Fertility Preservation in Patients With Cancer: Nurses’ Views, Experiences, and Perceptions of Benefits and Barriers
Objectives: To evaluate nurses’ views, experiences, and perceptions of the benefits and barriers to fertility preservation (FP) care for patients with cancer.
Sample & Setting: The sample consisted of 236 nurses who provided care before gonadotoxic treatment for people with cancer in three university hospitals in Istanbul, Turkey, from January to June 2018.
Methods & Variables: The data were collected using a participant information form and the Oncology FP Survey. The main research variables were nurses’ views, experiences, and perceptions of benefits and barriers to FP care. Data were evaluated using means, SDs, frequencies, and the Mann–Whitney U test.
Results: Patients and their families were informed about FP most of the time. This information was given by physicians about half the time and by nurses less than one-fourth of the time. Mean scores on the Oncology FP Survey were moderate and indicated challenges among nurses in self-confidence, self-awareness of personal limitations, and perceived barriers when providing effective FP care.
Implications for Nursing: Nurses face challenges in providing counseling about FP options for patients with cancer and their families. Increasing self-confidence, reducing personal limitations, and decreasing perceived barriers to FP care through appropriate training may improve nurses’ ability to provide FP counseling.
Jump to a section
Globally, about one million people aged 20–39 years are diagnosed with cancer every year (National Comprehensive Cancer Network [NCCN], 2022). The incidence of cancer in adolescents and young adults (AYAs) has increased since 2007; cancer has become the leading cause of disease-related (noninjury) death in AYAs (NCCN, 2022). Diagnosing cancer in AYAs can be challenging because of several factors. These include vague or nonspecific symptoms, low suspicion among healthcare providers, misdiagnosis or underdiagnosis, and psychosocial factors like coping with cancer at a young age or overcoming the stigma associated with cancer (Miller et al., 2020; NCCN, 2022). With the development of early diagnosis technologies and treatments in the field of oncology, long-term survival rates in children and AYAs with cancer have increased to more than 80% (Janssen et al., 2021). Although long-term treatment and follow-up are recommended for disease management in children and AYAs with cancer, the issue of fertility preservation (FP) in survivorship may be overlooked (Campbell & Woodard, 2020; Crespi et al., 2021). However, these patients may experience significant loss of fertility because of symptoms of disease; gonadotoxic side effects of endocrine treatment, surgery, chemotherapy, or radiation therapy; and psychosocial symptoms and side effects (Halpern et al., 2020). Infertility and childbearing difficulties remain major concerns for all AYA cancer survivors who are of reproductive age, regardless of diagnosis, prognosis, or treatment (NCCN, 2022). Although the awareness among healthcare providers of treatment-related damage to fertility is improving, many AYAs lack understanding about gonadotoxic treatments and their reproductive impacts (Fidler et al., 2019).
The field of oncofertility developed because of concerns about the future reproductive health, sexual life, and fertility potential of cancer survivors. Oncofertility is important for patients with cancer because it addresses the potential impact of cancer treatment on reproductive health and fertility. Cancer treatments can damage or destroy reproductive organs and cells, leading to infertility or reduced fertility. Oncofertility offers FP options to patients with cancer, allowing them to preserve their fertility before receiving potentially fertility-damaging treatments, providing hope and a sense of control in the face of a cancer diagnosis, and improving quality of life and mental health outcomes (Crespi et al., 2021; Fuchs et al., 2016; Grabowski et al., 2017; Yi & Syrjala, 2023). Therefore, the demand for FP care among children and AYAs with cancer has increased considerably.
It is a professional duty and an ethical responsibility for oncologists, nurses, and other health professionals involved in the treatment and care of children and AYAs with cancer to consider and advise on FP because these patients are expected to have positive outcomes from the treatment and may want to have children in the future. Within an interprofessional team approach for FP, nurses play a key role in providing medical care, patient education, counseling, and guidance (Crespi et al., 2021; Satılmış et al., 2021). Nurses can educate patients about the impacts of cancer treatment on fertility and inform them of available FP options. They can also help patients make informed decisions about FP by discussing the risks, benefits, and costs of each option. By incorporating oncofertility into cancer care, nurses can assist patients in achieving improved quality of life and long-term well-being, and they can offer patients greater opportunities to start or expand their families after cancer treatment. Although the necessity of safe and strong patient communication is stated in guidelines about FP from the American Society of Clinical Oncology and other medical organizations (Loren et al., 2013; Oktay et al., 2018; Practice Committee of the American Society for Reproductive Medicine, 2013), it is known that nurses take a limited role and responsibility in counseling (Kelvin, 2016; Parker et al., 2019). One of the gaps in the role of nurses in oncofertility is the lack of standardized training and education about options for FP. Many nurses may not be familiar with the latest FP techniques or may not have received training on how to provide oncofertility counseling to patients with cancer. This can result in limited patient education and support, and it may lead to missed opportunities for FP (Crespi et al., 2021; Xiao et al., 2023). FP treatment approaches and counseling are critically important for individuals diagnosed with cancer in childhood, adolescence, and young adulthood. This study was planned to evaluate nurses’ views, experiences, and perceptions of the benefits and barriers to providing FP care to patients with cancer.
