The African Caribbean Immigrant Cancer Survivor Experience in the United States: A Scoping Review of the Literature
Problem Identification: Growing numbers of African Caribbean immigrants with cancer reside in the United States and frequently encounter different challenges than survivors born in the United States.
literature Search: More than a decade of research was searched in the PubMed®, Embase®, CINAHL®, and Scopus® databases using terms reflective of African Caribbean immigrant survivors in the United States.
Data Evaluation: The initial search in this scoping review revealed 912 articles, with seven meeting inclusion criteria. Data extracted from articles included purpose/aims, design, sample/setting, methods, and results.
Synthesis: Five retrospective analyses, one case report, and one qualitative study comprised the final sample. Thematic analysis used to synthesize results revealed two themes: survival patterns and barriers.
Implications for Research: The results indicated a need to identify and address root causes of disparity, and track the effectiveness of available treatments and outcomes by country of birth. Research capturing the experiences of African Caribbean immigrants would benefit from collaboration with community leaders and survivors. Oncology nurses play critical roles in leading research and developing culturally informed practices in clinical settings.
Jump to a section
Cancer is a serious and unrelenting problem among Black people in the United States. Black Americans have the highest death rate from cancer of any racial or ethnic group and experience the shortest survival after diagnosis. The highest cancer incidence rates occur among Black men (American Cancer Society [ACS], 2019). Factors implicated in the high cancer burden experienced by Black Americans are myriad and complex and include biologic, inherited, and cultural differences, which can lead to higher risk for cancer. Other equally important factors are socioeconomic disparities, barriers and obstacles to accessing high-quality cancer care, and structural racism, all of which may result in higher incidence and mortality from cancer (ACS, 2021). Prostate cancer is the most commonly diagnosed cancer in Black men, and breast cancer is the most commonly diagnosed cancer in Black women (ACS, 2019).
Non-Hispanic Black people currently comprise approximately 13% of the total U.S. population (U.S. Census Bureau, 2019). Non-Hispanic Black people are the second largest underrepresented ethnic group in the United States and are projected to comprise about 15% of the total population by 2060 (U.S. Census Bureau, 2019). Black Americans are a diverse group primarily concentrated in the South (ACS, 2019). The Black immigrant population has increased considerably in the past 40 years to a total of more than 4 million Black immigrants residing in the United States in 2013 (Anderson, 2015). Rapid growth in the Black immigrant population is expected to continue, particularly in the Miami, New York City, and Washington, DC, metropolitan areas, where as many as a third of Black people are immigrants (Anderson, 2015).
About half of the Black immigrant population in the United States was born in Caribbean countries, particularly Jamaica and Haiti, and 38% of Black immigrants were born in African countries (ACS, 2019). About 63% of Caribbean immigrants lived in the New York and Miami metropolitan areas as of 2017 (Zong & Batalova, 2019). Compared to the total immigrant population, Caribbean immigrants are less likely to have limited English proficiency but more likely to have lower educational attainment or live in poverty (Zong & Batalova, 2019).
There has been an increased focus on identifying and eliminating disparities in cancer screening, detection, diagnosis, and treatment among members of underserved racial and ethnic groups in the United States, including members of immigrant groups. Immigrants face many challenges while navigating health systems to access cancer screening, diagnosis, and treatment, and they experience many barriers that frequently translate to worse clinical outcomes (Lockhart et al., 2018, 2020). Discrimination contributes to disparities in cancer care and results in lower-quality care for members of underrepresented racial and ethnic groups compared to care received by non-Hispanic White people (ACS, 2021). These disparities exist even when insurance status, age, severity of disease, and health status are comparable (ACS, 2021). Cultural factors may influence risk factor behaviors among racial and ethnic underrepresented groups, which can potentially affect the occurrence of cancer (ACS, 2021). This scoping review examines the scholarship targeting African Caribbean adult cancer survivors who immigrated to the United States. Results will be used to guide future research.
Methods
The authors followed the PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) Extension for Scoping Reviews (Tricco et al., 2018) and the framework outlined by Arksey and O’Malley (2005) to conduct a scoping review of the literature focused on African Caribbean immigrant survivors living in the United States. This framework addresses five steps as follows: create a research question, search for studies, select relevant studies, chart data, and then collate, summarize, and describe findings (Arksey & O’Malley, 2005). It provides a method to address an exploratory research question, map key concepts, find available evidence, identify gaps in research, and synthesize existing literature. PRISMA Extension for Scoping Reviews provides 20 essential steps for reporting scoping reviews and two optional steps. The optional steps are “12. Critical appraisal of individual sources of evidence” and “16. Critical appraisal within sources of evidence.” Because this scoping review was exploratory in nature and found relatively few studies, the authors concluded that these critical appraisal steps were not appropriate to the scoping review’s objectives (Tricco et al., 2018).
Literature Review
The authors performed searches in the PubMed®, Embase®, CINAHL®, and Scopus® databases. The search strategy focused on four broad groups of terms that described the following: (a) countries of origin and racial, ethnic, or nationality descriptors for African Caribbean people; (b) immigrants or immigration; (c) survivors or patients with cancer; and (d) the United States and individual state names. The search used keywords, controlled vocabulary terms, and Boolean search logic to combine terms with the goal of maximizing search recall. To identify the countries of origin for African Caribbean immigrants, the authors used the following definition of the “Caribbean Region” available in PubMed’s MeSH (Medical Subject Headings) Database:
The area that lies between continental North and South America and comprises the Caribbean Sea, the West Indies, and the adjacent mainland regions of southern Mexico, Central America, Colombia, and Venezuela. (National Library of Medicine, 2021)
The authors then used the names of these countries and territories as keywords, supplementing them with terms used to describe inhabitants of each country and the region, as well as appropriate controlled vocabulary terms associated with each database searched. Results were limited to English-language journal articles published from January 2011 through June 2021. This time span was chosen to collect and analyze the most current evidence focused on African Caribbean immigrant survivors in the United States.
