Direct-to-Consumer Genomic Testing Through an Ethics Lens: Oncology Nursing Considerations
Background: The use of direct-to-consumer genomic testing (DTCGT) is increasing, but this testing may not be comprehensive and may lack clinical validity and utility. The ethical constructs of beneficence, nonmaleficence, justice, and autonomy provide a framework for coordinating the care of patients and their families.
Objectives: This article provides an overview of the DTCGT process and reviews the ethical implications that affect clinical care.
Methods: A review of the literature was conducted using the following key words: genetics/genomics and direct-to-consumer testing. Common themes were identified, including test types, regulatory standards, marketing practices, ethics, privacy, and nursing implications.
Findings: An increased awareness of the clinical and ethical consequences of DTCGT is needed among healthcare providers and the general population. Oncology nurses can assist patients in navigating the field of genomics through consistent and comprehensive risk assessment, patient education about the risks and benefits of DTCGT, and referral to genomics professionals when appropriate.
Jump to a section
Earn free contact hours: Click here to connect to the evaluation. Certified nurses can claim no more than 1 total ILNA point for this program. Up to 1 ILNA point may be applied to Nursing Practice OR Oncology Nursing Practice OR Professional Practice/Performance OR Role of the APRN. See www.oncc.org for complete details on certification.
Technological advances and increased affordability have propelled exponential growth in the direct-to-consumer genomic testing (DTCGT) industry. To continue to provide optimal evidence-based care, oncology nurses need to maintain awareness of the changing landscape of genomic testing, including DTCGT. The global market for DTCGT is expected to be more than $4.4 billion by 2028 (Swain & Kharad, 2023). As patients become more active participants in their health care, they are increasingly engaging with third-party genomic testing services outside of the patient–provider relationship. To date, more than 26 million individuals have used DTCGT from five of the most prevalent companies (Offit et al., 2023).
Rising DTCGT rates are associated with increases in patient questions and concerns. DTCGT differs from clinical genomic testing that routinely occurs in oncology care. This article explores the ethical implications of DTCGT to provide oncology nurses with the knowledge required to competently address common patient situations related to DTCGT. In addition, this article provides context for the primary ethical principles of beneficence (do good), nonmaleficence (do no harm), justice (fairness), and autonomy (the right to make one’s own decisions).
Types of DTCGT
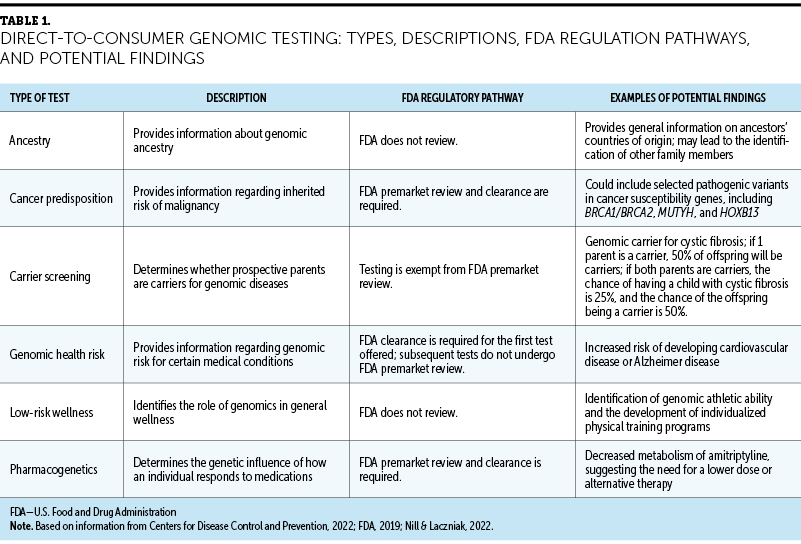
Genomic testing is categorized by its setting (e.g., clinical versus DTCGT) and the individual initiating the process (e.g., provider versus patient) (see Figure 1). DTCGT is characterized by the ability to purchase genomic tests directly without an order from or consultation with a healthcare professional. More than 120 companies offer DTCGT to consumers (National Library of Medicine, n.d.-c). The U.S. Food and Drug Administration (FDA, 2019) classifies DTCGT in six different categories with varying regulatory pathways: ancestry, cancer predisposition, carrier screening, genomic health risk, low-risk wellness, and pharmacogenetics tests (see Table 1).

