Health Literacy: Exploring Nursing Challenges to Providing Support and Understanding
Background: As patient advocates, oncology nurses must attend to varying levels of health literacy among patients and families. However, little is known about nurses’ experiences and comfort with health literacy assessment and providing health literacy support.
Objectives: The purpose of this study is to explore nurse communication and patient health literacy.
Methods: A cross-sectional survey design (N = 74) was used to explore nurse communication challenges with low-literacy patients and to measure nurses’ frequency of assisting with patient literacy needs, perceived degree of difficulty communicating with low-literacy populations, and perceived comfort with health literacy support.
Findings: A majority of the nurses reported communication challenges with patients who spoke English as a second language. Oncology nurses did not identify patient communication behaviors that indicated low health literacy. Nurses were least comfortable identifying low-literacy patients and assessing a patient’s health literacy level. More experienced nurses reported more difficulty with low-literacy populations than less experienced nurses. Providing health literacy support to patients should be a core nursing skill.
Jump to a section
Patients with cancer represent a population with unique health literacy needs. The complexity of managing cancer combined with rapidly growing treatment options requires patients to make difficult decisions that can be physically and emotionally distressing (Amalraj, Starkweather, Nguyen, & Naeim, 2009; Ballard & Hill, 2016). This may affect a patient’s ability to access healthcare services, use preventive measures, follow medical advice, and receive treatment to meet his or her needs (Amalraj et al., 2009; Ballard & Hill, 2016). Health literacy is multifaceted and includes cognitive, social, and navigational skills such as language proficiency, reading and numeracy skills, understanding risk and probability, and the communication skills needed to interact with healthcare providers (Eadie, 2014; Lambert & Keogh, 2014). Limited health literacy has been linked with poor disease management, nonadherence to treatment recommendations, increased hospitalizations, and patient or caregiver medication errors (Christensen, 2016; Eadie, 2014). In addition, when health literacy needs are not met, patients report a lack of understanding about their disease, have difficulty making decisions, have fears of dying, experience unexpected symptoms, and may rely on other sources to fill gaps in understanding (Cohen, Jenkins, Holston, & Carlson, 2013).
Health literacy is defined as an individual’s ability to receive, acquire, understand, and use information (Smedley, Stith, & Nelson, 2003). Nurses should assume all patients and families have low health literacy and difficulty understanding (e.g., assume a universal precautions approach), and, as such, the U.S. National Library of Medicine recommends a sixth-grade reading level for patient education (Ballard & Hill, 2016; Protheroe & Rowlands, 2013; U.S. National Library of Medicine, n.d.). As patient advocates, nurses must attend to varying levels of health literacy among patients and families (Eadie, 2014; Protheroe & Rowlands, 2013). Figure 1 provides an overview of nursing standards and national reports emphasizing health literacy as an essential component of quality nursing care. Effective methods for giving patients understandable and retainable information about their care have been identified as a priority for oncology nursing research (Cox, Arber, Gallagher, MacKenzie, & Ream, 2017). Although addressing health literacy has been nationally recognized as a healthcare imperative, little is known about nurses’ experiences and comfort with health literacy assessment and providing health literacy support.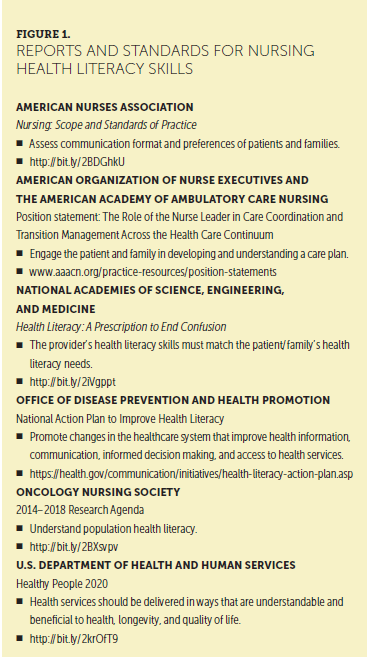
Background
Many tools can be used to ensure that nurses communicate effectively and meet patient health literacy needs. These tools include the teach-back method, speaking slowly, repeating important points, and encouraging patients to ask questions (Badaczewski et al., 2017; Ballard & Hill, 2016; Christensen, 2016; Cohen et al., 2013; Macabasco-O’Connell & Fry-Bowers, 2011; Nouri & Rudd, 2015; Protheroe & Rowlands, 2013). In addition, written information shared in clinical settings can be misunderstood by individuals with limited health literacy, making it important to supplement oral communication with plain-language materials to ensure patient understanding (Protheroe & Rowlands, 2013). To ensure patient understanding and address any health literacy barriers, nurses need to allow adequate time to determine the patient’s level of understanding, consider the patient’s emotional reaction to information, and involve family and other healthcare team members who can provide support (Cohen et al., 2013).
