Building a Program: Implications for Infrastructure, Nursing Education, and Training for CAR T-Cell Therapy
Background: Chimeric antigen receptor (CAR) T-cell therapy program development has regulatory demands and unique operational processes that vary across settings. The infrastructure in which CAR T-cell therapy is implemented has implications for nursing education and competencies.
Objectives: This article presents an overview of operational approaches to CAR T-cell therapy program development and oncology nurse education considerations. These are provided through the lens of two institutions approved to administer CAR T-cell therapy, with differing approaches to CAR T-cell program development, implementation, and staff training.
Methods: Development of freestanding CAR T-cell therapy programs are compared with programs embedded in a specialty area. Issues related to accreditation and financial considerations are explored. Distinct features of inpatient and ambulatory care settings are presented.
Findings: CAR T-cell therapy continues to expand as the number of centers offering approved therapies increases. Standardized workflow components and staff education are essential for best patient outcomes regardless of location and type of program that provides the therapy.
Jump to a section
As additional chimeric antigen receptor (CAR) T-cell therapies receive U.S. Food and Drug Administration (FDA) approval, more centers will provide care for patients undergoing this novel treatment. Following the approvals of tisagenlecleucel (Kymriah®) and axicabtagene ciloleucel (Yescarta®) in August and October 2017, respectively, programs authorized to administer these therapies burgeoned from 59 in May 2018 (ASCO Post, 2018) to 160 in February 2019 (Kite Pharma, n.d.; Novartis Pharmaceuticals, 2019). Standardized regulatory requirements inform the establishment of programs, but operational needs vary and range from freestanding CAR T-cell therapy programs to incorporating CAR T-cell therapy into existing service lines. Institutional infrastructure for CAR T-cell therapy is essential to meet the complex medical, logistic, training, and regulatory requirements of the treatment. This article presents an overview of current approaches to CAR T-cell therapy program design and implementation, as well as implications for the training and education of nurses providing care to these patients.
Program Oversight
A key decision point in designing and implementing a CAR T-cell therapy program is the determination of program oversight for the therapy because a high demand is placed on institutional resources. In many settings, CAR T-cell therapy has been embedded within existing blood and marrow transplantation (BMT) services. However, some institutions have developed distinct cell therapy–specific programs or may use a primary disease service, such as a leukemia or lymphoma team, for patient management (Mahmoudjafari et al., 2019). The organization of the program infrastructure may vary depending on the number and type of CAR T-cell therapies offered, patient volume, inpatient and outpatient resources, and preexisting service line composition. Regardless of how CAR T-cell therapy is incorporated into the institution, interprofessional teams are needed to effectively deliver this treatment to patients. A focus on determining the safest and most efficient way to support patients through the treatment plan should drive infrastructure decision making because of the complexity of care associated with CAR T-cell therapy.
CAR T-Cell Therapy in Blood and Marrow Transplantation Programs
In institutions with well-established, long-standing BMT programs, embedding the CAR T-cell therapy program within the BMT service may prove advantageous. Memorial Sloan Kettering Cancer Center (MSKCC) uses this approach (Perica, Curran, Brentjens, & Giralt, 2018). Existing BMT programs contain infrastructure that support regulatory, cellular processing, and clinical care delivery elements required for CAR T-cell therapy. Leveraging existing infrastructure can increase efficiency by avoiding system redundancies and capitalizing on optimized workflows.
With FDA approval of commercial CAR T-cell therapy products, MSKCC embedded a consultative service within the pediatric and adult BMT services (Perica et al., 2018). This consultative service was built on the established CAR T-cell therapy clinical trials program. Alignment of care delivery workflow led to an interprofessional workgroup, which tracked CAR T-cell therapy organizational activity. During program expansion, the workgroup provides oversight of complex patient management issues while maintaining the integrity of the research program.
Forming a centralized patient intake process provides one example of optimal workflow alignment. Patients access care via a single telephone line. Then, after compiling intake information, a designated team reviews eligibility for BMT, commercial, or investigational CAR T-cell therapy. The clinical nurse coordinator provides initial coordination of the care for the patient undergoing CAR T-cell therapy. This individual collaborates closely with clinical trials nurses to complete preliminary patient screening and gather relevant clinical information, such as laboratory and radiologic findings. The clinical nurse coordinator communicates results with the physician evaluation team and coordinates all pretreatment requirements, including patient education regarding the treatment plan and side effect management (McGuirk et al., 2017). The clinical nurse coordinator is available during the day to provide these services, but after-hours calls go to the on-call physician.
