Interprofessional Perspectives on Providing Spiritual Care for Patients With Lung Cancer in Outpatient Settings
Purpose: To explore palliative care and oncology clinicians’ perspectives on current challenges and facilitating factors in meeting the spiritual needs of patients with lung cancer and family caregivers. This study was conducted in preparation for a community-based lung cancer palliative care intervention.
Participants & Setting: 19 oncology and palliative care clinicians in three outpatient Kaiser Permanente sites in southern California.
Methodologic Approach: This multisite qualitative study used focus group and key informant interviews. Data were analyzed using content analysis methodology, and a team approach was used to validate findings.
Findings: Clinicians described facilitating factors (interprofessional team support, assessment of spiritual needs, clinician-provided spiritual support, and provision of culturally respectful spiritual care) and challenges (related to providing culturally respectful spiritual care by respecting the patients’ spiritual and cultural beliefs in an open way and in advocating for the patients’ wishes) they encountered when addressing patient and caregiver spiritual needs.
Implications for Nursing: This study demonstrated the need to provide nurses with practical tools, education, and a supportive environment to address patients’ and family caregivers’ spiritual concerns.
Jump to a section
Spirituality plays an important role in the lives of patients with cancer. Oncology nurses concerned with the whole person play a crucial role in supporting spiritual well-being in patients and families (Musgrave & McFarlane, 2003). However, in outpatient oncology settings, a clinical assessment of spirituality is generally limited to a single question on religious preference (Skalla & Ferrell, 2015). Consequently, underlying spiritual needs are often overlooked despite the patients’ wish to have their spiritual needs addressed in the context of their illness experience (McCord et al., 2004; Phelps et al., 2012).
Spiritual care is not solely the responsibility of one healthcare discipline. Rather, research has recommended an interprofessional approach that includes taking a spiritual history and knowing when to make appropriate referrals to chaplains and others trained in providing spiritual care (Puchalski et al., 2009). This study identified facilitating factors and challenges of providing spiritual support to patients and family caregivers in outpatient settings. This qualitative study is part of a larger ongoing two-phase intervention study conducted to test the dissemination of a palliative care intervention (PCI) for patients with non-small cell lung cancer and their primary family caregivers in community-based settings. Three outpatient Kaiser Permanente sites in southern California were chosen for the dissemination of the PCI because of their substantial commitment to supporting palliative care services and bridging outpatient services to the community (Nguyen et al., 2017).
Background
The International Consensus Conference in 2012 defined spirituality as “a dynamic and intrinsic aspect of humanity through which persons seek ultimate meaning, purpose, and transcendence, and experience relationship to self, family, others, community, society, nature, and the significant or sacred. Spirituality is expressed through beliefs, values, traditions, and practices” (Puchalski, Vitillo, Hull, & Reller, 2014, p. 646).
Suffering related to serious illness, such as cancer, often leads people to search for deeper meaning in their lives. Finding meaning in life is critical to effective coping, but the isolation and suffering associated with an illness can make this particularly difficult. Effective coping, including spiritual coping, can bring healing and restoration of wholeness (Puchalski et al., 2009). Examples of spiritual coping include praying, seeking comfort from faith, and obtaining support from members of a church (Abernethy, Chang, Seidlitz, Evinger, & Duberstein, 2002).
When spiritual concerns are not addressed, the patient or family caregiver may experience higher levels of distress and feelings of hopelessness. Spiritual distress, also known as spiritual suffering, may occur in situations where religious beliefs and practices fail to provide meaning or have a negative meaning, such as feelings of abandonment by God (Peteet & Balboni, 2013) or when a person’s illness experience contradicts his or her core beliefs (Bartel, 2004). In a systematic review of unmet supportive care needs of patients with lung cancer, Maguire et al. (2013) identified unmet spiritual needs as an area of major patient suffering. The inability to find meaning and purpose in life and concerns about the ability to maintain a positive outlook and reprioritize the remaining time were common experiences. Patients have noted the importance of God (or fate) in experiencing illnesses, attributing illnesses as being in line with God’s will. Underscoring their spiritual needs, patients also described a process of oscillating between hope and despair (Maguire et al., 2013).
