Mediterranean Diet: Outcomes From an Education Session Among Patients With Cancer and Nursing Staff
Background: Strong evidence supports the benefits of the Mediterranean diet, but little is reported among patients and nurses regarding knowledge about the diet and its health benefits.
Objectives: A pre-/post-test practice initiative was implemented to identify level of knowledge about the Mediterranean diet in patients with cancer and nursing staff and to provide education about the diet’s health benefits.
Methods: A 17-item survey was developed to assess knowledge and willingness to try or recommend the Mediterranean diet, current practices, and general nutrition knowledge. A 10-minute education session was provided to patients and nursing staff. Descriptive statistics were used.
Findings: The majority of patients reported eating from one to four servings of fruits and vegetables daily. For patients and nursing staff, post–education session scores demonstrated increased knowledge, willingness to try the diet, and perceived effectiveness of the diet.
Jump to a section
The neutropenic diet is characterized by the restriction of fresh fruits and vegetables (particularly those that come from the ground); elimination of raw or undercooked meats, fish, and eggs; and avoidance of dairy products made from unpasteurized milk. These foods are restricted because of a greater risk of foodborne illness (Wolfe et al., 2018). Patients undergoing hematopoietic stem cell transplantations or those receiving high doses of chemotherapy were previously directed to follow a neutropenic diet to decrease the incidence of foodborne infections while neutropenic or immunocompromised. Concerns about the neutropenic diet include limited and weak evidence that show beneficial effects, lack of standardized guidelines, and food restrictions for a patient population that is already at risk for malnutrition (Foster, 2014; Lassiter & Schneider, 2015; Sonbol et al., 2015; Wolfe et al., 2018). Malnutrition is strongly correlated with poorer quality of life and clinical outcomes. Therefore, adequate nutrition is critical for this patient population. Specifically, adequate nutrition during treatment can prevent and treat undernutrition, malnutrition, and cachexia; enhance adherence and tolerance to anticancer treatments; improve overall survival; reduce adverse effects of cancer treatment; and improve quality of life (Arends et al., 2017; Krishnasamy et al., 2017).
The American Institute for Cancer Research (AICR, n.d.-b) recommends following a plant-based diet, focusing on fruits, vegetables, grains, beans, nuts, and seeds. This recommendation further suggests to fill at least two-thirds of the plate with fruits, vegetables, whole grains, and beans and no more than one-third of the plate with lean meat, poultry, fish, and low-fat dairy foods (AICR, n.d.-b). Additional cancer prevention recommendations include limiting consumption of fast foods and other processed foods high in fat, starches or sugar, red and processed meats, sugar-sweetened beverages, and alcohol. Studies indicate that diets with more fruits and vegetables protect against certain cancers because of the protective components of the vitamins, minerals, antioxidants, phytochemicals, and fiber (AICR, n.d.-a). In addition, adhering to food-handling guidelines should provide adequate protection against any foodborne illness or infection, even among immunocompromised patients (U.S. Food and Drug Administration, 2019). The Mediterranean diet encompasses all of these cancer prevention recommendations (Davis et al., 2015).
The Mediterranean diet has gained popularity because of its well-researched health benefits. The Mediterranean diet has been associated with a decrease in chronic diseases, such as cardiovascular disease, Alzheimer disease, Parkinson disease, diabetes mellitus, and cancer (Romagnolo & Selmin, 2017). As shown in Figure 1, this dietary pattern is characterized by the wide consumption of plant-based foods, cereals, legumes, fish, and olive oil, as well as moderate red wine consumption (Bonaccio et al., 2013; Widmer et al., 2015). It limits processed meats and refined sugars. A diet high in fruits and vegetables has anti-inflammatory and antioxidant benefits (which include unsaturated fatty acids, fiber, and vitamin C) and is cancer-protective (Wang et al., 2014). In addition, the Mediterranean diet has been associated with a reduced risk of several types of cancers, including breast, colorectal, gastric, lung, and prostate (Jones et al., 2017; Schwingshackl et al., 2017; Toledo et al., 2015; Turati et al., 2018). 
Although there is strong evidence for adhering to the Mediterranean diet, it is unclear whether patients with cancer and nursing staff are aware of its benefits and health-protective components. One cross-sectional study conducted in the Netherlands examined 458 oncology nurses’ perceptions of whether they had sufficient knowledge to provide nutrition advice to patients. Among the 355 nurses providing nutrition advice to patients, 43% reported having insufficient knowledge about nutrition (Van Veen et al., 2017). These data are clinically important given that nurses are frequently asked nutrition questions by patients.