Established BMT programs have additional components that support embedding CAR T-cell therapy services. Data and quality management teams for BMT are well suited to maintain the data reporting and regulatory monitoring of the CAR T-cell therapy consultative service because of similar requirements for BMT therapies (Foundation for the Accreditation of Cellular Therapy [FACT], 2018a, 2018b). Apheresis centers supporting BMT programs must meet current regulatory requirements, such as those of FACT (2018a, 2018b) and the FDA (2018). Leveraging these existing staff and established processes for cell collection, storage, shipping, and receiving for CAR T-cell therapy programs provides an established foundation for a safe and efficient integration of this therapy. In addition, existing policies for cell thaw and infusion serve as a foundation for further development based on CAR T-cell therapy–specific requirements and regulations, potentially providing greater efficiency than creating new policies. Where applicable, programs can adopt existing clinical documentation methods and infusion monitoring flow sheets. Although BMT programs provide many of the operational and logistical features required for CAR T-cell therapy, program requirements can extend beyond BMT program content. One of the most significant differences is post–T-cell infusion management, when risk increases for cytokine release syndrome (CRS) and neurologic toxicity (NT).
CAR T-Cell Therapy Programs Separate From Blood and Marrow Transplantation Programs
Other institutions, such as the Seattle Cancer Care Alliance (SCCA), have established distinct programs for CAR T-cell therapy from existing BMT programs while continuing to leverage some aspects of the BMT infrastructure. For this program model, a separate service can centralize clinical care and staff education while developing expert teams to manage the treatment’s unique CRS and NT.
At SCCA, a cellular immunotherapy service provides clinical care in the outpatient setting while sharing existing quality, regulatory, cell therapy, and inpatient care with the BMT program. The service accommodates the growth of cell therapy trials across a variety of disease groups and T-cell types, as well as increasing patient volume. This outpatient location is staffed by a dedicated clinical care team that includes oncology physicians, advanced practice providers (APPs), nurses, pharmacists, social workers, and support staff.
Outpatient care includes evaluation, treatment (including lymphodepleting chemotherapy and cell infusions), and post-treatment monitoring. Outpatient clinic visits and infusion therapy are available seven days a week from 8 am to 8 pm in the department to ensure patients can be seen daily. FDA-approved CAR T-cell therapy, as well as investigational CAR T-cell, tumor infiltrating lymphocytes, and T-cell receptor therapies, are managed through this service. Outpatient triage and direct admission to the hospital unit are modeled from the well-developed BMT program care protocols to support patients receiving outpatient therapy. After-hours patient concerns are directed to a designated hospital nocturnist (a hospital-based physician who works during the night). This approach has allowed for the consolidation of cellular therapies in a centralized service, easing the administrative burden on individual disease teams and enhancing expertise in the unique toxicities of CAR T-cell therapy.
Referral pathways to a non–BMT-based CAR T-cell therapy clinical program determines how patients will access the therapy. At SCCA, an intake team of administrative staff and APPs works in conjunction with immunotherapy physicians and investigators to manage patient referrals for nontransplantation cellular therapies, both commercial and research. These pathways provide a centralized contact location for internal and external referral sources and promote prompt identification of available cellular therapy treatment options for patients.
Some institutions may embed CAR T-cell therapy within existing disease services, such as hematologic malignancies. When embedded in existing disease services, additional resources still are required to manage the cell therapy regulatory requirements and acute toxicities of treatment outside of a BMT or specialized CAR T-cell therapy program.