Methods and Variables
Sample and Setting
The research population consisted of 1,656 nurses working in three university hospitals in Istanbul, Turkey, in 2018, and the minimum sample size for this population was found to be 234 nurses, with a confidence interval of 95%, a margin of error of 5%, and a population incidence of 77% (i.e., the rate of nurses who rarely or never discuss FP) (Keim-Malpass et al., 2018). The final research sample consisted of 236 nurses who met the following inclusion criteria: (a) being a nurse caring for children and AYAs with cancer before receiving gonadotoxic treatment, (b) being available and working actively in the hospital during the research period, and (c) agreeing to participate in the study. Nurses were excluded if they met any of the following criteria: (a) not encountering patients with cancer in their routine work, (b) being on staff leave for any reason, (c) refusing to participate in the study, or (d) filling out the questionnaires incompletely.
Data Collection Tools
The research data were collected using a researcher-designed participant information form (PIF) and the Oncology FP Survey (OFPS) (Grabowski et al., 2017).
PIF: This form was prepared by the researchers to gather information about the nurses’ sociodemographic characteristics (age, gender, marital status, and education level) and professional characteristics (department in the hospital, duration of time working as a nurse, and when they were involved in the care of patients with cancer, such as at diagnosis or before or after chemotherapy, radiation therapy, or surgery). In addition, the PIF included questions about the views and experiences of nurses regarding FP. In these questions, FP counseling was defined as the process of informing patients and their families about the possibilities and options for FP, raising their awareness about FP, answering their questions, and directing them to relevant care providers for procedures. The PIF evaluated nurses’ views with six statements prepared by the researchers according to a literature review (Campbell & Woodard, 2020; Grabowski et al., 2017; Halpern et al., 2020). The statements were about the effects of cancer on fertility, the possibilities for the preservation of reproductive functions, concerns of patients about future fertility problems, concerns of patients’ families about future fertility problems, the necessity of FP counseling by the physicians before the treatment, and the necessity of FP counseling by the nurses. The nurses were asked to rate their agreement with each of these statements on a four-point continuum from “strongly agree” to “strongly disagree.” Each statement was considered separately and evaluated independently. Eight questions on the PIF evaluated nurses’ experiences regarding the availability of FP counseling in the clinic, health professionals who are involved in FP counseling, questions received about FP from patients, previous training about FP, methods known for FP, and directing patients for FP.
OFPS: Developed by Grabowski et al. (2017), this five-point, 15-item Likert-type scale was used to evaluate nurses’ perceptions of benefits and barriers to providing FP care for patients with cancer. A Turkish version of the OFPS with 12 items was developed and validated by Satılmış et al. (2021), with a Cronbach’s alpha reliability coefficient of 0.71. The total score ranges from 12 to 60 points. The subdimensions of this scale are self-confidence (3–15 points), self-awareness (4–20 points), and barriers (5–25 points). Self-awareness refers to awareness of personal limitations. Higher scores indicate greater perception of challenges to discussing FP with patients. Lower scores indicate that the nurses feel more able to discuss FP approaches with patients (Satılmış et al., 2021).
Data Collection
After obtaining institutional approval from the hospitals for the implementation of this study, the researchers contacted the potentially eligible nurses in cooperation with the managers of the institutions’ nursing services from January to June 2018. The nurses were informed about the aim of the study by the researchers, and those who agreed to participate filled out the data collection forms themselves. Each survey took an average of 15 minutes to complete.
Ethics Approval
Ethics committee permission was obtained from the Marmara University Medical Faculty Clinical Research Ethics Committee (Issue No. 09.2017.603), and institutional permission was obtained from the nursing services directorates of the hospitals where the research was conducted. The research was conducted in accordance with research and publication ethics as specified in the Declaration of Helsinki (World Medical Association, 2013). An informed consent form was obtained from each nurse after the researchers explained the purpose of the study.