Food safety information includes directives on what to eat and what to avoid for neutropenic or immunocompromised patients, but it does not outline a plan for a well-balanced diet (Sonbol et al., 2015). At Rush University Medical Center, an urban academic medical center in Chicago, Illinois, patients are provided guidelines on how to minimize foodborne illness, such as washing fruits and vegetables, avoiding unpasteurized dairy products, and listening to dietary suggestions when managing nausea, loss of appetite, taste changes, and mouth dryness. However, based on clinical observations, a number of patients with cancer were making poor food choices from the hospital menu, bringing in snacks from home that were mostly processed, or asking nursing staff if it was safe to eat fresh fruits and vegetables. These observations led the clinical team to develop the current practice project.
The purposes of this interprofessional project were to evaluate patients with cancer and nursing staff knowledge about the Mediterranean diet and to provide patient education about its health benefits, particularly in relation to consuming fruits and vegetables.
Methods
This practice initiative used a pre-/post-test survey design on a 32-bed hematology and stem cell transplantation unit in an urban academic medical center. A convenience sample of adult patients aged 18 years or older and all nursing staff were eligible to participate. This project was reviewed by the institutional review board and did not meet the definition of human subjects research.
Procedures
Based on a literature search about the Mediterranean diet, the clinical team could not find an existing survey for patients and nurses to evaluate knowledge about the Mediterranean diet and eating practices. Therefore, a 17-item survey was designed using evidence-based resources, including the Moli-sani Project (Bonaccio et al., 2013), the Mediterranean diet guidelines (Estruch et al., 2018), and the 2015–2020 Dietary Guidelines for Americans (U.S. Department of Health and Human Services & U.S. Department of Agriculture, 2015). This survey consisted of three questions assessing knowledge of, willingness to try or recommend, and beliefs about the Mediterranean diet; five questions assessing current eating practices and beliefs regardless of Mediterranean diet; five questions assessing general nutrition knowledge and Mediterranean diet knowledge; one question addressing the neutropenic diet, asking specifically if the patient believed that fruits and vegetables would cause illness; one question asking how patients received dietary recommendations from their healthcare team; and the final question asking about what would make it easier for patients with cancer to eat healthier (see Figure 2). A combination of multiple-choice and open-ended questions, as well as questions using a five-point Likert-type scale, were used in the survey. 
The same survey was administered to patients (17 items) and nursing staff (15 items). Two questions about personal diet (What is your current diet? What other sources of protein do you eat?) were eliminated from the nurses’ survey because of possible social desirability bias, meaning responding to a question in a favorable manner to please others. The surveys were reviewed for content validity by a certified specialist in oncology nutrition and beta tested with two patients. Initially, it was intended that patients would complete the surveys using a computer tablet; however, during beta testing, it was discovered that a paper-and-pencil format was preferred. Therefore, patient surveys were self-administered, and data were later entered into SurveyMonkey® by the project director. One question about eating practices related to sources of protein intake was eliminated from the post–education session survey because the wording of the question only captured practices prior to hospital admission and, therefore, did not seek behavior change following the education session.
For patients, the pre–education session survey was self-administered in the privacy of the hospital room. The project director was available to provide assistance, and patients were given as much time as needed to complete the survey. The post–education session survey was administered by the same project director 24–48 hours later and then entered into SurveyMonkey.
For nursing staff, the pre–education session survey was emailed and included the purpose of the survey, the total number of questions, estimated time necessary to complete the survey, and the hyperlink to the survey. Nursing staff were asked to complete the survey within one week. Nurses who completed an education session were sent an email with a link to the post–education session survey and asked to complete it within one week.
Education Materials
Education materials for patients and nursing staff were developed from information that was currently used for the general medical–surgical population at the academic medical center. These materials contained evidence-based recommendations for the Mediterranean diet and were originally developed by a registered dietitian at this institution using the Foodsafety.gov and Oldways Mediterranean diet websites. This information was modified by the project certified specialist in oncology nutrition to include food safety and handling practices for the population of patients with cancer, and a one-page educational handout was developed at an appropriate level of health literacy for patients with cancer. This handout included food safety recommendations, Mediterranean diet meal suggestions, serving size, and a magnet illustrating the Mediterranean diet food pyramid. Although red wine is a component of the Mediterranean diet, red wine consumption was not part of the educational materials. Nursing staff received the same handout as patients, along with additional research and evidence related to the benefits of the Mediterranean diet specific to a population of patients with cancer. To ensure consistency of how education materials were presented to patients and staff, the certified specialist in oncology nutrition trained the project director and was present at more than half of the education sessions to provide expertise if needed.