Regardless of the approach to oversight, successful CAR T-cell therapy programs require specialized interprofessional teams to address the complex infrastructure and patient care needs inherent in such programs. Table 1 provides an overview of possible roles and corresponding functions during CAR T-cell therapy implementation. 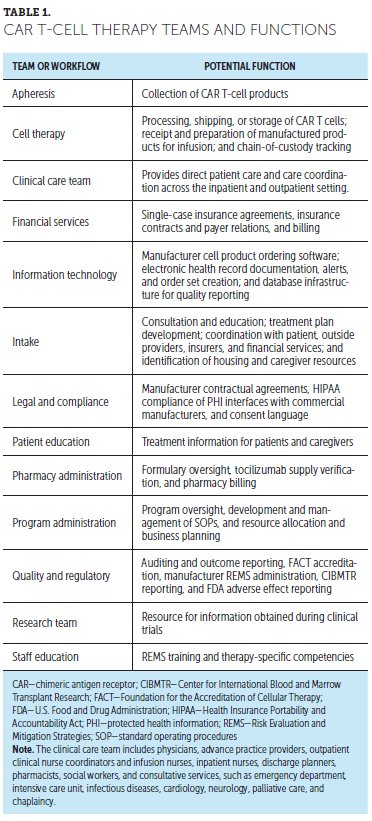
CAR T-Cell Infusion Settings
In addition to establishing oversight, programs also determine the context of care for CAR T-cell therapy. Although CAR T-cell therapy infusions most commonly occur in the inpatient setting (Komanduri, 2017), programs are expanding to include ambulatory infusions for some FDA-approved agents. Outpatient administration is not prohibited for either FDA-approved CAR T-cell agent; however, the onset, severity, and management of toxicities for each product are key considerations when determining preferred administration location (Teachy, Bishop, Maloney, & Grupp, 2018).
Similarities exist between inpatient and ambulatory settings, such as administration and monitoring of CAR T cells and nurse education. For example, cell therapy laboratory personnel must be able to travel to separate inpatient or outpatient locations with cell products, and a water bath must be available to defrost cells. Identification of an on-site care provider to respond to acute infusion issues is critical. There are, however, some unique considerations for each location.
Inpatient Considerations
Depending on inpatient census and unit size, the program may begin by embedding patients undergoing CAR T-cell therapy within the BMT unit, even if there is a freestanding program in the ambulatory setting. Inpatient BMT units are designed to meet FACT (2018b) standards for infection control, including methods to reduce airborne microbial contamination. The standards recommend positive-pressure HEPA filtration for rooms of patients at high-risk for infection. When HEPA filtration is not available, patients stay in single-patient rooms with measures to reduce exposure to sources of infection (FACT, 2018b).
Even when the patient care unit is not exclusively focused on CAR T-cell therapy, nurses providing care on the unit require focused CAR T-cell therapy education. Expert nurse staffing is challenging if staff varies day to day or if nurses are not prepared to care for patients undergoing CAR T-cell therapy. Strategies to provide CAR T-cell therapy education consistent with FACT (2018b) requirements include establishing expert resource teams or designated intensive care unit nurse support (see Table 2). 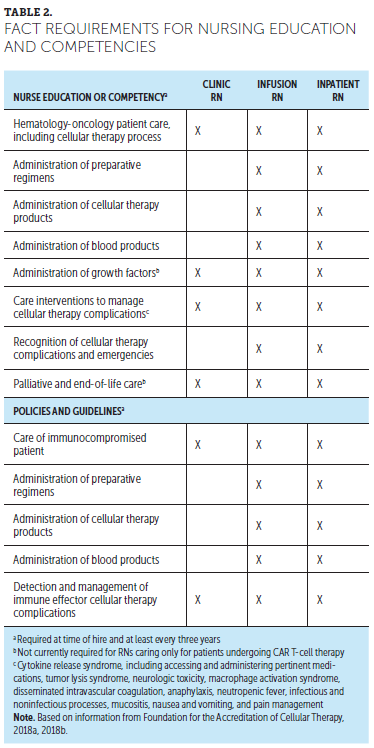
Outpatient Considerations
Additional factors should be taken into consideration when caring for patients undergoing CAR T-cell therapy in the outpatient setting. Access to care 24 hours per day, 7 days per week is a key consideration (FACT, 2018a, 2018b). Patients should be provided with a product-specific wallet card identifying that they have received a CAR T-cell product and providing information about the treating oncologist. Patient education for prompt symptom recognition and reporting is essential to the successful management of these patients (Kite Pharma, 2018; Novartis Pharmaceuticals, 2018b). All patients must be able to reliably contact a provider familiar with CAR T-cell therapy for new symptoms and to quickly access in-person assessment. This may occur through clinic triage, the emergency department (ED), or direct admission to a designated unit. Ideally, a bed on a designated unit is readily available. Procedures should be developed for times of high patient volume, which would ensure availability of appropriate beds. If a patient contacts a provider with symptoms and is unable to be directly admitted to an inpatient unit, the provider can then coordinate with the ED provider and act as a resource. Patients should be educated to show their wallet card any time they present with symptoms to a site outside of the BMT or CAR T-cell programs, such as the ED or an outside hospital. Staff in the ED should be educated about the potential to see a patient with symptoms of CRS or NT from CAR T-cell therapy, which may be similar to sepsis or cerebrovascular accident (Kite Pharma, 2018; Novartis Pharmaceuticals, 2018b). Testing of identified workflows is helpful to ensure that processes work as designed.