Established tools exist to assist nurses in assessing and communicating with patients who have limited health literacy, including the use of screening questions and plain-language communication strategies. However, current research highlights a major gap in nurses’ knowledge and assessment of patient health literacy (Christensen, 2016; Dickens, Lambert, Cromwell, & Piano, 2013). Nurses often overestimate a patient’s health literacy level, report using their gut feelings to assess patient health literacy skills, or rely on a patient’s educational level to assess health literacy (Dickens et al., 2013; Macabasco-O’Connell & Fry-Bowers, 2011; Parnell, 2014). Using a gut feeling to assess patient health literacy is problematic, and a patient’s level of health literacy cannot be assumed by simply looking at a patient’s age, level of education, or minority status. Nurses also tend to assume that patients fully understand information when they nod “yes” when asked questions, assume that using plain language is insulting to well-educated individuals, and assume that a patient will speak up when he or she has problems understanding (Parnell, 2014). Nurses often do not consider that health literacy extends beyond the use of medical terminology, including the impact of health literacy on patient understanding, access to care, and adherence (Macabasco-O’Connell & Fry-Bowers, 2011).
The current study builds on a cancer education program grant from the National Cancer Institute to develop a national nurse communication training program for oncology nurses called COMFORT (COMFORT Communication Project, 2016). COMFORT is an acronym that stands for the seven basic principles of palliative care communication (C—communication, O—orientation and options, M—mindful communication, F—family caregivers, O—openings, R—relating, and T—team). One of the seven modules of COMFORT teaches nurses how to assess patient health literacy needs (Christensen, 2016). Based on interactions with nurses who attended a two-day COMFORT communication skills-building course and in the process of developing curriculum material, the need to assess nurses’ health literacy skills became apparent. Nurses have not routinely received health literacy education as part of their professional preparation (Dickens et al., 2013). Therefore, this study explored nurse communication and health literacy skills by measuring the frequency of nurse experiences with patient and family health literacy needs, perceived degree of difficulty with low-literacy patient populations, and perceived comfort with health literacy support.
Methods
An open-ended survey was distributed to nurses attending a COMFORT communication training course for oncology nurses. COMFORT programs are delivered in a two-day train-the-trainer format, providing participants with a comprehensive curriculum about communication. Nurses voluntarily completed the survey prior to receiving course content. The survey was determined to be exempt under the institutional review board at the supporting institution.
Instrument
The research team developed a 30-item survey to measure nurse communication and health literacy support. The survey was developed based on the authors’ prior published research on nurse communication and with the U.S. Department of Health and Human Services ([USDHHS], 2010) National Action Plan to Improve Health Literacy as a framework. Additional items were included to learn more about communication in the context of low health literacy. First, to explore nurse communication and patient health literacy, two open-ended questions afforded nurses an opportunity to share a communication challenge that they experienced with a patient who had low health literacy. Nurses were asked to detail the experience and what could have been done to better support a patient with low health literacy.
Next, nurses were presented with five low health literacy patient populations (USDHHS, 2010). For each population, nurses were asked to indicate the frequency of providing care (rarely, sometimes, often, or always) and to rate the degree of communication difficulty on a scale of 0 (not difficult) to 10 (very difficult). To further assess frequency of providing health literacy support, nurses were asked to report how often they help patients and families to read hospital materials and complete hospital forms. Finally, participants were asked to report perceived comfort with health literacy support. Ratings were provided on a scale of 1 (very comfortable) to 10 (very uncomfortable). To address face validity, the survey was reviewed by experts in nursing, health literacy, and survey development.