In situations of spiritual distress, an in-depth spiritual assessment by a chaplain or person with advanced training in spiritual care may be warranted. This assessment can inform the healthcare team about coping strategies that may be helpful to a patient (Balboni et al., 2018). To first identify spiritual needs and/or spiritual distress, clinicians should take a spiritual history or employ screening tools. Typically, a spiritual assessment is conducted within an initial comprehensive evaluation in which, along with other assessments, a spiritual history is taken. This approach uses a sequence of targeted questions that capture a patient’s spiritual characteristics, resources, and needs (Steinhauser et al., 2017). Several standardized spiritual history tools have been documented as clinically useful in asking questions that facilitate spiritual conversations. Examples of spiritual history tools used in cancer care include the validated FICA Spiritual History Tool (Borneman, Ferrell, Otis-Green, Baird, & Puchalski, 2010; Puchalski & Romer, 2000), the SPIRIT model (Anandarajah & Hight, 2001), and the HOPE model (Frick, Riedner, Fegg, Hauf, & Borasio, 2006). Despite a number of tools, scant evidence shows clinicians using them, particularly in the outpatient setting, where spiritual care is rarely offered. Across settings, barriers to nurse-provided spiritual care have been well documented. Factors such as insufficient time (Abbas & Dein, 2011; Skalla & Ferrell, 2015), the challenge of lack of patient privacy to ask in-depth questions (Ronaldson, Hayes, Aggar, Green, & Carey, 2012), and lack of resources and training in spiritual conversations (Wittenberg, Ferrell, Goldsmith, & Buller, 2016) are often cited.
There is a gap in the current evidence base on how palliative care and oncology clinicians in outpatient settings address the spiritual concerns of patients with cancer and their family caregivers. The purpose of this study was to describe palliative care and oncology clinicians’ (in the areas of nursing, medicine, social work, and chaplaincy) perspectives on the challenges and facilitating factors in meeting the spiritual needs of patients with lung cancer and their family caregivers.
Theoretical Framework
The Reach Effectiveness Adoption Implementation Maintenance (RE-AIM) model was used for the PCI study and the current qualitative study (Glasgow, Vogt, & Boles, 1999). This conceptual framework was used to evaluate the effectiveness of translating intervention research into practice. To contribute to the successful implementation and dissemination of the PCI, the third dimension of RE-AIM, adoption, was used to guide this qualitative study. Adoption is further defined as how feasible it is for the program to be adopted in real-world settings and whether it can be adopted in low-resource settings. Assessing the facilitating factors and challenges within the organization before implementation can help gauge needs and ensure buy-in of the intervention (Demiris, Parker Oliver, Capurro, & Wittenberg-Lyles, 2013).
Methods
This study was conducted in preparation for implementing a nurse-led lung cancer PCI in community practice. The three components of the intervention included (a) attention to the patients’ and family caregivers’ quality-of-life dimensions (physical, psychological, social, and spiritual), (b) support for interprofessional team input in the plan of care, and (c) patient and caregiver education (Ferrell et al., 2015; Nguyen et al., 2017). This article focuses on the perceived factors that facilitate and challenge oncology and palliative care clinicians in their efforts to address patients’ and family caregivers’ spiritual needs. The overall qualitative study and methods have been reported elsewhere (Siler, Mamier, & Winslow, 2018).
This was a multisite qualitative study that used focus group and key informant phone interviews with oncology and palliative care clinicians. Focus group discussions were selected as the primary method of choice to capture interprofessional perspectives and enhance collaboration. Key informant telephone interviews were used as an alternative for clinicians who were unable to attend focus groups. Ethical approval was obtained from the institutional review board from Kaiser of southern California-Riverside, Fontana, and Anaheim, and deferred approval was obtained from Loma Linda University.
Setting and Participants
A purposive sample of participants represented a range of disciplines, including nurses, physicians, social workers, chaplains, and nurse administrators at three outpatient Kaiser Permanente sites in southern California. These sites provide outpatient palliative care and oncology services and were selected for the PCI study.
Eligible participants were employed at one of the three selected facilities, licensed in their profession, and had provided care for patients with lung cancer. Clinicians were contacted through their organization’s email system by the principal investigator of the PCI study. The email document described the purpose of the study and that participation was voluntary. Participants were asked to email or call the primary researcher of this study if they were interested in participating. Recruitment for individual telephone interviews was conducted after the completion of the three focus groups to invite clinicians who were unable to attend focus groups. As an alternative to written consent, an information sheet was distributed to participants. Content included the purpose and procedures of the study and information regarding confidentiality.
Data Collection
Focus group sessions with clinicians were held in a private, comfortable room at each designated facility and lasted about one hour. During the interview, discussion was generated with open-ended questions. First, the interviewer asked two questions: “What are the strengths of your palliative care team in meeting the quality-of-life (physical, social, psychological, and spiritual) needs of patients with lung cancer and family caregivers?” and “What are the challenges in meeting patient and family caregiver quality-of-life needs?” Participants provided handwritten responses to these questions. A focus group guide was used to further lead the discussion. To adapt the PCI to the cultural aspects of care, the authors explored cultural needs and included them in the analysis of spiritual needs. Table 1 describes the questions and guidelines used in the focus group and key informant interviews.