Outpatient Facilities
Logistical considerations for outpatient CAR T-cell therapy administration include room design and clinic hours. Per FACT (2018b) standards, the space should be designed to reduce the risk of infection transmission and allow for patient isolation. Hours of clinic operation must be long enough to support infusion, monitoring, and buffer time for unexpected process delays.
Access to daily clinic visits and infusions are important to be able to support patients receiving CAR T-cell therapy. Physical assessments, including neurologic status, regular laboratory and infusions of blood products, hydration, and medications, may be needed in the weeks following CAR T-cell therapy administration (Kite Pharma, 2017; Novartis Pharmaceuticals, 2018a). Laboratory, pharmacy, nursing, and APP or physician availability is fundamental to providing comprehensive outpatient care.
Caregiver Support
Inclusion of the caregiver in informed consenting and teaching and clinic visits should be expected at all time points in therapy. Education at the time of intake is imperative to ensure that patients and caregivers understand program requirements, such as the need for a 24-hour caregiver for at least four weeks or staying close to the center after treatment (Perica et al., 2018). If patients have rotating caregivers, establishing the coverage plan for the expected duration of therapy up front can help prevent unexpected gaps in caregiver availability. Caregiver support following therapy is critical to outpatient CAR T-cell therapy safety because of known toxicities. Social workers can assist with finding resources for housing, providing financial guidance, and completing family leave paperwork for patients and caregivers, in addition to providing psychosocial support.
Nursing Preparation
Comprehensive care for patients receiving CAR T-cell therapy requires nurses knowledgeable in the management of hematologic malignancies, BMT, and immunotherapy principles (FACT, 2018b). Because many facilities implementing CAR T-cell therapy programs do so in conjunction with an established BMT or hematologic malignancy program (Mahmoudjafari et al., 2019), established core curriculum of those programs also meets CAR T-cell therapy program needs. Standardized preparation of nurses includes management of treatment side effects, recognition and management of oncologic emergencies, and blood product and chemotherapy administration. As solid tumor targets for CAR T-cell therapy evolve, nurses specialized in hematologic malignancies may need to broaden their scope of clinical expertise and knowledge about solid tumor cancers.
Additional focused education includes CAR T-cell therapy treatment timelines, cellular infusion procedures, and management of unique side effects, such as CRS and NT. Recommendations from the Oncology Nursing Society (Wiley et al., 2017) state the importance of nurses knowing the class, specific agent, and protocols to follow to guide the administration and monitoring for patients receiving immunotherapy agents. Nurses caring for patients receiving commercial CAR T-cell therapy products are also required to complete product-specific Risk Evaluation and Mitigation Strategy (REMS) training (Kite Pharma, 2018; Novartis Pharmaceuticals, 2018b).
As CAR T-cell therapy evolves, programs can best serve nursing staff by establishing continuing education, offering periodic competency assessment, and providing updates about evidence-based care delivery. FACT (2018a, 2018b) has established standards for nursing training and competency for both BMT and immune effector cell (IEC) therapy. These standards serve as a guide for training and ongoing competency, regardless of an organization’s accreditation by FACT (n.d.).
