A Visual Case-Oriented Analysis of Stress-Related Symptoms in Caregivers of Allogeneic Bone Marrow Transplantation Recipients
Objectives: To describe trends in caregiver stress and stress-related symptoms (anxiety, depression, fatigue, and sleep disturbance) across 12 weeks post-transplantation.
Sample & Setting: 11 caregivers were recruited from a National Cancer Institute–designated comprehensive cancer center’s bone marrow transplantation (BMT) outpatient clinic in the southeastern United States.
Methods & Variables: A visual case-oriented analysis was conducted on data from 11 caregivers’ weekly self-reported data to identify trends after allogeneic BMT.
Results: The authors identified three primary trends as follows: U-shaped (highest symptoms at start of transplantation and end of study; n = 3), negatively sloped (highest symptoms at beginning of transplantation and decreasing over time; n = 2), and V-shaped predischarge (highest symptoms at start of transplantation and right before discharge home; n = 4). Two caregivers did not have postdischarge data because of patient death prior to study completion.
Implications for Nursing: Caregivers may benefit from additional support to manage their stress-related symptoms at the start of transplantation and just before discharge.
Jump to a section
Family and friend caregivers are increasingly relied on to care for patients receiving an allogeneic bone marrow transplantation (BMT) during the peritransplantation period (just before transplantation and 12 weeks after transplantation). Caregiving during the peritransplantation period is often accompanied by caregiving-related stress and downstream effects on caregivers’ health (e.g., high risk of anxiety, depression, fatigue, and cardiovascular disease) (Schulz & Beach, 1999; Stenberg et al., 2010; Trevino et al., 2017). Patients undergoing BMT are being discharged earlier to ambulatory and home care, with clinical care responsibilities shifting to caregivers and likely increasing the burdens that caregivers experience (Applebaum et al., 2016). In more recent care models, BMT recipients have been discharged to the responsibility of their caregivers as early as a few days after transplantation. Caregivers’ experiences with transition from inpatient to outpatient and home care when their stress levels are likely heightened have not been well described (Applebaum et al., 2016; Kisch et al., 2021).
Background
Caregivers are crucial in the care of recipients of allogeneic BMT, and their ability to provide care is directly affected by the caregivers’ own health. Because caregivers are so essential, BMT programs require patients to identify at least one primary caregiver before initiating transplantation (Applebaum et al., 2016; Foster et al., 2005). The caregiver must be committed to providing care 24 hours a day, seven days a week during the peritransplantation period (Applebaum et al., 2016; Foster et al., 2005). Patients are usually hospitalized until they are deemed medically stable, they are able to maintain their weight and nutritional status, and there is consistent evidence that the patient’s white blood cells have returned and the BMT has engrafted. At that point, if their permanent residence is distant from the BMT center, patients will move to temporary housing for as long as one year and are followed on an outpatient basis. Outpatient care consists of daily clinic visits and caregiver-driven, round-the-clock monitoring for transplantation-related side effects and toxicities (e.g., graft-versus-host disease, mental status changes, psychosocial issues) (Atilla et al., 2017; Bergeron, 2017; Maffini et al., 2017). Although patients are receiving outpatient follow-up, their caregivers are solely responsible for managing medications, transporting to and from clinic visits, monitoring for signs and symptoms of BMT-related complications, and deciding whether to contact the healthcare team (Von Ah et al., 2016; Williams, 2007). Little is known about how care setting transitions from hospital to outpatient care and subsequent changes to caregiving demands affect caregiver stress experiences.
Caregivers typically are screened prior to transplantation to ensure that they are capable of physically and mentally caring for patients undergoing BMT (Gemmill et al., 2011). Follow-up monitoring of the caregiver can range from informal check-ins during a patient’s clinical visit to formal assessment through distress screening (Wulff-Burchfield et al., 2013). The latter is often a rare occurrence because the visit typically focuses on the patient. Longitudinal work done by Kisch et al. (2021) highlighted that the greatest needs of caregivers of allogeneic BMT recipients included dealing with their feelings and knowing what to expect in the future, and that these needs do not always diminish over time.
Several factors may place caregivers at increased risk for caregiving-related stress, including being younger (aged younger than 35 years) (Kent, 2020) and having multiple caregiving roles (Bevans & Sternberg, 2012; Simoneau et al., 2013). Younger caregivers (aged younger than 35 years) may have less life experience in managing demands of caregiving than their older counterparts (Kent, 2020). Competing responsibilities for children (aged 0–17 years) or older adult family members may detract time and attention from patients undergoing BMT (Bevans & Sternberg, 2012; Simoneau et al., 2013). More intensive caregiver monitoring and psychosocial support may be needed for caregivers with multiple risk factors at pretransplantation screening. In addition, past research has demonstrated that, despite seemingly burdensome situations, caregivers of patients with cancer are still able to experience positive emotions (Li & Loke, 2013). However, it is unknown to what extent caregivers of allogeneic BMT recipients are able to experience positive emotions throughout the peritransplantation period.