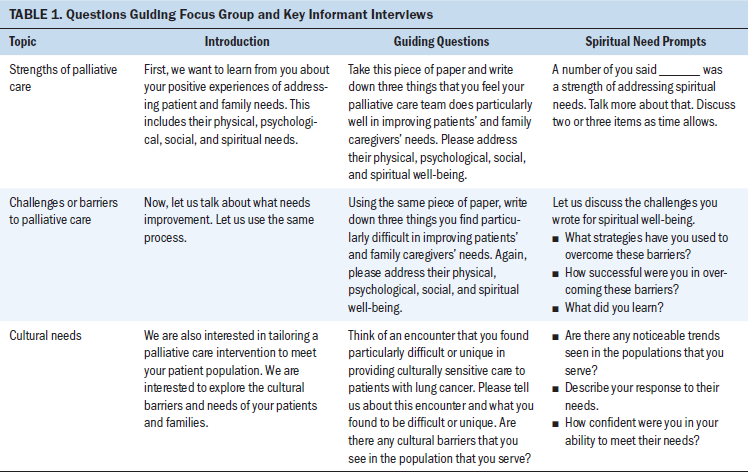
A team approach was used during each focus group session. The primary researcher of the study and a nurse researcher involved in the PCI facilitated discussion. A research associate designated to the PCI study assumed the role of notetaker and kept track of identifying information and notable quotes. In addition, at least one of the two principal investigators involved in the PCI study was present at each group session. At the completion of all three focus groups, the primary researcher conducted key informant telephone interviews with participants who were unable to attend group sessions. The same open-ended questions and interview guide was used. All focus group and phone interviews were audio recorded and transcribed verbatim.
Rigor
In this study, credibility was established by following distinct descriptions of conventional content analysis. Prolonged engagement with nurses participating in the study post–data collection helped ensure that the data accurately represented study participants. This was completed through telephone meetings with the research team and palliative care nurses in preparation to launch the intervention phase at each site. During these calls, the research team documented the challenges and successes of meeting quality-of-life needs, recruiting participants at each PCI site, and validating the needs of clinicians in successfully adopting the intervention. This study’s dependability was established through careful documentation of findings and decision making with multiple researchers. Confirmation of findings was conducted during the analysis phase using the methods of conventional content analysis of review, feedback, validation, and revision (Hsieh & Shannon, 2005). Confirmability of this research was established by the presence of at least two nurse researchers at each focus group, eliciting the insights of those who heard the perspectives of the clinicians firsthand. Debriefing after each focus group played a major role in maintaining rigor within the data collection phase of this study. The multisite, interprofessional design of this study, along with the team-based approach used for validating analysis results, ensured objectivity of findings and a broader perspective of possible transferability to other sites and populations.
Data Analysis
Focus group and key informant interviews were analyzed in the same manner. Initial analysis of transcripts was conducted manually and then organized using MAXQDA, a computer-based qualitative analysis program. Principles of conventional content analysis (Hsieh & Shannon, 2005) were used to guide qualitative analysis. The primary researcher of this study conducted analysis of data. Codes, categories, subcategories, and text exemplars were examined for feedback and validation with the PCI team, which consisted of two principal investigators and one nurse researcher. Validation occurred at three stages of the analysis process: after code selections, at the selection of text exemplars and definitions, and at the final analysis. The research team achieved consensus that data saturation was met after the five key informant interviews were conducted and analyzed. No new aspects were noted in these interviews when compared to the focus group findings.
Results
A diverse sample of 19 experienced palliative care and oncology clinicians representing nursing, medicine, social work, and chaplaincy participated in this study. In three focus group interviews, clinicians discussed interprofessional perspectives on meeting patients’ and family caregivers’ spiritual needs in the context of palliative care and the experience of lung cancer. Table 2 provides demographic characteristics of the sample.
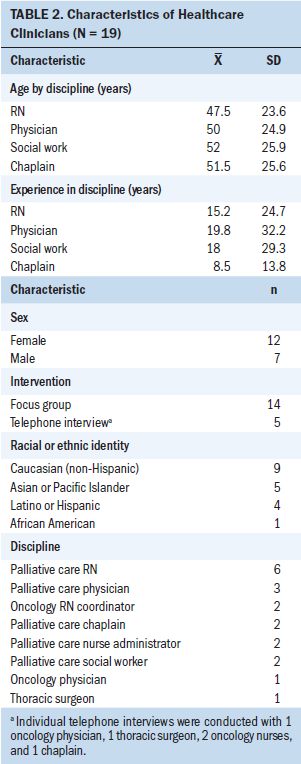
Fundamentally, all clinicians reported encountering spirituality in the context of caring for patients and their family caregivers. Specifically, they witnessed patients in distress and suffering, which evoked the understanding that the spiritual dimension surfaces in caring for these patients. As one physician said, “You used the term suffering, and I think that probably captures better the spiritual dimension of the illness.” The analysis of the interviews focused on clinicians’ strengths and challenges in addressing patient and family caregiver spiritual needs in the context of palliative care for patients with lung cancer and resulted in two categories: factors that facilitate addressing spiritual needs and challenges in providing culturally respectful care.