Implementation of these education requirements may vary based on the primary role of the nurse (clinic or infusion), location of practice (inpatient or outpatient), and whether the CAR T-cell therapy program is embedded in a BMT or freestanding program. Methods to educate staff are chosen based on the topic, desired outcome of the education, and principles of the adult learner. A didactic course, either in person or online, may be appropriate for general information where a one-on-one demonstration with a skills checklist may be better suited for a procedural task. APP training and competency are consistent with the physician requirements listed in the seventh edition of the FACT (2018b) standards and can be referred to for additional details.
In centers with combined BMT and CAR T-cell therapy programs, it is important to collaborate to ensure consistency in staff practice. Centers must also develop policies and procedures for product infusion and patient assessment if not already in place. Organizational practices for managing patient care should have consistent policies and procedures across BMT and CAR T-cell therapy programs to support safe and effective care for patients.
Financial Considerations
Because of the significant costs of CAR T-cell therapy, financial clearance for therapy is an important part of the intake process. CAR T-cell therapy is covered by most commercial payers on a case-by-case basis. Because CAR T-cell therapy is a newer treatment, total treatment costs can be unpredictable and are often affected by insurance contracts between insurers and institutions—termed single-case agreements—that outline reimbursement rates. Established payers have become more familiar with CAR T-cell therapy and are better equipped to negotiate and efficiently facilitate financial agreements. However, some payers are unfamiliar with these novel therapies and require periods of extended contract mediation, delaying the patient’s treatment.
Medicare reimbursement guidelines for commercial CAR T-cell therapy continue to evolve. The Centers for Medicare and Medicaid Services (CMS) outlined its 2019 Medicare national inpatient payment rate (under the diagnosis-related group (DRG)–autologous bone marrow transplantation or CAR T-cell immunotherapy) with an approximate payment of $39,000 to the institution (American Society for Blood and Marrow Transplantation [ASBMT], 2018; CMS, 2018). CMS also authorized a temporary new technology add-on payment with a maximum payment of $186,500 for eligible institutions (ASBMT, 2018). Because product acquisition costs range from $373,000 to $475,000, a resulting gap between cost and reimbursement may be approximately $186,000, which could affect the long-term financial viability of these agents (ASBMT, 2018; Gallegos, 2018). CAR T-cell therapy reimbursement changes will continue, requiring treatment centers to stay abreast of national and regional policies (Mahmoudjafari et al., 2019).
Outpatient administration of CAR T-cell therapy has a different payment structure under CMS guidelines, with a higher reimbursement rate ranging from $395,380 to $500,839 (Gallegos, 2018). CMS’s three-day rule transfers reimbursement rates to the inpatient rate if the patient is admitted to the hospital within three days of CAR T-cell therapy infusion (CMS, 2014; Gallegos, 2018). DRG-exempt cancer centers are reimbursed based on a different methodology and have different guidelines that apply. A product-specific timeline to side effect onset should be the primary consideration for determination of treatment and infusion location.
Geographic location of certified treatment facilities often requires patient relocation for treatment. Consideration of patient disease status, treatment timeline, and feasibility of therapy must be strategized carefully. Streamlined processes to obtain insurance approval and contracting agreements are crucial to expedite patient treatment. Delays in financial approval may impair a patient’s ability to undergo therapy. Support programs may be available through insurers or product manufacturers to assist with reimbursement, claims appeals, and travel and lodging.
Accreditation
Recognizing various approaches to develop a CAR T-cell therapy program infrastructure that promotes quality care, FACT (2018a; 2018b) has developed guidelines for BMT programs and IEC programs, which include products like CAR T cells and tumor-infiltrating lymphocytes (Maus & Nikiforow, 2017). The FACT accreditation process, like that of the Joint Commission, establishes rigorous criteria for safe care delivery that is transparent to the public. FACT (2018b) standards are developed through collaboration by those working in cellular therapy, and inspections are performed by those actively working in the field. These standards were initially developed for BMT; the IEC standards were added in January 2017. To date, accreditation is voluntary; however, commercial CAR T-cell therapy manufacturers, as well as some insurers, have indicated a preference for centers that are FACT-accredited for BMT and endorse receiving accreditation specifically for IEC (BlueCross BlueShield Association, 2018). CAR T-cell therapy programs can be accredited either as part of a BMT service or as freestanding programs.
