Caregiver-Reported Health Outcomes: Effects of Providing Reflexology for Symptom Management to Women With Advanced Breast Cancer
Purpose/Objectives: To determine the effects of delivering a reflexology intervention on health outcomes of informal caregivers, and to explore whether intervention effects are moderated by caregiver characteristics.
Design: Two-group, randomized clinical trial.
Setting: Eight oncology clinics in urban and rural regions of Michigan and Illinois.
Sample: 180 informal caregivers of patients with advanced breast cancer.
Methods: Caregivers were randomized to provide reflexology to individuals with cancer during a four-week period or to attention control. Data collection occurred at baseline and at weeks 5 and 11. Linear mixed-effects modeling was used to test intervention effects among all participants and the effects of the number of sessions delivered in the reflexology group.
Main Research Variables: Caregiver characteristics; psychological, physical, and social outcomes.
Findings: Caregiver fatigue in the reflexology group was reduced compared to controls at weeks 5 (p = 0.02) and 11 (p = 0.05). No differences were found for anxiety, depression, pain, physical function, sleep disturbance, satisfaction with participation in social roles, and pain interference between caregivers who delivered reflexology and those who did not.
Conclusions: Informal caregivers who provided reflexology to individuals with cancer did not have negative psychological, physical, or social outcomes. Fatigue levels were lower among caregivers who provided reflexology.
Implications for Nursing: Clinicians need to be aware that providing supportive care interventions, such as reflexology, to reduce symptom burden does not increase negative outcomes on informal caregivers who provide this care, and it may even lead to reduced fatigue.
Jump to a section
The number of caregivers supporting people with cancer was estimated to be 2.8 million in 2015 (National Alliance for Caregiving, 2016). Friend or family caregivers are individuals identified by the patient (Stenberg, Ruland, & Miaskowski, 2010) who provide unpaid assistance with chronic or disabling conditions, such as cancer (American Cancer Society, 2017; National Alliance for Caregiving, 2016). Engaging informal caregivers to provide symptom management can support patients with serious conditions (Reinhard, Given, Petlick, & Bemis, 2008). However, the time and type of activities devoted to caregiving may affect caregivers’ psychological, physical, and social health outcomes (Bevans & Sternberg, 2012; Girgis et al., 2013; Given, Given, & Sherwood, 2012; Northouse et al., 2013; Weiss et al., 2016). Integrative therapies, also known as complementary and alternative medicine (CAM), provide options for cancer symptom management when used in conjunction with standard medical care (National Cancer Institute, 2016). Reflexology, the application of pressure on specific reflexes located on the hands and feet, is an integrative therapy that has been tested with women with breast cancer for symptom management (Wyatt, Sikorskii, Rahbar, Victorson, & You, 2012). This article reports the findings on psychological, physical, and social health outcomes among informal caregivers who provided reflexology to patients with breast cancer to support symptom management.
Literature Review
Studies indicate that health may be affected by caregiving (Bradley et al., 2009; Lambert, Girgis, Lecathelinais, & Stacey, 2013; Northouse et al., 2013). A systematic review by Stenberg et al. (2010) identified pain, insomnia, and fatigue as the most prevalent physical problems, and depression and anxiety as the most prevalent emotional problems among caregivers of people with cancer. Caregivers of patients with cancer had higher levels of anxiety, depression, and sleep dysfunction (Applebaum, Farran, Marziliano, Pasternak, & Breitbart, 2014; Corà, Partinico, Munafò, & Palomba, 2012). Social health is also influenced as more time is devoted to caregiving activities and diminished in other aspects of daily life (Given et al., 2012; Stenberg et al., 2010; Van Houtven, Voils, & Weinberger, 2011). Caregiver characteristics, such as age, sex, race, ethnicity, spiritual preference, marital status, relationship to patient, employment, and health status, are important considerations when evaluating caregivers with differing health outcomes (Van Houtven et al., 2011). The personal relationship of the informal caregiver to the patient adds a dimension to the role that makes it uniquely different from professional patient–caregiver relationships. Such personal relationships may contribute to similar distress levels for the patient and caregiver (Badger et al., 2011; Northouse et al., 2013). For example, psychological and physical responses to a cancer diagnosis dually affect the patient and the caregiving spouse (Litzelman, Green, & Yabroff, 2016).
In contrast to research that provides knowledge of the effects of caring for a patient with cancer, less is known about how supportive interventions delivered by caregivers affect health outcomes (Hopkinson, Brown, Okamoto, & Addington-Hall, 2012). This study informs the science and practice of symptom management interventions by providing an understanding of the experience of informal caregivers while they support patients as an integral part of the cancer care team.
