). Mediating burden and stress over time: Caregivers of patients with primary brain tumor. Psycho-Oncology, 27, 607–612. https://doi.org/10.1002/pon.4527
Riekkola, J., Rutberg, S., Lilja, M., & Isaksson, G. (2019). Healthcare professionals’ perspective on how to promote older couples’ participation in everyday life when using respite care. Scandinavian Journal of Caring Sciences, 33, 427–435. https://doi.org/10.1111/scs.12640
Robinson, B.C. (1983). Validation of a caregiver strain index. Journal of Gerontology, 38, 344–348. https://doi.org/10.1093/geronj/38.3.344
Russell, B., Collins, A., Dowling, A., Dally, M., Gold, M., Murphy, M., . . . Philip, J. (2016). Predicting distress among people who care for patients living longer with high-grade malignant glioma. Supportive Care in Cancer, 24, 43–51. https://doi.org/10.1007/s00520-015-2739-0
Rutkowski, N.A., Lebel, S., Richardson, K., Mutsaers, B., Chasen, M., & Feldstrain, A. (2018). A little help from my friends: Social support in palliative rehabilitation. Current Oncology, 25, 358–365. https://doi.org/10.3747/co.25.4050
Sacher, M., Meixensberger, J., & Krupp, W. (2018). Interaction of quality of life, mood and depression of patients and their informal caregivers after surgical treatment of high-grade glioma: A prospective study. Journal of Neuro-Oncology, 140, 367–375. https://doi.org/10.1007/s11060-018-2962-x
Schulz, R., McGinnis, K.A., Zhang, S., Martire, L.M., Hebert, R.S., Beach, S.R., . . . Belle, S.H. (2008). Dementia patient suffering and caregiver depression. Alzheimer Disease and Associated Disorders, 22, 170–176. https://doi.org/10.1097/WAD.0b013e31816653cc
Segrin, C., Badger, T.A., & Sikorskii, A. (2019). A dyadic analysis of loneliness and health-related quality of life in Latinas with breast cancer and their informal caregivers. Journal of Psychosocial Oncology, 37, 213–227. https://doi.org/10.1080/07347332.2018.1520778
Serwe, K.M., Hersch, G.I., & Pancheri, K. (2017). Feasibility of using telehealth to deliver the “Powerful Tools for Caregivers” program. International Journal of Telerehabilation, 9, 15–22. https://doi.org/10.5195/ijt.2017.6214
Serwe, K.M., Hersch, G.I., Pickens, N.D., & Pancheri, K. (2017). Caregiver perceptions of a telehealth wellness program. American Journal of Occupational Therapy, 71, 7104350010p1–7104350010p5. https://doi.org/10.5014/ajot.2017.025619
Sherwood, P., Given, B., Given, C., Schiffman, R., Murman, D., & Lovely, M. (2004). Caregivers of persons with a brain tumor: A conceptual model. Nursing Inquiry, 11, 43–53.
Shiba, K., Kondo, N., & Kondo, K. (2016). Informal and formal social support and caregiver burden: The AGES Caregiver Survey. Journal of Epidemiology, 26, 622–628. https://doi.org/10.2188/jea.JE20150263
Shin, D.W., Park, K., Jeong, A., Yang, H.K., Kim, S.Y., Cho, M., & Park, J.H. (2019). Experience with age discrimination and attitudes toward ageism in older patients with cancer and their caregivers: A nationwide Korean survey. Journal of Geriatric Oncology, 10, 459–464. https://doi.org/10.1016/j.jgo.2018.09.006
Shumway-Cook, A., Brauer, S., & Woollacott, M. (2000). Predicting the probability for falls in community-dwelling older adults using the Timed Up & Go Test. Physical Therapy, 80, 896–903.