Data Analysis
A research team member transcribed all written, open-ended responses. Three members of the research team reviewed responses. Inductive content analysis was used in two phases: open coding to create categories and abstraction of data into categories (Elo & Kynas, 2008). Identification of categories emerged from strong representation throughout responses and was verified by coding and frequency calculation. Demographics and survey items were summarized using IBM SPSS Statistics, version 25.0, to produce descriptive statistics (frequency and mean scores).
Results
A total of 74 oncology nurses were surveyed, with 70 completing the open-ended items of the survey. The majority of oncology nurses surveyed were clinical nurses (n = 46), had 3–10 years of nursing experience (n = 25), and worked in the Western United States (n = 42). They came from a variety of settings, most commonly hospital (n = 50) and outpatient/ambulatory care (n = 14). Table 1 summarizes the demographic information.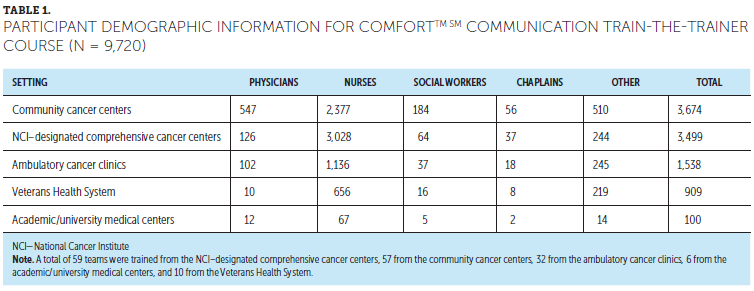
A majority of oncology nurses reported communication challenges with patients who spoke English as a second language, followed by patients with less than a high school education and ethnic minorities. Figure 2 provides examples of oncology nurse communication challenges with low-literacy patients. In addition to the five categories of low health literacy patient populations identified in the literature, three additional coding categories emerged from the analysis. Health literacy challenges were identified related to religious beliefs and patient emotional/psychological issues. In addition, some nurses described communication challenges but did not identify the low health literacy population.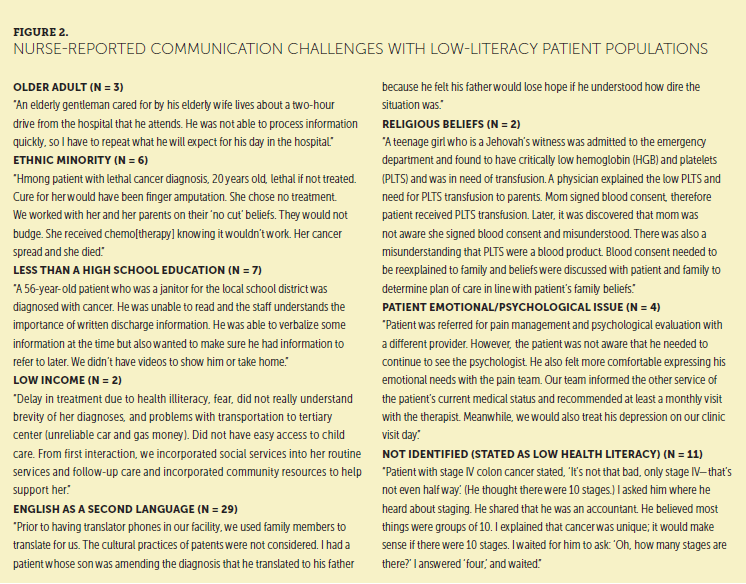
Overall, 36 oncology nurses (49%) did not identify patient communication behaviors that indicated low health literacy. Among the most commonly cited reasons for recognizing patient low health literacy was when patients asked nurses to interpret the physician’s use of jargon (n = 14, 19%), the patient’s nonverbal behavior indicated misunderstanding or complexity (n = 12, 17%), and when nurses realized that they had used a medical term that the patient did not understand (n = 5, 7%). Asking too many questions (n = 4, 6%) and asking few questions (n = 3, 3%) were less commonly identified as patient behaviors indicative of low health literacy.
Nurse recommendations for assessing patient health literacy included the following statements:
“Providers need to understand cultural beliefs and norms in order to prepare to reach patients fully.”
“Repeat explanations/options in a different way from a different provider to see if another perspective/attempt could be more successful.”