Conceptual Model
Adapted from Van Houtven et al. (2011), the caregiver outcomes model guided analysis of health outcomes for caregivers providing reflexology for symptom management to women with breast cancer. Symptom management of this type is particularly significant because it provides a sustainable in-home option that does not rely on external interventionists and is not limited to the study protocol period. The adapted model, operationalized in Figure 1, integrates the care activities performed on behalf of people with cancer, characteristics of caregivers of patients with cancer, and caregiver outcomes associated with psychological, physical, and social health (Frambes, Given, Lehto, Sikorskii, & Wyatt, 2017). The model accommodates not only direct relationships, but also potential moderation effects, defined by Baron and Kenny (1986) as variables that influence the direction or strength of relationship between independent and dependent variables.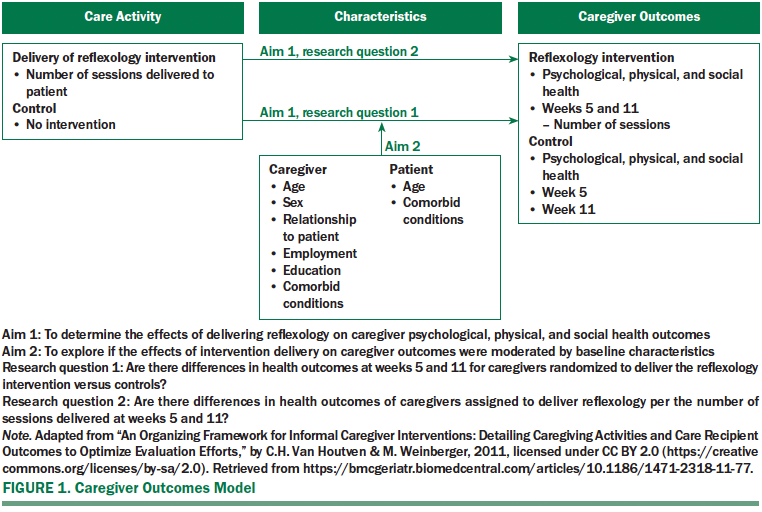
Purpose and Objectives
The primary purpose of the study was to determine the effects of delivering reflexology on caregiver psychological, physical, and social health outcomes. A secondary objective was to explore if the effects of intervention delivery on caregiver outcomes were moderated by caregiver and/or patient baseline characteristics, including age, sex, employment, and comorbidity. Specific research questions included the following:
• Are there differences in health outcomes at weeks 5 and 11 for caregivers randomized to deliver the reflexology intervention versus controls?
• Are there differences in health outcomes of caregivers assigned to deliver reflexology per the number of sessions delivered at weeks 5 and 11?
• Is there evidence for potential moderation of intervention effects by patient and caregiver age; caregiver sex, relationship to patient, employment, and medication; and health status (comorbid conditions)?
Methods
Design
A secondary analysis was used to examine outcomes in a sample of caregivers who were participants in a two-group randomized, controlled trial called Home-Based Symptom Management via Reflexology for Breast Cancer Patients (R01 CA157459), conducted from 2011–2016. The informal friend and family caregivers were chosen by women with advanced breast cancer and were trained by study staff to deliver a four-week reflexology protocol to the patient, if randomized to the intervention group. If randomized to the control group, caregivers received reflexology training after study completion. Patients in both groups received weekly symptom assessment, which provided attention in the control group. Caregivers provided data regarding their psychological, physical, and social health, and delivery of reflexology to the patient at baseline, one week after completion of the intervention (week 5), and at week 11 to determine any sustained effects.
Institutional review board approval for ethical treatment and protection of human participants was received from the investigators’ university and all recruitment sites. Signed informed consent was obtained from all participants. Data were stored on a secure study server at the investigators’ university; access to data was restricted by password protection and managed per institutional review board–approved procedures.
The main study findings on the primary outcome of patient symptom severity are reported elsewhere (Wyatt et al., 2016). Briefly, a significant reduction in patient symptoms was observed over time in the reflexology group compared to controls.
Setting and Participants
Caregivers and patients were recruited as dyads from eight cancer centers in central Michigan and in Illinois that served women from urban, suburban, and rural communities. Inclusion criteria for patients were the following: (a) aged 21 years or older; (b) diagnosed with stage III or IV breast cancer; (c) able to perform basic activities of daily living; (d) receiving chemotherapy or hormonal therapy; (e) able to speak and understand English; (f) have access to a telephone; (g) able to hear conversation; (h) cognitively oriented to time, place, and person (determined by recruiter); and (i) have a caregiver willing to participate in the study. Patient exclusion criteria were the following: (a) documented diagnosis of major mental illness (verified by the clinical record), (b) nursing home residency, (c) bedridden, (d) currently receiving regular reflexology, or (e) diagnosed with deep vein thrombosis or painful foot neuropathy.