The literature lacks an in-depth examination of the psychological and stress-related symptom experiences of caregivers transitioning from caring for patients as inpatients to caring for them in the ambulatory setting. Using a visual case-oriented approach, the authors aimed to describe the caregiver’s experience during an 8- to 12-week period after the patient’s allogeneic BMT. The authors will (a) describe trends in caregiver stress and psychoneurologic (PN) symptoms (anxiety, depression, fatigue, and sleep disturbance) 8–12 weeks post-transplantation and (b) describe contextual themes that explain trend patterns in PN symptoms. The authors also examined an exploratory aim focused on identifying whether caregivers of recipients of allogeneic BMT experience positive emotions throughout the peritransplantation period. Results from this study will be used to identify specific times when monitoring for caregiving-related stress and stress-related symptoms should be initiated and completed.
Theoretical Framework
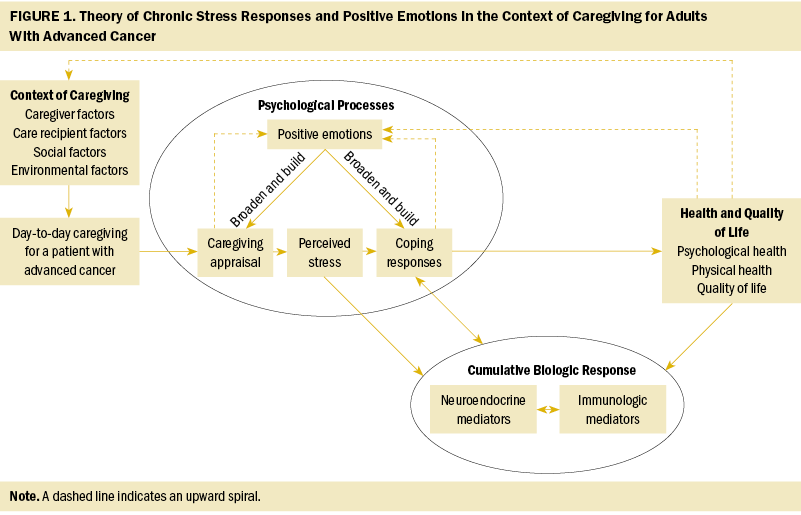
A synthesis (Tan, Santacroce, et al., 2022) (see Figure 1) of the psychoneuroimmunology-based paradigm (McCain et al., 2005; McCain & Smith, 1994) and the Broaden-and-Build Theory of Positive Emotions (Fredrickson, 2004, 2013) guided the primary study. The synthesized theory, “Theory of Chronic Stress Responses and Positive Emotions in the Context of Cancer Caregiving” (Tan, Santacroce, et al., 2022), informed the study design (semistructured interview guide) and analysis. This theory describes the complex psychological and physiologic processes that occur during chronically stressful caregiving, such as caring for an individual receiving an allogeneic BMT. When caregivers experience stressors, they subsequently appraise the stressor (benefit, threat, neutral appraisal), which then triggers the brain to produce interacting psychological (emotions) and physiologic (biologic changes and PN symptoms) changes. In this article, the authors focus on the psychological processes (self-reported positive and negative emotion), stress-related health outcomes (self-reported stress-related symptoms), and caregiving context (demographics and qualitative interviews); a forthcoming article will report biologic data from this study.
Methodology
A 12-week longitudinal case-oriented design was used to examine the stress and stress-related symptom experiences of 11 primary caregivers of patients undergoing an allogeneic BMT (Tan et al., 2021). The University of North Carolina (UNC) at Chapel Hill Institutional Review Board (IRB) and the Lineberger Comprehensive Cancer Center Protocol Review Committee provided ethical approval prior to study initiation. In this article, the authors report on the quantitative trend results and contextual details from qualitative data (monthly interviews and research field notes).
The authors used maximum variation sampling (Patton, 2002) to identify participants being treated at a BMT outpatient clinic at the UNC Lineberger Comprehensive Cancer Center in Chapel Hill. Participants were recruited using maximum variation sampling based on characteristics suggested by the literature to affect caregiving-related stress (i.e., age, gender, and employment). The authors collected data at the UNC Hospitals BMT outpatient clinic, intermediate-stepdown BMT unit, and home or temporary housing after discharge.
Eligible patients were identified from the BMT program schedules based on the following criteria: (a) scheduled to receive an allogeneic BMT in the next month, (b) aged 18 years or older, and (c) proficient in English to provide informed consent and authorization for abstraction of specific demographic and clinical data from their electronic health record. Eligible caregivers had to be (a) a designated caregiver of an eligible patient, (b) an adult aged 18 years or older, and (c) proficient in English well enough to provide informed consent and participate in study activities. Full recruitment procedures can be found in an associated protocol manuscript (Tan et al., 2021).
Survey Measures
Demographics: Caregiver demographic and socioeconomic items were collected using a modified version of the BRICS NINR (Biomedical Research Informatics Computing System National Institute of Nursing Research) Demographics survey (National Library of Medicine, 2016). Four additional context-related items were also included (relationship to patient, duration of relationship, multiple caregiving responsibilities, and shared caregiving).