Inclusion and Exclusion Criteria
Inclusion criteria were studies with participants who were survivors of all types and stages of cancer, aged 18 years or older, of any gender, immigrants, and currently living in the United States. No limits were placed on the number of years that immigrant survivors lived in the United States, the type of study design, or the type of evidence included in the review. At the beginning of the review process, the authors intended to include people from all countries and territories in the Caribbean Region defined by PubMed’s MeSH Database (National Library of Medicine, 2021). As the review proceeded, the authors decided to exclude individuals from Puerto Rico and the U.S. Virgin Islands because they are U.S. citizens, not immigrants. Unlike systematic reviews, developing or modifying inclusion and exclusion criteria post hoc is acceptable within the scoping review methodology because of the exploratory nature of the research question (Arksey & O’Malley, 2005). Studies were excluded if adult African Caribbean immigrant survivors comprised less than 50% of the total study sample, if articles failed to clearly delineate the race and ethnicity of their participants, or if study samples consisted of healthcare providers or families of adult immigrant survivors.
Figure 1 illustrates the steps of the study selection process using PRISMA guidelines (Moher et al., 2009). The authors used Covidence to facilitate the review process. Covidence removes duplicate citations and enables independent screening of titles and abstracts for inclusion, as well as full-text review for exclusion. When the authors reached different conclusions during the review process, they discussed the studies to reach consensus. The authors identified 130 studies for full-text review and selected 12 studies for data extraction. After closer examination of demographic data, 5 of these 12 studies were eliminated because of either insufficient African Caribbean participants based on inclusion criteria of 50% or greater, or difficulty in identifying African Caribbean immigrants within the total sample of survivors. As a result, the scoping review consisted of seven articles.

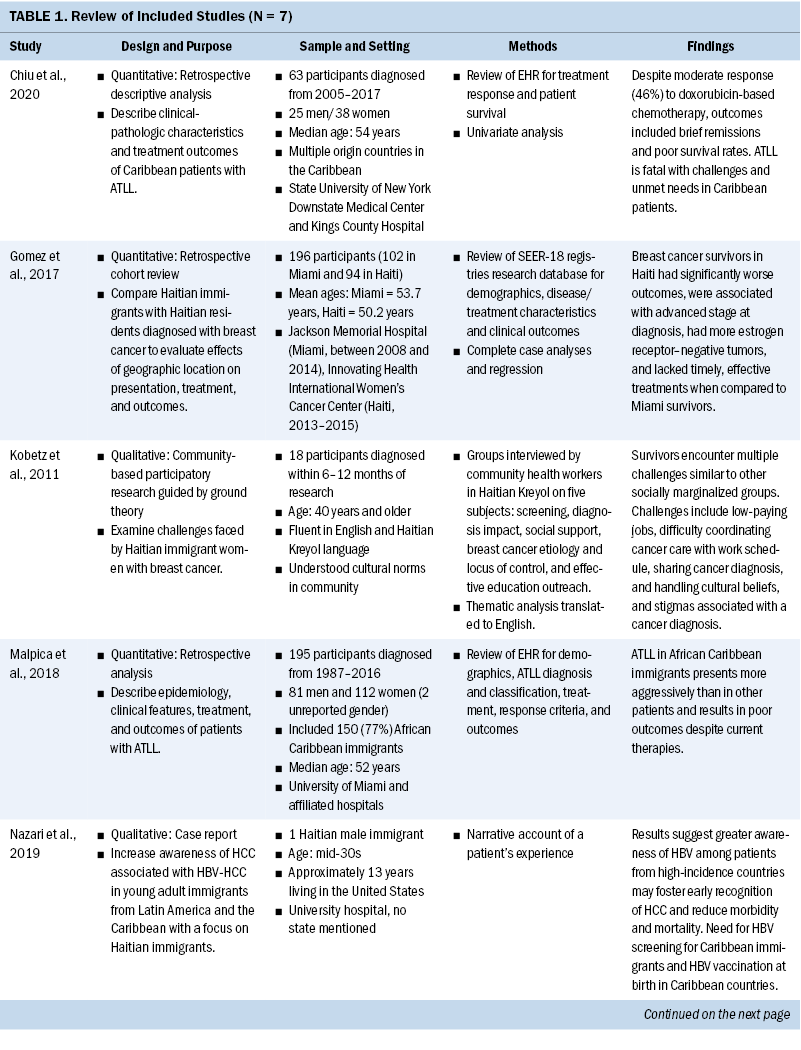
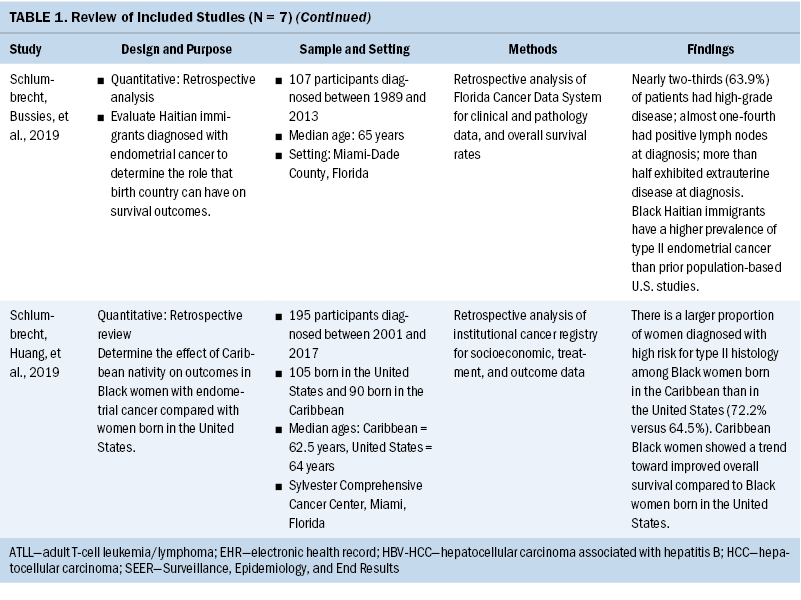
After reading the full-text versions of the studies, two authors who were experienced oncology nurse researchers extracted key data from each study into a matrix table to facilitate analysis and synthesis. Table 1 illustrates study data organized by author and publication date, design and purpose, sample population and setting, methodology, and results. This charting of studies facilitated thematic analysis based on common concepts noted across each study, which aligned with Arksey and O’Malley’s (2005) scoping review framework.