Data Analysis
IBM SPSS Statistics, version 22.0, was used to analyze the data. Quantitative data were evaluated using means, SDs, and frequencies. The Kolmogorov–Smirnov test was used to examine the normality distribution of the total OFPS scores. Because the data were not normally distributed, the Mann– Whitney U test was used to compare OFPS scores between nurses who did and did not provide FP counseling. Statistical significance was set at p < 0.05.
Results
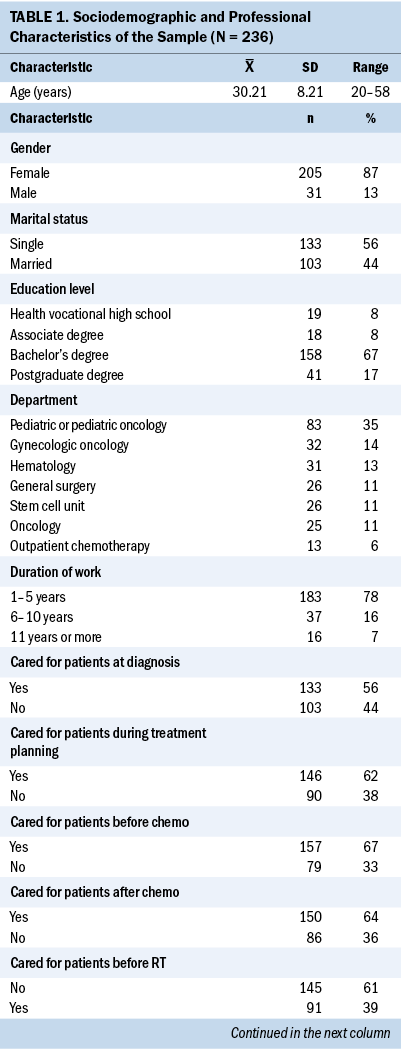
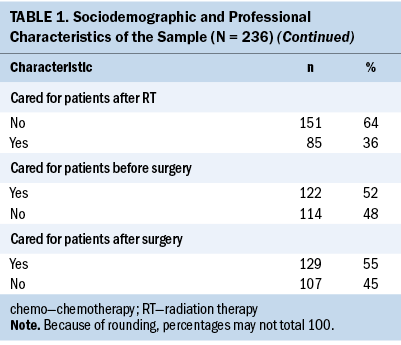
A total of 236 nurses providing care for people with cancer before they received gonadotoxic treatment participated in the study from three university hospitals in Istanbul, Turkey. The mean age of the nurses was 30.21 years (SD = 8.21, range = 20–58), and 87% (n = 205) were women. Of the participants, 35% (n = 83) worked in the pediatric or pediatric oncology service, had practiced an average of 7.72 years (SD = 8.41), and had worked with patients with cancer for an average of 4.08 years (SD = 5.12). Regarding when they were involved in caring for patients with cancer, 56% (n = 133) stated that they provided care during the diagnosis procedures, 62% (n = 146) at the treatment planning stage, 67% (n = 157) before chemotherapy, 64% (n = 150) after chemotherapy, 39% (n = 91) before radiation therapy, 36% (n = 85) after radiation therapy, 52% (n = 122) before surgery, and 55% (n = 129) after surgery. Table 1 presents the sociodemographic and professional characteristics of the nurses.
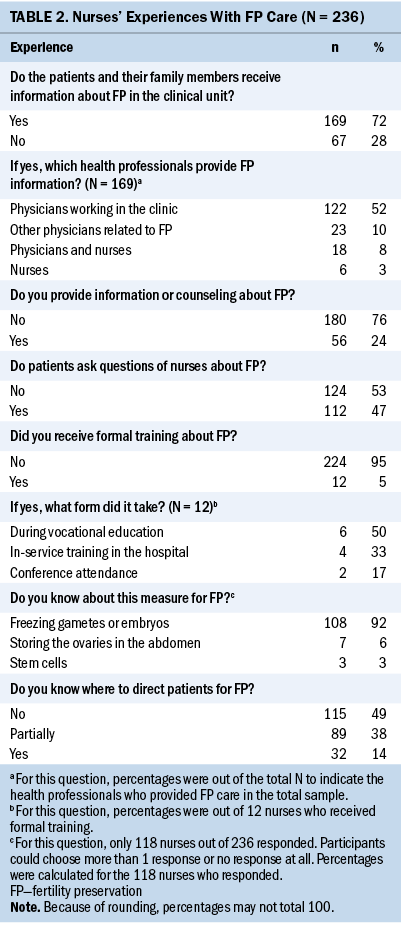
Nurses reported that patients and their families were informed about the FP measures in 72% of the clinics where they worked, and this information was given by the physician on 52% of those units. Of the nurses, 24% (n = 56) reported that they provided counseling about FP, and 5% (n = 12) stated that they received training for FP (in-service training, vocational education, or conference attendance). Detailed data about the experiences of nurses concerning FP practices on the units are presented in Table 2.