The caregiver inclusion criteria were the following: (a) friend or family member identified by the patient; (b) aged 18 years or older; (c) able and willing to provide the 30-minute protocol for four consecutive weeks; (d) able to speak and understand English; (e) have access to a telephone; (f) able to hear conversation; and (g) cognitively oriented to time, place, and person (determined by recruiter). The caregiver exclusion criteria were being unwilling or being unable to perform a return demonstration of the protocol with 90% accuracy according to training procedures. Training of caregivers and all sessions of reflexology were provided in the patient’s home.
Intervention
The research protocol specified that caregivers deliver a minimum of one session of reflexology per week to the patient for four consecutive weeks, with additional sessions if desired by the patient and caregiver. The protocol consisted of nine foot reflexes being stimulated by using a thumb-walking motion for 15 minutes per foot. A caregiver control group received usual care alone. Following the four-week protocol period, caregivers could continue delivering reflexology sessions.
Data Collection
Trained staff collected caregiver data from both study groups via telephone at baseline and at weeks 5 and 11. Each contact took about 30–45 minutes to complete and consisted of questions pertaining to the caregivers’ psychological, physical, and social health. In addition, demographic data were obtained during the first contact. Data were collected from patients on the same schedule and through weekly symptom calls during weeks 1–4. Caregivers who provided reflexology to patients were also called weekly during the four-week intervention period to obtain data regarding the number of sessions provided to the patient. Each call took about 10 minutes to complete.
Measures
The Patient-Reported Outcomes Measurement Information System ([PROMIS], 2016) Profile-29 was used to obtain psychological, physical, and social health data. The items that make up the PROMIS instruments were developed and tested for use with the general U.S. population with funding support from the National Institutes of Health (American Institutes for Research, 2016). The PROMIS-29 is a collection of short forms, each containing four items from seven primary PROMIS domains (depression, anxiety, physical function, fatigue, sleep disturbance, satisfaction with participation in social roles, and pain interference) rated on a Likert-type scale from 0–4 and a single item rating pain severity ranging from 0 (no pain) to 10 (worst imaginable) (PROMIS, 2016). PROMIS measures are reported as t scores, with the U.S. population mean being 50, with a standard deviation of 10. Higher values represent more of the construct present.
Short forms for anxiety (four items) and depression (four items) were used to measure psychological health (PROMIS, 2016). Anxiety items have the respondent rate frequency of feeling fearful, difficulties focusing, worry, and uneasiness during the past seven days. Similarly, the depression items include perceptions of worthlessness, helplessness, depression, and hopelessness during the past seven days. Both forms use a 0–4 scale for each item, with higher values representing higher frequency. Cronbach alphas were 0.9 for anxiety and 0.91 for depression.
Short forms for fatigue (four items), pain severity (one item, 0–10 scale), physical function (four items), and sleep disruption (four items) were used to assess physical health (PROMIS, 2016). Fatigue items reflect extent of fatigue during the past seven days. Cronbach alpha for the fatigue form was 0.9. The pain severity item represents pain experienced during the past seven days ranging from no pain (0) to the worst imaginable pain (10). Physical function items consist of four items rated on a scale from 0–4, with larger values representing higher levels of difficulty experienced during the past seven days. Physical function items reflect the respondent’s ability to complete chores, use stairs, walk, and run errands or shop during the past seven days. Cronbach alpha for the physical function short form was 0.91. The sleep disruption items are used for rating quality, nature, problems with sleep, and difficulties falling asleep, with larger values indicating better sleep quality. Cronbach alpha for sleep disruption was 0.84.
Social health (four items) reflects satisfaction with participation in social roles, including the amount and ability to work, ability to complete personal and household duties, and satisfaction with ability to perform daily routines during the past seven days. Higher values on the 0–4 scale reflect greater levels of satisfaction. Cronbach alpha for satisfaction with participation in social roles was 0.92.
The pain interference short form consists of four items indicative of the amount of interference from pain relative to performance of daily activities, work around the home, ability to participate in social activities, and enjoyment of life (PROMIS, 2016). Higher values on the 0–4 scale indicate higher levels of interference from pain during the past seven days. Cronbach alpha for pain interference was 0.93.
Information about the number of reflexology sessions during the intervention period was obtained from caregivers’ self-report during weekly telephone calls initiated by study staff. The number of reflexology sessions provided by the caregiver following the intervention period was obtained from patients during the exit interview at week 11.
Demographic data derived from caregivers included age, sex, race, ethnicity, marital status (reported as single, married/partnered, widowed, or divorced), relationship to patient with breast cancer, and employment status. Caregiver comorbidity was measured using the Bayliss Instrument, which identifies the presence of 21 common chronic conditions and associated ratings of associated limitations on daily activities (Bayliss, Ellis, & Steiner, 2009).