Results
Description of Studies
Most studies (n = 5) were quantitative, retrospective analyses of demographic and health-related data extracted from electronic health records or state and national cancer registries (Chiu et al., 2020; Gomez et al., 2017; Malpica et al., 2018; Schlumbrecht, Bussies, et al., 2019; Schlumbrecht, Huang, et al., 2019). The remaining two articles were a single case report (Nazari et al., 2019) and a qualitative participatory action study (Kobetz et al., 2011). Settings were in Florida (n = 5), New York (n = 1), and one study did not mention a setting. Haitians were represented among samples in all seven studies, either as the targeted sample (n = 4) or included among other African Caribbeans (n = 3) from Jamaica, Trinidad, Grenada, Saint Vincent, Guyana, Barbados, Antigua, Nevis, Panama, U.S./British Virgin Islands, Barbuda, St. Kitts, Martinique, and Tobago. While residents from the U.S. Virgin Islands were generally excluded because of their U.S. citizenship, the scoping review did include data about two U.S. Virgin Islands immigrants reported by Malpica et al. (2018). The demographic description given in the article did not provide enough detail to exclude these two cancer survivors from the study sample, consisting of 150 African Caribbean immigrants diagnosed with cancer. The number of years that survivors lived in the United States was mentioned by Nazari et al. (2019), who described one immigrant who lived in the United States for 13 years. Among all studies, men (n = 107) and women (n = 467), aged 27 to 88 years (median ages at diagnosis from 52 to 65 years across all studies) were represented. Study participants were diagnosed with the following cancers: adult T-cell lymphoma/leukemia (ATLL) (n = 2), breast (n = 2), endometrial (n = 2), and hepatitis-B (HBV)–associated hepatocellular carcinoma (HCC) (n = 1). Retrospective reviews reported sample sizes from 63 to 150 African Caribbean immigrant survivors (Chiu et al., 2020; Gomez et al., 2017; Malpica et al., 2018; Schlumbrecht, Bussies, et al., 2019; Schlumbrecht, Huang, et al., 2019); the qualitative study had 18 immigrants (Kobetz et al., 2011) and the case report included one participant (Nazari et al., 2019). All but one study was published from 2018 to 2020 (n = 6) (Chiu et al., 2020; Gomez et al., 2017; Malpica et al., 2018; Nazari et al., 2019; Schlumbrecht, Bussies, et al., 2019; Schlumbrecht, Huang, et al., 2019).
Theme 1: Survival Patterns
Six articles in this scoping review described the survival patterns (e.g., epidemiology/pathology, clinical presenting features, survival/treatment outcomes) of African Caribbean immigrants diagnosed with breast cancer (Gomez et al., 2017), endometrial cancer (Schlumbrecht, Bussies, et al., 2019; Schlumbrecht, Huang, et al., 2019), hepatocellular cancers (Nazari et al., 2019), and T-cell leukemias/lymphomas (Chiu et al., 2020; Malpica et al., 2018). Although every study included Haitian immigrants living in the United States, half of them (n = 3) included Haitians within a larger African Caribbean sample of immigrant survivors (Chiu et al., 2020; Malpica et al., 2018; Schlumbrecht, Huang, et al., 2019).
Breast cancer in Haitian immigrants: Breast cancer incidence and mortality continue to rise, particularly in low- and middle-income countries (Martei et al., 2018). Noted disparities in outcomes from breast cancer exist among women in different ethnic, racial, and socioeconomic groups, which may be a result of differences in biologic factors as well as disparities in access to screening and treatment. Confounding the situation is the lack of accurate information from cancer registries in many areas of the world (Gomez et al., 2017).
Gomez et al. (2017) compared Haitian immigrants diagnosed with breast cancer residing in Miami who presented at one tertiary, safety net medical center (n = 102), with women diagnosed with breast cancer at a cancer center in Haiti (n = 94). Researchers evaluated the impact of geographic location on the presentation, treatment, and outcomes of these women with breast cancer. Data were extracted from the Surveillance, Epidemiology, and End Results (SEER) registries. Results revealed women with breast cancer who were Haitian residents had “significantly worse” (Gomez et al., 2017, p. 389) health encounters, such as diagnoses at more advanced stages, shorter survival times, and higher mortality, than Haitian immigrants to Miami. Poorer outcomes in the Haitian residents’ cohort were attributed to lack of screening and access to care, limited pathologic evaluation of tumor receptor status, diagnosis and treatment delays, and no access to radiation therapy or HER2 targeted therapy. Women diagnosed with breast cancer in Haiti experienced a median wait time of 20 months from onset of symptoms to first medical evaluation of symptoms. In comparison, in the United States, median range of symptom duration before treatment was 30 to 40 days, with more than 60% of patients beginning treatment fewer than three months after symptoms began (Gomez et al., 2017).
Women who were residents of Haiti at the time of their diagnosis and treatment of breast cancer presented at later, more advanced stages and presented with more estrogen receptor–negative (ER-negative) disease than did immigrant women. Haitian women were almost twice as likely to be diagnosed with triple-negative breast cancer as Haitian immigrants living in Miami (all ER and HER2 testing was done in the United States). Implications from this study suggest that additional research in larger scale studies is warranted to discern if disparities exist within subgroups of African Caribbean women diagnosed with breast cancer (Gomez et al., 2017).
Endometrial cancer in African Caribbean and in Haitian immigrants: Like breast cancer, the incidence of endometrial cancer continues to rise globally. Although rising incidence is linked to increasing rates of obesity in women across the world, Black women are at higher risk for being diagnosed with type II, high grade, more aggressive endometrial tumors. The reasons Black women are being diagnosed with more aggressive tumors is theorized to be linked to genetic susceptibilities, differences in tumor histologies, and variability in risk factors (Schlumbrecht, Huang, et al., 2019). Black women account for almost 14% of deaths from endometrial cancer, although only 7% of new cases of endometrial cancer are diagnosed in Black women (Long et al., 2013).