Stress: Weekly self-reported perceived stress was collected using the National Institutes of Health (NIH) Toolbox Perceived Stress Fixed Form Age 18+, version 2.0 (Kupst et al., 2015). Participants were asked to rate their stress experiences in the past week using a five-point Likert-type scale ranging from 0 (never) to 4 (very often) (e.g., “How often have you been upset because of something that happened unexpectedly?”). A total score (range = 0–40) was calculated by summing item responses; higher scores indicate more perceived stress (Kupst et al., 2015). Reliability for the NIH Toolbox Perceived Stress Fixed Form Age 18+ is alpha = 0.91 (Kupst et al., 2015).
Stress-related symptoms: Stress-related symptoms were measured via the Patient-Reported Outcomes Measurement Information System–29 Profile (PROMIS-29 Profile). The PROMIS-29 Profile consists of the four-item short-form versions of eight domains. The following four domains were measured in this study: anxiety, depression, fatigue, and sleep disturbance (Bjorner et al., 2014; Flynn et al., 2015; Merriwether et al., 2017). Participants were asked to indicate how often they experienced a particular symptom in the past week on a scale from 1 (never) to 5 (always). Each domain score was calculated by averaging items; a higher average score indicates more symptoms experienced (Bjorner et al., 2014; Flynn et al., 2015; Merriwether et al., 2017). A single total stress-related symptom score was generated by summing the totals of each domain score (range = 0–16).
Semistructured Interview
The semistructured interviews explored caregiving-related experiences. Interviews were conducted every four weeks, audio recorded, and transcribed verbatim. Aliases were assigned to each participant for reporting purposes.
COVID-19–Related Changes
Because of the COVID-19 pandemic, in-person data collection stopped in March 2020 to reduce community spread. The three remaining participants were asked to continue in the study remotely. IRB approval was granted for the modification. No data were missing for the remaining three participants, monthly interviews were completed via telephone and audio recorded, and surveys were emailed or text messaged weekly.
Data Analysis
R statistical software was used to calculate descriptive statistics for each variable. For every continuous variable, the mean, standard deviation, median, and range were calculated. For each categorical variable, frequencies and percentages were calculated. The first author analyzed trends in person-reported data using a case-oriented visual analysis to describe trends during the 12 weeks post-transplantation. The first author graphically assembled weekly survey data along a days-since-transplantation timeline and visually searched for trend patterns (Docherty et al., 2016). The survey symptom data were plotted across time (days since transplantation) as a line chart of symptom scores for anxiety, depression, fatigue, and sleep disturbance; contextual information was included in text boxes along the graph (e.g., days since transplantation, clinical events, day of discharge).
Qualitative themes provided insights into experiences of caregiver stress and psychological states and influencing factors, as well as contextual grounding for each case. Monthly interviews were coded for patient events, such as patient transitions in care (e.g., discharge from hospital, medical emergencies), and caregiver events, such as accessing social support (e.g., talking with a pastor). From the list of coded events, a case summary was created for each participant that included information about other contexts of caregiving, such as shared caregiving responsibility, other caregiving responsibilities for children or other family, work status, and other life circumstances. Each participant’s trend graph was examined with the associated case summary and across similar trend types to identify common themes that may explain trend changes. Common trends were named by their visual appearance (e.g., U-shaped), and each case was organized into trend type; the resulting trend types and categorization were reviewed by another member of the research team.
Results
Sample Characteristics
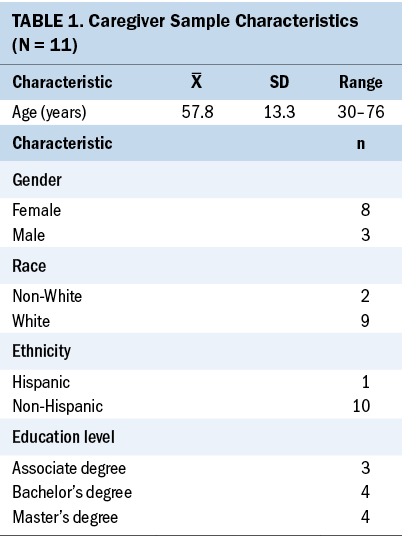
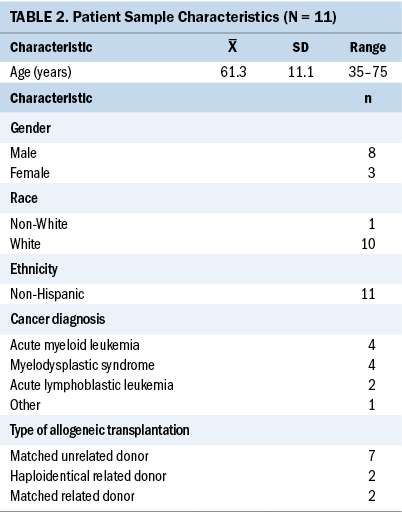
Caregivers’ ages ranged from 30 to 76 years (mean = 57.8 years, SD = 13.3); patients’ ages ranged from 35 to 75 years (mean = 61.3 years, SD = 11.1) (see Tables 1 and 2). Of the 11 patients, the majority were diagnosed with acute myeloid leukemia (36%) or myelodysplastic syndrome (36%). Most patients were male (73%), almost all were White (91%), and all were non-Hispanic. Of the 11 caregivers, all had at least some college, and most were female (73%), White (82%), and non-Hispanic (91%).