Factors That Facilitate Addressing Spiritual Needs
Four subcategories were identified as factors that facilitate addressing patient and family caregiver spiritual needs: interprofessional team support, assessment of spiritual needs, clinician-provided spiritual support, and provision of culturally respectful spiritual care.
Interprofessional team support: Interprofessional team support was defined as addressing spiritual needs through the assistance of a member of the interprofessional team, such as a chaplain, social worker, or nurse. Participants were most often referred to a social worker or chaplain for spiritual support, particularly when the clinician was not comfortable with addressing the spiritual dimension or felt it was outside of his or her scope of practice. One nurse shared, “With pressing psychological issues or spiritual, I refer them to the social worker because I’m not comfortable talking to them about spiritual and religious issues.” Likewise, an oncologist stated, “I don’t ask them directly what is your faith and spirituality, but my case manager, social worker, and the charge nurse [do].” Chaplains were not official members of the palliative care interprofessional teams at the three sites. However, staff at one location explained that they were fortunate to have a chaplain who extended services to their outpatient clinic. At that site, a palliative care nurse made the following statement: “Our chaplains are unofficially part of the group. When we see patients and families, [the chaplain] really knows what questions to pinpoint and ask.” This chaplain was also present in one focus group session with a palliative care team and favored an interprofessional team approach in which the chaplain helped address spiritual issues. Researchers observed that the spiritual needs of the patients and family were consistently relegated to the chaplain. In contrast, clinicians stressed difficulties in addressing spirituality in the absence of a chaplain—an organizational challenge at two of the sites: “It would be great to have maybe a chaplain available because I think most of us share privately that we feel we’re limited because we don’t have the proper training to maybe address it.”
Assessment of spiritual needs: Although clinicians generally referred patients to a member of the interprofessional team, some clinicians were aware of formal spiritual assessment tools to evaluate spiritual well-being; however, only one specific assessment tool was mentioned. This tool allowed for examining patients’ and family caregivers’ spiritual well-being. Clinicians explained that the social worker at each site conducted these more targeted psychosocial assessments for patients referred for social or psychological needs. Some clinicians have used their own wording of questions for inviting a dialogue on spirituality. Examples of these questions include “What helps you cope with all of this?” One of the nurses suggested that discussing the physical aspects of care first was helpful in staging dialogue around spirituality. “Ok, so we’ve addressed your understanding of your symptoms, now what helps you get through your day? . . . Some people say faith is important.”
Clinician-provided spiritual support: Clinicians provided spiritual support that was defined as interventions provided to spiritually support patients. More often, clinicians identified interventions other than prayer, such as being there and listening to the patient. Other interventions included meditation, music, and distraction of patients’ thoughts away from their illness, as described by one oncology nurse: “I encourage them to meditate or listen to music they like, just to get their heads out of the disease.”
Provision of culturally respectful spiritual care: In addition to assessing spiritual needs and providing spiritual interventions, clinicians incorporated cultural considerations in their interactions with patients and family caregivers. Clinicians described culturally spiritual care as “meeting spiritual needs in an open way and respecting the cultural beliefs of others.” Respecting the beliefs of patients and family caregivers provided space for patients to initiate a spiritual conversation. Building on an established relationship of trust, clinicians sought to listen to patients and work with their religious beliefs. Clinicians explained that they intentionally used language congruent with patients’ beliefs and their view of God or higher power. This approach helped them to interact with patients who had a different belief system than them. A social worker, for example, shared how she contextualized prayers by neutralizing language with patients from different religious backgrounds:
I have standard, neutral prayer phrases that I’ve used before that work really well with me and with families, even if it’s something that’s a religion outside of what I’m comfortable with. I make very neutral prayer statements.
Challenges in Providing Culturally Respectful Care
Challenges in meeting patient and family caregiver needs were related to barriers like meeting spiritual needs and providing culturally sensitive and ethical care. Challenges in providing culturally respectful care were categorized into two subcategories: providing culturally respectful spiritual care and advocating for the patient.