Schlumbrecht, Huang, et al. (2019) postulated that the country of birth may be an important consideration affecting outcomes from endometrial cancer, because it may predispose women to varying types of environmental exposures and epigenetic changes. Because one in every 10 Black people in the United States are immigrants, and 50% of immigrants are from the Caribbean, these researchers evaluated the role of Caribbean country of birth on survival outcomes in Black women with invasive endometrial cancer diagnosed and treated in Miami in one institution between 2001 and 2017 (N = 1,964). Study participants were non-Hispanic Black women born in the Caribbean or the United States as identified an institutional cancer registry (Schlumbrecht, Huang, et al., 2019).
A total of 195 women met the inclusion criteria for the study (105 born in the United States and 90 born in Caribbean countries) (Schlumbrecht, Huang, et al., 2019). No differences were noted between U.S. and Caribbean Black women by age of diagnosis, treatments received, or current alcohol use. More Caribbean women (72.2%) were diagnosed with type II tumors compared to 64.5% of U.S. women. However, Caribbean women appeared to have higher long-term survival rates compared to women born in the United States, although the difference was not statistically significant (Schlumbrecht, Huang, et al., 2019).
Study results confirm that Black women from the Caribbean are at much higher risk for the development of type II endometrial cancer (Schlumbrecht, Huang, et al., 2019). Specific factors that place these women at higher risk are not currently known, although genetic predisposition may play a significant role (Schlumbrecht, Huang, et al., 2019).
In a similar study conducted by Schlumbrecht, Bussies, et al. (2019), data were obtained from the Florida Cancer Data System, Florida’s cancer registry, to identify a cohort of women aged 18 years and older from Miami-Dade County who were diagnosed with endometrial cancer between 1989–2013 and whose country of birth was Haiti (n = 107; median age 65 years). Clinical data were extracted and analyzed to determine associations with overall survival. Almost 64% of patients were diagnosed with type II, high- grade tumor histology, and more than 52% presented with extrauterine metastatic disease at time of diagnosis. These outcomes are comparable to those described in the study conducted by Schlumbrecht, Huang, et al. (2019). Further investigation is needed to determine the genetic, epigenetic, and behavioral impacts on the incidence of endometrial cancer in non-Hispanic Black women, which is growing at a rate faster than in women in other racial and ethnic groups (Cote et al., 2015; Schlumbrecht, Huang, et al., 2019).
HBV-associated HCC in Haitian immigrants: HBV is endemic in many Latin American and Caribbean countries such as Haiti, and incidence of HCC is highest in U.S. immigrants from Haiti among all Caribbean immigrants (Roman et al., 2014; Wasley et al., 2010). Although HBV is treatable if detected early and screening guidelines are available, many Haitian immigrants are not screened or vaccinated. HBV prevalence in Haiti is very high, with an estimated seroprevalence rate of 2%–8% compared to the U.S. rate of 0.27% (Roman et al., 2014; Wasley et al., 2010).
Nazari et al. (2019) relate a case report of a young Haitian immigrant in his mid-30s who was hepatitis B surface antigen positive and subsequently diagnosed with HCC. With no known previous significant medical history, he presented to the emergency department with a two-week history of epigastric pain and a 20-pound unintentional weight loss within the preceding two months. The patient’s physical evaluation was otherwise unremarkable. He denied alcohol, nonsteroidal anti-inflammatory drug use, or recent infection, had no history of sexually transmitted infection, and denied injection drug use and blood transfusions. He reported more than a dozen sexual partners in the past year with consistent use of condoms. The patient had moved to the United States at age 17 and had not received childhood vaccines for HBV.
The admitting physician ordered a computed tomography of the abdomen and pelvis, revealing multiple lesions in the liver. Moderately differentiated HCC was confirmed. Positron-emission tomography scans showed areas of diffuse metastasis. The patient had a positive hepatitis B surface antigen test at the time of initial workup. This patient was not a surgical candidate. Despite treatment as part of a clinical trial, the patient died 15 months after diagnosis.
This patient had two factors that placed him at high risk for HBV infection, immigration from a high prevalence country and his sexual practices, and he should have been offered screening and hepatitis B vaccination as part of a primary care visit. The study concluded that healthcare providers should maintain a high level of suspicion for infection with HBV, particularly for immigrants from Caribbean countries (Nazari et al., 2019).
ATLL in African Caribbean immigrants: ATLL is a rare peripheral T-cell cancer caused by the human T-cell leukemia virus type I (HTLV-1) most commonly transmitted during breastfeeding, blood product transfusions, sharing of contaminated needles, and during sexual intercourse. HTLV-1 is endemic in many parts of the world, including Japan and the Caribbean countries of Haiti, Jamaica, and the Dominican Republic (Gessain & Cassar, 2012). Cases of ATLL diagnosed in the United States reflect migration patterns from endemic areas such as Japan and the Caribbean (Chiu et al., 2020). ATLL is typically diagnosed in adults in their 60s and 70s, with the more aggressive acute type diagnosed most frequently. Although treatment is available, ATLL remains incurable and is associated with poor survival outcomes (Chiu et al., 2020; Malpica et al., 2018).
Malpica et al. (2018) described the results of a retrospective analysis of cases of 195 patients diagnosed with ATLL between January 1987 and December 2016 at the University of Miami and affiliated hospitals in the region with a high prevalence of HTLV-1 diseases to determine epidemiology, clinical features, treatment, and survival outcomes to guide diagnosis and treatment options for this rare and challenging cancer. More than 90% of patients in this cohort presented with aggressive ATLL, and most were women. Most patients (77%) were immigrants from Haiti (39%), Jamaica (24%), and other islands in the Caribbean. The median age at diagnosis was 52 years, which is similar to other studies describing African Caribbean patients diagnosed with ATLL. However, the median age observed in the Caribbean cohort is a decade younger than observed in Japanese patients, a different ethnic group with high incidence rates of ATLL (Satake et al., 2015).
