Mindful Breathing: Effects of a Five-Minute Practice on Perceived Stress and Mindfulness Among Patients With Cancer
Background: Cancer can cause undesired side effects that can significantly alter patients’ perceived stress and mindfulness. The integration of nonpharmacologic, complementary health interventions, such as mindful breathing, is potentially useful in reducing stress and promoting the well-being of patients during treatment.
Objectives: This study examined the effects of a five-minute mindful breathing practice performed three times per day for three months on perceived stress and mindfulness among patients with cancer.
Methods: This longitudinal, randomized controlled study used a two-group, pre-/post-study design. Patients with distress scores of 4 or higher were randomized into two study arms. Participants in the intervention group were educated on mindfulness and guided on how to perform a five-minute mindful breathing practice. Perceived stress and mindfulness were assessed at baseline, one month postintervention, and three months postintervention.
Findings: Both groups had no significant difference in perceived stress and mindfulness scores at baseline. At three months, the intervention group reported a significant reduction in stress and an increase in mindfulness.
Jump to a section
Cancer is a significant global healthcare issue. Cancer and its treatment can often cause undesired side effects that can significantly alter patients’ perceived stress and mindfulness either temporarily or permanently. The emotional and psychological state of patients with cancer during treatment can be fragile. Patients might experience stress that upsets all aspects of their lives, including emotions, behavior, thinking ability, and physical health, all of which can significantly affect the ability to cope during treatment (National Comprehensive Cancer Network [NCCN], 2021). Patients with cancer can use complementary health approaches, such as natural products or mind–body practices, to manage physical symptoms and psychological distress. Therefore, the integration of a nonpharmacologic mind–body practice, such as mindful breathing, is an effective, evidence-based, complementary health approach that can be beneficial to patients without any adverse reactions (National Center for Complementary and Integrative Health, 2018).
The concept of mindfulness originates from ancient contemplative traditions and has been integrated in a secular way for stress reduction in health care since the 1970s (Harrington & Dunne, 2015). The practice of mindfulness helps individuals to motivate internal resources to openly face issues, to be conscious of and position themselves to overcome pressure, and to push themselves through it (Kabat-Zinn, 2013). Mindfulness creates a psychological distance between an individual’s perception of a stressful stimulus and the resulting response, such as thoughts, actions, and speech.
A review by Creswell (2017) found a number of studies that showed the potential benefits of mindfulness-based interventions in different patient populations, as well as in healthy adults and children. In a study by Wu et al. (2019), a systematic, well-defined, group-based, patient-centered psychotherapy educational program that integrated mindful meditation enabled patients to respond positively instead of reacting impulsively with negative emotions. Mindfulness-based stress reduction (MBSR) and mindfulness-based cognitive therapy (MBCT) place significant emphasis on engaging participants in formal meditative practices, and dialectical behavior therapy and acceptance and commitment therapy incorporate a range of informal mindfulness exercises to approach treatment (Janssen et al., 2018). Mindfulness-based interventions are potentially useful in reducing stress and promoting the well-being of patients during treatment (Wirth et al., 2019).
Mindful breathing is a simple mind–body practice that provides a foundation for further mindfulness-based intervention. This practice aims to bring attention and focus on breathing to feel the effects of the breath in the body. Controlled and rhythmic breathing modulates the insula, and the interoceptive network increases interoception and its associated function (Fox & Cahn, 2018). Sequentially, increased vagal tone activates the parasympathetic nervous system and deactivates the sympathetic nervous system. Mindfulness practice is associated with lower amygdala activation, which can enhance cognitive awareness (Kral et al., 2018). These cognitive gains facilitate stress regulation and, in turn, generate a sense of calm, peace, and balance (Gibson, 2019). Research has examined the immediate effects of mindful breathing. A randomized controlled trial of a five-minute mindful breathing intervention among patients in palliative care revealed rapid improvement in perceived distress and physiological responses (Ng et al., 2016). However, there is still a lack of evidence on the long-term efficacy of a five-minute mindful breathing intervention to decrease stress and promote mindfulness.