Caregiver Stress Response Trends Across 8–12 Weeks Post-Transplantation
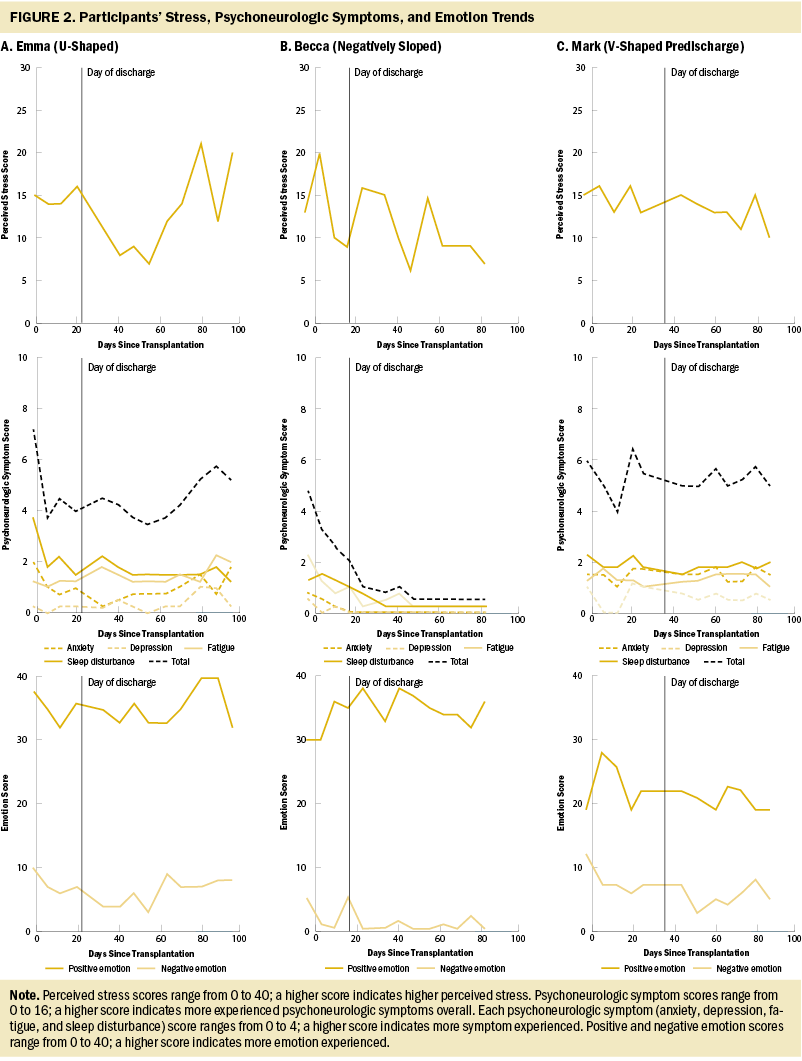
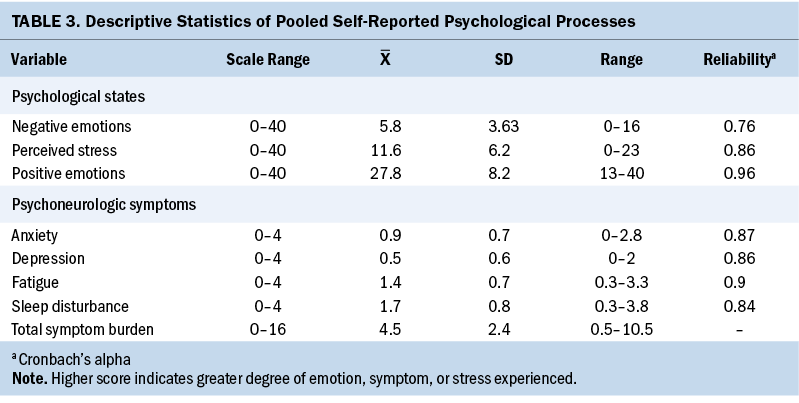
For each caregiver, scores were plotted against days since transplantation for perceived stress, PN symptoms, anxiety, depression, sleep disturbance, fatigue, and total symptom (see Figure 2). Notations were made with vertical lines on each graph indicating patient-related condition and environment changes, such as intensive care unit transfers, discharge from the hospital, and return to their own home. Mean score and standard deviation for each self-reported psychological process are reported in Table 3.
Perceived Stress
Caregivers’ perceived stress varied over time. Across time and cases, the mean perceived stress score was 11.6, which demonstrated an average low to moderate level of stress (range = 0–40). The highest perceived stress was typically experienced at the beginning of transplantation (mean = 12.55, SD = 6.11) and at the end of study follow-up at week 12 (mean = 12, SD = 5.86). During the week following discharge (week 6), caregivers had the lowest perceived stress (mean = 10, SD = 8.07). Baseline interviews with caregivers highlighted that caregivers felt stressed about “not knowing what to expect when [the patient] received transplant” and often had experiences during the admission process that were stressful.