Providing culturally respectful spiritual care: Major concerns were expressed in addressing patient and family caregiver spiritual needs in an open, nonleading manner. Addressing spirituality was viewed as more difficult to address than physical needs. One nurse shared, “Even asking us to identify it is difficult. . . . We’re so often doing the physical.” Asking about spirituality, feeling uncomfortable with spiritual issues, and prioritizing spirituality in the plan of care were identified concerns. Clinicians did not know what questions to ask or whether asking questions about spirituality was appropriate within their clinical role. For example, a physician said, “I don’t know that I can actually ask people about their spirituality . . . in an unbiased fashion.” Although a few clinicians used questions to explore their patients’ spiritual needs, most felt that questions about spirituality beyond patients’ religious affiliations were a challenge. One nurse said, “It’s usually just seeing if they’re religiously affiliated, but not anything beyond that, which is already in their chart.” Many clinicians mentioned not being comfortable with spiritual issues. A nurse shared, “I think it’s just an area that we’re just not as comfortable with because we haven’t really been touching on that.” Challenges in addressing spirituality were also related to prioritizing spirituality into the plan of care. Clinicians explained that spirituality was often addressed last or not at all. One physician shared, “There is still so much other information to go over with the patient, there is not time to talk about spirituality.”
Advocating for the patient: Challenges in providing culturally respectful care included clinicians’ responsibility for advocating for the patient’s wishes while also assessing the cultural norms and dynamics of the patient’s family. Conflicts arose when the goals of clinicians and patients were not in agreement. This was expressed particularly in the areas of decision making and communication between the patient and family and between the family and clinician. This included the common tension between patients and families’ wishes. A nurse explained, “It triggers feelings within us, because we want to be the patient’s best advocate, and what does that look like?” Another nurse described the challenge of advocating for patients while also considering the dynamics of the family:
Even in the consult, in the outpatient setting, she deferred to the son, whatever the son wanted to do, you know, even though she was kind of leaning more toward no treatment. I try to encourage them to write it out [in] an advance directive.
Discussion
The findings provide insight into the perspectives of oncology and palliative care clinicians on providing spiritual care in outpatient settings. These perspectives can be used to guide future interventions to prepare clinicians in supporting the spiritual well-being of patients and family caregivers. Based on these findings, the authors offer some recommendations on how to better support and prepare clinicians for this role.
Interprofessional Team Approach
Spiritual assessment and spiritual care were not typically seen as part of the clinicians’ role; rather, they were considered to be under the purview of social workers or chaplains. Therefore, clinicians were not inclined to take on this role. Interprofessional team support could mitigate the problem of not addressing spirituality when a specialist, such as a chaplain or social worker, is part of the team. Conversely, the absence of a spiritually trained clinician likely leads to the neglect of spirituality. Abbas and Dein (2011) found that several clinicians chose not to have spiritual conversations with patients because they were aware of their limitations and were unsure of when to refer them to other members of the interprofessional team.
Quality palliative care in oncology practice is inclusive of spiritual care; therefore, a team approach is necessary. Spiritual care cannot be exclusively assigned to social workers or chaplains. However, these healthcare providers play key roles because they are often trained in in-depth spiritual assessments and interventions. For a successful team approach, clinicians need to be aware of spiritual issues, competently draw on short screening or spiritual assessment or history tools, and know when a referral is warranted (Puchalski et al., 2009).
Assessment of Spiritual Needs
This study sheds light on the scarce use of spiritual history and spiritual screening tools. As generalists, clinicians play a key role in referring patients to trained spiritual care experts. If clinicians do not know how to examine spiritual well-being, it is highly likely that spiritual needs will go undetected. In these cases, clinicians will not assess spirituality beyond asking for a patient’s religious preference. As a result, targeted education about the role of spirituality and religion in helping patients cope with illness may be useful, along with structured tools that are easy to use in the outpatient setting (Abbas & Dein, 2011; Skalla & Ferrell, 2015).
Provision of Culturally Respectful Spiritual Care
Providing culturally respectful spiritual care was one of the major needs discussed by clinicians and defined as meeting patients’ spiritual needs in an open way. Clinicians practiced this by inquiring about patients’ beliefs and not imposing their personal beliefs on them. Clinicians’ perspectives about their roles in meeting spiritual needs centered on a mutual understanding of cultural norms and respect for patients and families. This helped build trusting relationships among clinicians, patients, and caregivers. Carpenter and Berry (2016) said, “Having a respect for the patient and family members’ hopes and goals for what they want to achieve during the illness is essential” (p. 440). Conflicts may arise when the goals of clinicians and patients differ. Likewise, Mazanec and Panke (2016) warned that the “three most common sources of cultural conflict are between the patient and family, among the healthcare team members, and among the healthcare team patient and family” (p. 423). Culturally respectful spiritual care provides language for clarifying differences and what is important to patients and family caregivers.
In line with nurses’ roles in providing culturally respectful spiritual care, patient-centered cancer care requires culturally sensitive approaches to ensure patients’ well-being (Schrank et al., 2017), as well as respect for the patients’ and family members’ hopes and goals for what they want to achieve during their illness (Carpenter & Berry, 2016). Any endeavors to integrate spiritual care in outpatient settings fundamentally hinge on understanding and respecting the cultural perspectives and spiritual needs of patients and families.