Data Analysis
Because all caregiver outcomes were specified a priori, the primary analyses used a 0.05 level of significance for two-sided tests. For the exploratory moderation analyses, findings were given lower strength of interpretation (p ≤ 0.1) and were considered hypothesis-generating for future research. SAS®, version 9.4, was used for data analyses.
Baseline comparisons for caregivers in the reflexology and control groups were performed using t tests and chi-square tests for caregiver characteristics, potential moderators, and outcome variables.
Data from participants were analyzed as randomized, using the intention-to-treat principle. Attrition rates and reasons were compared to determine that the lack of differences between groups at baseline was not affected by attrition.
The primary analysis examined the effects of providing reflexology on the caregiver’s psychological, physical, and social health outcomes, as measured by the PROMIS instruments. Each health outcome was analyzed separately using the linear mixed-effects (LME) model that generalizes classical analysis of repeated measures and allows for data missing at random, time-varying covariates, and structured covariance matrix. Group assignment (reflexology or control); caregiver health outcomes at baseline, 5 weeks, or 11 weeks; and time by group interaction were entered as explanatory variables. The least squares (LS) mean at each time point was output from the model, and a test of the difference by study group yielded a formal test of significance for the hypotheses associated with the first research question. For the second research question, data were analyzed to determine the relationship between the number of sessions provided and caregiver health outcomes at weeks 5 and 11. The group assignment variable was not applicable in this analysis; instead, the number of reflexology sessions delivered during the four-week intervention period and during weeks 5–11 was the variable of interest in the LME models. The test for its significance yielded a formal test of significance of the relationship between the number of sessions provided and caregiver health outcomes at weeks 5 and 11.
Moderation of intervention effects by caregiver and patient characteristics (age, sex, race, ethnicity, relationship to the patient, employment, and comorbidities) relative to caregiver health outcomes at weeks 5 and 11 was explored by including group by potential moderator interaction terms (one at a time) in the LME model, which also included the baseline value of the caregiver health outcome, time (week 5 or 11), potential moderator, and study group.
Sample Size and Power Considerations
The sample size considerations for the trial were based on patient outcomes. For this secondary analysis of the caregiver sample, using the analytic strategy described previously, longitudinal comparisons were performed for 70 caregivers in the reflexology group and 67 caregivers in the control group who completed at least one interview after baseline. With correlation of 0.6 between pairs of repeated measures of caregiver outcomes, differences between groups corresponding to 0.39 of the adjusted standard deviation or greater were detectable as statistically significant with power of 0.8 or greater in two-sided tests at 0.05 level of significance.
[[{"type":"media","view_mode":"media_original","fid":"34931","attributes":{"alt":"","class":"media-image","height":"789","typeof":"foaf:Image","width":"371"}}]]
Results
A total of 256 caregivers of eligible women with breast cancer consented to participate in the parent study. All 256 caregivers were randomized to either reflexology or control groups in the parent trial; of the 256, 180 (70%) agreed to provide data about their own health outcomes and were included in this secondary analysis (see Figure 2). No differences existed between the reflexology and control group caregivers at baseline with regard to demographic characteristics (see Table 1) or caregiver outcome variables (see Table 2). No differences were found in attrition by study group (data not shown).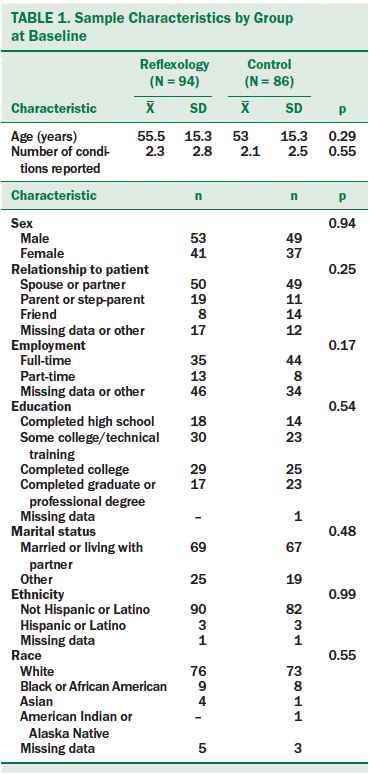
Baseline Characteristics of Caregivers
More male than female caregivers were in this sample (56%); this is attributed directly to the exclusive patient diagnosis of breast cancer and the majority of caregivers being spouses or partners. The average age of caregivers was 54 years; most were employed at least part-time and had some college education. The sample was comprised primarily of White, non-Hispanic/non-Latino caregivers, consistent with the demographic makeup of the geographic locations served by the participating oncology clinics in the midwestern United States.