Despite treatment with recommended first-line therapies such as zidovudine and interferon alpha, the median survival for patients in this study who presented with acute, aggressive ATLL was 4.1 months with a 4-year survival rate of 10%. ATLL, particularly in African Caribbean patients diagnosed with aggressive subtypes, remains a largely incurable, fatal disease (Malpica et al., 2018; Zell et al., 2016).
More recently, Chiu et al. (2020) completed a retrospective analysis of 63 patients who were diagnosed with ATLL between 2005 and 2017 at two affiliated New York City hospitals serving a predominantly Caribbean population. The study’s median age at diagnosis was 54 years. Like the findings reported by Malpica et al. (2018), most participants were women, and most were diagnosed with acute, aggressive subtypes of ATLL. More than 80% of patients were treated with first-line chemotherapy protocols, which resulted in an overall response rate of 46%. The median overall survival was 5.5 months with median relapse by four months. The overall survival rate at one year was 20%, comparable to previously published survival rates in this population. The study concluded that it is imperative to further investigate epigenetic, biologic, and other factors that may result in poor outcomes in Caribbean immigrants diagnosed with ATLL to determine more effective treatment strategies, which could lead to improved long-term survival outcomes (Chiu et al., 2020).
Theme 2: Barriers
Breast cancer in Haitians: A study conducted by Kobetz et al., (2011) focused on the challenges encountered by 18 Haitian immigrant breast cancer survivors. It was conducted in the Little Haiti area of Miami as part of the community-based participatory research (CBPR) program, Patne en Aksyon (Partners in Action). The objectives of CBPR are to allow community leaders to define the focus of research based on the community’s language preferences, literacy levels, and sociocultural context as it relates to health and disease prevention (Kobetz et al., 2011). Other CBPR objectives are for community leaders to identify culturally appropriate recruitment strategies and methods of data accumulation.
Study participants were interviewed in three focus groups made of six Haitian women over three months, who were diagnosed with breast cancer within the past 6–12 months. Community health workers conducted the focus groups in the Kreyol language using a guide developed with community and academic partners. The goals of the guide were to elicit discussion in five major areas: (a) knowledge of screening recommendations, (b) causes of breast cancer and participant beliefs about locus of control related to health and disease, (c) availability of social support systems, (d) impact of diagnosis of breast cancer, and (e) survivors’ recommendations of effective strategies and methods for health-related educational outreach in their communities (Kobetz et al., 2011).
Study findings and participant experiences reflected those reported by other socially marginalized groups (Kobetz et al., 2011). Significant demographic and sociodemographic shifts among survivors are projected to continue in the short term (Alfano et al., 2019). Survivors from disadvantaged groups suffer poorer health outcomes because of informational, communication, structural, and financial barriers encountered in accessing timely care and appropriate treatment (Lee Smith & Hall, 2015). Participants in the study by Kobetz et al. (2011) described barriers they encountered, such as reduced capacity to work after being diagnosed with cancer, hesitancy to disclose a cancer diagnosis because of fears their cancer diagnosis would be viewed by others as a punishment from God, fears of stigmatization from others in the community who believe that cancer is contagious, obstacles to screening, and treatment delays. These barriers reduce quality of life and result in poorer survival outcomes among medically underserved communities (Kobetz et al., 2011).
Discussion
This scoping review provides an evidence-based account about the experiences of African Caribbean cancer survivors who immigrated to the United States. Arksey and O’Malley’s (2005) scoping framework guided this review. It provides readers with a first step that maps the “extent, range, and nature of research activity” (p. 21) and highlights potential gaps in current evidence that may warrant future investigation (Arksey & O’Malley, 2005).
Study Samples
This review revealed a paucity of evidence dominated by retrospective reviews. This differed from previous scoping reviews on Hispanic/Latinx and Asian immigrant survivors, which contained a greater diversity of study design and comprised 18 and 32 studies, respectively (Lockhart et al., 2018, 2020). Differences may be because of the small portion of African Caribbean immigrants within the U.S. population compared to Hispanic/Latinx and Asian immigrants. African Caribbean survivors may have been grouped in study samples labeled as Non-Hispanic African, African American, or Black and were not effectively tracked. A study by Walters (1994) found that many Caribbean immigrants preferred to be identified by their native countries rather than being clustered among a larger category of Black or African American.
Many Black immigrants arriving in the United States, particularly Haitians, settled in Miami and New York City (Anderson, 2015). Migration patterns might explain the predominance of Haitian study participants and settings in this review. It is important to collect evidence about access to healthcare services, providers, and community support among African Caribbean immigrants who reside in other U.S. regions congruent with their cultural customs. Like prior scoping reviews (Lockhart et al., 2018, 2020), the median age of study participants, ranging from 52 to 65 years, highlights the need to identify effective strategies to proactively address survivors’ challenges such as balancing work and home responsibilities with cancer treatments and side effects. The predominance of women in this review likely resulted from greater representation of breast and endometrial cancers in the included studies. A few comparison studies illustrated valuable collaborations between researchers in the United States and Caribbean countries.
Themes
Evidence captured from the retrospective reviews on survival patterns provides insight into the challenges encountered by health professionals in diagnosing and treating select cancers in the African Caribbean immigrant population compared with other racial and ethnic groups. Survival studies in this review were mapped by cancer type, and targeted the African Caribbean subgroup when available to facilitate comparison with other datasets that describe survival patterns by cancer diagnosis, race, or ethnicity.
Results illustrate the deleterious impact that healthcare disparities, such as delayed diagnosis and treatment, lack of access, and lack of effective treatments, may pose on survival. Future research is needed to validate reasons for these disparities and test creative strategies to minimize them. Aggregated data from retrospective reviews were frequently based on broad ethnic populations and labeled as “African Caribbean” or “Black,” rather than using subgroups that reflected immigrants’ nativity. Similar aggregate analyses were also prevalent in previous reviews about Hispanic/Latinx and Asian immigrants (Lockhart et al., 2018, 2020). Collecting data by subgroups may reveal underlying genetic differences, culturally influenced lifestyles, and environmental influences that affect survival outcomes (Gomez et al., 2017). Further study could increase awareness of existing disparities within high-risk subgroups who could benefit from targeted prevention, screening, and treatment (Gomez et al., 2017).