Total Symptom Score
Symptoms varied across time for caregivers’ self-reported anxiety, depression, fatigue, and sleep disturbance. In caregivers who completed the full 12-week study, three main symptom trend line types were identified as follows: U-shaped, negatively sloped (downward over time), and V-shaped predischarge. In U-shaped trends (e.g., Harriet, Jessica, and Emma) (see Figure 2A), caregivers experienced their highest stress-related symptoms at the start of transplantation and at week 12. Caregivers with U-shaped trends had worsening symptoms after discharge. This may be because of the caregiver having additional demands caring for the patient related to returning home. For example, two caregivers began working full-time again (Harriet and Jessica), and one began caring for her children and the patient at home by week 12 (Emma). Of note, one participant who had a low symptom score on weeks 10 and 11 had gone on vacation with her family (Jessica).
Negatively sloped trend line patterns were identified in two caregivers; in these trends, the highest stress-related symptoms were experienced at the beginning of transplantation (e.g., Lily, Becca). These caregivers reported fewer stress-related symptoms as time went on. Lily and Becca often described that they were “getting used to a new normal” and were feeling more “confident in [their] ability to care for [the patient].” Of note, Becca’s symptom scores were low after discharge, and in interviews, she rarely described feeling stressed (see Figure 2B). During interviews after discharge, Becca often described the time with the patient as a “second honeymoon” and that she was “really enjoying [her] time with [the patient].”
V-shaped predischarge trends were identified in four caregivers. In V-shaped predischarge trends, stress-related symptoms were highest at the beginning of transplantation and right before discharge. After discharge, their stress-related symptoms were either stable (e.g., Mark, Gretchen) or decreased over time (e.g., Leanne, Amelia). In scenarios where the patient died or went to the intensive care unit emergently, caregivers had higher levels of stress-related symptoms before the event (e.g., Victor, Eli). In one case, Victor’s wife died suddenly, and Victor had steadily increasing stress-related symptoms up until the patient’s death. Caregivers’ symptom trends after transplantation mirrored how the patient was doing clinically. For example, caregivers described that when patients’ energy levels improved, it “lessen[ed] the workload” because the patient was able to be more independent.
Anxiety Symptom Trends
At baseline, caregivers stated they felt anxious about the unknown, including not knowing what would happen, worrying about the transplantation not working, worrying about their ability to provide care, and worrying about the patient dying. Three caregivers stated that the reality of caregiving came prior to transplantation; one stated that when the doctors were “talking about the graft versus host, and we had to sign the papers and everything. At the end was, ‘And this could end with infection, and this leads to death.’” Caregivers often mentioned feeling anxious that “nothing was moving up” when referring to the patient’s blood counts and reported having anxiety in the weeks prior to discharge. In some cases, caregivers said that they were anxious to “get the patient home” and were “worried about if something bad were to happen at home.”
Depression Symptom Trends
Nine caregivers whose patients were discharged to outpatient follow-up and home care described feeling more depressive symptoms while waiting for recovery of the patient’s blood counts. Often, caregivers described feeling depressed and impatient that “things were not kicking in.” For example, Lily stated that she was “starting to get a little depressed” because there was a possibility that her husband would have to stay at the hospital for another 28 days. Lily stated, “If there’s no engraftment, plan B is like kind of doing more chemotherapy backing almost to the beginning.” Mark, Eli, and Jessica similarly described that their depressive symptoms occurred when they perceived that the patient’s white blood cell count was not returning as they expected.
Sleep Disturbance and Fatigue Symptom Trends
Frequently, sleeping in the hospital was reported as negatively affecting the caregivers’ ability to sleep. Emma described her experience sleeping in the hospital as follows:
Terrible . . . ‘cause you’re in the hospital and when somebody’s comin’ in, you know, to check vitals or do this and that . . . but it would get to where you’re so tired you didn’t care. . . . You’d get used to people comin’ in and out.
When patients and their caregivers returned to their own homes, their sleep disturbance symptoms were typically lower. In addition, caregivers who described having anxiety or worry also tended to report during interviews and self-report that they had more sleep disturbance. For example, Gretchen reported experiencing problems with sleep during the 12 weeks after transplantation. She stated that she could fall asleep but would “wake up very early, and then [she] couldn’t go back to sleep” because she would “wake up worrying about things.” Eli often reported experiencing “bad dreams start up” and that it was “driving [him] nuts” because he would lay there and “try to rest and just have all these bad thoughts going through [his] head of what might happen.”
Discussion
Using a multimethod case-oriented approach, the authors described the stress-related symptom experiences of 11 caregivers of allogeneic BMT recipients during the 12 weeks after transplantation. The authors found the following three primary stress-related symptom trends in caregivers: U-shaped, negatively sloped, and V-shaped predischarge. Although caregivers had overall low to moderate stress-related symptom scores, they still described having depression, anxiety, sleep disturbance, and fatigue symptoms during interviews, reported elsewhere (Tan, Fredrickson, et al., 2022). The disconnect between qualitative descriptions and survey scores may be evidence that caregivers still experience stress-related symptoms but below the “clinical” threshold typically used in patients who are chronically ill. The results of this study identify specific time points when caregivers are likely to experience more stress-related symptoms and cases where positive emotions experientially buffered stress-related symptoms in caregivers with negatively sloped symptom trends. Specifically, stress-related symptoms were highest in all trend types before transplantation or just at the start of transplantation, which could indicate the need for earlier psychosocial or symptom management interventions for these caregivers. Some caregivers, specifically those with U-shaped trends, with higher symptoms at the end of follow-up, may benefit from additional support in comparison to caregivers whose symptoms subside over time. Interventions such as well-timed psychotherapy and psychoeducational interventions could benefit caregiver psychological health (for systematic reviews, see Ferrell & Wittenberg, 2017; Lee et al., 2021).