[[{"type":"media","view_mode":"media_original","fid":"34936","attributes":{"alt":"","class":"media-image","height":"513","typeof":"foaf:Image","width":"371"}}]]
Caregiver Outcomes at Weeks 5 and 11 by Group
The LS means of caregiver health outcomes and their standard errors (SEs) for the reflexology and control groups at weeks 5 and 11 are presented in Table 3. Lower LS mean values at each time point represent the presence of less of the construct (outcome). For example, improvement in fatigue was reflected by a significantly lower LS mean for reflexology caregivers compared to controls at weeks 5 (p = 0.02) and 11 (p = 0.05). No differences were noted between groups at week 5 or 11 on anxiety, depression, pain severity, physical function, sleep disturbance, satisfaction with participation in social roles, or pain interference.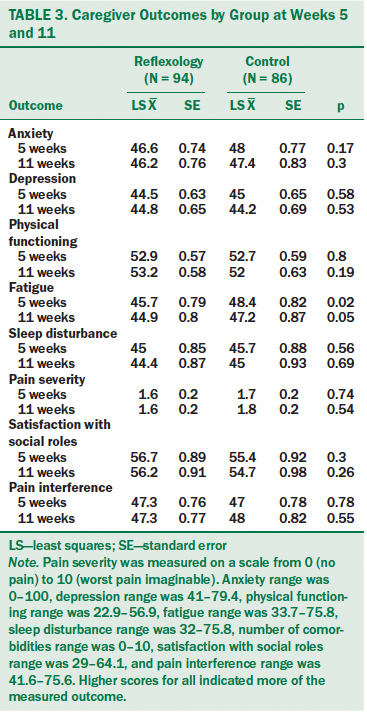
Association of Increasing Number of Sessions Delivered on Caregiver Outcomes
For this analysis, the association between the increasing number of reflexology sessions delivered and caregiver outcomes is reported as a model coefficient (see Table 4). Negative model coefficients indicate negative associations; a larger number of sessions was associated with less negative impact on physical, psychological, and social outcomes. This was true for all outcomes except pain severity. For example, fatigue was reported at lower levels as caregivers provided more sessions. However, the strength of this association did not reach statistical significance (p = 0.09). 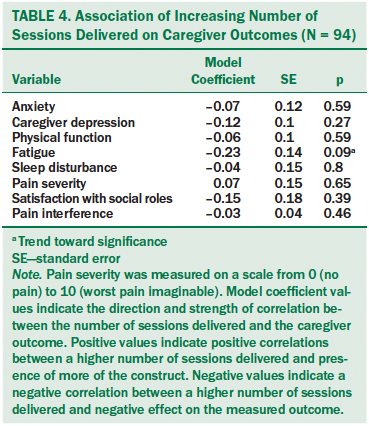
Moderation of the Effect of Reflexology Delivery on Caregiver Health Outcomes
Findings suggested the possibility that the sex of the caregiver may moderate the effect of reflexology delivery on physical functioning. In the reflexology group, female caregivers had better physical functioning than male caregivers, with time-averaged LS means of 53.97 (SE = 0.71) versus 52.28 (SE = 0.63), respectively (p = 0.07). Such difference did not exist among the caregivers in the control group.
The patient–caregiver relationship potentially modified the effects of reflexology delivery on caregiver depressive symptoms. Differences existed between the reflexology and control group caregivers regarding relationship to the patient and mean depression scores. Caregivers who were friends of the women with breast cancer reported lower levels of depressive symptoms in the reflexology group as compared to the control group with time-averaged LS means of 42.97 (SE = 2.05) versus 46.84 (SE = 1.51), respectively (p = 0.06).
Caregiver comorbidity is another potential moderator, as indicated by an interaction between study group and number of comorbid conditions (F[1,135] = 3.03, p = 0.08). In the control group, the number of comorbid conditions was negatively associated with the satisfaction of participation in social roles (slope = –0.72, SE = 0.0); in other words, higher numbers of comorbid conditions were associated with lower satisfaction in social roles. Conversely, in the reflexology group, the slope did not indicate a negative effect between higher number of comorbidities and lower satisfaction with participation in social roles (slope = 0.05, SE = 0.48).
Discussion
Caregivers provide vital support to patients with advanced breast cancer undergoing treatment, a trend that has grown as more patients receive most of their care in the home environment. It is imperative that caregivers’ health outcomes are examined in relation to providing symptom management for the patient at home. Such evaluation can potentially promote sustainability of caregiving activities and can lead to a better understanding of informal caregiver quality-of-life issues.
This study specifically expands the knowledge that evaluates the vulnerability of caregivers of people with cancer and the influence of intervention delivery on important outcomes, such as fatigue. The findings showed that fatigue was lower for the reflexology caregivers as compared to the caregivers in the control group. In contrast, other research has shown that the fatigue levels of caregivers of people with cancer increased over time (Almutairi, Alodhayani, Alonazi, & Vinluan, 2017; Badger et al., 2011; Kim, Spillers, & Hall, 2012), but the specific types and extent of care activities performed by caregivers were not reported. Although further research is needed, the benefits found in the current study for delivery of a specific intervention, such as reflexology, may hold promise for reducing caregiver fatigue.