Training and competency requirements have been established by FACT (2018a, 2018b) for all staff. FACT has also defined standards for the physical environment of the clinical unit(s), evaluation and management of the donor and recipient (autologous and allogeneic), required policies, performance of clinical research, quality management, and reporting of data. Many of these standards apply to BMT and IEC programs, supporting potential efficiencies of a combined program.
In the case of a combined program, a survey by FACT (every three years) is required to maintain accreditation. If a program were to seek independent IEC accreditation, the same survey would apply. When the CAR T-cell therapy program is separate from the BMT program in the same organization, each program will be surveyed independently. Many components within the individual programs may cross over between IEC and BMT, but each program requires FACT accreditation and must submit survey information of those components, including quality and data management programs and personnel data, which includes nurses. 
Conclusion
As CAR T-cell therapy programs continue to expand, nurses can take the lead in program development, education, and training. Although oversight from embedded or freestanding programs and care requirements will continue to evolve, existing standards from organizations, such as FACT, provide structure from which to build safe and effective programs. For those developing programs, use of regulatory, organizational, and evidence-based standards is fundamental to supporting the development of a successful program, and, ultimately, the safe and effective care of patients.
About the Author(s)
Lenise Taylor, MN, RN, AOCNS®, BMTCN®, is a clinical nurse specialist at the Seattle Cancer Care Alliance and University of Washington Medical Center in Seattle; Elizabeth S. Rodriguez, DNP, RN, OCN®, is the director of nursing in the David H. Koch Center for Cancer Care at Memorial Sloan Kettering Cancer Center in New York, NY; Anne Reese, BSN, RN, OCN®, is an RN and professional practice coordinator at the Seattle Cancer Care Alliance and Bezos Family Immunotherapy Clinic; and Karen Anderson, MN, RN, AOCNS®, BMTCN®, CRNI, is a PhD student in the College of Nursing at the University of Arizona in Tucson and an infusion RN manager at the Banner University of Arizona Cancer Center in Tucson. The authors take full responsibility for this content. This supplement was supported by an independent educational grant from Bristol-Myers Squibb. Anderson has previously served on advisory boards for Kite Pharma. The article has been reviewed by independent peer reviewers to ensure that it is objective and free from bias. Mention of specific products and opinions related to those products do not indicate or imply endorsement by the Oncology Nursing Society. Taylor can be reached at ltaylor@seattlecca.org, with copy to CJONEditor@ons.org. (Submitted January 2019. Accepted January 31, 2019.)
References
American Society for Blood and Marrow Transplantation. (2018). Re: Follow-up to August 30, 2018 meeting; Proposed CAR-T coverage and payment options. Retrieved from http://www.hematology.org/Advocacy/ASH-Testimony/2018/9101.aspx
ASCO Post. (2018, May 25). Treatment centers authorized to administer CAR T-cell therapy. Retrieved from http://www.ascopost.com/issues/may-25-2018/treatment-centers-authorized…
BlueCross BlueShield Association. (2018). Blue Distinction® Centers for Cellular Immunotherapy CAR-T therapy selection criteria. Retrieved from https://www.bcbs.com/sites/default/files/file-attachments/page/BDSC_Cel…
Centers for Medicare and Medicaid Services. (2014). Three day payment window: Implementation of new statutory provision pertaining to Medicare 3-day (1-day) payment window policy—Outpatient services treated as inpatient. Retrieved from https://www.cms.gov/Medicare/Medicare-Fee-for-Service-Payment/AcuteInpa…
Centers for Medicare and Medicaid Services. (2018). Medicare program; hospital inpatient prospective payment systems for acute care hospitals and the long-term care hospital prospective payment system and policy changes and fiscal year 2019 rates; quality reporting requirements for specific providers; Medicare and Medicaid electronic health record (EHR) incentive programs (promoting interoperability programs) requirements for eligible hospitals, critical access hospitals, and eligible professionals; Medicare cost reporting requirements; and physician certification and recertification of claims. Retrieved from https://bit.ly/2AAZMLb
Foundation for the Accreditation of Cellular Therapy. (n.d.). What FACT accreditation means to patients and their families. Retrieved from http://www.factwebsite.org/Inner.aspx?id=351
Foundation for the Accreditation of Cellular Therapy. (2018a). FACT immune effector cells accreditation manual (1st ed., v.1.1). Omaha, NE: Author.