Sibalija, J., Savundranayagam, M.Y., Orange, J.B., & Kloseck, M. (2018). Social support, social participation, & depression among caregivers and non-caregivers in Canada: A population health perspective. Aging and Mental Health. Advance online publication. https://doi.org/10.1080/13607863.2018.1544223
Stacey, F.G., James, E.L., Chapman, K., & Lubans, D.R. (2016). Social cognitive theory mediators of physical activity in a lifestyle program for cancer survivors and carers: Findings from the ENRICH randomized controlled trial. International Journal of Behavioral Nutrition and Physical Activity, 13, 49. https://doi.org/10.1186/s12966-016-0372-z
Stall, N.M., Kim, S.J., Hardacre, K.A., Shah, P.S., Straus, S.E., Bronskill, S.E., . . . Rochon, P.A. (2019). Association of informal caregiver distress with health outcomes of community-dwelling dementia care recipients: A systematic review. Journal of the American Geriatrics Society, 67, 609–617. https://doi.org/10.1111/jgs.15690
Stepler, R. (2015, November 18). 5 facts about family caregivers. Retrieved from http://www.pewresearch.org/fact-tank/2015/11/18/5-facts-about-family-ca…
Sterba, K.R., Armeson, K., Zapka, J., Scallion, M.A., Garris, T.K., Graboyes, E.M., . . . Day, T.A. (2019). Evaluation of a survivorship needs assessment planning tool for head and neck cancer survivor-caregiver dyads. Journal of Cancer Survivorship, 13, 117–129. https://doi.org/10.1007/s11764-019-0732-1
Tana, C., Lauretani, F., Ticinesi, A., Gionti, L., Nouvenne, A., Prati, B., . . . Maggio, M. (2019). Impact of nutritional status on caregiver burden of elderly outpatients. A cross-sectional study. Nutrients, 11, E281. https://doi.org/10.3390/nu11020281
Tatangelo, G., McCabe, M., Macleod, A., & You, E. (2018). “I just don’t focus on my needs.” The unmet health needs of partner and offspring caregivers of people with dementia: A qualitative study. International Journal of Nursing Studies, 77, 8–14. https://doi.org/10.1016/j.ijnurstu.2017.09.011
Thornton, M., & Travis, S.S. (2003). Analysis of the reliability of the Modified Caregiver Strain Index. Journals of Gerontology, Series B, 58, S127–S132. https://doi.org/10.1093/geronb/58.2.s127
Ullgren, H., Tsitsi, T., Papastavrou, E., & Charalambous, A. (2018). How family caregivers of cancer patients manage symptoms at home: A systematic review. International Journal of Nursing Studies, 85, 68–79. https://doi.org/10.1016/j.ijnurstu.2018.05.004
Wittenberg, E., Goldsmith, J.V., Williams, Y., & Lee, A. (2018). Caring for family caregivers: A pilot test of an online COMFORTTM SM communication training module for undergraduate nursing students. Journal of Cancer Education. Advance online publication. https://doi.org/10.1007/s13187-018-1452-3
Wittenberg, E., Xu, J., Goldsmith, J., & Mendoza, Y. (2019). Caregiver communication about cancer: Development of a mhealth resource to support family caregiver communication burden. Psycho-Oncology, 28, 365–371. https://doi.org/10.1002/pon.4950
Wood, R., Taylor-Stokes, G., & Lees, M. (2019). The humanistic burden associated with caring for patients with advanced non-small cell lung cancer (NSCLC) in three European countries—A real-world survey of caregivers. Supportive Care in Cancer, 27, 1709–1719. https://doi.org/10.1007/s00520-018-4419-3
Yang, X., Hao, Y., George, S.M., & Wang, L. (2012). Factors associated with health-related quality of life among Chinese caregivers of the older adults living in the community: A cross-sectional study. Health Quality of Life Outcomes, 10, 143. https://doi.org/10.1186/1477-7525-10-143
Yesavage, J.A., Brink, T.L., Rose, T.L., Lum, O., Huang, V., Adey, M., & Leirer, V.O. (1982). Development and validation of a geriatric depression screening scale: A preliminary report. Journal of Psychiatric Research, 17, 37–49.
Zafar, S.Y., Peppercorn, J.M., Schrag, D., Taylor, D.H., Goetzinger, A.M., Zhong, X., & Abernethy, A.P. (2013). The financial toxicity of cancer treatment: A pilot study assessing out-of-pocket expenses and the insured cancer patient’s experience. Oncologist, 18, 381–390. https://doi.org/10.1634/theoncologist.2012-0279
Zarit, S.H., Todd, P.A., & Zarit, J.M. (1986). Subjective burden of husbands and wives as caregivers: A longitudinal study. Gerontologist, 26, 260–266. https://doi.org/10.1093/geront/26.3.260
Zheng, Y., Head, B.A., & Schapmire, T.J. (2016). A systematic review of telehealth in palliative care: Caregiver outcomes. Telemedicine and e-Health, 22, 288–294. https://doi.org/10.1089/tmj.2015.0090
Zung, W.W., Richards, C.B., & Short, M.J. (1965). Self-rating depression scale in an outpatient clinic. Further validation of the SDS. Archives of General Psychiatry, 13, 508–515.