Perceived Benefits of DTCGT
Some individuals perceive DTCGT to be more convenient than clinical testing because the process does not require multiple appointments and is faster and more affordable (Offit et al., 2023). With DTCGT, individuals have multiple options. Individuals can research test prices; in most cases, testing is performed without the benefit of pretest risk assessment and genetic counseling. Individuals may also perceive DTCGT to be more confidential because they are not obligated to share results with their healthcare team (Ayala-Lopez & Nichols, 2020). Individuals may assume they will receive clear, accurate health information to actively manage their health, allowing them to feel empowered (Horton et al., 2019).
Genomic Testing Strategies
Genomic testing influences treatment decisions, measurement of treatment response, the development of new regimens, discussions related to prognosis, and, in the case of germline testing, estimation of the risk of developing malignancy in individuals and their family members. Most DTCGT focuses on the germline risks of developing cancer and other diseases. Clinical genomic testing can include next-generation sequencing and single nucleotide variant technologies for germline and somatic (acquired) pathogenic variants (Helzlsouer et al., 2020). In the clinical setting, the technology selected depends on the patient’s personal and family history, as well as on previous genomic testing results. Next-generation sequencing assesses almost the entire genetic code in a gene or multiple genes to identify whether variants are present. In contrast, single nucleotide variant technology searches for only specific variants. This method may be helpful when looking for a known variant in familial cascade testing; however, single nucleotide variant technology is inadequate if there is not a known pathogenic variant in which a multigene panel is indicated to explore cancer risk more comprehensively. Many direct-to-consumer tests use single nucleotide variant analysis and do not sequence the entire gene (Horton et al., 2019).
DTCGT screens for only a few specific variants in a limited number of genes associated with malignancy or other diseases (Kilbride & Bradbury, 2020). For example, a popular DTCGT company, 23andMe, advertises that their test assesses the risk of developing cancer, but it is limited. The 23andMe test explores three variants in the BRCA1/BRCA2 genes and two variants in the MUTYH gene (National Library of Medicine, n.d.-a). This type of single nucleotide variant technology will detect only a small number of germline pathogenic variants that increase the risk of developing malignancy. In the context of nonmaleficence, inadequate genomic analysis and poor consumer awareness could lead individuals to underestimate their risk of developing malignancy and miss opportunities to increase surveillance or risk-reducing surgery to decrease morbidity and mortality.
Genomic Test Evaluation and Regulation
The following methods are used to assess genomic tests: (a) analytic validity, which refers to how well the test predicts the presence or absence of a variant; (b) clinical validity, which is how well a variant is related to disease risk; and (c) clinical utility, which determines whether this information will be helpful in improving patient outcomes (National Human Genome Research Institute, 2022b). Regulatory bodies monitoring DTCGT often fail to address these concepts adequately; there is no oversight for clinical utility. In the absence of healthcare professionals guiding the testing process, DTCGT results may be miscommunicated and misinterpreted.
Test Interpretation
Once testing is complete, correct interpretation of results drives appropriate medical intervention. After completing DTCGT, individuals are often offered the opportunity to download their raw data for an additional fee. Raw data are the result of extracting one’s genotype from a provided sample. For an additional fee, individuals can run these data through a third-party interpretation service. Most testing companies state that raw data should be used only for research or educational purposes, rather than for clinical decision-making (National Library of Medicine, n.d.-b). Ethical concerns related to the use of raw data include a lack of privacy protections once downloaded or stored, little regulation of interpretation services, the potential for individuals to receive upsetting results without counseling, and false-positive findings, in which the presence of a pathogenic variant is incorrectly identified (National Library of Medicine, n.d.-b). These concerns have significant implications in the context of nonmaleficence, with potential for harm for individuals and their family members.
Another emerging issue is the need to reinterpret the clinical significance of genomic variants over time. Although an individual’s genomic sequence does not change, continued advancements in knowledge can lead to changes in interpretation and assigned pathogenicity. In clinical genomic testing, reclassification is ongoing, and changes are communicated to the ordering provider, who then revises recommendations for care with the patient. Variant reclassification and notification policies are not clear in DTCGT (Marchant et al., 2020). Future liability must be considered when determining who is responsible for the reinterpretation of these variants. Justice is another consideration, given that healthcare access issues could affect an individual’s ability to obtain updated or reinterpreted genomic data.