Education Session
Patients received a 10-minute education session immediately after they completed the pre–education session survey. Nursing staff received a 10-minute education session as a brief in-service after they completed the pre–education session survey. Ten education sessions were conducted during the project period by the certified specialist in oncology nutrition or project director and offered at varying times to allow nursing staff working all shifts to participate.
Data Analysis
Data were analyzed using descriptive statistics to report percentages of responses. For six of the multiple-choice questions, percentages exceeded 100% because respondents were able to select more than one answer. For three of the Likert-type scale questions, weighted averages were used to assess pre– and post–education session survey items. Percent change was calculated to determine the effects pre– and post–education session.
Results
Patients
Pre–education session survey: Thirty-four patients completed the pre–education session survey. Of these patients, one was transferred off the unit and six were not feeling well enough to participate, resulting in 27 completed post–education session surveys (79% completion rate). Among the 34 patients who completed the pre–education session survey, more than half (n = 21) were aged 55 years or older, and the majority (n = 24) were diagnosed with leukemia (see Table 1). The main reasons for the current hospital admission included scheduled chemotherapy (n = 16), stem cell transplantation (n = 8), and workup of a new diagnosis (n = 8). 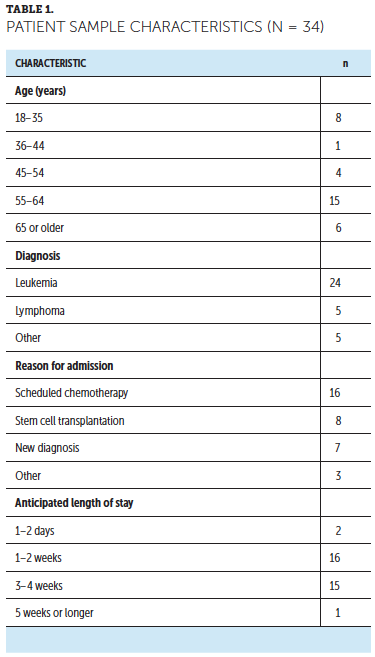
The majority of patients (n = 23) reported that a diet had not been recommended by a healthcare provider, and 13 believed a general diet was the best diet for patients with cancer. When asked about current eating practices, 21 patients reported trying to eat healthy; 11 patients eat what is easily available; 14 patients eat what a family member, friend, or caregiver provides; and 7 patients eat what is most affordable (patients were able to respond to more than one category). With respect to fruits and vegetables, the majority of patients (n = 27) reported eating from one to four servings daily. Twenty-five patients responded that, when washed well, fruits and vegetables are part of a healthy diet for patients with cancer, nine responded that they can cause infection or illness, and seven responded that they can interfere with medications. When asked how many fruits and vegetables are recommended as part of the Mediterranean diet, 14 patients did not know, 10 reported one to three servings, 7 reported five to seven servings, and only 3 reported eight or more servings per day. Guidelines from the Mediterranean diet recommend 8 or more servings of fruits and vegetables per day (Oldways Preservation and Exchange Trust, 2009). When asked how often red meat is recommended as a source of protein according to the Mediterranean diet, 20 patients did not know, 12 reported once per week, and 1 each reported once per day and three to four times per week. Guidelines from the Mediterranean diet recommend one serving of red meat per week (Oldways Preservation and Exchange Trust, 2009). The majority of patients identified that meal ideas (n = 20) and help cooking meals (n = 14) would make it easier to eat healthier while at home and while receiving treatment.