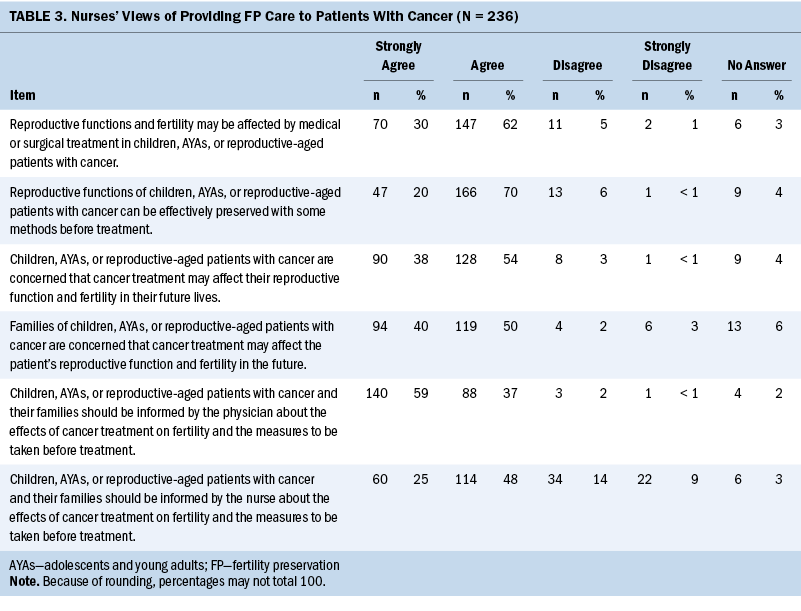
Most nurses stated that they agreed (n = 147, 62%) or strongly agreed (n = 70, 30%) with the statement that reproductive functions and fertility may be affected because of medical or surgical treatment for cancer in children, AYAs, and people of reproductive age. About the possibility of the preservation of reproductive functions in those patients, 70% of nurses (n = 166) agreed that reproductive functions can be effectively preserved with some methods before treatment. They were aware of concerns of patients (agree: n = 128, 54%; strongly agree: n = 90, 38%) and their families (agree: n = 119, 50%; strongly agree: n = 94, 40%) about future fertility problems. Although 59% (n = 140) of nurses strongly agreed with the idea that patients and their families should be informed by the physician about the effects of cancer treatment on fertility and the precautions to be taken before treatment, 48% (n = 114) agreed with the statement that nurses should provide this information. Table 3 shows the distribution of nurses’ views on FP in patients with cancer.
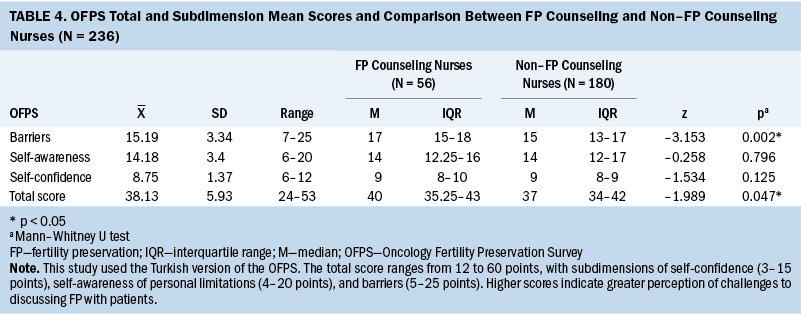
The mean OFPS total score was 38.13 (SD = 5.93, range = 24–53). The mean subdimension scores were 8.75 (SD = 1.37, range = 6–12) for self-confidence, 14.18 (SD = 3.4, range = 6–20) for self-awareness of personal limitations, and 15.19 (SD = 3.34, range = 7–25) for barriers. In the barriers subdimension, the scores of the nurses who provided counseling (median = 17, interquartile range [IQR] = 15–18) were higher than the scores for those who did not provide FP counseling (median = 15; IQR = 13–17), and this difference was found to be statistically significant (p = 0.002). The median total OFPS scores were significantly higher (p = 0.047) among nurses who reported providing FP counseling in their practice (median = 40, IQR = 35.25–43) than the scores for those who did not (median = 37, IQR = 34–42). The total and subdimension scores on the OFPS and their comparison between nurses who did and did not report providing FP counseling are given in Table 4.