An additional finding associated with fatigue was that caregivers who delivered more sessions of reflexology demonstrated a trend toward lower levels of several symptoms, including fatigue. Because of this trend in outcomes, more investigation is warranted regarding the types and intensity of supportive symptom management interventions encouraged for caregivers.
Although the potential moderator analyses were exploratory and findings could be because of chance, examination of the associations between caregiver outcomes and patient and caregiver characteristics provides insights that warrant further consideration. In terms of psychological outcomes, friends who provided reflexology compared to friends in the control group reported a trend toward lower levels of depressive symptoms. This finding potentially underscores the importance of friendship relationships as a factor in explaining caregiver psychological health, which is a new contribution to caregiver literature. The majority of the available literature focuses on familial relationships. Even leaders in the field of caregiving, such as Northouse, Katapodi, Schafenacker, and Weiss (2012), have investigated the psychological responses of family caregivers only, finding that a reciprocal relationship existed between the patient and caregiver’s distress. In addition, Kim, Baker, and Spillers (2007) found that adult daughters caring for a parent with cancer experienced the highest levels of caregiving stress. This response has been attributed to the large proportion of caregivers being daughters and emotional sharing of response to the patient’s disease (Kim et al., 2008). In light of the current study findings that friends may be less susceptible to depressive symptoms, clinicians may want to include friends as an option to partner with patients. This broad view of caregiving has the potential for reducing the burden on family while widening the support system.
In the reflexology group, female caregivers reported better physical functioning than men, indicating that the additional task of delivering reflexology did not adversely affect women. Although recent literature has included consideration of caregivers’ physical outcomes, differentiation between men and women was not reported (Boele et al., 2013; Chih et al., 2013). There may be potential gender issues that affect the experience of physical function decrements between male and female caregivers. Male caregivers may need extra support in this regard.
When examining the impact on social support, the number of comorbid conditions did not negatively affect caregiver satisfaction with participation in social roles. Caregiver outcomes linked to social health have been noted in other studies (Badger et al., 2011; Boele et al., 2013; Northouse et al., 2013), but those studies have not found relationships to the presence of comorbid conditions.
Limitations
The results of this study are generalizable only to caregivers of women with advanced breast cancer who satisfy the inclusion criteria. Although efforts to obtain a diverse sample of caregivers were made, the diversity of the sample was limited to the populations served by the participating sites. The lowered representation of minority and less educated participants is a limitation. The communication between caregivers and patient dyads beyond the delivery of reflexology in the intervention group was not measured and neither was the number of non-reflexology session contacts between caregivers and patients in the reflexology group. Although randomization equalizes the influences of other factors, this information could be useful in assessing future caregiver outcomes.
Implications for Practice and Research
Nurses have optimal opportunities to assist people with cancer and identify caregivers to support them during treatment and recovery. The findings that providing reflexology does not increase negative outcomes for informal caregivers and might contribute to reduced fatigue allows clinicians to confidently recommend looking beyond family members who are most often identified as caregivers. In addition, considering potential informal caregivers beyond immediate family members provides a larger pool of resources and potentially better likelihood of identifying vital support for the patient with cancer.
Although this research has provided insight regarding reflexology for symptom management, the findings further suggest the potential for caregivers to provide a variety of symptom management interventions. The question becomes the following: “What other interventions may prove beneficial when delivered by a caregiver?” Future research can address this. Consistently rigorous methods, as outlined for reflexology, provide a template for validation of other interventions delivered to patients with cancer by caregivers.
Conclusion
Further research examining associations between performing specific care activities is warranted to determine if the findings of the study are applicable to other interventions. The findings of this study suggest that caregivers who provide reflexology for a patient with advanced breast cancer may experience health benefits (e.g., less fatigue), fewer symptoms with intensity of reflexology participation, better psychological health for caregivers in friend–patient dyads, and better physical functioning for female caregivers. In addition, the number of comorbid conditions did not adversely affect caregiver social health outcomes for those providing reflexology. Through their meaningful involvement in patients’ symptom management, caregivers also have the potential for enhanced outcomes.