Post–education session survey: Table 2 indicates that patients showed improved knowledge about the Mediterranean diet recommendations after the education session. As noted in Table 3, patients’ knowledge, willingness to try, and belief of effectiveness of the Mediterranean diet favorably changed from pre– to post–education session. 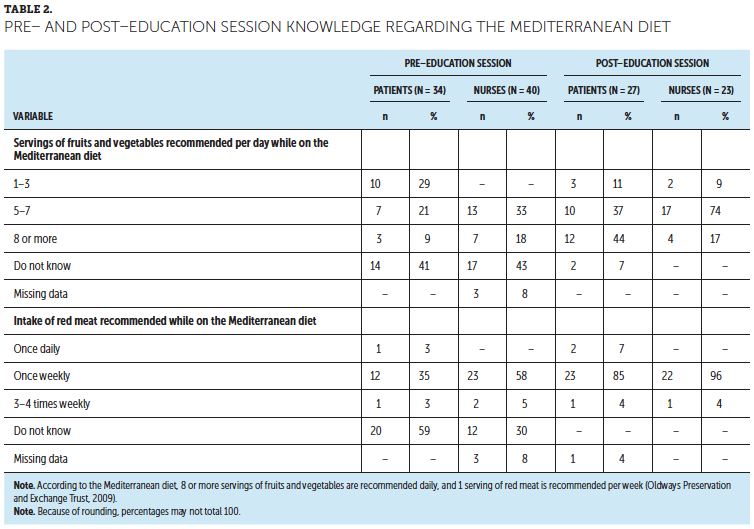
Nursing Staff
Pre–education session survey: Of the 53 nursing staff working on the hematology and stem cell transplantation unit, 40 completed the pre–education session survey. Among these, all were RNs, with more than one-third (n = 16) having one to five years nursing experience and two-thirds (n = 21) having greater than five years of experience. More than half held a professional certification, either OCN® or BMTCN® (see Table 4). 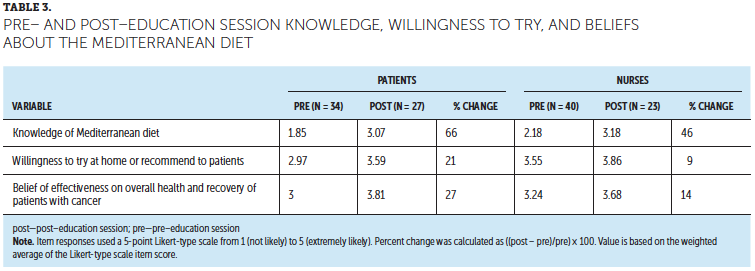
Nursing staff were asked about what they recommend when a patient asks what they should eat at home or during and after treatment; for this question, nurses could choose more than one response. Twenty-four nurses responded that they refer patients to the admission or discharge booklet for information, 13 recommend a safe-handling diet (which emphasizes safe food-handling practices and guidelines to minimize foodborne illness), and 9 recommend the neutropenic diet or refer patients to a consultation with a dietitian. When asked which diet is best for patients with cancer to follow, 13 nurses responded that they believed the general diet to be best, 10 responded with the safe-handling diet, and 7 responded with the Mediterranean diet. When asked about patients with cancer eating fresh fruits and vegetables, almost all nurses (n = 38) responded that, when washed well, they are part of a healthy diet; however, 5 nurses reported they can cause infection, and 11 reported they can interfere with medications. When asked how many fruits and vegetables are recommended as part of the Mediterranean diet, 17 nurses did not know, 13 reported five to seven servings, and 7 reported eight or more servings per day. When asked how often red meat is recommended as a source of protein according to the Mediterranean diet, 12 nurses did not know, 23 reported once per week, and 2 reported three to four times per week. 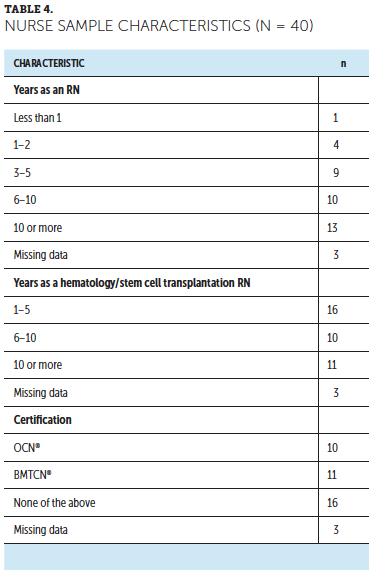
Post–education session survey: More than half of the nurses on staff (n = 28) attended the education session, and 23 nurses completed the post–education session survey. Nursing staff also showed improved knowledge about the Mediterranean diet recommendations after the education session. They experienced favorable changes with respect to knowledge, willingness to try, and belief of effectiveness of the Mediterranean diet from pre– to post–education session.
Discussion
The purpose of this project was to identify knowledge of patients with cancer and nursing staff about the Mediterranean diet and to provide education about the diet’s health benefits, particularly in relation to fruits and vegetables. Several important findings were observed.