The current findings provide further support that caregivers of patients receiving BMT experience caregiving-related stress (Applebaum et al., 2016). In addition, some caregivers’ stress-related symptoms (anxiety, depression, sleep disturbance, and fatigue) showed increases over time after patient discharge. In three unique cases, caregivers returned to work full-time (n = 2) or resumed care of their young children (n = 1). In these cases, increasing stress-related symptoms were seen after discharge. Their qualitative data demonstrated that a return to normal life after discharge was accompanied by a return to normal life demands. In comparison to other caregivers in this study, these three caregivers were younger, with ages ranging from 30s to 40s. Evidence has demonstrated that younger adult caregivers are at unique risk for caregiving-related stress because of their competing life and role demands (Kent, 2020). In comparison to caregivers who were already retired or who did not have other caregiving responsibilities, caregivers who work full-time or have additional caregiving responsibilities for young children or parents may be at increased risk for caregiving-related stress.
The current findings also provide initial descriptive evidence for the “Theory of Chronic Stress Responses and Positive Emotions in the Context of Cancer Caregiving” (Tan, Santacroce, et al., 2022), in which the authors hypothesize that cumulative experiences of positive emotion can buffer the negative effects of stress. The authors found that in the current sample of caregivers, participants experienced positive emotions throughout the weeks post-transplantation, despite the high intensity of care provided and uncertainty surrounding allogeneic BMT.
Limitations
The current study focused on the experiences of primary caregivers of allogeneic BMT recipients; therefore, after the patient receiving a BMT died, they were unable to continue the study with bereaved caregivers. In addition, the authors note that the start of the COVID-19 pandemic may have added additional worry about caregiving because of risk of exposure for the patient. The current study was also limited by the lack of diversity of the sample.
Implications for Nursing and Future Research
Caregivers are essential to cancer care. Despite being heavily involved in the care of patients receiving allogeneic BMT, their health is not routinely followed during the patient’s cancer care journey. Caregivers are typically screened for distress at baseline as an assurance that the patient has someone available to provide “sufficient support.” Support services for caregivers often are not used even when they are available (Applebaum et al., 2014). The authors highlight that although some caregivers do better than others initially, certain situations may increase a caregiver’s need for support (e.g., emergent clinical changes like sepsis). The authors recommend that health clinicians assess caregivers beyond initial assessment before transplantation (Gemmill et al., 2011; Shaffer et al., 2019). Nurse clinicians are uniquely positioned to identify caregivers who are at risk and provide holistic care.
Few studies have longitudinally examined caregiving experiences. Additional exploration of the experiences of different types of caregivers caring for medically complex patients is needed, particularly as care continues to transition to earlier discharge to home and outpatient care. Research on younger adult caregivers and historically marginalized or excluded caregiving populations, such as marginalized sex and gender caregivers, is needed. The current study included one nonspousal caregiver, three younger adult caregivers, and two caregivers from an underrepresented racial or ethnic group.
The authors sought to identify time points during the peritransplantation period that may require targeted intervention. Based on the current findings, the authors identified that during the start of transplantation and when waiting for BMT engraftment before discharge are two times that caregivers may need additional support to manage their stress. Interventions may be necessary before transplantation begins because caregiving for the patient often begins before transplantation is even considered.

Conclusion
The current study’s findings provide a detailed description of self-reported post-transplantation symptoms and emotions of 11 caregivers of allogeneic BMT recipients. This study is an initial step to better understanding caregivers’ experiences and identifying times when they may be at increased risk for caregiving-related stress.
About the Authors
Kelly R. Tan, PhD, RN, is a postdoctoral fellow in the Lineberger Comprehensive Cancer Center and Barbara Fredrickson, PhD, is the Kenan Distinguished Professor in the Department of Psychology and Neuroscience, both at the University of North Carolina at Chapel Hill; Hudson Santos Jr., PhD, RN, is a professor and the Dolores J. Chambreau Endowed Chair in Nursing in the School of Nursing and Health Studies at the University of Miami in Florida; and William Wood, MD, is an associate professor of medicine in the Lineberger Comprehensive Cancer Center and in the School of Medicine, Todd A. Schwartz, DrPH, is a professor in the Department of Biostatistics and School of Nursing, and Deborah K. Mayer, PhD, RN, AOCN®, is the Frances Hill Fox Distinguished Professor Emeritus in the School of Nursing, all at the University of North Carolina at Chapel Hill. This research was supported by the National Institutes of Health National Institute of Nursing Research (F31NR018098) and the Rita and Alex Hillman Foundation. Tan was also supported by the National Institutes of Health National Cancer Institute (T32CA116339) during the preparation of this manuscript. Wood has received research funding from Genentech and Pfizer, consulted for Teladoc, and served in an advisory capacity for Koneksa Health. Tan, Fredrickson, Santos, Wood, and Mayer contributed to the conceptualization and design. Tan completed the data collection. Tan and Schwartz provided statistical support. Tan, Santos, and Mayer provided the analysis. Tan, Fredrickson, Wood, and Mayer contributed to the manuscript preparation. Tan can be reached at krtan@email.unc.edu, with copy to ONFEditor@ons.org. (Submitted October 2021. Accepted February 17, 2022.)