Barriers expressed by Haitian immigrant survivors (Kobetz et al., 2011) mirrored obstacles cited in previous scoping reviews on the experience of immigrant survivors (Lockhart et al., 2018, 2020). For example, Hispanic/Latinx immigrant survivors were challenged by a lack of knowledge about cancer-related topics (Costas-Muniz et al., 2013), cultural beliefs (Buki et al., 2008), and issues affecting treatment adherence (Gany et al., 2011, 2013). Haitian women’s socioeconomic concerns associated with a cancer diagnosis aligned with those expressed by Asian immigrants (Wang et al., 2013). However, social support issues experienced by Haitian survivors were framed as quality-of-life challenges among Asian immigrant survivors (Centers for Disease Control and Prevention, 2019; Lee et al., 2013; Lewis et al., 2010). It is critical to understand the barriers experienced by immigrant survivors who comprise a vulnerable, underserved, and growing U.S. population. Identifying root causes of health disparities and testing creative strategies to minimize those disparities in clinical practice and research can improve cancer outcomes.
Limitations
This review had several limitations, despite efforts taken to minimize them. First, the search terms, selected databases, and time span for inclusion may have prevented the retrieval of additional studies. However, an experienced health science librarian guided the search process, and two seasoned oncology nurse researchers carefully reviewed each study to determine its congruence with the review’s purpose. It was important to capture research that reflected the current experience of African Caribbean immigrants.
Second, excluding studies with samples that contained less than 50% African Caribbean immigrants limited the number of studies in the review. Conducting this critical appraisal in this review may have decreased the final sample to a larger degree. However, this decision was essential to capture and map current evidence relevant to the review’s purpose.
Third, only one study (Nazari et al., 2019) cited the number of years that immigrant survivors had resided in the United States. None of the studies mentioned participants’ immigration or socioeconomic status. This data could showcase the potential unmet needs of survivors at different points along their timeline of immigration to the United States.
Finally, the predominance of retrospective analyses in this review provides valuable data for future interventions regarding African Caribbean immigrants’ treatment and survival outcomes. However, only one study (Kobetz et al., 2011) contained the immigrants’ own perspectives. Obtaining the personal experiences of immigrant survivors is crucial in designing and testing culturally appropriate interventions.
Implications for Nursing
To the authors’ best knowledge, this is the first scoping review that synthesized published evidence about African Caribbean immigrants diagnosed with cancer and living in the United States. Because of the novelty of this review and the growing number of African Caribbean immigrants to the United States, these results provide direction to oncology nurses who play pivotal roles in cancer research and clinical practice. Only one study in this review (Kobetz et al., 2011) was coauthored by a nurse.
The Oncology Nursing Society’s current research agenda (Von Ah et al., 2019) provides nurse researchers the opportunity to improve the health outcomes of African Caribbean immigrant survivors by prioritizing health disparities among socioeconomically disadvantaged populations in the United States. Recent updates to the ONS research agenda provide nurses with additional guidance regarding research priorities aimed to address structural racism and health inequities (Jones et al. 2021a), and with strategies that promote equity in oncology healthcare access and workforce development (Jones et al, 2021b). Additional focus on the growing population of older survivors can strengthen access to cancer care and survival outcomes.
Retrospective reviews tracking the cancer survival patterns of African Caribbean immigrants in the United States should continue, because they provide valuable information regarding factors that influence survival, such as risk factors, pathology, and treatment effectiveness. The survival studies in this review used data from 1987 to 2017 (Chiu et al., 2020; Gomez et al., 2017; Malpica et al., 2018; Schlumbrecht, Bussies, et al., 2019; Schlumbrecht, Huang, et al., 2019), warranting ongoing studies to reflect more recent disease patterns and current treatment responses. Sorting and analyzing data by specific racial and ethnic subgroups within the larger African Caribbean population dataset may provide insight regarding the impact of birth country, genetics, lifestyle factors, and cultural customs on cancer outcomes. Exploring reasons for health disparities and developing interventions to address them are essential next steps. Finally, research is needed to gain insight into the personal experiences of African Caribbean immigrants after receiving and while managing their cancer diagnoses. Exploring the cultural norms, beliefs, values, and practices unique to each subgroup will enable researchers to target interventions and reduce disparities. The CBPR study by Kobetz et al. (2011) provides an excellent model for oncology nurse researchers to replicate by partnering with community group members to address the unmet needs of survivors in a culturally informed manner.
In addition to guiding future research, this scoping review may offer direction to healthcare professionals by providing culturally informed care to African Caribbean immigrant survivors. As suggested by Kobetz et al. (2011), oncology nurses need to assume leadership roles in educating others about the needs of African Caribbean immigrants diagnosed with cancer, advocating for survivors to reduce health disparities, partnering with individuals and groups in the African Caribbean community who can provide personal perspectives framed by cultural beliefs, values, and practices, and implementing strategies that minimize barriers and improve survival outcomes.

Conclusion
This scoping review captured a decade of research about African Caribbean immigrants in the United States who are cancer survivors. The results revealed a variety of retrospective reviews of survival patterns and offered strategies for future treatment and exploration. Two studies shared the personal accounts of immigrants after their cancer diagnosis, and one of these studies provided insight into their lives through their own voices. The results of this review provide direction for future research and culturally informed cancer practice.