Because of the scarcity of evidence on mindful breathing and patient-reported outcomes, this study aimed to examine the effects of a five-minute mindful breathing intervention on perceived stress and mindfulness in patients with cancer undergoing treatment. This study is important in guiding patients to make informed decisions pertaining to the use of mindful breathing during treatment for cancer. By practicing mindful breathing, patients are more likely to be able to cope with treatment and cancer-related stress, which may positively affect their health and overall well-being during treatment. The purpose of the study was to examine the effects of five minutes of mindful breathing three times per day for three months on perceived stress and mindfulness among patients with cancer.
Methods
A two-arm, randomized controlled, longitudinal study was conducted in a tertiary referral teaching hospital from April 2018 to May 2019. The study was reviewed and approved by the University Malaya Medical Centre Medical Research Ethics Committee.
Sample
The sample size of the study was calculated using G*Power software, version 3.0.10, based on an alpha of 0.05, a power of 80%, and a modest effect size (Ng et al., 2016). An additional 20% of the calculated sample size was added to anticipate nonadherence and missing data. The final calculated sample size was 50 for the intervention group and 50 for the control group. The inclusion criteria were patients diagnosed with stage I–III cancer with a distress score of 4 or higher on the NCCN (2021) Distress Thermometer (DT) who could understand and follow simple instructions. Patients who had difficulty breathing, patients with cognitive or comprehension issues, or patients diagnosed with advanced stage cancer (stage IV) were excluded. The researchers intend to study a cohort of patients with advanced stage cancer separately.
Procedures
Patients who met the inclusion criteria were invited to participate in the study, and those who agreed to participate were screened for distress using the DT. Patients with a distress score of 4 or higher were randomly assigned to either the intervention or control group using computer-generated random numbers. Participants in the control group received standard care with routine health education on coping with cancer treatment provided by the nurses. In addition to standard care and routine health education, participants in the intervention group were educated on physical and emotional health, physiology of stress, mindfulness, and mindful breathing and were given resources for learning more about mindful breathing (Oxford Mindfulness Centre, n.d.; Tan et al., 2017; Winston, 2016). Participants in the intervention group were then taught to perform five minutes of mindful breathing. The research assistant who taught the mindful breathing intervention received a training session in advance to ensure procedure and intervention standardization.
Intervention
Mindful breathing is a mindfulness exercise that involves using breathing as an object of attention (Tan et al., 2017). A brief version of a five-minute mindful breathing intervention was adapted from Beng et al. (2016). It consisted of the following three steps: (a) adopt a physical posture, (b) establish a mindfulness anchor, and (c) maintain mindfulness. To adopt a physical posture, participants were helped to sit upright on a chair, which helped them to maintain positive mental health and well-being. Participants were then taught how to establish a mindfulness practice by controlling the mind to be present in the moment. One of the easiest ways to do this is by paying attention to the process of breathing. In the last step, participants were encouraged to maintain their focus in the present moment and regulate ruminations while continuing to be in a mindful state by paying attention to the breathing process. Participants were constantly reminded to focus on their breathing whenever their mind wandered. They were guided to focus their attention on the breathing process for five minutes. A booklet that contained information on mindful breathing and a breathing diary was distributed to participants. The booklet was made available in three languages: English, Bahasa Malaysia, and Mandarin. The participants were required to perform the five-minute mindful breathing practice three times per day (morning, afternoon, and night) and document their experiences in the breathing diary for three months. Researchers sent weekly reminders to the participants to improve adherence to the practice. Reminders were also sent to clarify instructions and address participants’ questions. Participants completed a self-administered questionnaire, which consisted of the study instruments and the patient characteristic items, at baseline once they consented to participate in the study, one month postintervention (T1), and three months postintervention (T2).
Instruments
Perceived stress is operationally defined as feelings or thoughts that individuals have about how much stress they are under during a given period. In the current study, perceived stress was measured using the 10-item Perceived Stress Scale (PSS-10) (Cohen et al., 1983). The PSS-10 measures perceived stress using a five-point, Likert-type scale ranging from 0 (never) to 4 (very often). Item responses for each participant are calculated by reverse scoring four items (4, 5, 7, and 8) and summing all items, yielding a total perceived stress score ranging from 0 to 40, with higher scores indicating higher levels of perceived stress.