References
Applebaum, A.J., Bevans, M., Son, T., Evans, K., Hernandez, M., Giralt, S., & DuHamel, K. (2016). A scoping review of caregiver burden during allogeneic HSCT: Lessons learned and future directions. Bone Marrow Transplant, 51(11), 1416–1422. https://doi.org/10.1038/bmt.2016.164
Applebaum, A.J., Farran, C.J., Marziliano, A.M., Pasternak, A.R., & Breitbart, W. (2014). Preliminary study of themes of meaning and psychosocial service use among informal cancer caregivers. Palliative and Supportive Care, 12(2), 139–148. https://doi.org/10.1017/S1478951513000084
Atilla, E., Atilla, P.A., Toprak, S.K., & Demirer, T. (2017). A review of late complications of allogeneic hematopoietic stem cell transplantations. Clinical Transplantation, 31(10), e13062. https://doi.org/10.1111/ctr.13062
Bergeron, A. (2017). Late-onset noninfectious pulmonary complications after allogeneic hematopoietic stem cell transplantation. Clinics in Chest Medicine, 38(2), 249–262. https://doi.org/10.1016/j.ccm.2016.12.013
Bevans, M., & Sternberg, E.M. (2012). Caregiving burden, stress, and health effects among family caregivers of adult cancer patients. JAMA, 307(4), 398–403. https://doi.org/10.1001/jama.2012.29
Bjorner, J.B., Rose, M., Gandek, B., Stone, A.A., Junghaenel, D.U., & Ware, J.E., Jr. (2014). Method of administration of PROMIS scales did not significantly impact score level, reliability, or validity. Journal of Clinical Epidemiology, 67(1), 108–113. https://doi.org/10.1016/j.jclinepi.2013.07.016
Docherty, S.L., Vorderstrasse, A., Brandon, D., & Johnson, C. (2016). Visualization of multidimensional data in nursing science. Western Journal of Nursing Research, 39(1), 112–126. https://doi.org/10.1177/0193945916672448
Ferrell, B., & Wittenberg, E. (2017). A review of family caregiving intervention trials in oncology. CA: A Cancer Journal for Clinicians, 67(4), 318–325. https://doi.org/10.3322/caac.21396
Flynn, K.E., Dew, M.A., Lin, L., Fawzy, M., Graham, F.L., Hahn, E.A., . . . Weinfurt, K.P. (2015). Reliability and construct validity of PROMIS® measures for patients with heart failure who undergo heart transplant. Quality of Life Research, 24(11), 2591–2599. https://doi.org/10.1007/s11136-015-1010-y
Foster, L.W., McLellan, L.J., Rybicki, L.A., Dabney, J., Welsh, E., & Wolwell, B.J. (2005). Allogeneic BMT and patient eligibility based on psychosocial criteria: A survey of BMT professionals. Bone Marrow Transplant, 37(2), 223–228. https://doi.org/10.1038.sj.bmt.1705219
Fredrickson, B.L. (2004). The Broaden-and-Build Theory of Positive Emotions. Philosophical Transactions of the Royal Society of London. Series B: Biological Sciences, 359(1449), 1367–1378. https://doi.org/10.1098/rstb.2004.1512
Fredrickson, B.L. (2013). Positive emotions broaden and build. In P. Devine & A. Plant (Eds.), Advances in experimental social psychology (Vol. 47, pp. 1–53). Elsevier. https://doi.org/10.1016/b978-0-12-407236-7.00001-2
Gemmill, R., Cooke, L., Williams, A.C., & Grant, M. (2011). Informal caregivers of hematopoietic cell transplant patients: A review and recommendations for interventions and research. Cancer Nursing, 34(6), E13–E21. https://doi.org/10.1097/NCC.0b013e31820a592d
Kent, E.E. (2020). Time to recognize and support emerging adult caregivers in public health. American Journal of Public Health, 110(12), 1720–1721. https://doi.org/10.2105/AJPH.2020.305951
Kisch, A.M., Bergkvist, K., Alvariza, A., Årestedt, K., & Winterling, J. (2021). Family caregivers’ support needs during allo-HSCT—A longitudinal study. Supportive Care in Cancer, 29(6), 3347–3356. https://doi.org/10.1007/s00520-020-05853-8
Kupst, M.J., Butt, Z., Stoney, C.M., Griffith, J.W., Salsman, J.M., Folkman, S., & Cella, D. (2015). Assessment of stress and self-efficacy for the NIH Toolbox for Neurological and Behavioral Function. Anxiety, Stress, and Coping, 28(5), 531–544. https://doi.org/10.1080/10615806.2014.994204
Lee, J., Chen, H.C., Lee, J.X., & Klainin-Yobas, P. (2021). Effects of psychosocial interventions on psychological outcomes among caregivers of advanced cancer patients: A systematic review and meta-analysis. Supportive Care in Cancer, 29(12), 7237–7248.