The majority of patients reported that they were not given any specific healthy eating recommendations to follow during treatment. Because of the overwhelming amount of information that patients with cancer receive, it is possible that nutrition information is not on the forefront of their minds. It may be helpful to have standardized nutrition information for nursing staff to give patients. These findings are similar to a qualitative study by Beeken et al. (2016) in which patients with cancer generally did not recall receiving any nutrition information from a health professional; if they did, the advice was inconsistent. Patients with cancer are often hospitalized for weeks, presenting the healthcare team with many opportunities to reinforce healthy eating strategies. Another qualitative study reported a lack of consensus among healthcare providers as to the best time to suggest dietary changes for cancer survivors (Coa et al., 2015). At the current authors’ institution, nursing staff frequently encourage patients to eat anything while receiving chemotherapy to ensure caloric intake, regardless of nutritional value. Despite the popularity of the Mediterranean diet, the current project’s findings suggest that patients and nursing staff had limited knowledge about this particular diet (U.S. News and World Report, 2019). Based on this project’s findings, education about the Mediterranean diet can improve knowledge scores for patients and nurses, as well as increase patients’ and nurses’ willingness to add fruits and vegetables to their diet.
Nursing staff survey results indicate that nurses were inconsistent in their nutrition recommendations to patients. This may be because of insufficient nutrition knowledge and/or personal eating practices that may influence what they recommend to patients. Van Veen et al. (2017) also noted a lack of knowledge among oncology nurses, along with providing inconsistent nutrition advice to patients. Nurses who reported insufficient knowledge were also more likely to recommend oral nutrition supplements or a dietitian consultation and were less likely to advise fluid intake as compared to nurses who perceived sufficient nutrition knowledge.
The majority of patients reported consuming few fruits and vegetables. This finding was contradictory to their stated beliefs, because most patients responded that fruits and vegetables are part of a healthy diet when well washed. Although patients reported trying to eat healthy, they were not meeting daily recommendations (U.S. Department of Health and Human Services & U.S. Department of Agriculture, 2015), much less adhering to the guidelines of the Mediterranean diet. Eating healthy refers to consuming adequate amounts of fruits, vegetables, lean sources of protein, and dairy and limiting the amount of saturated fat, sodium, and added sugars consumed, but it also takes into account personal preferences, culture, and budget (U.S. Department of Health and Human Services & U.S. Department of Agriculture, 2015). This project’s findings are similar to national data, which report that the average U.S. adult eats about 10% of the recommended amount of fruits and vegetables each day (Centers for Disease Control and Prevention, 2018). Of note, this project’s findings differ from the study findings of Beeken et al. (2016) in which a cancer diagnosis acted as a prompt for patients to improve dietary practices by eating more fruits and vegetables.
Although only one-fourth of this project’s patients responded that fruits and vegetables can cause infection or illness, it is concerning that patients still state their belief that the neutropenic guidelines are relevant. The current authors’ institution discontinued use of the neutropenic diet in 2011 on the inpatient menu, but nearly 10 years later, patients are still asking about its practice. Even as many institutions are abandoning the neutropenic diet, others across the country still adhere to its recommendations (Wolfe et al., 2018). Therefore, continued education among patients and nursing staff is needed to reinforce evidence-based dietary recommendations.
Limitations
Although this practice initiative resulted in favorable outcomes, there are limitations to note. First, this initiative was designed as a practice change, and a comparison group was not included. Further investigation is warranted using a rigorous research design to determine the effect of patient and nursing staff education with respect to clinical outcomes. Second, this project used a relatively small convenience sample; therefore, findings may not be generalizable. In addition, many nurses were not able to attend the education session because of patient care assignments and responsibilities.
Implications for Practice
Nursing staff need to be well informed to provide consistent nutrition information to patients. Encouraging patients to increase fruit and vegetable intake is part of a healthy diet. The current practice initiative was simple and affordable and can be easily replicated in other patient populations. The findings revealed that nurses believe fruits and vegetables are part of a healthy diet, but they are uncertain whether they are safe for patients with cancer to consume. These findings indicate an important area for additional nursing staff education. 