“Make sure the staff is well trained in watching for verbal and nonverbal cues. . . . Be very cognizant of using medical speech. Patients have a scary new diagnosis and adding jargon that they don’t understand makes the moment scarier and more foreign.”
“The phone interpreter is very helpful but sometimes being an outsider creates trust issues with the patient who already has great fear and anxiety with the situation. If there was an actual person in the institution who spoke the language, teaching/communication is easier.”
Use of a translator (n = 25, 36%) and asking the patient what they understand (n = 21, 30%) were most common, with nurses also reporting that it was important to talk slow and use repetition (n = 14, 20%). The teach-back method was also recognized as a useful tool (n = 15, 22%).
Nurses reported that the low health literacy populations that they encountered most frequently were older adults (n = 42, 57%), patients with low income levels (n = 41, 55%), ethnic minorities (n = 35, 48%), and patients who do not speak English as a first language (n = 34, 46%). A majority of oncology nurses (n = 38, 51%) reported that they sometimes help patients and family caregivers read and complete hospital materials and forms. On a scale ranging from 1 (very prepared) to 10 (not prepared), nurses reported feeling generally prepared to work with patients and families who have low health literacy (mean = 4.53) and that their institution was prepared to provide care to low-literacy patients (mean = 4.62).
Regarding communication difficulties, on a scale ranging from 0 (not difficult) to 10 (very difficult), patients who do not speak English as a first language (mean = 7.53), ethnic minorities (mean = 6.32), and older adults (mean = 5.69) were considered the most difficult patient populations to communicate with. Table 2 provides a summary of the perceived degree of difficulty with low literacy patient populations by years of nursing experience. Nurses with more experience (11–20 years, mean = 7.53; 21–30 years, mean = 7.18; 31–43 years, mean = 7.5) reported more difficulty with patients who do not speak English as a first language compared to less experienced nurses (0–2 years, mean = 6.33). Overall, nurses with the most experience (31–43 years) reported the highest degree of difficulty with low-literacy patient populations.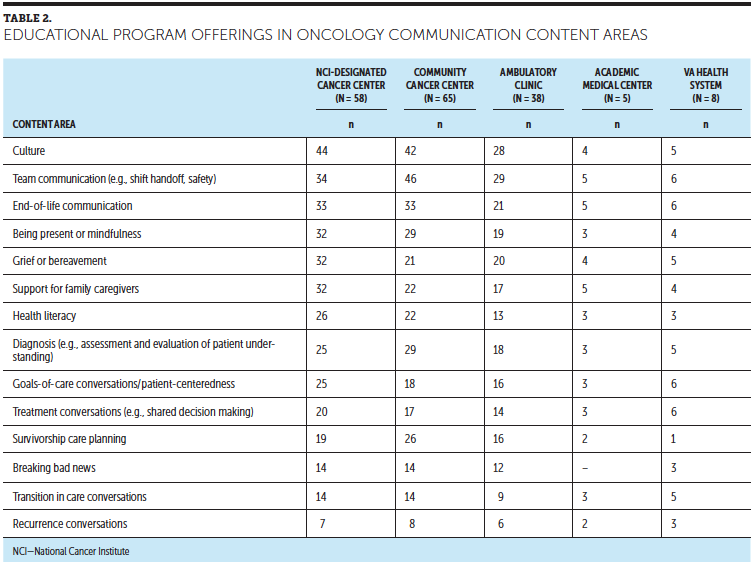
Regarding perceived comfort with health literacy support on a scale ranging from 1 (very comfortable) to 10 (very uncomfortable), across all years of experience, nurses were least comfortable identifying low-literacy patients (mean = 4.54) and assessing a patient’s health literacy level (mean = 4.64). Nurses were most comfortable working with a medically trained interpreter (mean = 2.72). Overall, nurses reported general comfort with health literacy support with all mean scores lower than 5 on the 10-point scale, with the exception of less experienced nurses who reported less comfort with assessing a patient’s health literacy level (mean = 5.67). Table 3 summarizes nurses’ perceived comfort with health literacy support by years of experience.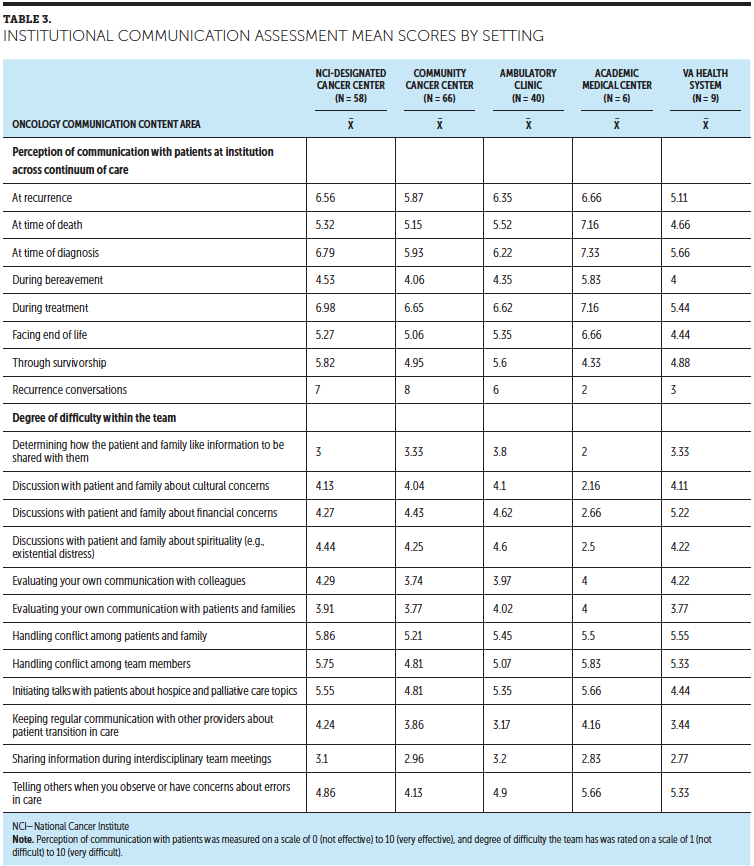