Mindfulness was measured using the Cognitive and Affective Mindfulness Scale–Revised (CAMS-R). The CAMS-R is a 12-item, Likert-type scale that measures mindfulness in general daily experience (Feldman et al., 2006). Each item is rated on a scale ranging from 1 to 4 (1 = rarely/not at all, 2 = sometimes, 3 = often, and 4 = almost always), with higher total scores indicating higher levels of mindfulness.
A pilot study was conducted with 10 patients with cancer to confirm that the methods and instruments used were applicable and feasible. The content validity of the PSS-10 and the CAMS-R was ascertained by getting feedback from a panel of experts.
Data Analysis
A Shapiro–Wilk test was used to determine normality for the dependent variables (perceived stress and mindfulness). The p values were more than 0.05, with asymmetry and kurtosis between –2 and 2. Therefore, the data are assumed to be normally distributed. An independent-samples t test was conducted to compare the levels of perceived stress and mindfulness between the control and intervention groups. A p value of < 0.05 was considered significant.
Results
One hundred and eighty-three patients were invited to participate in the study. Forty-six patients declined to participate because of a lack of interest, and 37 patients were excluded from the study because they had a distress score of less than 4 on the DT. The remaining 100 patients were randomly assigned to the control group (n = 50) or the intervention group (n = 50). The response rate was 54.6%, with 83 participants having successfully completed the study (41 participants in the control and 42 in the intervention group, respectively). Reasons for not completing the study included poor physical health (n = 5) and finding participation burdensome (n = 4) for participants in the control group and nonadherence (n = 5) and poor physical health (n = 3) in the intervention group. The adherence rate was at 84% in the intervention group.
The average age of participants in the control and intervention groups was 56 years (SD = 13.6) and 54 years (SD = 11.15), respectively. The mean distress score for the control group was 5.59 (SD = 1.71) and 5.81 (SD = 1.51) for the intervention group. There were no significant differences (p > 0.05) between the control and intervention groups in age, distress score, ethnicity, marital status, education level, disease stage, and treatment type. Demographic information and treatment characteristics for the control and intervention groups are presented in Table 1. 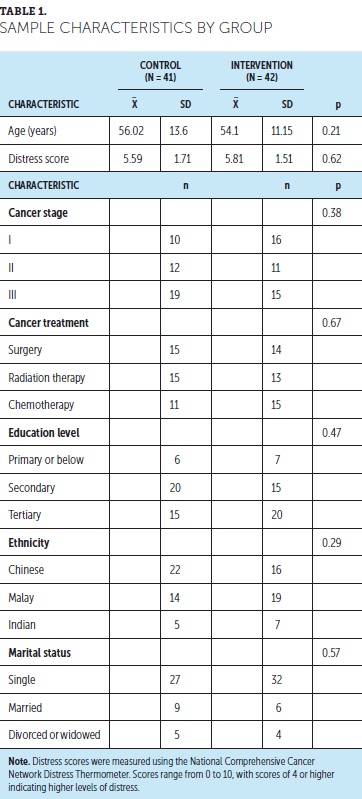
The intervention and control groups had no significant difference in mean perceived stress scores at baseline and T1. However, there was a significance difference between the control (mean = 29.02, SD = 3.42) and intervention (mean = 25.55, SD = 5.57) groups (t[81] = 3.4, p = 0.001) at T2. There was also a significant difference (p = 0.02) in mean perceived mindfulness scores at baseline and T2 (see Table 2). 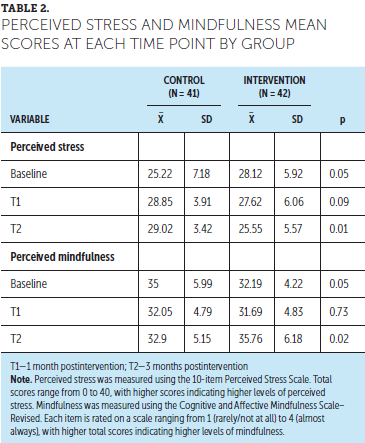
Mean difference (MD) scores between the control and intervention groups are presented in Table 3. In the intervention group, participants’ levels of perceived stress were significantly different between T2 and baseline (MD = –2.57, p = 0.03), indicating a significant reduction in the level of perceived stress experienced. The effect size (d = 0.44) was medium (Cohen, 1988). In the control group, there was a significant difference in participants’ perceived stress between T2 and baseline (MD = 3.8, p = 0.007) and T1 and baseline (MD = 3.63, p = 0.006), indicating an increase in the level of perceived stress experienced by participants. In the intervention group, the level of perceived mindfulness between T2 and baseline was significantly different (MD = 3.57, SD = 7.55, p = 0.001), indicating a significant increase in perceived mindfulness. The effect size was large (d = 0.62) (Cohen, 1988). Participants in the control group reported a decreased level of mindfulness from baseline to T2. The decrease was significant between T1 and baseline (MD = –2.95, SD = 6.62, p = 0.001). The effect size was large (d = 0.54) (Cohen, 1988). 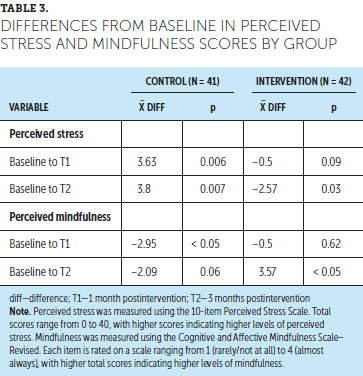
Discussion