Supportive Environment
Findings reflect the time constraints of a busy outpatient healthcare system but also the level of priority clinicians assign to addressing spiritual needs. Although nurse managers involved in this study welcomed education and were supportive of addressing spiritual needs, they had limited resources to draw on in terms of chaplains and social workers. Clinicians expressed doubts about having the time and privacy to address spirituality. As in the current study, Ronaldson et al. (2012) found insufficient time and lack of patient privacy to be common barriers for palliative care nurses and acute care nurses. To integrate spiritual tools and improve education, it is important to consider the clinical environments in which nurses work and whether these environments support the integration of spiritual care. The frequency of nurses providing spiritual care has been linked to employer support and whether nurses self-identified as spiritual and/or religious (Taylor, Gober-Park, et al., 2017). In a cross-sectional Australian study of outpatient palliative care and acute care nurses, palliative care nurses provided more spiritual care and had positive perspectives on spiritual care, which were associated with their spiritual caring (Ronaldson et al., 2012). In Israel, a study by Musgrave & McFarlane (2004) identified oncology and non-oncology nurses’ spiritual well-being as a predictor of their attitudes in spiritual care. In a comparison of nurse spiritual care in four U.S. studies, Taylor, Mamier, Ricci-Allegra, and Foith (2017) noticed a significant difference in the frequency of spiritual care between nurses working in a faith-based tertiary care health system versus an intensive care unit working in a secular health system. Likewise, Taylor, Gober-Park, et al. (2017), surveying Christian nurses around the United States, found a significant difference in the frequency of spiritual care practice depending on whether the employing hospital was faith-based or secular, the latter scoring lower in frequency of providing spiritual care. Specifically, nurse managers’ perceived support of spiritual care played a key role. Nurses who felt that their managers were supportive were more inclined to provide spiritual care than their counterparts. If spiritual care is a low administrative priority, clinicians likely will not receive education on how to assess spirituality and how to provide culturally sensitive spiritual care. Ill-prepared for this role, most will not reserve time to address the spiritual needs of patients and family caregivers.
Last, clinicians desired to include spiritual care specialists like chaplains in the plan of care and on the team. In fact, the only chaplain involved in a focus group was considered an unofficial member who extended services to the outpatient palliative care services. The organizational challenge of not having a chaplain on staff was discussed in the focus groups and individual telephone interviews. Organizations that desire to cultivate an environment that welcomes spiritual support for patients and family caregivers should incorporate chaplains and other spiritual care workers as official members of the interprofessional team. It is then more likely that clinicians will feel supported and view spiritual support as a significant aspect of quality care.
Limitations
A limitation to this study was the low representation of oncology clinicians in focus group interviews. Although clinicians who were not on a palliative care team were invited to participate in this study, oncology clinicians had a low response rate. For this reason, individual interviews with oncology nurses and physicians were added. When these did not yield new data, researchers concluded data saturation. In addition, because a chaplain was not directly involved with outpatient palliative care services at each site, only one chaplain participated in the focus groups. To get a more in-depth perspective of trained spiritual care workers, the authors recruited a chaplain involved with inpatient palliative care for an individual phone interview. This perspective was useful in exploring the practices and challenges of addressing the spiritual needs of patients with lung cancer and their family caregivers. The perspectives of social workers were absent at one site; however, the role and perspectives of the social workers at the two sites were robust and viewed as a good representation of this discipline in preparation for the PCI by the research team. The final sample size was representative of the total workforce involved in the PCI and sufficient to obtain data saturation. Future studies in other settings should explore to what degree the findings from this study are transferrable and if additional facilitators and challenges emerge.
Implications for Nursing
This study is unique because it translates the perspectives of clinicians involved in an ongoing PCI study and describes the challenges of integrating spiritual care into clinical practice. Team support is a vital resource, but for clinicians to take a more active role in communicating with patients and families about their spiritual needs in this environment, oncology nurses must possess the skills for taking a spiritual history or screening for spiritual issues. Future research should explore interventions for improving healthcare providers’ confidence in delivering culturally sensitive spiritual care.
A follow-up investigation with clinicians after the PCI implementation at each site may be helpful in recognizing the success and challenges of applying the components of the PCI. Specifically, the nurse-led PCI provided training for nurses and written education for the patient and family caregiver; this also provided nurses with a structured template for addressing the spiritual needs of patients and family caregivers. The identified spirituals needs were to be included in an interprofessional plan of care. Providing written education may be helpful in guiding nurses and other professionals through difficult conversations and the assessment of patients’ spiritual needs.

Conclusion
This study presented the opportunities and challenges of providing spiritual support in busy outpatient settings with limited access to professional spiritual care providers. To this end, targeted spiritual care education is needed for the interprofessional team to work together in support of patients and families. In addition, the organizational culture of the outpatient oncology setting must be consistent with this goal. Careful analysis of facilitating factors and challenges should be further explored in settings that desire to implement a comprehensive PCI that is inclusive of culturally sensitive spiritual care through a team of interprofessional clinicians.