Li, Q., & Loke, A.Y. (2013). The positive aspects of caregiving for cancer patients: A critical review of the literature and directions for future research. Psycho-Oncology, 22(11), 2399–2407.
Maffini, E., Festuccia, M., Brunello, L., Boccadoro, M., Giaccone, L., & Bruno, B. (2017). Neurologic complications after allogeneic hematopoietic stem cell transplantation. Biology of Blood and Marrow Transplant, 23(3), 388–397.
McCain, N.L., Gray D.P., Walter J.M., & Robins J. (2005). Implementing a comprehensive approach to the study of health dynamics using the psychoneuroimmunology paradigm. Advances in Nursing Science, 28(4), 320–332.
McCain, N.L., & Smith J.C. (1994). Stress and coping in the context of psychoneuroimmunology: A holistic framework for nursing practice and research. Archives of Psychiatric Nursing, 8(4), 221–227. https://doi.org/10.1016/0883-9417(94)90063-9
Merriwether, E.N., Rakel, B.A., Zimmerman, M.B., Dailey, D.L., Vance, C.G.T., Darghosian, L., . . . Sluka, K.A. (2017). Reliability and construct validity of the Patient-Reported Outcomes Measurement Information System (PROMIS) instruments in women with fibromyalgia. Pain Medicine, 18(8), 1485–1495. https://doi.org/10.1093/pm/pnw187
National Library of Medicine. (2016). Form: BRICS NINR Demographics. U.S. Department of Health and Human Services, National Institutes of Health. https://cde.nlm.nih.gov/formView?tinyId=XJo315r5M#general-details
Patton, M.Q. (2002). Qualitative research and evaluation methods (3rd ed.). Sage Publications.
Schulz, R., & Beach, S.R. (1999). Caregiving as a risk factor for mortality: The Caregiver Health Effects Study. JAMA, 282(23), 2215–2219. https://doi.org/10.1001/jama.282.23.2215
Shaffer, K.M., Benvengo, S., Zaleta, A.K., Levine, M., Bellantoni, C., Dannaoui, A., . . . Applebaum, A.J. (2019). Feasibility and acceptability of distress screening for family caregivers at a cancer surgery center. Oncology Nursing Forum, 46(2), 159–169. https://doi.org/10.1188/19.ONF.159-169
Simoneau, T.L., Mikulich-Gilbertson, S.K., Natvig, C., Kilbourn, K., Spradley, J., Grzywa-Cobb, R., . . . Laudenslager, M.L. (2013). Elevated peri-transplant distress in caregivers of allogeneic blood or marrow transplant patients. Psycho-Oncology, 22(9), 2064–2070. https://doi.org/10.1002/pon.3259
Stenberg, U., Ruland, C.M., & Miaskowski, C. (2010). Review of the literature on the effects of caring for a patient with cancer. Psycho-Oncology, 19(10), 1013–1025. https://doi.org/10.1002/pon.1670
Tan, K.R., Fredrickson, B.L., Santos, H., Wood, W.A., Schwartz, T.A., & Mayer, D.K. (2022). Psychological processing among caregivers of allogeneic bone marrow transplant recipients: Qualitative findings from a longitudinal study. Journal of Psychosocial Oncology. https://doi.org/10.1080/07347332.2022.2107467
Tan, K.R., Santacroce, S.J., Mayer, D.K., & Fredrickson, B.L. (2022). A literature review of linkages between positive emotions, stress, and health in caregivers of adults with advanced cancer [Manuscript in preparation].
Tan, K.R., Santacroce, S.J., Wood, W.A., Mayer, D.K., Santos, H., Mucha, P.J., . . . Fredrickson, B.L. (2021). Positive psychological states and stress responses in caregivers of adults receiving an allogeneic bone marrow transplant: A study protocol. Journal of Advanced Nursing, 77(4), 2073–2084. https://doi.org/10.1111/jan.14742
Trevino, K.M., Prigerson, H.G., & Maciejewski, P.K. (2017). Advanced cancer caregiving as a risk for major depressive episodes and generalized anxiety disorder. Psycho-Oncology, 27(1), 243–249. https://doi.org/10.1002/pon.4441
Von Ah, D., Spath, M., Nielsen, A., & Fife, B. (2016). The caregiver’s role across the bone marrow transplantation trajectory. Cancer Nursing, 39(1), E12–E19. https://doi.org/10.1097/NCC.0000000000000242
Williams, L.A. (2007). Whatever it takes: Informal caregiving dynamics in blood and marrow transplantation. Oncology Nursing Forum, 34(2), 379–387. https://doi.org/10.1188/07.ONF.379-387
Wulff-Burchfield, E.M., Jagasia, M., & Savani, B.N. (2013). Long-term follow-up of informal caregivers after allo-SCT: A systematic review. Bone Marrow Transplantation, 48(4), 469–473. https://doi.org/10.1038/bmt.2012.123