Foundation for the Accreditation of Cellular Therapy. (2018b). FACT-JACIE international standards for hematopoietic cellular therapy product collection, processing and administration (7th ed.). Omaha, NE: Author.
Gallegos, A. (2018). CMS finalizes CAR T-cell therapy inpatient payments. Oncology Practice. Retrieved from https://www.mdedge.com/oncologypractice/article/173086/practice-managem…
Kite Pharma. (n.d.). Yescarta® authorized treatment centers. Retrieved from https://www.yescarta.com/treatment-centers
Kite Pharma. (2017). Yescarta® (axicabtagene ciloleucel) [Package insert]. Retrieved from https://www.fda.gov/downloads/UCM581226.pdf
Kite Pharma. (2018). Yescarta® (axicabtagene ciloleucel) Risk Evaluation and Mitigation Strategy. Retrieved from https://www.yescartarems.com
Komanduri, K. (2017). American Society for Blood and Marrow Transplantation FY19 CAR-T MS-DRG request [open letter]. Retrieved from https://higherlogicdownload.s3.amazonaws.com/ASBMT/43a1f41f-55cb-4c97-9…
Mahmoudjafari, Z., Hawks, K.G., Hsieh, A.A., Plesca, D., Gatwood, K.S., & Culos, K.A. (2019). American Society for Blood and Marrow Transplantation Pharmacy Special Interest Group survey on chimeric antigen receptor T cell therapy administrative, logistic, and toxicity management practices in the United States. Biology of Blood and Marrow Transplantation, 25, 26–33. https://doi.org/10.1016/j.bbmt.2018.09.024
Maus, M.V., & Nikiforow, S. (2017). The why, what, and how of the new FACT standards for immune effector cells. Journal for Immunotherapy of Cancer, 5, 36. https://doi.org/10.1186/s40425-017-0239-0
McGuirk, J., Waller, E.K., Qayed, M., Abhyankar, S., Ericson, S., Holman, P., . . . Myers, G.D. (2017). Building blocks for institutional preparation of CTL019 delivery. Cytotherapy, 19, 1015–1024. https://doi.org/10.1016/j.jcyt.2017.06.001
Novartis Pharmaceuticals. (2018a). Kymriah® (tisagenlecleucel) [Package insert]. Retrieved from https://www.fda.gov/downloads/UCM573941.pdf
Novartis Pharmaceuticals. (2018b). Kymriah® (tisagenlecleucel) Risk Evaluation and Mitigation Strategy (REMS). Retrieved from http://www.kymriah-rems.com
Novartis Pharmaceuticals. (2019). Find a Kymria® treatment center. Retrieved from https://www.us.kymriah.com/treatment-center-locator
Perica, K., Curran, K.J., Brentjens, R.J., & Giralt, S.A. (2018). Building a CAR garage: Preparing for the delivery of commercial CAR T cell products at Memorial Sloan Kettering Cancer Center. Biology of Blood and Marrow Transplantation, 24, 1135–1141. https://doi.org/10.1016/j.bbmt.2018.02.018
Teachy, D.T., Bishop, M.R., Maloney, D.G., Grupp, S.A., (2018). Toxicity management after chimeric antigen receptor T cell therapy: One size does not fit ‘ALL’. Nature Reviews. Clinical Oncology, 15, 218.
U.S. Food and Drug Administration. (2018). CFR—Code of federal regulations Title 21. Retrieved from https://www.accessdata.fda.gov/scripts/cdrh/cfdocs/cfcfr/CFRSearch.cfm?…
Wiley, K., LeFebvre, K.B., Wall, L. Baldwin-Medsker, A., Nguyen, K., Marsh, L., & Baniewicz, D. (2017). Immunotherapy administration: Oncology Nursing Society recommendations. Clinical Journal of Oncology Nursing, 21(2, Suppl.), 5–7. https://doi.org/10.1188/17.CJON.S2.5-7