The authors gratefully acknowledge Tami Borneman, RN, MSN, and Huong Nguyen, PhD, RN, for their contribution to the conceptualization and analysis.
About the Author(s)
Shaunna Siler, PhD, RN, is an assistant professor, Iris Mamier, PhD, MSN, RN, is an associate professor, and Betty W. Winslow, PhD, RN, is a professor emerita, all in the School of Nursing at Loma Linda University in California; and Betty R. Ferrell, PhD, RN, MA, FAAN, FPCN, CHPN, is a director and professor in the Division of Nursing Research and Education at the City of Hope Comprehensive Cancer Center in Duarte, CA. This research was funded by a National Institute of Nursing Research Diversity supplement award (3R01NR015341-02W1; principal investigator: Betty R. Ferrell). During the writing of this article, Winslow was supported by funding from the Robert Wood Johnson Foundation and has received additional support from the RAND Corporation. Siler, Mamier, and Ferrell completed the data collection and provided statistical support. All authors contributed to the conceptualization and design, provided the analysis, and contributed to the manuscript preparation. Siler can be reached at shaunna.siler@ucdenver.edu, with copy to ONFEditor@ons.org. (Submitted April 2018. Accepted July 3, 2018.)
References
Abbas, S.Q., & Dein, S. (2011). The difficulties assessing spiritual distress in palliative care patients: A qualitative study. Mental Health, Religion and Culture, 14, 341–352. https://doi.org/10.1080/13674671003716780
Abernethy, A.D., Chang, H.T., Seidlitz, L., Evinger, J.S., & Duberstein, P.R. (2002). Religious coping and depression among spouses of people with lung cancer. Psychosomatics, 43, 456–463. https://doi.org/10.1176/appi.psy.43.6.456
Anandarajah, G., & Hight, E. (2001). Spirituality and medical practice: Using the HOPE questions as a practical tool for spiritual assessment. American Family Physician, 63, 81–89.
Balboni, M.J., Sullivan, A., Smith, P.T., Zaidi, D., Mitchell, C., Tulsky, J.A., . . . Balboni, T.A. (2018). The views of clergy regarding ethical controversies in care at the end of life. Journal of Pain and Symptom Management, 55, 65–74. https://doi.org/10.1016/j.jpainsymman.2017.05.009
Bartel, M. (2004). What is spiritual? What is spiritual suffering? Journal of Pastoral Care and Counseling, 58, 187–201. https://doi.org/10.1177/154230500405800304
Borneman, T., Ferrell, B., Otis-Green, S., Baird, P., & Puchalski, C. (2010). Evaluation of the FICA spiritual assessment tool (501). Journal of Pain and Symptom Management, 39, 406–407. https://doi.org/10.1016/j.jpainsymman.2009.11.149
Carpenter, J., & Berry, P. (2016). Communication principles in spiritual care. In C. Dahlin, P.J. Coyne, & B.R. Ferrell (Eds.), Advanced practice in palliative nursing. New York, NY: Oxford University Press.
Demiris, G., Parker Oliver, D., Capurro, D., & Wittenberg-Lyles, E. (2013). Implementation science: Implications for intervention research in hospice and palliative care. Gerontologist, 54, 163–171. https://doi.org/10.1093/geront/gnt022
Ferrell, B., Sun, V., Hurria, A., Cristea, M., Raz, D.J., Kim, J.Y., . . . Koczywas, M. (2015). Interdisciplinary palliative care for patients with lung cancer. Journal of Pain and Symptom Management, 50, 758–767. https://doi.org/10.1016/j.jpainsymman.2015.07.005
Frick, E., Riedner, C., Fegg, M.J., Hauf, S., & Borasio, G.D. (2006). A clinical interview assessing cancer patients’ spiritual needs and preferences. European Journal of Cancer Care, 15, 238–243. https://doi.org/10.1111/j.1365-2354.2005.00646.x
Glasgow, R.E., Vogt, T.M., & Boles, S.M. (1999). Evaluating the public health impact of health promotion interventions: The RE-AIM framework. American Journal of Public Health, 89, 1322–1327.
Hsieh, H.F., & Shannon, S.E. (2005). Three approaches to qualitative content analysis. Qualitative Health Research, 15, 1277–1288. https://doi.org/10.1177%2F1049732305276687
Maguire, R., Papadopoulou, C., Kotronoulas, G., Simpson, M.F., Mcphelim, J., & Irvine, L. (2013). A systematic review of supportive care needs of people living with lung cancer. European Journal of Oncology Nursing, 17, 449–464.