Discussion
In this study, nurses reported that patients and their families were informed about FP measures in 72% (n = 169) of the clinics where they worked. Of note, only 3% (n = 6) of the health professionals responsible for delivering this information were nurses; most nurses (n = 122, 52%) reported that physicians delivered it. However, the American Society of Clinical Oncology and various medical organizations extend the responsibility of FP education to other health professionals involved in the daily management of patients receiving oncology care (Kelvin, 2016; Loren et al., 2013; Parker et al., 2019). No literature has been identified pertaining to all nurses working in the prechemotherapy, diagnostic, and presurgical phases of care. Consequently, these research findings can be interpreted in the context of studies involving only oncology nurses. In their study conducted with pediatric oncology nurses, advanced practice nurses, and physicians, Fuchs et al. (2016) found that 93.6% of physicians, 74.6% of advanced practice nurses, and 48.2% of pediatric oncology nurses discussed FP approaches with patients. Similarly, regarding pretreatment discussion about FP, Overbeek et al. (2014) reported that 97% of physicians, Murray et al. (2016) stated that 93.6% of physicians, and Terenziani et al. (2013) reported that 64 of 68 pediatric oncology physicians informed patients about FP approaches (Nassau et al., 2020). It has been reported that nurses provide less information and counseling than physicians, although this may be related to team dynamics. Studies found that 48.2% of pediatric oncology nurses (Overbeek et al., 2014), 73%–77% of oncology nurses and RNs (Keim-Malpass et al., 2018), and 51.9% of nurses (Murray et al., 2016) discussed with and informed patients about FP approaches. As a result of this research, it was found that physicians and nurses discussed FP approaches with patients to a limited extent and provided little information. However, more than half of the nurses (n = 169, 72%) in the current study stated that patients received information about FP. Research and anecdotal evidence suggest that among patients with cancer, awareness and interest in FP have increased (Campbell & Woodard, 2020; Crespi et al., 2021; Keim-Malpass et al., 2018). In the literature, no rate was found regarding patients’ desire to receive information about FP, which may vary widely depending on factors including the patient’s age, type of cancer, cultural factors, and the healthcare setting (Becze, 2018; Loren et al., 2013).
In the current study, only 5% (n = 12) of the nurses reported that they had received formal training related to FP approaches. A parallel study conducted by Parker et al. (2019) involving oncology nurses indicated that a substantially higher percentage (36.8%) of the nurses had received training about FP approaches. In the current study, it was observed that the nurses knew only three methods of FP, and almost half of the nurses knew about the method of gamete/embryo freezing (n = 108, 46%). The literature states that nurses have a lack of knowledge about FP approaches (Crespi et al., 2021; Fuchs et al., 2016; Keim-Malpass et al., 2018). In a study assessing the knowledge of oncology nurses regarding FP methods, it was found that the proportion of nurses who correctly answered true–false questions on a 13-item validated knowledge tool ranged from 56.8% to 94.6% (Parker et al., 2019). In a study conducted with Dutch oncology nurses (N = 421), 31% stated that they had sufficient information about fertility problems, and 28% stated that they had limited or no information (Krouwel et al., 2017). The nurses who participated in the current study stated that they did not know where to direct patients. In contrast, Fuchs et al. (2016) found that 81.1% of the nurses in their study knew about FP guidelines and technologies. The current study found that the percentage of nurses involved in FP counseling for patients with cancer was very low compared to oncology nurses in previous studies. These results reveal the educational needs of all nurses, not just oncology nurses, who care for patients with cancer, from diagnosis to care before gonadotoxic treatment.