Regulation
DTCGT regulation in the United States falls under the Clinical Laboratory Improvement Act (CLIA), the FDA, the Federal Trade Commission, the Centers for Medicare and Medicaid Services, and some individual state regulations (Sharkey, 2019). No entity has complete oversight of DTCGT, creating fragmented regulatory processes (see Figure 2).

FDA: The FDA authorizes the use of genomic testing for screening and disease diagnosis. The FDA uses enforcement discretion to regulate genomic tests; therefore, they may elect not to exercise their authority over these products (National Human Genome Research Institute, 2022b). To date, FDA regulation depends on whether a test is marketed as a commercial kit or, more commonly, is available as a laboratory-developed test. Commercial kits are sold to the laboratory and regulated by the FDA as a medical device, whereas laboratory-developed tests are marketed under enforcement discretion without an assessment of analytic or clinical validity (Healthcare Fraud Prevention Partnership, 2020). Laboratory-developed tests are not regulated by how well they identify variants (analytic validity) or correlate associated risks of disease (clinical validity). Regarding beneficence, it is challenging to identify any benefits of DTCGT if tests are not proven to have analytic and clinical validity.
Centers for Medicare and Medicaid Services: Although the FDA determines the regulation of tests, the Centers for Medicare and Medicaid Services manages laboratories and ensures testing occurs according to CLIA standards. These standards examine quality, precision, and reliability of testing within a laboratory. The Centers for Medicare and Medicaid Services regulates analytic validity, but there is no federal oversight of clinical validity. Testing results may be accurate, but disease risks and recommendations are not standardized. Laboratories performing tests, including DTCGT, of lower complexity as defined by the FDA (2020) may waive regulation requirements if the testing procedures meet CLIA standards (National Human Genome Research Institute, 2022b). According to the Centers for Disease Control and Prevention (2023), very few DTCGT laboratories are CLIA certified.
Federal Trade Commission: The Federal Trade Commission exercises regulatory authority when there are concerns about unfair or deceptive practices. If there are risks associated with misleading privacy claims or inadequate data security, the Federal Trade Commission may take legal action. For example, in one case, companies marketing customized nutritional supplements, allegedly based on consumer genomic data, were charged with deceptive advertising and lax data security (National Human Genome Research Institute, 2022b).
Lack of oversight: No U.S.-based regulatory bodies have standards to regulate the clinical utility of genomic testing (National Human Genome Research Institute, 2022b). DTCGT methods associated with a low risk or used for nonmedical purposes are not reviewed before being offered to consumers (FDA, 2019). This fragmented oversight results in a lack of repercussions for DTCGT companies using genomic data. Given the lack of federal regulation, data sharing and the use of genomic information are often governed by policies specific to each company (Daviet et al., 2022). Ethically, patient autonomy is at risk because the use of their own genomic data is not under their control.
Advertising and Fraud Risks With DTCGT
Genomic data are unique because of their unchanging nature and potential to identify individuals and families. Despite the claims of DTCGT companies, there is potential for misuse because of the sensitive nature of the information captured (Daviet et al., 2022). DTCGT companies may employ methods of advertising that exploit individuals’ trust by claiming that the process is comprehensive and the results are clinically useful (Nill & Laczniak, 2022). For example, an individual may be led to believe that ambiguous DTCGT results are accurate, actionable, and performed with the support of a healthcare provider. By doing so, individuals may make potentially harmful healthcare decisions related to personalized cancer screening based on inadequate information. From the ethical perspectives of justice and nonmaleficence, these marketing practices may not be fair, balanced, or in the best interest of individuals.