After three months of participating in a five-minute mindful breathing practice three times per day, the intervention group reported a significantly lower stress level and an improved level of mindfulness compared to the control group. This is consistent with the study by Beng et al. (2016), which reported that a five-minute mindful breathing intervention may reduce distress rapidly in patients and families in the palliative care setting. Similarly, Ng et al. (2016) surmised that patients with cancer in palliative care experienced rapid improvements in perceived distress, with significant reductions in blood pressure, pulse rate, breathing rate, as well as galvanic skin response and increment of skin surface temperature, after participating in five minutes of mindful breathing. In general, mindfulness training enhances a more positive state of mind and fewer traumatic avoidance symptoms (Boyd et al., 2018). Being mindful has assisted patients in being present in the moment instead of worrying about the past or feeling stressed about the future. Mindful breathing has been associated with harmonizing communication between the mind and breathing and increasing positive automatic thoughts by bringing awareness to the natural rhythm of the breath (Cho et al., 2016). Mindful breathing can help patients to detach from their thoughts, feelings, and emotions, which could allow them to work through and understand those feelings instead of allowing feelings of stress to overwhelm them. Mindful breathing is a simple mind–body practice that can help to enhance the mind’s capacity to improve the overall health and to ease the body into a state of calm and relaxation (Zaccaro et al., 2018).
The intervention group in the current study reported an adherence rate of 84%. This provides initial evidence that performing a five-minute mindful breathing practice three times per day is a feasible intervention and can be incorporated into the daily lives of patients with cancer. Mindful breathing can be performed by simply focusing attention on the breathing process of inhalation and exhalation. It is a quick and easy mind–body practice that requires no instructor, can be performed in an impromptu manner at any given time or place during stressful moments, and helps to reduce negative emotions.
The results of the current study have expanded on the existing literature on the therapeutic benefits of mindfulness interventions for patients with cancer in addition to traditional in-person programs, such as MBSR or MBCT. A paradigm shift that integrates conventional medicine and evidence-based nonpharmacologic interventions during the cancer trajectory is inevitable as more patients wish to proactively contribute to their health and well-being (Nguyen et al., 2016). A five-minute mindful breathing intervention could be recommended to patients with cancer as a stress management technique to buffer against stress during the journey to survival or during the recovery process following treatment.
Although 183 patients were approached for the current study, 46 patients declined to participate. One reason may be the typical response to stress, in which the individual decides to avoid situations and people who are associated with stressful events (Rosiek-Kryszewska & Leksowski, 2018). It is also important to note that 37 patients who were approached recorded a stress score of 3 or less on the DT, which indicates that these patients did not perceive themselves to be stressed. However, there could be a possibility that these patients failed to recognize feelings of stress (American Psychological Association, 2013).
Strengths and Limitations
The results of this study showed that a five-minute mindful breathing practice performed on a regular basis (three times per day) for three months provided sustainable effects that alleviated stress and restored levels of mindfulness among patients with cancer. Regular mindful breathing can be more beneficial to patients compared to standard two-hour, weekly group sessions guided by a therapist for two months in addition to a one-day retreat with a MBSR or MBCT program. This finding is rather encouraging because the five-minute mindful breathing practice is relatively simple to learn, inexpensive, and can easily be integrated into daily life. The high adherence rate in the current study (84%) indicates that mindful breathing can be done alone, anywhere, and at any time.