In this study, most nurses agreed that reproductive functions and fertility in children and AYAs with cancer may be affected because of treatment, and most agreed that this could cause concern for patients and their families. The results of this research indicate that nurses’ perspectives on FP and counseling, particularly for newly diagnosed patients, children, or AYAs with cancer, align with existing literature (Crespi et al., 2021; Keim-Malpass et al., 2018; Krouwel et al., 2017; Murray et al., 2016; Parker et al., 2019). The most notable finding in the current study is that a significant proportion of nurses expressed a lack of responsibility for educating patients about FP approaches. Nurses felt that physicians were responsible (strongly agree: n = 140, 59%; agree: n = 88, 37%) for educating patients about FP. Contrary to this research, Krouwel et al. (2017) and Parker et al. (2019) reported that oncology nurses are optimistic about their role in helping to discuss FP approaches with patients and their families because they feel responsible for doing so. They argued that FP counseling roles will develop when nurses’ knowledge levels on this subject increase (Krouwel et al., 2017; Parker et al., 2019; Takeuchi et al., 2018). Nurses’ attitudes about their responsibilities and roles in FP counseling may be affected by factors including lack of information, perceived barriers, and the attitudes of physicians and other health professionals. Importance should be given to raising the awareness of the entire team in addition to raising each nurse’s individual awareness of the FP counseling role.
The nurses participating in the present study had a moderate average total score on the OFPS and reported some challenges in self-confidence, self-awareness of personal limitations, and perceived barriers in counseling for FP. A study conducted by Parker et al. (2019) among oncology nurses indicated moderate scores in self-confidence (mean = 9.5, SD = 3.39), self-awareness (mean = 20.44, SD = 2.93), and total OFPS (mean = 49.58, SD = 7.43). In addition, oncology nurses received moderate to higher scores in the barriers subdimension of the OFPS compared to nurses in the current study. Similarly, a study conducted by Takeuchi et al. (2018) assessing the impact of a training program about FP approaches for nonphysician healthcare providers found that nurses had low mean scores in terms of confidence, knowledge, and counseling skills. Common barriers for nurses regarding FP counseling were lack of knowledge, poor patient prognosis, and insufficient time. In addition, lack of access to fertility specialists, financial obligations, patient character, organizational complexity, role confusion, and personal limitations around religious or moral values related to patients or assisted reproductive technology were determined to be influential factors (Crespi et al., 2021; Grabowski et al., 2017; Keim-Malpass et al., 2018; Krouwel et al., 2017).
A striking conclusion from the current study is that the total OFPS scores of the nurses who reported providing FP counseling were significantly higher than the scores of the nurses who did not. Counseling nurses may be aware of FP approaches and the importance of educating patients about FP, but the lack of time and resources allocated for counseling may create obstacles. Nurses who provide FP counseling may experience more difficulties and may be more aware of barriers around providing this counseling than nurses who do not. In their systematic review, Crespi et al. (2021) reported that nurses’ lack of resources and lack of time, as well as role confusion, constitute obstacles for counseling.
Limitations
The research was conducted at three university hospitals in Istanbul where FP services are intensively provided. The generalizability of this research may be limited because of the inability of researchers to access all nurses working on the relevant units, such as nurses who worked at night, were on leave, or were otherwise unavailable. In addition, all data were self-reported by the participants, so they may be subject to bias.
Implications for Nursing
Nurses play a vital role in caring for patients with cancer, including those who may be at risk for fertility loss because of cancer treatments. It is crucial for nurses to be knowledgeable about FP options and to have open discussions with patients about their reproductive health. However, based on the available literature and the results of this study, nurses may experience various barriers to discussing FP with patients with cancer. Lack of confidence and personal limitations might be explained by the limited information and experience around FP provided during professional education and in-service training at the hospitals. Increasing nurses’ self-confidence, reducing personal limitations, and decreasing perceived barriers through appropriate training will improve nurses’ ability to provide FP counseling. Nurses need to be aware of these potential barriers and should be supported in improving their knowledge and skills in this area. To improve the perceptions of the counseling role of nurses, developing unit protocols and establishing team meetings with other health professionals may be useful in clarifying the expectations and responsibilities related to FP counseling. Additional research is recommended to determine nurses’ needs, improve their FP counseling skills, and develop and evaluate the effectiveness of FP training programs for nurses.

Conclusion
The nurses participating in the study reported some challenges in providing education and counseling on FP options to patients with cancer and their families. These challenges were mainly related to factors like nurses’ self-confidence, personal limitations, and perceived barriers. Many factors, such as the lack of information, personal beliefs about the need for and efficacy of FP methods, attitudes about the responsibilities and roles of nurses in FP counseling, and lack of communication skills in discussing FP with patients and their families, may also affect nurses’ willingness to provide FP counseling.