The risk of fraud is real. DTCGT can also be promoted via telemarketing, with potential financial and protected personal information losses. In 2019, federal agents raided laboratories and charged 35 people with performing fraudulent genomic testing, resulting in an estimated $2.1 billion lost billing to federal healthcare insurance programs (U.S. Department of Health and Human Services, 2023). Fraudulent telemarketing can use several approaches. Medicare beneficiaries may be contacted by telemarketers and informed that Medicare will pay for genomic testing. The telemarketer gets a physician to sign off, so a laboratory—often of questionable quality—will process the test. The physician receives a kickback in exchange for ordering the test. Alternatively, the patient is given a form to be signed by their primary provider, who then becomes the ordering provider. The patient is encouraged to sign the form quickly before the offer expires. The laboratory processes the test and bills Medicare, which reimburses the laboratory for the test. The laboratory shares the proceeds with the telemarketer. In addition to fraudulent practices, there is a risk of identity theft because these telemarketers have access to protected information. Fraud and identify theft are associated with the ethical construct of maleficence because they risk patient harm.
Cost of DTCGT
The cost of clinical genomic testing varies depending on insurance coverage, the type of test selected, individual and family history, and the complexity of the testing process. Costs of genomic testing range from less than $100 to thousands of dollars (Healthcare Fraud Prevention Partnership, 2020). Insurance coverage and financial assistance programs have made clinical testing more affordable with self-pay options comparable to DTCGT. DTCGT is self-pay, with individuals assuming the cost of testing. Individuals may choose DTCGT because testing may appear to be simpler and less expensive because there is no need to meet an insurance deductible, take personal time from work for appointments, or pay co-pays for counseling. Most DTCGT companies recommend that individuals pursue confirmatory testing in clinical settings in a CLIA-certified laboratory if any concerning variants are identified from testing, essentially negating any perceived benefit of cost savings. In terms of justice, the added expenses associated with confirmatory testing in clinical settings may not be affordable to all, raising concerns of inequity.
Implications for Nursing
Privacy
Many DTCGT companies use consumer data for ancillary objectives and share and/or sell information to third parties (Daviet et al., 2022). Corporate ownership of personal genomic information is worrisome because companies use data at their own discretion, completely out of the control of consumers (Nill & Laczniak, 2022). One of the largest DTCGT companies, 23andMe, has confirmed that it resells users’ genomic data to clinical research and pharmaceutical establishments (Raz et al., 2020). This has implications for autonomy because individuals are unable to make decisions about the use of their own genomic information once testing is initiated. In addition, DTCGT companies may not be transparent with consumers regarding their privacy policies. Some companies alter their policies without informing consumers (Daviet et al., 2022). Often this information is not available prior to the purchase of DTCGT kits, which has significant implications for the informed consent process.
Individuals’ genomic data potentially allow them to draw conclusions about their relatives. When an individual submits a personal sample, they have indirectly submitted the genomic data of their entire family without their consent (Kitnick, 2020). Unlike direct-to-consumer genomic ancestry testing, clinical testing does not provide results that link relatives. Privacy may be further compromised with DTCGT because of cybersecurity vulnerability or requests for data access from law enforcement during criminal searches (Ayala-Lopez & Nichols, 2020). If individuals cannot control the access and use of their own genomic data, patient autonomy is nonexistent.
Informed Consent
The use of retrospectively collected data complicates the process of obtaining and updating informed consent. To accommodate this, DTCGT companies frequently ask consumers for blanket permission to use their personal data for all future research at the time of consent. However, it is unlikely at the time of initial consent that consumers will fully grasp the implications and risks of future research (Daviet et al., 2022). Given the unique qualities of genomic information, comprehensive informed consent is difficult to obtain. In the absence of true informed consent, patient autonomy does not exist. Individuals are unable to exercise their freedom to make an educated decision about whether to undergo genomic testing if they do not receive adequate information related to potential future uses in advance.
Genetic Information Nondiscrimination Act
The Genetic Information Nondiscrimination Act was passed to protect individuals against discrimination associated with their genomic information. This legislation prevents health insurers and employers from discriminating based on family history of disease and/or genomic test results (Areheart & Roberts, 2019). However, the Genetic Information Nondiscrimination Act’s protections do not apply to life, long-term care, or disability insurance, or to those who receive care via insurance providers sponsored by the military or federal government (Underhill-Blazey & Klehm, 2020). This has implications in the context of nonmaleficence. Individuals may assume that the benefits of DTCGT will outweigh the risks and that information gained will benefit them and their future medical management. However, positive test findings can have significant implications on future insurability for life, long-term care, or disability insurance. If these risks are not communicated fairly and equitably during pretest counseling or informed consent processes, then the ethical principle of justice is in jeopardy as well.