However, this study does have several limitations that should be considered when interpreting the results. First, participants were recruited from a single health center. A larger-scale study that includes participants from multiple centers is needed to provide greater statistical reliability. Second, although participants were randomly assigned to either the control or intervention group using computer-generated random numbers to mitigate selection biases, inadequate allocation concealment may be subjected to allocation biases. Third, patients with advanced stage cancer were excluded from the study to ensure the homogeneity of the sample. Additional research is needed to expand the current findings regarding the potential benefits of mindful breathing in this cohort of patients living with metastatic cancer. Despite these limitations, this study is the first to examine the sustainable effects of a five-minute mindful breathing intervention among patients with cancer. 
Conclusion
Mindful breathing combines rhythmic breathing and attention paying to the present moment in an accepting, nonjudgmental way. The practice of mindful breathing slows down the breathing pattern and intensifies vagus nerve action. It also helps to regulate the body’s responses to stress. The five-minute mindful breathing intervention showed positive effects in reducing stress and improving mindfulness in patients with cancer during treatment. This study offers evidence supporting the use of regular sessions of five-minute mindful breathing practice, which can be easily implemented in tandem with standard health education to patients with cancer across the cancer trajectory. 
About the Author(s)
Ping Lei Chui, RN, BNSc, MMedSc, PhD, is a nurse lecturer in the Department of Nursing Science, Suetyen Wai, MBBS, is a doctor, Lee-Lee Lai, MMSc, is a lecturer in the Department of Nursing Science, Mee Hong See, MD, is an associate professor and a breast surgeon consultant in the Department of Surgery, and Seng Beng Tan, MRCP, is an associate professor in palliative medicine in the Department of Medicine, all in the Faculty of Medicine at the University of Malaya in Kuala Lumpur, Malaysia. The authors take full responsibility for this content. This work was supported by the University of Malaya Specialist Centre Care Grant (Project No. PV026-2017). The article has been reviewed by independent peer reviewers to ensure that it is objective and free from bias. Chui can be reached at chuipinglei@um.edu.my, with copy to CJONEditor@ons.org. (Submitted June 2020. Accepted August 11, 2020.)
References
American Psychological Association. (2013). How stress affects your health. https://www.apa.org/topics/stress/health
Beng, T.S., Ahmad, F., Loong, L.C., Chin, L.E., Zainal, N.Z., Guan, N.C., . . . Meng, C.B.C. (2016). Distress reduction for palliative care patients and families with 5-minute mindful breathing: A pilot study. American Journal of Hospice and Palliative Medicine, 33(6), 555–560. https://doi.org/10.1177/1049909115569048
Boyd, J.E., Lanius, R.A., & McKinnon, M.C. (2018). Mindfulness-based treatments for posttraumatic stress disorder: A review of the treatment literature and neurobiological evidence. Journal of Psychiatry and Neuroscience, 43(1), 7–25. https://doi.org/10.1503/jpn.170021
Cho, H., Ryu, S., Noh, J., & Lee, J. (2016). The effectiveness of daily mindful breathing practices on test anxiety of students. PLOS ONE, 11(10), e0164822. https://doi.org/10.1371/journal.pone.0164822
Cohen, J. (1988). Statistical power analysis for the behavioral sciences (2nd ed.). Lawrence Erlbaum Associates.