About the Authors
İlkay Güngör Satılmış, PhD, RN, is an associate professor in the Department of Women’s Health and Gynecologic Nursing in the Florence Nightingale Faculty of Nursing at Istanbul University– Cerrahpaşa; Dilek Coşkuner Potur, PhD, RN, is an associate professor in the Obstetrics and Gynecology Nursing Department in the Faculty of Health Sciences at Marmara University in Istanbul; Meltem Mecdi Kaydırak, PhD, RN, is an associate professor in the Department of Women’s Health and Gynecologic Nursing in the Florence Nightingale Faculty of Nursing at Istanbul University– Cerrahpaşa; and Semiha Akın Eroğlu, PhD, RN, is a professor in the Department of Internal Medicine Nursing in the Hamidiye Faculty of Nursing at the University of Health Sciences in Istanbul, all in Turkey. No financial relationships to disclose. Potur and Kaydırak completed the data collection. Kaydırak provided statistical support. Potur provided the analysis. Kaydırak, Satılmış, and Potur contributed to the manuscript preparation. All authors contributed to the conceptualization and design. Satılmış can be reached at ilkay.gungorsatilmis@iuc.edu.tr, with copy to ONFEditor@ons.org. (Submitted August 2022. Accepted September 20, 2023.)
References
Becze, E. (2018). What competencies are required for oncology nurse generalists? ONS Voice. https://voice.ons.org/news-and-views/what-competencies-are-required-for…
Campbell, S.B., & Woodard, T.L. (2020). An update on fertility preservation strategies for women with cancer. Gynecologic Oncology, 156(1), 3–5. https://doi.org/10.1016/j.ygyno.2019.11.001
Crespi, C., Adams, L., Gray, T.F., & Azizoddin, D.R. (2021). An integrative review of the role of nurses in fertility preservation for adolescents and young adults with cancer. Oncology Nursing Forum, 48(5), 491–505. https://doi.org/10.1188/21.ONF.491-505
Fidler, M.M., Frobisher, C., Hawkins, M.M., & Nathan, P.C. (2019). Challenges and opportunities in the care of survivors of adolescent and young adult cancers. Pediatric Blood and Cancer, 66(6), e27668. https://doi.org/10.1002/pbc.27668
Fuchs, A., Kashanian, J.A., Clayman, M.L., Gosiengfiao, Y., Lockart, B., Woodruff, T.K., & Brannigan, R.E. (2016). Pediatric oncology providers’ attitudes and practice patterns regarding fertility preservation in adolescent male cancer patients. Journal of Pediatric Hematology/Oncology, 38(2), 118–122. https://doi.org/10.1097/MPH.0000000000000488
Grabowski, M.C., Spitzer, D.A., Stutzman, S.E., & Olson, D.W.M. (2017). Development of an instrument to examine nursing attitudes toward fertility preservation in oncology. Oncology Nursing Forum, 44(4), 497–502. https://doi.org/10.1188/17.ONF.497-502
Halpern, J.A., Das, A., Faw, C.A., & Brannigan, R.E. (2020). Oncofertility in adult and pediatric populations: Options and barriers. Translational Andrology and Urology, 9(Suppl. 2), S227–S238. https://doi.org/10.21037/tau.2019.09.27
Janssen, S.H.M., van der Graaf, W.T.A., van der meer, D.J., Manten-Horst, E., & Husson, O. (2021). Adolescent and young adult (AYA) cancer survivorship practices: An overview. Cancers, 13(19), 4847. https://doi.org/10.3390/cancers13194847
Keim-Malpass, J., Fitzhugh, H.S., Smith, L.P., Smith, R.P., Erickson, J., Douvas, M.G., . . . Duska, L. (2018). What is the role of the oncology nurse in fertility preservation counseling and education for young patients? Journal of Cancer Education, 33(6), 1301–1305. https://doi.org/10.1007/s13187-017-1247-y
Kelvin, J.F. (2016). Fertility preservation before cancer treatment: Options, strategies, and resources. Clinical Journal of Oncology Nursing, 20(1), 44–51. https://doi.org/10.1188/16.CJON.44-51
Krouwel, E.M., Nicolai, M.P.J., van Steijn–van Tol, A.Q.M.J., Putter, H., Osanto, S., Pelger, R.C.M., & Elzevier, H.W. (2017). Fertility preservation counseling in Dutch oncology practice: Are nurses ready to assist physicians? European Journal of Cancer Care, 26(6), e12614. https://doi.org/10.1111/ecc.12614