Legal Concerns
Legal consequences of healthcare professionals’ actions are governed by the concept of negligence. Healthcare professionals are held accountable when they fail to abide by generally accepted standards of medical practice. However, with the rapid advancement of genomic testing and precision medicine, generally accepted standards of practice may not yet be established (McGrath et al., 2021). With DTCGT, the presence or absence of these standards is irrelevant because healthcare professionals may not be involved in the testing process. Healthcare professionals become liable if they do not recognize the need for testing and do not manage results from testing appropriately. Patients are more likely to undergo DTCGT if they feel their needs are unmet or if their family history and potential health risks are ignored (Majumder et al., 2021). With beneficence in mind, healthcare systems can develop evidence-based policies and educational offerings to better prepare nurses for these situations, which can address future liability concerns (Marchant et al., 2020).
Identifying the clinical utility of a test or a recommendation for prevention is already a challenging task because healthcare professionals work to link genomic variants to associated disease risks. False-positive results may lead to unnecessary invasive intervention, and false-negative results could lead to the absence of intervention for patients who would greatly benefit. The misinterpretation of results represents a liability concern (Marchant et al., 2020). In a study of 49 patient samples, 40% of variants initially identified by DTCGT were not present when more rigorous sequencing was performed. Another study also demonstrated that multiple variants confirmed by sequencing had been incorrectly classified as pathogenic (Tandy-Connor et al., 2018). Clinicians need to understand this potential liability and risk of harm from inappropriate care. Some professional organizations have developed formal position statements encouraging caution when using or interpreting DTCGT data to help healthcare professionals navigate the emerging DTCGT landscape.

Psychological Impact
For some individuals, genomic testing results can be upsetting. In a survey of 23,196 consumers who had undergone DTCGT, 61% of respondents reported findings that relayed new healthcare information about themselves or a relative. This included distressing news that a parent was not their biologic parent, or they had a sibling of whom they were unaware. Consumers who learned they were conceived via donor (sperm, egg, or embryo) reported that they regretted their decision to pursue DTCGT (Guerrini et al., 2022). Patients are at risk for uncovering life-altering information, including situations of rape, abandonment, or other family confidences. Ethically, pretest counseling offers opportunities to weigh concerns about beneficence and nonmaleficence and places patients in a position of autonomy where, once educated and informed, they can decide about testing at their discretion.

Oncology nurses regularly encounter questions and ethical considerations regarding DTCGT (see Figure 3). Staying up to date on the genomic testing process enables nurses to provide basic education about DTCGT, including potential risks, limitations, and ethical concerns. Figure 4 presents resources to increase knowledge and awareness of genomic concepts and DTCGT.

Conclusion
With more individuals pursuing DTCGT, it is likely that requests for the interpretation of results in the clinical setting will increase accordingly. The current labor force of genetics professionals is already deficient, and these patient conversations can be time-consuming (Redlinger-Grosse et al., 2021). Oncology nurses can meet this disparity (Brothers & Knapp, 2018). One way genomic testing disparities can be addressed is to train nurses to appropriately advocate for patients and emphasize their role in family history collection, patient education on the limitations of DTCGT, the use of genetics professionals, and the appropriate implementation of interventions, with the goal of providing patients with comprehensive, ethical genomic care.

About the Authors
Cheryl Ann VerStrate, DNP, RN, AGPCNP-BC, OCN®, is an assistant professor in the Kirkhof College of Nursing at Grand Valley State University in Grand Rapids, MI; and Suzanne M. Mahon, DNS, RN, AOCN®, AGN-BC, FAAN, is professor emerita in the Division of Hematology/Oncology in the Department of Internal Medicine and the Trudy Busch Valentine School of Nursing at Saint Louis University in Missouri. The authors take full responsibility for this content. The authors were participants in the Clinical Journal of Oncology Nursing Writing Mentorship Program. The article has been reviewed by independent peer reviewers to ensure that it is objective and free from bias. VerStrate can be reached at verstche@gvsu.edu, with copy to CJONEditor@ons.org. (Submitted February 2023. Accepted March 23, 2023.)