About the Authors
Joan Such Lockhart, PhD, RN, CNE®, ANEF, FAAN, is a professor and the director of the MSN Nursing Education Program in the School of Nursing at Duquesne University in Pittsburgh, PA; Melinda G. Oberleitner, DNS, RN, FAAN, is the LHC Group–endowed dean of the College of Nursing and Allied Health Professions and the SLEMCO/BORSF Endowed professor in the Department of Nursing at the University of Louisiana in Lafayette; and David A. Nolfi, MLS, AHIP, is the head of research engagement and the health sciences/science, technology, engineering, and math initiatives and assessment coordinator in Gumberg Library at Duquesne University. No financial relationships to disclose. All authors contributed to the conceptualization and design and completed the data collection. Lockhart and Oberleitner provided statistical support and the analysis. All authors contributed to the article preparation. Lockhart can be reached at JLockhart76@gmail.com, with copy to ONFEditor@ons.org. (Submitted July 2021. Accepted December 20, 2021.)
References
Alfano, C.M., Leach, C.R., Smith, T.G., Miller, K.D., Alcaraz, K.I., Cannady, R.S., . . . Brawley, O.W. (2019). Equitably improving outcomes for cancer survivors and supporting caregivers: A blueprint for care delivery, research, education, and policy. CA: A Cancer Journal for Clinicians, 69(1), 35–49. https://doi.org/10.3322/caac.21548
American Cancer Society. (2019). Cancer facts and figures for African Americans, 2019-2021. https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and…
American Cancer Society. (2021). Cancer facts and figures, 2021. https://www.cancer.org/research/cancer-facts-statistics/all-cancer-fact…
Anderson, M. (2015). A rising share of the U.S. Black population is foreign born. Pew Research Center. https://www.pewresearch.org/social-trends/2015/04/09/a-rising-share-of-…
Arksey, H., & O’Malley, L. (2005). Scoping studies: Towards a methodological framework. International Journal of Social Research Methodology, 8(1), 19–32. https://doi.org/10.1080/1364557032000119616
Buki, L.P., Garcés, D.M., Hinestrosa, M.C., Kogan, L., Carrillo, I.Y., & French, B. (2008). Latina breast cancer survivors’ lived experiences: Diagnosis, treatment, and beyond. Cultural Diversity and Ethnic Minority Psychology, 14(2), 163–167. https://doi.org/10.1037/1099-9809.14.2.163
Centers for Disease Control and Prevention. (2019). Hepatitis B vaccination of adults. https://www.cdc.gov/hepatitis/hbv/vaccadults.htm
Chiu, E., Samra, B., Tam, E., Baseri, B., Lin, B., Luhrs, C., . . . Sidhu, G. (2020). Clinical characteristics and outcomes of Caribbean patients with adult T-cell lymphoma/leukemia at two affiliated New York City hospitals. JCO Global Oncology, 6, 548–556. https://doi.org/10.1200/JGO.19.00208
Costas-Muniz, R., Sen, R., Leng, J., Aragones, A., Ramirez, J., & Gany, F. (2013). Cancer stage knowledge and desire for information: Mismatch in Latino cancer patients? Journal of Cancer Education, 28, 458–465. https://doi.org/10.1007/s13187-013-0487-8
Cote, M.L., Ruterbusch, J.J., Olson, S.H., Lu, K., & Ali-Fehmi, R. (2015). The growing burden of endometrial cancer: A major racial disparity affecting Black women. Cancer Epidemiology, Biomarkers and Prevention, 24(9), 1407–1415. https://doi.org/10.1158/1055-9965.EPI-15-0316
Gany, F., Ramirez, J., Nierodzick, M.L., McNish, T., Lobach, I., & Leng, J. (2011). Cancer Portal Project: A multidisciplinary approach to cancer care among Hispanic patients. JCO Oncology Practice, 7(1), 31–38. https://doi.org/10.1200/JOP.2010.000036
Gany, F., Yogendran, L., Massie, D., Ramirez, J., Lee, T., Winkel, G., . . . Leng, J. (2013). “Doctor, what do I have?” Knowledge of cancer diagnosis among immigrant/migrant minorities. Journal of Cancer Education, 28, 165–170. https://doi.org/10.1007/s13187-012-0429-x
Gessain, A., & Cassar, O. (2012). Epidemiological aspects and world distribution of HTLV-1 infection. Frontiers in Microbiology, 3, 388. https://doi.org/10.3389/fmicb.2012.00388
Gomez, A., DeGennaro, V., George, S.H.L., Reis, I.M., Santamaria, E. Westin, G.F., . . . Hurley, J. (2017). Presentation, treatment, and outcomes of Haitian women with breast cancer in Miami and Haiti: Disparities in breast cancer — a retrospective cohort. JCO Global Oncology, 3(4), 389–397. https://doi.org/10.1200/jgo.2016.005975
Jones, R.A., Hirschey, R., Campbell, G., Cooley, M.E., Somayaji, D., Lally, R., . . . Gullatte, M.M. (2021a). Update to 2019–2022 ONS Research Agenda: Rapid review to address structural racism and health inequities. Oncology Nursing Forum, 48(6), 589–600. https://doi.org/10.1188/21.ONF.589-600
Jones, R.A., Hirschey, R., Campbell, G., Cooley, M.E., Somayaji, D., Lally, R., . . . Gullatte, M.M. (2021b). Update to 2019–2022 ONS Research Agenda: Rapid review to promote equity in oncology healthcare access and workforce development. Oncology Nursing Forum, 48(6), 604–612. https://doi.org/10.1188/21.ONF.604-612
Kobetz, E., Menard, J., Dietz, N., Hazan, G., Soler-Vila, H., Lechner, S., . . . Auguste, P. (2011). Contextualizing the survivorship experiences of Haitian immigrant women with breast cancer: Opportunities for health promotion. Oncology Nursing Forum, 38(5), 555–560. https://doi.org/10.1188/11.ONF.555-560
Lee, S., Chen, L., Ma, G.X., Fang, C.Y., Oh, Y., & Scully, L. (2013). Challenges and needs of Chinese and Korean American breast cancer survivors: In-depth interviews. North American Journal of Medicine and Science, 6(1), 1–8.