Loren, A.W., Mangu, P.B., Beck, L.N., Brennan, L., Magdalinski, A.J., Partridge, A.H., . . . Oktay, K. (2013). Fertility preservation for patients with cancer: American Society of Clinical Oncology clinical practice guideline update. Journal of Clinical Oncology, 31(19), 2500–2510. https://doi.org/10.1200/JCO.2013.49.2678
Miller, K.D., Fidler-Benaoudia, M., Keegan, T.H., Hipp, H.S., Jemal, A., & Siegel, R.L. (2020). Cancer statistics for adolescents and young adults, 2020. CA: A Cancer Journal for Clinicians, 70(6), 443–459. https://doi.org/10.3322/caac.21637
Murray, A.N., Chrisler, J.C., & Robbins, M.L. (2016). Adolescents and young adults with cancer: Oncology nurses report attitudes and barriers to discussing fertility preservation. Clinical Journal of Oncology Nursing, 20(4), 93–100. https://doi.org/10.1188/16.CJON.E93-E99
Nassau, D.E., Chu, K.Y., Blachman-Braun, R., Castellan, M., & Ramasamy, R. (2020). The pediatric patient and future fertility: Optimizing long-term male reproductive health outcomes. Fertility and Sterility, 113(3), 489–499. https://doi.org/10.1016/j.fertnstert.2020.01.003
National Comprehensive Cancer Network. (2022). NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines®): Adolescent and young adult oncology [v.1.2022]. https://www.nccn.org/professionals/physician_gls/pdf/aya.pdf
Oktay, K., Harvey, B.E., Partridge, A.H., Quinn, G.P., Reinecke, J., Taylor, H.S., . . . Loren, A.W. (2018). Fertility preservation in patients with cancer: ASCO clinical practice guideline update. Journal of Clinical Oncology, 36(19), 1994–2001.
Overbeek, A., van den Berg, M., Louwé, L., Wendel, E., ter Kuile, M., Kaspers, G., . . . Hilders, C. (2014). Practice, attitude and knowledge of Dutch paediatric oncologists regarding female fertility. Netherlands Journal of Medicine, 72(5), 264–270.
Parker, L., Nelson, M., Marcus, J., & McKenzie, L. (2019). Knowledge gaps, barriers, and facilitators to fertility preservation counseling among oncology nurses managing the care of newly diagnosed cancer patients [Doctor of Nursing Practice project, Georgia State University]. ScholarWorks @ Georgia State University. https://doi.org/10.57709/14482294
Practice Committee of the American Society for Reproductive Medicine. (2013). Fertility preservation in patients undergoing gonadotoxic therapy or gonadectomy: A committee opinion. Fertility and Sterility, 100(5), 1214–1223. https://doi.org/10.1016/j.fertnstert.2013.08.012
Satılmış, İ.G., Kaydırak, M.M., Akın, S., & Potur, D.C. (2021). Onkolojide Fertilitenin Korunması Ölçeği’nin Türkçe’ye uyarlanması: Geçerlik ve güvenirlik çalışması [Turkish adaptation of the Oncology Fertility Preservation Survey: A validity and reliability study]. Ankara Sağlık Bilimleri Dergisi, 10(2), 1–12. https://doi.org/10.46971/ausbid.890220
Takeuchi, E., Kato, M., Miyata, K., Suzuki, N., Shimizu, C., Okada, H., . . . Miyoshi, Y. (2018). The effects of an educational program for non-physician health care providers regarding fertility preservation. Supportive Care in Cancer, 26(10), 3447–3452. https://doi.org/10.1007/s00520-018-4217-y
Terenziani, M., Spinelli, M., Jankovic, M., Bardi, E., Hjorth, L., Haupt, R., . . . Byrne, J. (2013). Practices of pediatric oncology and hematology providers regarding fertility issues: A European survey. Pediatric Blood and Cancer, 61(11), 2054–2058. https://doi.org/10.1002/pbc.25163
Xiao, Y., Li, J., Lei, J., Li, X., Hu, M., Zhao, J., . . . Chen, O. (2023). Qualitative study of the fertility information support experiences of young breast cancer patients. European Journal of Oncology Nursing, 62, 102275. https://doi.org/10.1016/j.ejon.2023.102275
World Medical Association. (2013). WMA Declaration of Helsinki: Ethical principles for medical research involving human subjects. https://www.wma.net/policies-post/wma-declaration-of-helsinki-ethical-p…
Yi, C.J., & Syrjala, K.L. (2023). Overview of cancer survivorship in adolescents and young adults. In M. Yushak (Ed.), UpToDate. https://www.uptodate.com/contents/overview-of-cancer-survivorship-in-ad…