References
American College of Obstetricians and Gynecologists. (2021). Consumer testing for disease risk. ACOG Committee Opinion No. 816. Obstetrics and Gynecology, 137, e1–e6. https://www.acog.org/clinical/clinical-guidance/committee-opinion/artic…
Areheart, B.A., & Roberts, J.L. (2019). GINA, big data, and the future of employee privacy. Yale Law Journal, 128(3), 710–790.
Ayala-Lopez, N., & Nichols, J.H. (2020). Benefits and risks of direct-to-consumer testing. Archives of Pathology and Laboratory Medicine, 144(10), 1193–1198. https://doi.org/10.5858/arpa.2020-0078-RA
Brothers, K.B., & Knapp, E.E. (2018). How should primary care physicians respond to direct-to-consumer genetic test results? AMA Journal of Ethics, 20(9), E812–E818. https://doi.org/10.1001/amajethics.2018.812
Centers for Disease Control and Prevention. (2022). Genomics and precision health: Genetic testing. https://www.cdc.gov/genomics/gtesting/genetic_testing.htm
Centers for Disease Control and Prevention. (2023). Clinical Laboratory Improvement Amendments (CLIA): CLIA laboratory search. https://www.cdc.gov/clia/LabSearch.html
Daviet, R., Nave, G., & Wind, J. (2022). Genetic data: Potential uses and misuses in marketing. Journal of Marketing, 86(1), 7–26. https://doi.org/10.1177/0022242920980767
Guerrini, C.J., Robinson, J.O., Bloss, C.C., Brooks, W.B., Fullerton, S.M., Kirkpatrick, B., . . . McGuire, A.L. (2022). Family secrets: Experiences and outcomes of participating in direct-to-consumer genetic relative–finder services. American Journal of Human Genetics, 109(3), 486–497. https://doi.org/10.1016/j.ajhg.2022.01.013
Healthcare Fraud Prevention Partnership. (2020). Genetic testing: Fraud, waste, and abuse [White paper]. https://www.cms.gov/files/document/hfpp-genetic-testing-fwa-white-paper…
Helzlsouer, K., Meerzaman, D., Taplin, S., & Dunn, B.K. (2020). Humanizing big data: Recognizing the human aspect of big data. Frontiers in Oncology, 10, 186. https://doi.org/10.3389/fonc.2020.00186
Horton, R., Crawford, G., Freeman, L., Fenwick, A., Wright, C.F., & Lucassen, A. (2019). Direct-to-consumer genetic testing. BMJ, 367, l5688. https://doi.org/10.1136/bmj.l5688
Kilbride, M.K., & Bradbury, A.R. (2020). Evaluating web-based direct-to-consumer genetic tests for cancer susceptibility. JCO Precision Oncology, 4, 161–169. https://doi.org/10.1200/PO.19.00317
King, E., & Mahon, S.M. (2017). Genetic testing: Challenges and changes in testing for hereditary cancer syndromes. Clinical Journal of Oncology Nursing, 21(5), 589–598. https://doi.org/10.1188/17.CJON.589-598
Kitnick, J. (2020). Killer’s code—Familial DNA searches through third-party databases under Carpenter. Cardozo Law Review, 41(2), 855–898. https://cardozolawreview.com/killers-code-familial-dna-searches-through…
Mahon, S.M. (2018). Direct-to-consumer genetic testing: Helping patients make informed choices. Clinical Journal of Oncology Nursing, 22(1), 33–36. https://doi.org/10.1188/18.CJON.33-36
Majumder, M.A., Guerrini, C.J., & McGuire, A.L. (2021). Direct-to-consumer genetic testing: Value and risk. Annual Review of Medicine, 72, 151–166. https://doi.org/10.1146/annurev-med-070119-114727
Marchant, G., Barnes, M., Evans, J.P., LeRoy, B., & Wolf, S.M. (2020). From genetics to genomics: Facing the liability implications in clinical care. Journal of Law, Medicine and Ethics, 48(1), 11–43. https://doi.org/10.1177/1073110520916994
McGrath, S.P., Peabody, A.E., Jr., Walton, D., & Walton, N. (2021). Legal challenges in precision medicine: What duties arising from genetic and genomic testing does a physician owe to patients? Frontiers in Medicine, 8, 663014. https://doi.org/10.3389/fmed.2021.663014