Mazanec, P., & Panke, T. (2016). Culturally respectful palliative care. In C. Dahlin, P.J. Coyne, & B.R. Ferrell (Eds.), Advanced practice in palliative nursing. New York, NY: Oxford University Press.
McCord, G., Gilchrist, V.J., Grossman, S.D., King, B.D., McCormick, K.E., Oprandi, A.M., . . . Srivastava, M. (2004). Discussing spirituality with patients: A rational and ethical approach. Annals of Family Medicine, 2, 356–361.
Musgrave, C.F., & McFarlane, E.A. (2003). Oncology and nononcology nurses’ spiritual well-being and attitudes toward spiritual care: A literature review. Oncology Nursing Forum, 30, 523–527. https://doi.org/10.1188/03.ONF.523-527
Musgrave, C.F., & McFarlane, E.A. (2004). Intrinsic and extrinsic religiosity, spiritual well-being, and attitudes toward spiritual care: A comparison of Israeli Jewish oncology nurses’ scores. Oncology Nursing Forum, 31, 1179–1183. https://doi.org/ 10.1188/04.ONF.1179-1183
Nguyen, H.Q., Cuyegkeng, T., Phung, T.O., Jahn, K., Borneman, T., Macias, M., . . . Ferrell, B.R. (2017). Integration of a palliative care intervention into community practice for lung cancer: A study protocol and lessons learned with implementation. Journal of Palliative Medicine, 20, 1327–1337.
Peteet, J.R., & Balboni, M.J. (2013). Spirituality and religion in oncology. CA: A Cancer Journal for Clinicians, 63, 280–289. https://doi.org/10.3322/caac.21187
Phelps, A.C., Lauderdale, K.E., Alcorn, S., Dillinger, J., Balboni, M.T., Van Wert, M., . . . Balboni, T.A. (2012). Addressing spirituality within the care of patients at the end of life: Perspectives of patients with advanced cancer, oncologists, and oncology nurses. Journal of Clinical Oncology, 30, 2538–2544.
Puchalski, C., Ferrell, B., Virani, R., Otis-Green, S., Baird, P., Bull, J., . . . Sulmasy, D. (2009). Improving the quality of spiritual care as a dimension of palliative care: The report of the consensus conference. Journal of Palliative Medicine, 12, 885–904.
Puchalski, C., & Romer, A.L. (2000). Taking a spiritual history allows clinicians to understand patients more fully. Journal of Palliative Medicine, 3, 129–137. https://doi.org/10.1089/jpm.2000.3.129
Puchalski, C.M., Vitillo, R., Hull, S.K., & Reller, N. (2014). Improving the spiritual dimension of whole person care: Reaching national and international consensus. Journal of Palliative Medicine, 17, 642–656. https://doi.org/10.1089/jpm.2014.9427
Ronaldson, S., Hayes, L., Aggar, C., Green, J., & Carey, M. (2012). Spirituality and spiritual caring: Nurses’ perspectives and practice in palliative and acute care environments. Journal of Clinical Nursing, 21, 2126–2135.
Schrank, B., Rumpold, T., Amering, M., Masel, E.K., Watzke, H., & Schur, S. (2017). Pushing boundaries—culture-sensitive care in oncology and palliative care: A qualitative study. Psycho-Oncology, 26, 763–769. https://doi.org/10.1002/pon.4217
Siler, S., Mamier, I., & Winslow, B. (2018). The perceived facilitators and challenges of translating a lung cancer palliative care intervention into community-based settings. Journal of Hospice and Palliative Nursing, 20, 407–415.
Skalla, K.A., & Ferrell, B. (2015). Challenges in assessing spiritual distress in survivors of cancer. Clinical Journal of Oncology Nursing, 19, 99–104. https://doi.org/10.1188/15.CJON.99-104
Steinhauser, K.E., Fitchett, G., Handzo, G.F., Johnson, K.S., Koenig, H.G., Pargament, K.I., . . . Balboni, T.A. (2017). State of the science of spirituality and palliative care research part I: Definitions, measurement, and outcomes. Journal of Pain and Symptom Management, 54, 428–440.
Taylor, E.J., Gober-Park, C., Schoonover-Shoffner, K., Mamier, I., Somaiya, C.K., & Bahjri, K. (2017). Nurse religiosity and spiritual care: An online survey. Clinical Nursing Research. Advance online publication. https://doi.org/10.1177/1054773817725869
Taylor, E.J., Mamier, I., Ricci-Allegra, P., & Foith, J. (2017). Self-reported frequency of nurse-provided spiritual care. Applied Nursing Research, 35, 30–35.
Wittenberg, E., Ferrell, B., Goldsmith, J., & Buller, H. (2016). Provider difficulties with spiritual and forgiveness communication at the end of life. American Journal of Hospice and Palliative Care, 33, 843–848. https://doi.org/10.1177/1049909115591811