Conclusion
This project provides evidence that nutrition education is important for patients with cancer and nursing staff. Providing nutrition education allows patients to be informed and helps them understand that, when washed well, fruits and vegetables are safe to eat and are part of a healthy diet.. This is particularly important because fruit and vegetable intake was low among this project’s patient population. Additional projects are needed to identify and develop strategies for patients with cancer to increase fruit and vegetable intake and tailor meals according to cultural preferences. [[{"fid":"55296","view_mode":"default","fields":{"format":"default","alignment":"","field_file_image_alt_text[und][0][value]":false,"field_file_image_title_text[und][0][value]":false},"link_text":null,"type":"media","field_deltas":{"1":{"format":"default","alignment":"","field_file_image_alt_text[und][0][value]":false,"field_file_image_title_text[und][0][value]":false}},"attributes":{"class":"media-element file-default","data-delta":"1"}}]]
About the Author(s)
Karine R. Otten, MSN, RN, ANP-BC, OCN®, is a hematology/oncology urgent care nurse practitioner, Beth A. Staffileno, PhD, FAHA, is a professor in the Department of Adult Health and Gerontological Nursing in the College of Nursing and co-director of the Center for Clinical Research and Scholarship, Marisa Mozer, MS, RD, CSO, LDN, CNSC, is an advanced clinical dietitian, all at Rush University Medical Center; and Cate Maidlow, MSN, RN, OCN®, CNL, is a clinical research nurse at Rush University Cancer Center, all in Chicago, IL. The authors take full responsibility for this content. This project received funding from the Juliet A. Shaffer Recine Nursing Oncology Research Award. The article has been reviewed by independent peer reviewers to ensure that it is objective and free from bias. Otten can be reached at karine_otten@rush.edu, with copy to CJONEditor@ons.org. (Submitted July 2019. Accepted October 15, 2019.)
References
American Institute for Cancer Research. (n.d.-a). AICR’s foods that fight cancerTM. https://www.aicr.org/foods-that-fight-cancer
American Institute for Cancer Research. (n.d.-b). Cancer prevention recommendations. https://www.aicr.org/reduce-your-cancer-risk/recommendations-for-cancer…
Arends, J., Baracos, V., Bertz, H., Bozzetti, F., Calder, P.C., Deutz, N.E.P., . . . Weimann, A. (2017). ESPEN expert group recommendations for action against cancer-related malnutrition. Clinical Nutrition, 36(5), 1187–1196. https://doi.org/10.1016/j.clnu.2017.06.017
Beeken, R.J., Williams, K., Wardle, J., & Croker, H. (2016). “What about diet?” A qualitative study of cancer survivors’ views on diet and cancer and their sources of information. European Journal of Cancer Care, 25(5), 774–783. https://doi.org/10.1111/ecc.12529
Bonaccio, M., Di Castelnuovo, A., Costanzo, S., De Lucia, F., Olivieri, M., Donati, M.B., . . . Bonanni, A. (2013). Nutrition knowledge is associated with higher adherence to Mediterranean diet and lower prevalence of obesity. Results from the Moli-sani study. Appetite, 68, 139–146. https://doi.org/10.1016/j.appet.2013.04.026
Centers for Disease Control and Prevention. (2018). State indicator report on fruits and vegetables, 2018. https://www.cdc.gov/nutrition/downloads/fruits-vegetables/2018/2018-fru…
Coa, K.I., Smith, K.C., Klassen, A.C., Caulfield, L.E., Helzlsouer, K., Peairs, K., & Shockney, L. (2015). Capitalizing on the “teachable moment” to promote healthy dietary changes among cancer survivors: The perspectives of health care providers. Supportive Care in Cancer, 23(3), 679–686. https://doi.org/10.1007/s00520-014-2412-z
Davis, C., Bryan, J., Hodgson, J., & Murphy, K. (2015). Definition of the Mediterranean diet; a literature review. Nutrients, 7(11), 9139–9153. https://doi.org/10.3390/nu7115459