Overall, nurses perceived a degree of difficulty with low-literacy patient populations but reported feeling comfortable with health literacy support. Nurses with less experience (less than 10 years) report more comfort than experienced nurses (greater than 10 years) with the following health literacy support: identifying a patient or family member who has low health literacy, teaching a goal to help a patient/family member improve self-care, and acknowledging cultural differences.
Discussion
A nurse’s ability to assess patient understanding and adapt to communication challenges related to health literacy needs is essential in the provision of quality nursing care. In the current study, nurse communication challenges with low health literacy populations were primarily with patients who spoke English as a second language. This is consistent with a growing culturally diverse patient population, making it crucial to train nurses to attend to cultural communication issues and health literacy to improve the quality of care and patient outcomes (Lie, Carter-Pokras, Braun, & Coleman, 2012). Patients from cultural minority groups may be more at risk for low health literacy levels because of communication challenges caused by language barriers and experience of bias (Singleton & Krause, 2010). Implicit racial/ethnic bias, defined as negative attitudes toward minority groups, exists among healthcare professionals, affecting patient–provider interaction, treatment decision and adherence, and patient health outcomes (Hall et al., 2015). For example, nurses in a study by Galinato, Montie, Shuman, Patak, and Titler (2016) reported having trouble explaining how to use the call light to patients with limited English proficiency, and perceived that these patients may not be getting the same quality of care as native English-speaking patients. Language barriers between nurses and patients can have an effect on nursing care and may be more problematic for nurses than for physicians (Haider et al., 2015).
Knowing about a patient’s language and culture is crucial for knowing how health literate may be in a given situation (Singleton & Krause, 2010). Even when interpreters are used or when patients with English as a second language appear to have adequate English-speaking/listening skills, cultural issues can still affect the quality of nurse–patient communication (Singleton & Krause, 2010). Prior research has shown that nurses consider language differences as barriers to quality care and perceive translators as useful; however, nurses can also serve as gatekeepers to the use of a translator (Bernard et al., 2005). Future research is needed to develop strategies for nurses to work with translators when assessing patient health literacy (Hyatt et al., 2017). Findings from this study illustrate that nurses see language differences as a literacy barrier but do not demonstrate understanding of patient behaviors indicating low health literacy.