Cohen, S., Kamarck, T., & Mermelstein, R. (1983). A global measure of perceived stress. Journal of Health and Social Behavior, 24(4), 385–396. https://doi.org/10.2307/2136404
Creswell, J.D. (2017). Mindfulness interventions. Annual Review of Psychology, 68(1), 491–516. https://doi.org/10.1146/annurev-psych-042716-051139
Feldman, G., Hayes, A., Kumar, S., Greeson, J., & Laurenceau, J.P. (2006). Mindfulness and emotion regulation: The development and initial validation of the Cognitive and Affective Mindfulness Scale-Revised (CAMS-R). Journal of Psychopathology and Behavioral Assessment, 29(3), 177–190. https://doi.org/10.1007/s10862-006-9035-8
Fox, K., & Cahn, B.R. (2018). Meditation and the brain in health and disease. https://doi.org/10.31231/osf.io/m2sez
Gibson, J. (2019). Mindfulness, interoception, and the body: A contemporary perspective. Frontiers in Psychology, 10, 2012. https://doi.org/10.3389/fpsyg.2019.02012
Harrington, A., & Dunne, J.D. (2015). When mindfulness is therapy: Ethical qualms, historical perspectives. American Psychologist, 70(7), 621–631. https://doi.org/10.1037/a0039460
Janssen, M., Heerkens, Y., Kuijer, W., van der Heijden, B., & Engels, J. (2018). Effects of mindfulness based stress reduction on employees’ mental health: A systematic review. PLOS ONE, 13(1), e0191332. https://doi.org/10.1371/journal.pone.0191332
Kabat-Zinn, J. (2013). Full catastrophe living: Using the wisdom of your body and mind to face stress, pain, and illness (revised ed.). Bantam Books.
Kral, T.R.A., Schuyler, B.S., Mumford, J.A., Rosenkranz, M.A., Lutz, A., & Davidson, R.J. (2018). Impact of short- and long-term mindfulness meditation training on amygdala reactivity to emotional stimuli. NeuroImage, 181, 301–313. https://doi.org/10.1016/j.neuroimage.2018.07.013
National Center for Complementary and Integrative Health. (2018). Complementary, alternative, or integrative health: What’s in a name? U.S. Department of Health and Human Services. https://www.nccih.nih.gov/health/complementary-alternative-or-integrati…
National Comprehensive Cancer Network. (2021). NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines®): Distress management [v.2.2021]. https://www.nccn.org/professionals/physician_gls/pdf/distress.pdf
Ng, C.G., Lai, K.T., Tan, S.B., Sulaiman, A.H., & Zainal, N.Z. (2016). The effect of 5 minutes of mindful breathing to the perception of distress and physiological responses in palliative care cancer patients: A randomized controlled study. Journal of Palliative Medicine, 19(9), 917–924. https://doi.org/10.1089/jpm.2016.0046
Nguyen, L.T., Yates, P., Annoussamy, L.C., & Truong T.Q. (2016). The effectiveness of non-pharmacological interventions in the management of symptom clusters in adult cancer patients: A systematic review protocol. JBI Database of Systematic Reviews and Implementation Reports, 14(4), 49–59. https://doi.org/10.11124/jbisrir-2016-2476
Oxford Mindfulness Centre. (n.d.). Resources and free audio practices. University of Oxford Department of Psychiatry. https://www.oxfordmindfulness.org/learn-mindfulness/resources
Rosiek-Kryszewska, A., & Leksowski, K. (2018). Healthcare administration for patient safety and engagement. IGI Global. https://doi.org/10.4018/978-1-5225-3946-9
Tan, S.B., Capelle, D.P., Zainal, N.Z., Lim, E.J., Loh, E.C., & Lam, C.L. (2017). Mindfulness: A new paradigm of psychosocial care in the palliative care setting in Southeast Asia. Annals of the Academy of Medicine, Singapore, 46(9), 339–346.
Winston, D. (2016). A 5-minute breathing meditation to cultivate mindfulness. https://www.mindful.org/a-five-minute-breathing-meditation
Wirth, M.D., Franco, R., Wagner Robb, S., Daniels, K., Susko, K., Hudson, M.F., & O’Rourke, M.A. (2019). Randomized controlled trial of a 4-week mindfulness intervention among cancer survivors compared to a breathing control. Cancer Investigation, 37(4–5), 227–232. https://doi.org/10.1080/07357907.2019.1610968
Wu, R., Liu, L.L., Zhu, H., Su, W.J., Cao, Z.Y., Zhong, S.Y., . . . Jiang, C.L. (2019). Brief mindfulness meditation improves emotion processing. Frontiers in Neuroscience, 13, 1074. https://doi.org/10.3389/fnins.2019.01074
Zaccaro, A., Piarulli, A., Laurino, M., Garbella, E., Menicucci, D., Neri, B., & Gemignani, A. (2018). How breath-control can change your life: A systematic review on psycho-physiological correlates of slow breathing. Frontiers in Human Neuroscience, 12, 353. 10.3389/fnhum.2018.00353