Estruch, R., Salas-Salvadó, J., Covas, M.I., Corella, D., Arós, F., Gómez-Gracia, E., . . . Martínez-González, M.A. (2018). Primary prevention of cardiovascular disease with a Mediterranean diet supplemented with extra-virgin olive oil or nuts. New England Journal of Medicine, 378(25), e34. https://doi.org/10.1056/NEJMoa1800389
Foster, M. (2014). Reevaluating the neutropenic diet: Time to change. Clinical Journal of Oncology Nursing, 18(2), 239–241. https://doi.org/10.1188/14.CJON.239-241
Jones, P., Cade, J.E., Evans, C.E.L., Hancock, N., & Greenwood, D.C. (2017). The Mediterranean diet and risk of colorectal cancer in the UK Women’s Cohort Study. International Journal of Epidemiology, 46(6), 1786–1796. https://doi.org/10.1093/ije/dyx155
Krishnasamy, K., Yoong, T.L., Chan, C.M., Choong, L.P., & Chinna, K. (2017). Identifying malnutrition: Nutritional status in newly diagnosed patients with cancer. Clinical Journal of Oncology Nursing, 21(1), E23–E29. https://doi.org/10.1188/17.CJON.E23-E29
Lassiter, M., & Schneider, S.M. (2015). A pilot study comparing the neutropenic diet to a non-neutropenic diet in the allogeneic hematopoietic stem cell transplantation population. Clinical Journal of Oncology Nursing, 19(3), 273–278. https://doi.org/10.1188/15.CJON.19-03AP
Oldways Preservation and Exchange Trust. (2009). Mediterranean diet pyramid. https://oldwayspt.org/resources/oldways-mediterranean-diet-pyramid
Romagnolo, D.F., & Selmin, O.I. (2017). Mediterranean diet and prevention of chronic diseases. Nutrition Today, 52(5), 208–222. https://doi.org/10.1097/NT.0000000000000228
Schwingshackl, L., Schwedhelm, C., Galbete, C., & Hoffmann, G. (2017). Adherence to Mediterranean diet and risk of cancer: An updated systematic review and meta-analysis. Nutrients, 9(10), 1063. https://doi.org/10.3390/nu9101063
Sonbol, M.B., Firwana, B., Diab, M., Zarzour, A., & Witzig, T.E. (2015). The effect of a neutropenic diet on infection and mortality rates in cancer patients: A meta-analysis. Nutrition and Cancer, 67(8), 1232–1240. https://doi.org/10.1080/01635581.2015.1082109
Toledo, E., Salas-Salvadó, J., Donat-Vargas, C., Buil-Cosiales, P., Estruch, R., Ros, E., . . . Martínez-González, M.A. (2015). Mediterranean diet and invasive breast cancer risk among women at high cardiovascular risk in the PREDIMED trial: A randomized clinical trial. JAMA Internal Medicine, 175(11), 1752–1760. https://doi.org/10.1001/jamainternmed.2015.4838
Turati, F., Carioli, G., Bravi, F., Ferraroni, M., Serraino, D., Montella, M., . . . La Vecchia, C. (2018). Mediterranean diet and breast cancer risk. Nutrients, 10(3), 326. https://doi.org/10.3390/nu10030326
U.S. Food and Drug Administration (2019). Food safety for people with cancer. https://www.fda.gov/food/people-risk-foodborne-illness/food-safety-peop…
U.S. Department of Health and Human Services & U.S. Department of Agriculture. (2015). 2015–2020 dietary guidelines for Americans (8th ed.). https://health.gov/dietaryguidelines/2015/guidelines
U.S. News and World Report (2019, January 2). U.S. news reveals best diets rankings for 2019. https://www.usnews.com/info/blogs/press-room/articles/2019-01-02/us-new…
Van Veen, M.R., Hoedjes, M., Versteegen, J.J., van de Meulengraaf-Wilhelm, N., Kampman, E., & Beijer, S. (2017). Improving oncology nurses’ knowledge about nutrition and physical activity for cancer survivors. Oncology Nursing Forum, 44(4), 488–496. https://doi.org/10.1188/17.ONF.488-496
Wang, X., Ouyang, Y., Liu, J., Zhu, M., Zhao, G., Bao, W., & Hu, F.B. (2014). Fruit and vegetable consumption and mortality from all causes, cardiovascular disease, and cancer: Systematic review and dose-response meta-analysis of prospective cohort studies. BMJ, 349, g4490. https://doi.org/10.1136/bmj.g4490
Widmer, R.J., Flammer, A.J., Lerman, L.O., & Lerman, A. (2015). The Mediterranean diet, its components, and cardiovascular disease. American Journal of Medicine, 128(3), 229–238. https://doi.org/10.1016/j.amjmed.2014.10.014
Wolfe, H.R., Sadeghi, N., Agrawal, D., Johnson, D.H., & Gupta, A. (2018). Things we do for no reason: Neutropenic diet. Journal of Hospital Medicine, 13(8), 573–576.