Although nurses identified checking for patient understanding as a recommended health literacy skill to meet communication challenges, they also reported being least comfortable with assessing and identifying patient health literacy levels. These findings suggest that nurses have knowledge regarding the importance of providing health literacy support but may not have the necessary communication skills to include screening questions as part of their clinical routine or provide patient education at the recommended sixth-grade level. It has been noted that clinical use of health literacy tools requires continuous communication training and support (Welch, VanGeest, & Caskey, 2011).
Nurses with more experience reported the highest degree of difficulty with low-literacy patients. Although having a BSN degree, having more experience, and the nursing practice environment are indicators of clinical expertise (McHugh & Lake, 2010), research on nursing education has shown that senior baccalaureate nursing students have higher levels of principled thinking than more experienced nurses (Ham, 2004). When the effect of years of experience on moral reasoning was assessed, it was found that as nurses gained more experience, their use of principled thinking decreased. Because health literacy support requires principled thinking for nurses to adjust their communication based on the patient’s health literacy needs, findings from this study suggest that nurses with more experience have difficulty with low-literacy patients as a result of limited exposure to health literacy concepts and curriculum (McCleary-Jones, 2016).
The current study supports the need for ongoing communication skills building for nurses in the area of health literacy, particularly in the area of assessment. Oncology nurses had little recognition of specific patient behaviors that signified low health literacy, suggesting that they may not be knowledgeable of low health literacy indicators. Research has shown that patients who have low health literacy avoid asking questions; show signs of nervousness, confusion, and frustration; fill out forms incompletely or incorrectly; and may make excuses when asked to read printed materials (Egbert & Nanna, 2009). Teaching health literacy assessment is essential to ensure that a patient’s health literacy level is not assumed based on his or her level of education, age, or minority status.
Findings from this study guide future curriculum content for health literacy education for nurses. First, indicators of low literacy should be taught as tools for identifying literacy needs so that nurses can provide interventions for specific populations at risk for low health literacy (Nouri & Rudd, 2015). Second, questions for assessing literacy should be broadened beyond asking for patient understanding. Nurses in this study reported that the physician’s use of medical jargon was the most common reason for identifying patient literacy needs. Asking patients if anything needs to be clarified after a physician visit is an important strategy that can be included in training curricula. When doing this, using open-ended questions that promote patient responses (e.g., “What questions do you have?”) as opposed to closed-ended questions (e.g., “Do you have any questions?”) is important.
Figure 3 provides a summary of recommended health literacy tools for nurses. The teach-back method is a communication strategy endorsed by the American Medical Association and Joint Commission, and research has shown that use of the teach-back method improves patient-centered communication and increases participation with healthcare providers (Badaczewski et al., 2017). The Plain Language Planner for Palliative Care© (PLP) is a tool for communicating about oncology, palliative care, and cancer treatment side effects in plain language at the sixth-grade level (COMFORT Communication Project, 2016), and use of the PLP has been shown to reduce the use of jargon for nurses (Wittenberg, Goldsmith, Ferrell, & Platt, 2015). Future research is needed to address nurses’ efficacy of these tools, as well as determine the impact on patient outcomes.
Limitations
Although the sample for this study reflected nurses with varying levels of experience in varied settings, it was nevertheless a convenience sample consisting of nurses already attending the COMFORT communication course. The sample was relatively small, consisting of 74 nurses completing the survey, making it difficult to generalize to the entire population. The study could have been strengthened by collecting information on participants’ level of nursing education. Finally, self-reported data were collected for this study. This method may evoke social desirability bias, or the tendency of participants to provide responses that portray themselves in a positive light.
Conclusion
Communication challenges related to low literacy by the patient are commonly experienced by nurses, confirming a need for continued education for health literacy skills for nurses at every level (Macabasco-O’Connell & Fry-Bowers, 2011). By taking a universal precautions approach and assuming that every patient needs health literacy support, nurses can positively affect patient outcomes. Nurse communication training is needed to ensure that nurses conduct a health literacy assessment for every patient and use plain language strategies to provide health literacy support.