About the Author(s)
Frambes is an assistant professor in the Department of Nursing at Calvin College in Grand Rapids, MI; Sikorskii is a professor in the College of Nursing at the University of Arizona in Tuscon; and Tesnjak is a graduate of the Department of Statistics and Probability, and Wyatt is a professor, Lehto is an associate professor, and Given is a distinguished professor, all in the College of Nursing, all at Michigan State University in East Lansing. This research was funded by a grant (1R01 CA 157459-01) from the National Institutes of Health/National Cancer Institute and Michigan State University Graduate Research Fellowships. Frambes, Sikorskii, Wyatt, Lehto, and Given contributed to the conceptualization and design. Frambes, Sikorskii, and Wyatt completed the data collection. Frambes, Sikorskii, and Tesnjak provided statistical support. Frambes, Sikorskii, Tesnjak, and Given provided the analysis. Frambes, Sikorskii, Wyatt, and Lehto contributed to the manuscript preparation. Frambes can be reached at dawn.frambes@calvin.edu, with copy to editor at ONFEditor@ons.org. Submitted January 2017. Accepted for publication March 16, 2017.
References
Almutairi, K.M., Alodhayani, A.A., Alonazi, W.B., & Vinluan, J.M. (2017). Assessment of health-related quality of life among caregivers of patients with cancer diagnosis: A cross-sectional study in Saudi Arabia. Journal of Religion and Health, 56, 226–237. doi:10.1007/s10943-016-0261-4
American Cancer Society. (2017). What a cancer caregiver does. Retrieved from https://www.cancer.org/treatment/caregivers/what-a-caregiver-does.html
American Institutes for Research. (2016). Calibration studies testing. Retrieved from http://www.nihpromis.com/measures/CalibrationStudiesTesting
Applebaum, A.J., Farran, C.J., Marziliano, A.M., Pasternak, A.R., & Breitbart, W. (2014). Preliminary study of themes of meaning and psychological service use among informal cancer caregivers. Palliative and Supportive Care, 12, 139–148. doi:10.1017/S1478951513000084
Badger, T.A., Segrin, C., Figueredo, A.J., Harrington, J., Sheppard, K., Passalacqua, S., . . . Bishop, M. (2011). Psychosocial interventions to improve quality of life in prostate cancer survivors and their intimate or family partners. Quality of Life Research, 20, 833–844. doi:10.1007/s11136-010-9822-2
Baron, R.M., & Kenny, D.A. (1986). The moderator-mediator variable distinction in social psychological research: Conceptual, strategic, and statistical considerations. Journal of Personality and Social Psychology, 51, 1173–1182.
Bayliss, E.A., Ellis, J.L., & Steiner, J.F. (2009). Seniors’ self-reported multimorbidity captured biopsychosocial factors not incorporated into two other data-based morbidity measures. Journal of Clinical Epidemiology, 62, 550–557. doi:10.1016/j.jclinepi.2008.05.002
Bevans, M., & Sternberg, E.M. (2012). Caregiving burden, stress, and health effects among family caregivers of adult cancer patients. JAMA, 307, 398–403. doi:10.1001/jama.2012.29
Boele, F.W., Hoeben, W., Hilverda, K., Lenting, J., Calis, A.L., Sizoo, E.M., . . . Klein, M. (2013). Enhancing quality of life and mastery of informal caregivers of high-grade glioma patients: A randomized controlled trial. Journal of Neuro-Oncology, 111, 303–311. doi:10.1007/s11060-012-1012-3
Bradley, S.E., Sherwood, P.R., Kuo, J., Kammerer, C.M., Gettig, E.A., Ren, D., . . . Given, B. (2009). Perceptions of economic hardship and emotional health in a pilot sample of family caregivers. Journal of Neuro-Oncology, 93, 333–342. doi:10.1007/s11060-008-9778-z
Chih, M.Y., DuBenske, L.L., Hawkins, R.P., Brown, R.L., Dinauer, S.K., Cleary, J.F., & Gustafson, D.H. (2013). Communicating advanced cancer patients’ symptoms via the internet: A pooled analysis of two randomized trials examining caregiver preparedness, physical burden and negative mood. Palliative Medicine, 27, 533–543. doi:10.1177/0269216312457213
Corà, A., Partinico, M., Munafò, M., & Palomba, D. (2012). Health risk factors in caregivers of terminal cancer patients: A pilot study. Cancer Nursing, 35, 38–47. doi:10.1097/NCC.0b013e31820d0c23
Frambes, D., Given, B., Lehto, R., Sikorskii, A., & Wyatt, G. (2017). Informal caregivers of cancer patients: Review of interventions, care activities, and outcomes. Western Journal of Nursing Research. Advanced online publication. doi:10.1177/0193945917699364