National Human Genome Research Institute. (2022a). Direct-to-consumer genetic testing FAQ for healthcare professionals. https://www.genome.gov/For-Health-Professionals/Provider-Genomics-Educa…
National Human Genome Research Institute. (2022b). Regulation of genetic tests. https://www.genome.gov/about-genomics/policy-issues/Regulation-of-Genet…
National Library of Medicine. (n.d.-a). Can a direct-to-consumer genetic test tell me whether I will develop cancer? MedlinePlus. https://medlineplus.gov/genetics/understanding/dtcgenetictesting/dtccan…
National Library of Medicine. (n.d.-b). What can raw data from a direct-to-consumer genetic test tell me? MedlinePlus. https://medlineplus.gov/genetics/understanding/dtcgenetictesting/dtcraw…
National Library of Medicine. (n.d.-c). What is direct-to-consumer genetic testing? MedlinePlus. https://medlineplus.gov/genetics/understanding/dtcgenetictesting/direct…
Nill, A., & Laczniak, G. (2022). Direct-to-consumer genetic testing and its marketing: Emergent ethical and public policy implications. Journal of Business Ethics, 175, 669–688. https://doi.org/10.1007/s10551-020-04632-z
Offit, K., Sharkey, C.M., Green, D., Wu, X., Trottier, M., Hamilton, J.G., . . . Stadler, Z.K. (2023). Regulation of laboratory-developed tests in preventive oncology: Emerging needs and opportunities. Journal of Clinical Oncology, 41(1), 11–21. https://doi.org/10.1200/JCO.22.00995
Pritchard, D., Goodman, C., & Nadauld, L.D. (2022). Clinical utility of genomic testing in cancer care. JCO Precision Oncology, 6, e2100349. https://doi.org/10.1200/PO.21.00349
Raz, A.E., Niemiec, E., Howard, H.C., Sterckx, S., Cockbain, J., & Prainsack, B. (2020). Transparency, consent and trust in the use of customers’ data by an online genetic testing company: An exploratory survey among 23andMe users. New Genetics and Society, 39(4), 459–482. https://doi.org/10.1080/14636778.2020.1755636
Redlinger-Grosse, K., Anderson, K., Birkeland, L., Zaleski, C., & Reiser, C. (2021). 6 feet apart but working together. Journal of Genetic Counseling, 30(4), 1069–1073. https://doi.org/10.1002/jgc4.1408
Sharkey, C.M. (2019). Direct-to-consumer genetic testing: The FDA’s dual role as safety and health information regulator. DePaul Law Review, 68(2), 343–384.
Swain, R., & Kharad, S. (2023). Direct-to-consumer (DTC) genetic testing market. Global Market Insights. https://www.gminsights.com/industry-analysis/direct-to-consumer-dtc-gen…
Tandy-Connor, S., Guiltinan, J., Krempely, K., LaDuca, H., Reineke, P., Gutierrez, S., . . . Davis, B.T. (2018). False-positive results released by direct-to-consumer genetic tests highlight the importance of clinical confirmation testing for appropriate patient care. Genetics in Medicine, 20(12), 1515–1521. https://doi.org/10.1038/gim.2018.38
Underhill-Blazey, M., & Klehm, M.R. (2020). Genetic discrimination: The Genetic Information Nondiscrimination Act’s impact on practice and research. Clinical Journal of Oncology Nursing, 24(2), 135–137. https://doi.org/10.1188/20.CJON.135-137
U.S. Department of Health and Human Services. (2023). Nationwide genetic testing fraud. Office of the Inspector General. https://oig.hhs.gov/newsroom/media-materials/media-materials-nationwide…
U.S. Food and Drug Administration. (2019). Direct-to-consumer tests. https://www.fda.gov/medical-devices/in-vitro-diagnostics/direct-consume…
U.S. Food and Drug Administration. (2020). CLIA categorizations. https://www.fda.gov/medical-devices/ivd-regulatory-assistance/clia-cate…