About the Author(s)
Elaine Wittenberg, PhD, is an associate professor in the Department of Communication Studies at California State University in Los Angeles; Betty Ferrell, PhD, RN, MA, FAAN, FPCN, CHPN®, is a professor in the Division of Nursing Research and Education at the City of Hope Comprehensive Cancer Center in Duarte, CA; Elisa Kanter, BA, is a student in the Department of Health and Strategic Communication Studies at Chapman University in Orange, CA; and Haley Buller, MSHSC, is a research supervisor in the Division of Nursing Research and Education at the City of Hope Comprehensive Cancer Center. The authors take full responsibility for this content. This study was funded, in part, by the National Cancer Institute of the National Institutes of Health (award number R25CA174627). The article has been reviewed by independent peer reviewers to ensure that it is objective and free from bias. Wittenberg can be reached at elaine.wittenberg2@calstatela.edu, with copy to CJONEditor@ons.org. (Submitted April 2017. Accepted May 26, 2017.)
References
Amalraj, S., Starkweather, C., Nguyen, C., & Naeim, A. (2009). Health literacy, communication, and treatment decision-making in older cancer patients. Oncology, 23, 369–375.
Badaczewski, A., Bauman, L.J., Blank, A.E., Dreyer, B., Abrams, M.A., Stein, R.E., . . . Sharif, I. (2017). Relationship between teach-back and patient-centered communication in primary care pediatric encounters. Patient Education and Counseling, 100, 1345–1352. https://doi.org/10.1016/j.pec.2017.02.022
Ballard, D., & Hill, J. (2016). The nurse’s role in health literacy of patients with cancer. Clinical Journal of Oncology Nursing, 20, 232–234. https://doi.org/10.1188/16.CJON.232-234
Bernard, A.C., Summers, A., Thomas, J., Ray, M., Rockich, A., Barnes, S., . . . Kearney, P. (2005). Novel Spanish translators for acute care nurses and physicians: Usefulness and effect on practitioners’ stress. American Journal of Critical Care, 14, 545–550.
Chew, L.D., Bradley, K.A., & Boyko, E.J. (2004). Brief questions to identify patients with inadequate health literacy. Family Medicine, 36, 588–594.
Christensen, D. (2016). The impact of health literacy on palliative care outcomes. Journal of Hospice and Palliative Nursing, 18, 544–549. https://doi.org/10.1097/NJH.0000000000000292
Cohen, M.Z., Jenkins, D., Holston, E.C., & Carlson, E.D. (2013). Understanding health literacy in patients receiving hematopoietic stem cell transplantation. Oncology Nursing Forum, 40, 508–515. https://doi.org/10.1188/13.ONF.508-515
COMFORT Communication Project. (2016). Retrieved from www.communicatecomfort.com
Cornett, S. (2009). Assessing and addressing health literacy. Online Journal of Issues in Nursing, 14(3). https://doi.org/10.3912/OJIN.Vol14No03Man02
Cox, A., Arber, A., Gallagher, A., MacKenzie, M., & Ream, E. (2017). Establishing priorities for oncology nursing research: Nurse and patient collaboration. Oncology Nursing Forum, 44, 192–203. https://doi.org/10.1188/17.ONF.192-203
Dickens, C., Lambert, B.L., Cromwell, T., & Piano, M.R. (2013). Nurse overestimation of patients’ health literacy. Journal of Health Communication, 18(Suppl. 1), 62–69. https://doi.org/10.1080/10810730.2013.825670
Eadie, C. (2014). Health literacy: A conceptual review. MEDSURG Nursing, 23, 1–13.
Egbert N., & Nanna K.M. (2009). Health literacy: Challenges and strategies. Online Journal of Issues in Nursing, 14(3). https://doi.org/10.3912/OJIN.Vol14No03Man01
Elo, S., & Kynas, H. (2008). The qualitative content analysis process. Journal of Advanced Nursing, 62, 107–115. https://doi.org/10.1111/j.1365-2648.2007.04569.x
Galinato, J., Montie, M., Shuman, C., Patak, L., & Titler, M. (2016). Perspectives of nurses on patients with limited English proficiency and their call light use. Global Qualitative Nursing Research, 3, 1–9. https://doi.org/10.1177/2333393616637764
Haider, A.H., Schneider, E.B., Sriram, N., Scott, V.K., Swoboda, S.M., Zogg, C.K., . . . Cooper, L.A. (2015). Unconscious race and class biases among registered nurses: Vignette-based study using implicit association testing. Journal of the American College of Surgeons, 220, 1077–1086. https://doi.org/10.1016/j.jamcollsurg.2015.01.065
Hall, W.J., Chapman, M.V., Lee, K.M., Merino, Y.M., Thomas, T.W., Payne, B.K., . . . Coyne-Beasley, T. (2015). Implicit racial/ethnic bias among health care professionals and its influence on health care outcomes: A systematic review. American Journal of Public Health, 105(12), e60–e76. https://doi.org/10.2105/AJPH.2015.302903
Ham, K. (2004). Principled thinking: A comparison of nursing students and experienced nurses. Journal of Continuing Education in Nursing, 35(2), 66–73.