Lee Smith, J. & Hall, I.J. (2015). Advancing health equity in cancer survivorship: Opportunities for public health. American Journal of Preventive Medicine, 49(6, Suppl. 5), S477–S482. https://doi.org/10.1016/j.amepre.2015.08.008
Lewis, T.T., Aiello, A.E., Leurgans, S., Kelly, J., & Barnes, L.L. (2010). Self-reported experiences of everyday discrimination are associated with elevated C-reactive protein levels in older African-American adults. Brain, Behavior, and Immunity, 24(3), 438–443. https://doi.org/10.1016/j.bbi.2009.11.011
Lockhart, J.S., Oberleitner, M.G., & Nolfi, D.A. (2018). The Hispanic/Latino immigrant cancer survivor experience in the United States: A scoping review. In C.E. Kasper & R. Zoucha (Eds.), Annual review of nursing research: Vol 37. Transcultural and social research (pp. 119–160). Springer Publishing.
Lockhart, J.S., Oberleitner, M.G., & Nolfi, D.A. (2020). The Asian immigrant cancer survivor experience in the United States: A scoping review of the literature. Cancer Nursing, 43(3), 177–199. https://doi.org/10.1097/NCC.0000000000000797
Long, B., Liu, F.W., & Bristow, R.E. (2013). Disparities in uterine cancer epidemiology, treatment, and survival among African Americans in the United States. Gynecologic Oncology, 130(3), 652–659. https://doi.org/10.1016/j.ygyno.2013.05.020
Malpica, L., Pimentel, A., Reis, I.M., Gotuzzo, E., Lekakis, L., Komanduri, K., . . . Ramos, J.C. (2018). Epidemiology, clinical features, and outcome of HTLV-1–related ATLL in an area of prevalence in the United States. Blood Advances, 2(6), 607–620. https://doi.org/10.1182/bloodadvances.2017011106
Martei, Y.M., Pace, L.E., Brock, J.E., & Schulman, L.N. (2018). Breast cancer in low- and middle-income countries. Clinics in Laboratory Medicine, 38(1), 161–173. https://doi.org/10.1016/j.cll.2017.10.013
Moher, D., Liberati, A., Tetzlaff, J., & Altman, D.G. (2009). Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. PLOS Medicine, 6(7), e1000097. https://doi.org/10.1371/journal.pmed.1000097
National Library of Medicine. (2021). Caribbean region. MeSH Database. https://www.ncbi.nlm.nih.gov/mesh/?term=caribbean+region
Nazari, M., Rosenblum, J.S., & Trumbo, S. (2019). Hepatitis B–associated hepatocellular carcinoma in a young Haitian man: A review of screening guidelines. BMJ Case Reports, 12, e230530. https://doi.org/10.1136/bcr-2019-230530
Roman, S., Jose-Abrego, A, Fierro, N.A., Escobedo-Melendez, G., Ojeda-Granados, C., Martinez-Lopez, E., & Panduro, A. (2014). Hepatitis B virus infection in Latin America: A genomic medicine approach. World Journal of Gastroenterology, 20(23), 7181–7196.
Satake, M., Yamada, Y., Atogami, S., & Yamaguchi, K. (2015). The incidence of adult T-cell leukemia/lymphoma among human T-lymphotropic virus type 1 carriers in Japan. Leukemia and Lymphoma, 56(6), 1806–1812. https://doi.org/10.3109/10428194.2014.964700
Schlumbrecht, M., Bussies, P., Huang, M., Kobetz, E., & George, S. (2019). Endometrial cancer among a cohort of urban Haitian immigrants. World Journal of Clinical Oncology, 10(10), 340–349. https://doi.org/10.5306/wjco.v10.i10.340
Schlumbrecht, M., Huang, M., Hurley, J., & George, S. (2019). Endometrial cancer outcomes among non-Hispanic US born and Caribbean born Black women. International Journal of Gynecological Cancer, 29(5), 897–903. https://doi.org/10.1136/ijgc-2019-000347
Tricco, A.C., Lillie, E., Zarin, W., O’Brien, K.K., Colquhoun, H., Levac, D., . . . Straus, S.E. (2018). PRISMA extension for scoping reviews (PRISMA-ScR): Checklist and explanation. Annals of Internal Medicine, 169(7), 467–473. https://doi.org/10.7326/M18-0850
U.S. Census Bureau. (2019). Annual estimates of the resident population by sex, race, and Hispanic origin for the United States, states, and counties: April 1, 2010 to July 1, 2018. https://www2.census.gov/programs-surveys/popest/tables/2010-2018/state/…
Walters, M.C. (1994). Ethnic and racial identities of second-generation Black immigrants in New York City. International Migration Review, 28(4), 795–820. http://doi.org/10.2307/2547158
Wang, J.H., Adams, I.F., Tucker-Seeley, R., Gomez, S.L., Allen, L., Huang, E., . . . Pasick, R.J. (2013). A mixed method exploration of survivorship among Chinese American and non-Hispanic White breast cancer survivors: The role of socioeconomic well-being. Quality of Life Research, 22(10), 2709–2720. https://doi.org/10.1007/s11136-013-0374-0
Wasley, A, Kruszon-Moran, D., Kuhnert, W., Simard, E.P., Finelli, L., McQuillan, G., & Bell, B. (2010). The prevalence of hepatitis B virus infection in the United States in the era of vaccination. Journal of Infectious Diseases, 202(2), 192–201. https://doi.org/10.1086/653622
Von Ah, D., Brown, C.G., Brown, S.J., Bryant, A.L., Davies, M., Dodd, M., . . . Cooley, M.E. (2019). Research agenda of the Oncology Nursing Society: 2019-2022. Oncology Nursing Forum, 46(6), 654–669. https://doi.org/10.1188/19.ONF.654-669
Zell, M., Assal, A., Derman, O., Kornblum, N., Battini, R., Wang, Y., . . . Janakiram, M. (2016). Adult T-cell leukemia/lymphoma in the Caribbean cohort is a distinct clinical entity with dismal response to conventional chemotherapy. Oncotarget, 7(32), 51981–51990. https://doi.org/10.18632/oncotarget.10223
Zong, J., & Batalova, J. (2019). Caribbean immigrants in the United States. Migration Policy Institute. https://www.migrationpolicy.org/print/16425