Girgis, A., Lambert, S.D., McElduff, P., Bonevski, B., Lecathelinais, C., Boyes, A., & Stacey, F. (2013). Some things change, some things stay the same: A longitudinal analysis of cancer caregivers’ unmet supportive care needs. Psycho-Oncology, 22, 1557–1564. doi:10.1002/pon.3166
Given, B.A., Given, C.W., & Sherwood, P. (2012). The challenge of quality cancer care for family caregivers. Seminars in Oncology Nursing, 28, 205–212. doi:10.1016/j.soncn.2012.09.002
Home-Based Symptom Management Via Reflexology for Breast Cancer Patients. (2011–2016). Retrieved from https://clinicaltrials.gov/ct2
Hopkinson, J.B., Brown, J.C., Okamoto, I., & Addington-Hall, J.M. (2012). The effectiveness of patient-family carer (couple) intervention for the management of symptoms and other health-related problems in people affected by cancer: A systematic literature search and narrative review. Journal of Pain and Symptom Management, 43, 111–142. doi:10.1016/j.jpainsymman.2011.03.013
Kim, Y., Baker, F., & Spillers, R.L. (2007). Cancer caregivers’ quality of life: Effects of gender, relationship, and appraisal. Journal of Pain and Symptom Management, 34, 294–304. doi:10.1016/j.jpainsymman.2006.11.012
Kim, Y., Spillers, R.L., & Hall, D.L. (2012). Quality of life of family caregivers 5 years after a relative’s cancer diagnosis: Follow-up of the national quality of life survey for caregivers. Psycho-Oncology, 21, 273–281. doi:10.1002/pon.1888
Lambert, S.D., Girgis, A., Lecathelinais, C., & Stacey, F. (2013). Walking a mile in their shoes: Anxiety and depression among partners and caregivers of cancer survivors at 6 and 12 months post-diagnosis. Supportive Care in Cancer, 21, 75–85. doi:10.1007/s00520-012-1495-7
Litzelman, K., Green, P.A., & Yabroff, K.R. (2016). Cancer and quality of life in spousal dyads: Spillover in couples with and without cancer-related health problems. Support Care in Cancer, 24, 763–771. doi:10.1007/s00520-015-2840-4
National Alliance for Caregiving. (2016). Cancer caregiving in the U.S.: An intense, episodic, and challenging care experience. Retrieved from http://www.caregiving.org/wp-content/uploads/2016/06/CancerCaregivingRe…
National Cancer Institute. (2016). Topics in integrative, alternative, and complementary therapies (PDQ®)—Health professionals version. Retrieved from https://www.cancer.gov/about-cancer/treatment/cam/hp/cam-topics-pdq
Northouse, L.L., Katapodi, M.C., Schafenacker, A.M., & Weiss, D. (2012). The impact of caregiving on the psychological well-being of family caregivers and cancer patients. Seminars in Oncology Nursing, 28, 236–245. doi:10.1016/j.soncn.2012.09.006
Northouse, L.L., Mood, D.W., Schafenacker, A., Kalemkerian, G., Zalupski, M., LoRusso, P., . . . Kershaw, T. (2013). Randomized clinical trial of a brief and extensive dyadic intervention for advanced cancer patients and their family caregivers. Psycho-Oncology, 22, 555–563. doi:10.1002/pon.3036
Patient-Reported Outcomes Measurement Information System. (2016). PROMIS®. Retrieved from http://www.healthmeasures.net/explore-measurement-systems/promis
Reinhard, S., Given, B., Petlick, N., & Bemis, A. (2008). Supporting family caregivers in providing care. In R. Hughes (Ed.), Patient safety and quality: An evidence-based handbook for nurses (pp. 1–64). Rockville, MD: Agency for Healthcare Research and Quality.
Stenberg, U., Ruland, C.M., & Miaskowski, C. (2010). Review of the literature on the effects of caring for a patient with cancer. Psycho-Oncology, 19, 1013–1025. doi:10.1002/pon.1670
Van Houtven, C., Voils, C.I., & Weinberger, M. (2011). An organizing framework for informal caregiver interventions: Detailing caregiving activities and caregiver and care recipient outcomes to optimize evaluation efforts. BMC Geriatrics, 11, 77. doi:10.1186/1471-2318-11-77
Weiss, D.M., Northouse, L.L., Duffy, S.A., Ingersoll-Dayton, B., Katapodi, M.C., & LoRusso, P.M. (2016). Qualitative analysis of the experience of mental fatigue of family caregivers of patients with cancer in phase I trials [Online exclusive]. Oncology Nursing Forum, 43, E153–E160. doi:10.1188/16.ONF.E153-E160
Wyatt, G., Sikorskii, A., Rahbar, M.H., Victorson, D., & You, M. (2012). Health-related quality-of-life outcomes: A reflexology trial with patients with advanced-stage breast cancer. Oncology Nursing Forum, 39, 568–577. doi:10.1188/12.ONF.568-577
Wyatt, G., Sikorskii, A., Tesnjak, I., Frambes, D., Holmstrom, A., Luo, Z., . . . Tamkus, D. (2016). Caregiver-delivered reflexology for symptom management during breast cancer treatment. Manuscript in preparation.