Hyatt, A., Lipson-Smith, R., Schofield, P., Gough, K., Sze, M., Aldridge, L., . . . Butow, P. (2017). Communication challenges experienced by migrants with cancer: A comparison of migrant and English-speaking Australian-born cancer patients. Health Expectations, 20, 886–895. https://doi.org/10.1111/hex.12529
Lambert, V., & Keogh, D. (2014). Health literacy and its importance for effective communication. Part 1. Nursing Children and Young People, 26(3), 31–37. https://doi.org/10.7748/ncyp2014.04.26.3.31.e387
Lie, D., Carter-Pokras, O., Braun, B., & Coleman, C. (2012). What do health literacy and cultural competence have in common? Calling for a collaborative professional pedagogy. Journal of Health Communication, 17(Suppl. 3), 13–22. https://doi.org/10.1080/10810730.2012.712625
Macabasco-O’Connell, A., & Fry-Bowers, E.K. (2011). Knowledge and perceptions of health literacy among nursing professionals. Journal of Health Communication, 16(Suppl. 3), 295–307. https://doi.org/10.1080/10810730.2011.604389
McCleary-Jones, V. (2016). A systematic review of the literature on health literacy in nursing education. Nurse Educator, 41, 93–97. doi:10.1097/NNE.0000000000000204
McHugh, M.D., & Lake, E.T. (2010). Understanding clinical expertise: Nurse education, experience, and the hospital context. Research in Nursing and Health, 33, 276–287. https://doi.org/10.1002/nur.20388
Morris, N.S., MacLean, C.D., Chew, L.D., Littenberg, B. (2006). The Single Item Literacy Screener: Evaluation of a brief instrument to identify limited reading ability. BMC Family Practice, 7, 21.
Nouri, S.S., & Rudd, R.E. (2015). Health literacy in the “oral exchange”: An important element of patient–provider communication. Patient Education and Counseling, 98, 565–571. https://doi.org/10.1016/j.pec.2014.12.002
Parnell, T.A. (2014). Health literacy in nursing: Providing person-centered care. New York, NY: Springer.
Protheroe, J., & Rowlands, G. (2013). Matching clinical information with levels of patient health literacy. Nursing Management, 20(3), 20–21.
Singleton, K., & Krause, E.M. (2010). Understanding cultural and linguistic barriers to health literacy. Kentucky Nurse, 58(4), 4, 6–9.
Smedley, B.D., Stith, A.Y., & Nelson, A.R. (Eds.). (2003). Unequal treatment: Confronting racial and ethnic disparities in health care. Washington, DC: National Academies Press.
Speros, C.I. (2011). Promoting health literacy: A nursing imperative. Nursing Clinics of North America, 46, 321–333. https://doi.org/10.1016/j.cnur.2011.05.007
U.S. Department of Health and Human Services. (2010). National action plan to improve health literacy. Washington, DC: Author. Retrieved from http://bit.ly/2arGr0M
U.S. National Library of Medicine. (n.d.). How to write easy-to-read health materials. Retrieved from http://www.nlm.nih.gov/medlineplus/etr.html
Welch, V.L., VanGeest, J.B., & Caskey, R. (2011). Time, costs, and clinical utilization of screening for health literacy: A case study using the Newest Vital Sign (NVS) instrument. Journal of the American Board of Family Medicine, 24, 281–289. https://doi.org/10.3122/jabfm.2011.03.100212
Wittenberg, E., Goldsmith, J., Ferrell, B., & Platt, C.S. (2015). Enhancing communication related to symptom management through plain language. Journal of Pain and Symptom Management, 50, 707–711. https://doi.org/10.1016/j.jpainsymman.2015.06.007


